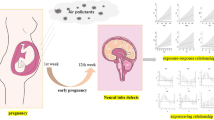
Abstract
Exposure to air pollution during pregnancy has been linked to birth defects. But the directions of studies on the associations between air pollutants exposure and effect on the incidence of congenital heart disease (CHDs) were inconsistent. To date, few studies were concentrated on the effects of both particulate matter and gaseous air pollutant exposure on CHDs across the full gestational week simultaneously. Our study aimed to investigate the critical exposure windows for each air pollutant throughout 40 gestational weeks. Data on CHDs, air pollution, and meteorological factors from 2013 to 2019 were collected in Lanzhou, China. A distributed lag nonlinear model combined with a quasi-Poisson regression model was applied to evaluate the weekly exposure–lag–response association between air pollutants levels and CHDs, and the subgroup analyses were conducted by gender (baby boy and baby girl). The study included 1607 mother–infant pairs. The results demonstrated that exposure of pregnant women to particulate matter ≤ 5 μm (PM2.5) at lag 1–4 weeks was significantly associated with the risk of CHDs, and the strongest effects were observed in the lag 1 week (1.150, 95%CI 1.059–1.248). For exposure to particulate matter ≤ 10 μm (PM10) at lag 1–3 weeks, the strongest effects were observed in the lag 1 week (1.075, 95% CI 1.026–1.128). For exposure to sulfur dioxide (SO2) at lag 1–4 weeks, the strongest effects were observed in the lag 1 week (1.154, 95% CI 1.025–1.299). For exposure to carbon monoxide (CO) at lag 1–3 weeks, the strongest effects were observed in the lag 1 week (1.089, 95% CI 1.002–1.183). For exposure to ozone (O3) concentration at lag 9–15 weeks, the strongest effects were observed in the lag 15 weeks (1.628, 95% CI 1.001–2.649). The cumulative effects of PM2.5, PM10, SO2, and CO along weeks with a maximum of 1.609 (95%CI 1.000–2.589), 1.286 (95%CI 1.007–1.641), 1.648 (95%CI 1.018–2.668), and 1.368 (95%CI 1.003, 1.865), respectively. The effects were obvious in the initial gestational weeks too. Through the gender stratification analysis, the air pollutants with significant effects were PM2.5 for baby boys and PM2.5, PM10, SO2, CO, NO2, and O3 for baby girl. For the relationship between CHDs and air pollution in Lanzhou, PM2.5, PM10, SO2, CO, and O3 played an important role in the initial gestational weeks, especially for baby girl.






Similar content being viewed by others
Data availability
The data of the mother–infant pairs that support the findings of this study were provided by the Lanzhou Birth Defects Surveillance System. The data are not publicly available due to privacy or ethical restrictions. The data on air pollutants from 2013 to 2019 was obtained from the website of the National Real-Time Urban Air Quality Release Platform, these data were derived from the following resources available in the public domain: [http://106.37.208.233:20035]. The meteorological data for the same period were obtained from the China Meteorological Data Network, these data were derived from the following resources available in the public domain: [http://data.cma.cn/]. This study did not involve animal testing.
References
Agay-Shay, K., Friger, M., Linn, S., Peled, A., Amitai, Y., & Peretz, C. (2013). Air pollution and congenital heart defects. Environmental Research, 124, 28–34. https://doi.org/10.1016/j.envres.2013.03.005
Allen, M. J., & Sheridan, S. C. (2018). Mortality risks during extreme temperature events (ETEs) using a distributed lag non-linear model. International Journal of Biometeorology, 62, 57–67. https://doi.org/10.1007/s00484-015-1117-4
Avissar-Whiting, M., Veiga, K. R., Uhl, K. M., Maccani, M. A., Gagne, L. A., Moen, E. L., & Marsit, C. J. (2010). Bisphenol A exposure leads to specific microRNA alterations in placental cells. Reproductive Toxicology, 29(4), 401–406. https://doi.org/10.1016/j.reprotox.2010.04.004
Backes, C. H., Nelin, T., Gorr, M. W., & Wold, L. E. (2013). Early life exposure to air pollution: How bad is it? Toxicology Letters, 216, 47–53. https://doi.org/10.1016/j.toxlet.2012.11.007
Bai, L., Woodward, A., & Liu, Q. (2014). Temperature and mortality on the roof of the world: A time-series analysis in three Tibetan counties, China. Science of the Total Environment., 485–486, 41–48. https://doi.org/10.1016/j.scitotenv.2014.02.094
Bové, H., Bongaerts, E., Slenders, E., Bijnens, E. M., Saenen, N. D., Gyselaers, W., Van Eyken, P., Plusquin, M., Roeffaers, M. B. J., Ameloot, M., & Nawrot, T. S. (2019). Ambient black carbon particles reach the fetal side of human placenta. Nature Communications, 1, 3866. https://doi.org/10.1038/s41467-019-11654-3
Brook, R. D., Franklin, B., Cascio, W., Hong, Y., Howard, G., Lipsett, M., Luepker, R., Mittleman, M., Samet, J., Smith, S. C., & Tager, I. (2004). Air pollution and cardiovascular disease: A statement for healthcare professionals from the expert panel on population and prevention science of the American Heart Association. Circulation, 109(21), 2655–2671. https://doi.org/10.1161/01.CIR.0000128587.30041.C8
Buchet, J. P., Roels, H., Hubermont, G., & Lauwerys, R. (1978). Placental transfer of lead, mercury, cadmium, and carbon monoxide in women. II. influence of some epidemiological factors on the frequency distributions of the biological indices in maternal and umbilical cord blood. Environmental Research, 15, 494–503. https://doi.org/10.1016/0013-9351(78)90128-7
Burton, G. J., & Jauniaux, E. (2018). Development of the human placenta and fetal heart: Synergic or independent? Frontiers in Physiology, 9, 373. https://doi.org/10.3389/fphys.2018.00373
Center CBDM. (2012) Chinese National Criteria of Birth Defects and Tiny Deformities stated. Available online http://www.mchscn.cn/admin/wenjian/wxjxbgbz-2012.pdf
Chakraborty, J., Collins, T. W., & Grineski, S. E. (2016). Environmental justice research: Contemporary issues and emerging topics. International Journal of Environmental Research and Public Health. https://doi.org/10.3390/ijerph13111072
China MaCHMMi. (2013). Available online https://www.docin.com/p-1676277666.html.
Dadvand, P., Rankin, J., Rushton, S., & Pless-Mulloli, T. (2011a). Association between maternal exposure to ambient air pollution and congenital heart disease: A register-based spatiotemporal analysis. American Journal of Epidemiology, 173, 171–182. https://doi.org/10.1093/aje/kwq342
Dadvand, P., Rankin, J., Rushton, S., & Pless-Mulloli, T. (2011b). Ambient air pollution and congenital heart disease: A register-based study. Environmental Research, 111, 435–441. https://doi.org/10.1016/j.envres.2011.01.022
Duan, W., Wang, X., Cheng, S., Wang, R., & Zhu, J. (2021). Influencing factors of PM(2.5) and O(3) from 2016 to 2020 based on DLNM and WRF-CMAQ. Environmental Pollution (barking, Essex : 1987), 285, 117512. https://doi.org/10.1016/j.envpol.2021.117512
Gasparrini, A. (2011). distributed lag linear and non-linear models in R: The package dlnm. Journal of Statistical Software, 43, 1–20.
Gasparrini, A., Armstrong, B., & Kenward, M. G. (2010). Distributed lag non-linear models. Statistics in Medicine, 29, 2224–2234. https://doi.org/10.1002/sim.3940
Gebretensae, Y. A., & Asmelash, D. (2021). Trend analysis and forecasting the spread of COVID-19 Pandemic in Ethiopia using Box-Jenkins modeling procedure. International Journal of General Medicine, 14, 1485–1498. https://doi.org/10.2147/ijgm.S306250
Hansen, C. A., Barnett, A. G., Jalaludin, B. B., & Morgan, G. G. (2009). Ambient air pollution and birth defects in brisbane, australia. PLoS ONE, 4, e5408. https://doi.org/10.1371/journal.pone.0005408
Hao, J., Peng, L., Cheng, P., Li, S., Zhang, C., Weinan, F., Dou, L., Yang, F., & Hao, J. (2021). A time series analysis of ambient air pollution and low birth weight in Xuzhou, China. International Journal of Environmental Health Research, 32(6), 1238–1247. https://doi.org/10.1080/09603123.2020.1867828
Heidari-Beni, M., Golshahi, J., Esmaillzadeh, A., & Azadbakht, L. (2015). Potato consumption as high glycemic index food, blood pressure, and body mass index among Iranian adolescent girls. ARYA Atheroscler, 11, 81–87.
Hove, J. R., Köster, R. W., Forouhar, A. S., Acevedo-Bolton, G., Fraser, S. E., & Gharib, M. (2003). Intracardiac fluid forces are an essential epigenetic factor for embryonic cardiogenesis. Nature, 421, 172–177. https://doi.org/10.1038/nature01282
Ibrahim, M. F., Hod, R., Ahmad Tajudin, M. A. B., Wan Mahiyuddin, W. R., Mohammed Nawi, A., & Sahani, M. (2022). Children’s exposure to air pollution in a natural gas industrial area and their risk of hospital admission for respiratory diseases. Environmental Research, 210, 112966. https://doi.org/10.1016/j.envres.2022.112966
Jakpor, O., Chevrier, C., Kloog, I., Benmerad, M., Giorgis-Allemand, L., Cordier, S., Seyve, E., Vicedo-Cabrera, A. M., Slama, R., Heude, B., & Schwartz, J. (2020). Term birthweight and critical windows of prenatal exposure to average meteorological conditions and meteorological variability. Environment International, 142, 105847. https://doi.org/10.1016/j.envint.2020.105847
Janssen, B. G., Godderis, L., Pieters, N., Poels, K., Kiciński, M., Cuypers, A., Fierens, F., Penders, J., Plusquin, M., Gyselaers, W., & Nawrot, T. S. (2013). Placental DNA hypomethylation in association with particulate air pollution in early life. Particle and Fibre Toxicology. https://doi.org/10.1186/1743-8977-10-22
Javadinejad, S., Ostad-Ali-Askari, K., & Jafary, F. (2019). Using simulation model to determine the regulation and to optimize the quantity of chlorine injection in water distribution networks. Modeling Earth Systems and Environment, 5, 1015–1023. https://doi.org/10.1007/s40808-019-00587-x
Jin, L., Qiu, J., Zhang, Y., Qiu, W., He, X., Wang, Y., Sun, Q., Li, M., Zhao, N., Cui, H., & Liu, S. (2015). Ambient air pollution and congenital heart defects in Lanzhou, China. Environmental Research Letters. https://doi.org/10.1088/1748-9326/10/7/074005
Jinyu, X., & Qingqing, W. (2017). Genetic factors in the pathogenesis of congenital heart disease: Research progress. Chinese Journal of Obstetrics & Gynecology and Pediatrics (electronic Edition), 13, 611–615. https://doi.org/10.3877/cma.j.issn.1673-5250.2017.05.020
Jixiang, X., Geng, W., Geng, X., Cui, L., Ding, T., Xiao, C., Zhang, J., Tang, J., & Zhai, J. (2020). Study on the association between ambient air pollution and daily cardiovascular death in Hefei, China. Environmental Science and Pollution Research, 27(1), 547–561. https://doi.org/10.1007/s11356-019-06867-4
Kalkstein, A. J., Kalkstein, L. S., Vanos, J. K., Eisenman, D. P., & Grady Dixon, P. (2018). Heat/mortality sensitivities in Los Angeles during winter: A unique phenomenon in the United States. Environmental Health, 17, 45. https://doi.org/10.1186/s12940-018-0389-7
Kim, H., & Lee, J. T. (2019). On inferences about lag effects using lag models in air pollution time-series studies. Environmental Research, 171, 134–144. https://doi.org/10.1016/j.envres.2018.12.032
Kowalski, W. J., Pekkan, K., Tinney, J. P., & Keller, B. B. (2014). Investigating developmental cardiovascular biomechanics and the origins of congenital heart defects. Frontiers in Physiology, 5, 408. https://doi.org/10.3389/fphys.2014.00408
Lavigne, E., Lima, I., Hatzopoulou, M., Van Ryswyk, K., Decou, M. L., Luo, W., van Donkelaar, A., Martin, R. V., Chen, H., Stieb, D. M., & Crighton, E. (2019). Spatial variations in ambient ultrafine particle concentrations and risk of congenital heart defects. Environment International, 130, 104953. https://doi.org/10.1016/j.envint.2019.104953
Liu, Y., Chen, S., Zühlke, L., Black, G. C., Choy, M., Li, N., & Keavney, B. D. (2019). Global birth prevalence of congenital heart defects 1970–2017: Updated systematic review and meta-analysis of 260 studies. International Journal of Epidemiology, 48(2), 455–463. https://doi.org/10.1093/ije/dyz009
Moore-Morris, T., van Vliet, P. P., Andelfinger, G., & Puceat, M. (2018). Role of epigenetics in cardiac development and congenital diseases. Physiological Reviews, 98, 2453–2475. https://doi.org/10.1152/physrev.00048.2017
Ostad-Ali-Askari, K., Shayannejad, M., & Ghorbanizadeh-Kharazi, H. (2017). Artificial neural network for modeling nitrate pollution of groundwater in marginal area of Zayandeh-rood River, Isfahan. Iran. KSCE Journal of Civil Engineering, 21, 134–140. https://doi.org/10.1007/s12205-016-0572-8
Padula, A. M., Tager, I. B., Carmichael, S. L., Katharine Hammond, S., Yang, W., Lurmann, F., & Shaw, G. M. (2013). Ambient air pollution and traffic exposures and congenital heart defects in the San Joaquin Valley of California: Air pollution and congenital heart defects. Paediatric and Perinatal Epidemiology, 27(4), 329–339. https://doi.org/10.1111/ppe.12055
Pang, Y., Liu, S., Yan, L., Wang, Q., Li, L., Chu, C., Ning, J., Zhang, B., Wang, X., Ma, S., & Su, D. (2021). Associations of long-term exposure to traffic-related air pollution with risk of valvular heart disease based on a cross-sectional study. EcotoxIcology and Environmental Safety, 209, 111753. https://doi.org/10.1016/j.ecoenv.2020.111753
Pedersen, M., Garne, E., Hansen-Nord, N., Hjortebjerg, D., Ketzel, M., Raaschou-Nielsen, O., Andersen, A. M. N., & Sørensen, M. (2017). Exposure to air pollution and noise from road traffic and risk of congenital anomalies in the Danish National Birth Cohort. Environmental Research, 159, 39–45. https://doi.org/10.1016/j.envres.2017.07.031
Ren, Z., Zhu, J., Gao, Y., Yin, Q., Maogui, H., Dai, L., Deng, C., Yi, L., Deng, K., Wang, Y., Li, X., & Wang, J. (2018). Maternal exposure to ambient PM10 during pregnancy increases the risk of congenital heart defects: Evidence from machine learning models. Science of the Total Environment, 630, 1–10. https://doi.org/10.1016/j.scitotenv.2018.02.181
Stingone, J. A., Luben, T. J., Daniels, J. L., Fuentes, M., Richardson, D. B., Aylsworth, A. S., Herring, A. H., Anderka, M., Botto, L., Correa, A., Gilboa, S. M., Langlois, P. H., Mosley, B., Shaw, G. M., Siffel, C., & Olshan, A. F. (2014). Maternal exposure to criteria air pollutants and congenital heart defects in offspring: Results from the national birth defects prevention study. Environmental Health Perspectives, 122(8), 863–872. https://doi.org/10.1289/ehp.1307289
Tan, C. M. J., & Lewandowski, A. J. (2020). The transitional heart: From early embryonic and fetal development to neonatal life. Fetal Diagnosis and Therapy, 47, 373–386. https://doi.org/10.1159/000501906
Vecoli, C., Pulignani, S., & Andreassi, M. G. (2016). Genetic and epigenetic mechanisms linking air pollution and congenital heart disease. Journal of Cardiovascular Development and Disease. https://doi.org/10.3390/jcdd3040032
Wang, W., Guo, W., Cai, J., Guo, W., Liu, R., Liu, X., et al. (2021). Epidemiological characteristics of tuberculosis and effects of meteorological factors and air pollutants on tuberculosis in Shijiazhuang, China: A distribution lag non-linear analysis. Environmental Research, 195, 110310. https://doi.org/10.1016/j.envres.2020.110310
Warner, P. (2015). Poisson regression. Journal of Family Planning and Reproductive Health Care, 41, 223–224. https://doi.org/10.1136/jfprhc-2015-101262
WHO. (2011). Public health and environment database: Outdoor Air Pollution in Cities. Available online http://www.who.int/phe/health_topics/outdoorair/databases/en.
Wick, P., Malek, A., Manser, P., Meili, D., Maeder-Althaus, X., Diener, L., Diener, P. A., Zisch, A., Krug, H. F., & von Mandach, U. (2010). Barrier capacity of human placenta for nanosized materials. Environmental Health Perspectives, 118(3), 432–436. https://doi.org/10.1289/ehp.0901200
Xu, M., & Xie, Q. (2014). Analysis on the Influence Of Time Series Length On The Monthly Streamflow Forecast Effect Based On ARIMA model. Journal of Yangtze University (natural Science Edition), 11, 6–10. https://doi.org/10.16772/j.cnki.1673-1409.2014.34.007
Yang, B. Y., Qu, Y., Guo, Y., Markevych, I., Heinrich, J., Bloom, M. S., Bai, Z., Knibbs, L. C., Li, S., Chen, G., & Jalaludin, B. (2021). Maternal exposure to ambient air pollution and congenital heart defects in China. Environment International, 153, 106548. https://doi.org/10.1016/j.envint.2021.106548
Yitshak-Sade, M., Kloog, I., Schwartz, J. D., Novack, V., Erez, O., & Just, A. C. (2021). The effect of prenatal temperature and PM(2.5) exposure on birthweight: Weekly windows of exposure throughout the pregnancy. Environment International, 155, 106588. https://doi.org/10.1016/j.envint.2021.106588
Yogev-Baggio, T., Bibi, H., Dubnov, J., Or-Hen, K., Carel, R., & Portnov, B. A. (2010). Who is affected more by air pollution-sick or healthy? Some evidence from a health survey of schoolchildren living in the vicinity of a coal-fired power plant in Northern Israel. Health & Place, 16, 399–408. https://doi.org/10.1016/j.healthplace.2009.11.013
Yu, H., Wang, Y., Peng, Q., Shao, Y., Duan, C., Zhu, Y., et al. (2020). Influence of coarse particulate matter on chickenpox in Jiading District, Shanghai, 2009–2018: A distributed lag non-linear time series analysis. Environmental Research, 190, 110039. https://doi.org/10.1016/j.envres.2020.110039
Zhang, B., Zhao, J., Yang, R., Qian, Z., Liang, S., Bassig, A., Zhang, Y., Ke, H., Shunqing, X., Dong, G., Zheng, T., & Yang, S. (2016). Ozone and other air pollutants and the risk of congenital heart defects. Scientific Reports. https://doi.org/10.1038/srep34852
Zhang, H., Zhang, X., Zhao, X., Cheng, G., Chang, H., Ye, X., Wang, J., Yu, Z., Wang, Q., & Huang, C. (2022). Maternal exposure to air pollution and congenital heart diseases in Henan, China: A register-based case-control study. Ecotoxicology and Environmental Safety., 229, 11307010. https://doi.org/10.1016/j.ecoenv.2021.113070
Zhang, Q., Sun, S., Sui, X., Ding, L., Yang, M., Li, C., Zhang, C., Zhang, X., Hao, J., Xu, Y., & Lin, S. (2021). Associations between weekly air pollution exposure and congenital heart disease. Science of the Total Environment., 757, 143821. https://doi.org/10.1016/j.scitotenv.2020.143821
Zhao, L., Chen, L., Yang, T., Wang, T., Zhang, S., Chen, L., Ye, Z., Luo, L., & Qin, J. (2020). Birth prevalence of congenital heart disease in China, 1980–2019: A systematic review and meta-analysis of 617 studies. European Journal of Epidemiology, 35(7), 631–642. https://doi.org/10.1007/s10654-020-00653-0
Zhou, Y., Gilboa, S. M., Herdt, M. L., Lupo, P. J., Dana Flanders, W., Liu, Y., Shin, M., Canfield, M. A., & Kirby, R. S. (2017). Maternal exposure to ozone and PM2.5 and the prevalence of orofacial clefts in four U.S. states. Environmental Research, 153, 35–40. https://doi.org/10.1016/j.envres.2016.11.007
Zhu, G., Zhu, Y., Wang, Z., Meng, W., Wang, X., Feng, J., Li, J., Xiao, Y., Shi, F., & Wang, S. (2021). The association between ambient temperature and mortality of the coronavirus disease 2019 (COVID-19) in Wuhan, China: A time-series analysis. BMC Public Health. https://doi.org/10.1186/s12889-020-10131-7
Zhu, S., Xia, L., Wu, J., Chen, S., Chen, F., Zeng, F., Chen, X., Chen, C., Xia, Y., Zhao, X., & Zhang, J. (2018). Ambient air pollutants are associated with newly diagnosed tuberculosis: A time-series study in Chengdu, China. Science of the Total Environment, 631–632, 47–55. https://doi.org/10.1016/j.scitotenv.2018.03.017
Funding
This work was supported by the Lanzhou talent innovation project (2019-RC-25), the Lanzhou- birth defects monitoring network construction, and the study of congenital heart disease causes to explore integration; Science and Technology Project in Chengguan District, Lanzhou (2020-2-11-13), Factors influencing the occurrence of adverse maternal pregnancy outcomes.
Author information
Authors and Affiliations
Contributions
WZ: Retrieve literature, methodology, statistical analysis, and writing original paper. YY, LZ, RW, LP: investigation, data collection, database establishment. YL, YY: Software, investigation, data check. YH, YB, XR: Funding acquisition, supervision, retrieve literature. YB: Funding design, modification of the paper. NC: Funding design, writing-reviewing, and editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
No ethics involved.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
All individual participants and all authors agree to publication in the Journal, the copyright to the English-language article is transferred to the Journal effective if and when the article is accepted for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhang, W., Yang, Y., Liu, Y. et al. Associations between congenital heart disease and air pollutants at different gestational weeks: a time-series analysis. Environ Geochem Health 45, 2213–2228 (2023). https://doi.org/10.1007/s10653-022-01315-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10653-022-01315-8