Abstract
Background Noncompaction cardiomyopathy (NCCM) is a rare disorder with persistance of the embryonic pattern of myoarchitecture. NCCM is characterized by loosened, spongy myocardium associated with a high incidence of systolic and diastolic left ventricular (LV) dysfunction and heart failure (HF). It is known that LV dysfunction contributes to elevated left atrial (LA) and pulmonary vascular pressures, however atrial function has not been examined in NCCM. The objective of the present study was to assess LA systolic function characterized by LA ejection force (LAEF) in NCCM patients using real-time three-dimensional echocardiography (RT3DE) and to compare to control subjects. Methods The study comprised 17 patients with an established diagnosis of NCCM and their results were compared to 17 healthy age-matched controls with no evidence of cardiovascular disease. Forty-one percent of NCCM patients were in NYHA functional class II / III HF. Previously proposed echocardiographic diagnostic criteria for NCCM were used. All patients underwent conventional two-dimensional echocardiography and RT3DE. LAEF was measured based on MA annulus diameter (LAEF3D-MAD) and area (LAEF3D-MAA) using RT3DE. Results The presence and severity of mitral regurgitation were more frequent in NCCM patients than in control subjects. LV diameters and mitral annulus were significantly increased in NCCM patients. Compared with control subjects, both LAEF3D-MAD (3.8 ± 2.2 vs 2.3 ± 1.0 kdyne, P < 0.05) and LAEF3D-MAA (12.7 ± 7.6 vs 4.9 ± 2.1 kdyne, P < 0.01) were significantly increased in NCCM patients. Conclusions LAEF as a characteristic of LA systolic function is increased in NCCM patients compared to normal individuals. These results can suggest compensating left atrial work against the dysfunctional LV in NCCM patients.
Similar content being viewed by others
Introduction
Noncompaction cardiomyopathy (NCCM) is a rare disorder with persistance of the embryonic pattern of myoarchitecture, and has been assumed to occur as a consequence to intrauterine arrest of compaction [1]. NCCM is characterized by loosened, spongy myocardium associated with a high incidence of systolic and diastolic left ventricular (LV) dysfunction and heart failure. It is known that LV dysfunction contributes to elevated left atrial (LA) and pulmonary vascular pressures, however atrial function has not been examined in NCCM. It is difficult to assess non-invasively LA contraction, but Manning et al. reported a non-invasive method for the evaluation of LA ejection force (LAEF) as a characteristic of LA systolic function [2]. Anwar et al. demonstrated the usefulness of real-time three-dimensional echocardiography (RT3DE) for the evaluation of LAEF [3]. The objective of the present study was to assess LAEF in NCCM patients using RT3DE and to compare to control subjects.
Methods
Patient populations
The study comprised 17 patients with an established diagnosis of NCCM and their results were compared to 17 healthy age-matched controls with no evidence of cardiovascular disease. All patients and control subjects were in sinus rhytm and all of them were examined by two-dimensional echocardiography (2DE) and RT3DE.
Diagnostic criteria for NCCM
Previously proposed echocardiographic diagnostic criteria for NCCM by Jenni et al. were used to include patients into the present study from the Outpatient Clinic of Erasmus Medical Center, Rotterdam during 3 years [4]: (1) absence of coexisting cardiac anomalies, (2) segmental, excessive thickening of the LV wall with a two-layered structure: a thin, compacted epicardial layer and a much thicker, noncompacted layer with the characteristic appearance of numerous, prominent trabeculations (meshwork) and deep intertrabecular recesses, (3) colour Doppler evidence of deeply perfused intertrabecular recesses, and (4) predominant localization of thickening in the LV apical, midlateral, and midinferior walls. Hypertensive heart disease was excluded by clinical and echocardiographic examinations (septal thickness < 13 mm).
2DE examination
The 2DE was undertaken with the patient lying in the left lateral decubitus position using both apical and parasternal views. The 2DE studies were performed using a 3.5-MHz transducer and a commercially available ultrasound system (Sonos 7500, Philips, Best, The Netherlands). The following measures were obtained: (1) LV end-diastolic diameter (LV-EDD) and LV end-systolic diameter (LV-ESD) by M-mode echocardiography; (2) LV fractional shortening (LV-FS); (3) peak velocities of transmitral E and A waves with pulsed Doppler and (4) mitral regurgitation graded as mild (jet area < 4 cm2), moderate (jet area 4–8 cm2), and severe (jet area > 8 cm2) according to maximum jet area by color Doppler.
RT3DE examination
RT3DE was performed using the same ultrasound system, and performed with a X-4 matrix transducer capable of providing real-time B-mode and colour Doppler. The 3D images were collected within 5–7 s of breath holding in full-volume mode. The 3D data were transferred to an offline analysis system (TomTec Inc., Munich, Germany). Data were stored digitally and subsequently evaluated by two echocardiographers. Data analysis of RT3DE imaging was based on a two-dimensional approach relying on the echocardiographic images obtained from the apical views and on manual tracing of inner border of the mitral annulus (MA). Once this was completed the surface area was automatically delineated and could be visualized from different points of views. Manual modification was done to correct any image if necessary. The following measures were obtained: (1) MA diameter (MAD3D) and area (MAA3D) measured at end-diastole (just before mitral valve closure) and (2) LAEF3D-MAD and LAEF3D-MAA calculated by formula as 0.5 × 1.06 × (MAD3D or MAA3D) × V2, where V is the peak velocity of A wave, 1.06 gm/cm3 is blood viscosity and 0.5 is a coefficient factor [2] (Fig. 1).
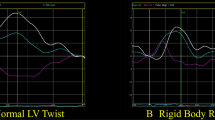
Automatically cropped two-dimensional image from real-time three-dimensional echocardiographic dataset demonstrating left ventricular cavity in a patient with noncompaction cardiomyopathy (A). Measurement of mitral annulus area and mitral inflow A wave velocity can help calculation of left atrial ejection force as a characteristic of atrial systole. Real-time three-dimensional echocardiography allows the `en-face` evaluation of mitral annulus helping exact measurement of mitral annulus diameter and area (B). Abbreviations: MA: mitral annulus, MAD: mitral annulus diameter, E and A: mitral inflow E and A wave velocity measured by pulsed Doppler
Statistical analysis
All data obtained by 2DE or RT3DE were presented as mean ± SD. Data analysis was performed using statistical software (SPSS, Version 12.1, SPSS Inc, Chicago, USA). Independent sample t test was performed to compare between means of variables of groups to determine the statistical significance of difference. The level of significance was set to p < 0.05. In our department, an excellent correlation (r = 0.82, P < 0.0001) has been described between MAD3D and MRI measurements of MAD [5]. There was no significant difference between MAD3D and MADMRI. Similarly, there was no difference between MAA3D and MAAMRI.
Results
Clinical and 2D echocardiographic data
Clinical and echocardiographic data of NCCM patients and controls are shown in Tables 1 and 2. The presence and severity of mitral regurgitation were more frequent in NCCM patients than in control subjects. LV diameters were significantly increased, while LV-FS was significantly decreased in NCCM patients. The number of noncompacted segments was 5.4 ± 2.9 in NCCM patients, which did not show any correlation with any echocardiographic parameters.
RT3DE data
Acquisition and postprocessing of RT3DE data were performed successfully with clear delineation of the MA in all patients. Compared with control subjects, MAD3D and MAA3D were significantly larger, while LAEF3D-MAD and LAEF3D-MAA were significantly increased in NCCM patients (P < 0.05) (Table 2).
Discussion
Left atrial ejection force (LAEF), based on classic Newtonian mechanics, provides a physiological assessment of atrial systolic function and is a potentially useful index for assessing atrial contribution to diastolic performance. To the best of authors` knowledge this is the first time to demonstrate increased LAEF during RT3DE indicating high LA workload in NCCM patients. NCCM is known to be a relatively new clinicopathologic entity characterized by a pattern of prominent trabecular meshwork and deep intertrabecular recesses communicating with the LV cavity [1]. Results of recent studies confirmed the hypothesis that isolated ventricular noncompaction can be a part of a more widespread cardiomyopathy, involving both the morphologically normal and dysmorphic LV myocardial segments [6–9]. However, the pathophysiological mechanisms of LV dysfunction remained unclear and, moreover little is known about LA function in NCCM.
Manning et al. surmised that LAEF is equal to left ejection volume times acceleration of LA flow according to Newton’s law of motion (force equals mass times acceleration) [2]. Anwar et al. confirmed that RT3DE is a useful method for the evaluation of LAEF3D-MAA [3]. In recent studies MAA3D has been confirmed to be traced successfully with good interobserver agreement and comparable to magnetic resonance imaging [5]. RT3DE allowed exact ‘en-face’ measurement of MAA3D suggesting overstretching and dilatation in dilated [10], hypertrophic [3, 10] and noncompaction cardiomyopathy (present study). LAEF was higher in hypertrophic cardiomyopathy (HCM) patients compared with control subjects, with the highest value found in patients with obstructive HCM due to higher LV resistance [3]. LAEF3D-MAA calculated by the MAA3D-derived formula was higher in HCM patients than by the ‘mitral valve area’-derived formula either by 2D echocardiography or RT3DE [3].
In the present study, 41% of NCCM patients were in NYHA functional class II / III HF. Recently, Triposkiadis et al. demonstrated that in patients with HF, LAEF and LA kinetic energy are higher than in normal controls [11]. This is most likely due to LA dilation, which compensates for the depressed LA systolic shortening and increases LA active emptying volume and LA contribution to LV stroke volume, maintaining LV stroke volume and cardiac output [11, 12]. However, it should be noted that other authors found decreased LA kinetic energy in patients with advanced HF (NYHA functional class III HF) [13, 14]. It has been concluded that LA systolic failure contributes to the transition from moderate to advanced HF.
Limitations
During evaluation of LA systolic function, consideration of other factors affecting LAEF is important. According to recent findings, age considerably influences LAEF [15]. This fact could also affect our results, but no significant differences were found in age between NCCM patients and controls. LA systolic function is deteriorated in patients with sick sinus syndrome and in those with paroxysmal atrial fibrillation [16]. However, all of our patients were in sinus rhythm. Cioffi et al. demonstrated that LV geometry can also influence LA size and function [17]. The concentric LV pattern was associated with the greatest LA volumes and with the strongest LAEF, suggesting that chronic pressure overload more than volume overload stimulates the LA in increasing its workload. Left atrial dilation can be resulted from chronic mitral regurgitation, which can also affect LA systolic function. Another important limitation is that left atrial contraction produces both the forward blood flow toward the LV through the mitral valve and backward flow towards the pulmonary veins. Unfortunately, only the forward blood flow was examined during the present study.
Conclusions
LAEF is increased in NCCM patients compared to normal individuals. These results can suggest compensating left atrial work against the dysfunctional LV in NCCM patients. However, further studies are warranted evaluating LA function by RT3DE in patients with different stages of NCCM.
Abbreviations
- 2DE:
-
Two-dimensional echocardiography
- 3D:
-
Three-dimensional
- LA:
-
Left atrium
- LAEF:
-
Left atrial ejection force
- LV:
-
Left ventricle
- LV-EDD:
-
Left ventricular end-diastolic diameter
- LV-ESD:
-
Left ventricular end-systolic diameter
- MA:
-
Mitral annulus
- MAA:
-
Mitral annulus area
- MAD:
-
Mitral annulus diameter
- MRI:
-
Magnetic resonance imaging
- NCCM:
-
Noncompaction cardiomyopathy
- RT3DE:
-
Real-time three-dimensional echocardiography
- V:
-
Peak velocity of A wave
References
Chin TK, Perloff JK, Williams RG, Jue K, Mohrmann R (1990) Isolated noncompaction of left ventricular myocardium. A study of eight cases. Circulation 82:507–513
Manning WJ, Silverman DI, Katz SE, Douglas PS (1993) Atrial ejection force: a noninvasive assessment of atrial systolic function. J Am Coll Cardiol 22:221–225
Anwar AM, Soliman OI, Geleijnse ML, Michels M, Vletter WB, Nemes A et al (2007) Assessment of left atrial ejection force in hypertrophic cardiomyopathy using real-time three-dimensional echocardiography. J Am Soc Echocardiogr 20:744–748
Jenni R, Oechslin E, Schneider J, Attenhofer Jost C, Kaufmann PA (2001) Echocardiographic and pathoanatomical characteristics of isolated left ventricular non-compaction: a step towards classification as a distinct cardiomyopathy. Heart 86:666–671
Anwar AM, Soliman OI, Ten Cate FJ, Nemes A, McGhie JS, Krenning BJ, et al (2007) True mitral annulus diameter is underestimated by two-dimensional echocardiography as evidenced by real-time three-dimensional echocardiography and magnetic resonance imaging. Int J Cardiovasc Imaging (in press)
Lofiego C, Biagini E, Ferlito M, Pasquale F, Rocchi G, Perugini E et al (2006) Paradoxical contributions of non-compacted and compacted segments to global left ventricular dysfunction in isolated left ventricular noncompaction. Am J Cardiol 97:738–741
Sengupta PP, Mohan JC, Mehta V, Jain V, Arora R, Pandian NG et al (2004) Comparison of echocardiographic features of noncompaction of the left ventricle in adults versus idiopathic dilated cardiomyopathy in adults. Am J Cardiol 94:389–391
Jenni R, Wyss CA, Oechslin EN, Kaufmann PA (2002) Isolated ventricular noncompaction is associated with coronary microcirculatory dysfunction. J Am Coll Cardiol 39:450–454
Oechslin EN, Attenhofer Jost CH, Rojas JR, Kaufmann PA, Jenni R (2000) Long-term follow-up of 34 adults with isolated left ventricular noncompaction: a distinct cardiomyopathy with poor prognosis. J Am Coll Cardiol 36:493–500
Anwar AM, Soliman OI, Nemes A, Germans T, Krenning BJ, Geleijnse ML, et al (2007) Assessment of mitral annulus size and function by real-time three-dimensional echocardiography in cardiomyopathy: comparison with magnetic resonance imaging. J Am Soc Echocardiogr 20:941–948
Triposkiadis F, Harbas C, Sitafidis G, Skoularigis J, Demopoulos V, Kelepeshis G (2007) Echocardiographic assessment of left atrial ejection force and kinetic energy in chronic heart failure. Int J Cardiovasc Imag (in press)
Linderer T, Chatterjee K, Parmley WW, Sievers RE, Glantz SA, Tyberg JV (1983) Influence of atrial systole on the Frank-Starling relation and the end-diastolic pressure-diameter relation of the left ventricle. Circulation 67:1045–1053
Stefanadis C, Dernellis J, Lambrou S, Toutouzas P (1998) Left atrial energy in normal subjects, in patients with symptomatic mitral stenosis, and in patients with advanced heart failure. Am J Cardiol 82:1220–1223
Dernellis JM, Panaretou MP (2003) Effects of digoxin on left atrial function in heart failure. Heart 89:1308–1315
Mattioli AV, Tarabini CE, Vivoli D, Molinari R, Mattioli G (1995) Atrial ejection force: findings in healthy subjects. Cardiologia 40:341–345
Tokushima T, Utsunomiya T, Yoshida K, Kido K, Ogawa T, Ryu T et al (2000) Left atrial systolic function assessed by left atrial ejection force in patients with sick sinus syndrome and paroxysmal atrial fibrillation. Jpn Heart J 41: 723–732
Cioffi G, Stefenelli C (2002) Comparison of left ventricular geometry and left atrial size and function in patients with aortic stenosis versus those with pure aortic regurgitation. Am J Cardiol 90:601–606
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License ( https://creativecommons.org/licenses/by-nc/2.0 ), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Nemes, A., Anwar, A.M., Caliskan, K. et al. Evaluation of left atrial systolic function in noncompaction cardiomyopathy by real-time three-dimensional echocardiography. Int J Cardiovasc Imaging 24, 237–242 (2008). https://doi.org/10.1007/s10554-007-9261-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-007-9261-5