Abstract
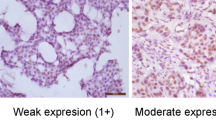
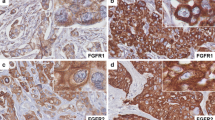
Perturbations of transforming growth factor-beta (TGF-β) signaling are pivotal to tumorigenesis and tumor progression through their effects on cell proliferation and cell invasion. This study aims to evaluate the association of TGF-βRII and pSmad2 protein expressions in breast tissue with clinicopathological factors and prognosis of breast cancer. Expression of the TGF-βRII and pSmad2 proteins was assessed in breast tissue of 1,045 breast cancer cases in the Shanghai Breast Cancer Study using a double immunofluorescence staining method, which was validated with standard single immunostains. TGF-βRII expression intensity was positively associated with younger age at diagnosis (P = 0.03), pre-menopausal status (P = 0.03), and lower TNM stage (P = 0.04). Cytoplasmic predominant expression pattern of TGF-βRII was associated with older age at diagnosis (P = 0.04) and invasive histological type (P = 0.03). Increased pSmad2 expression was associated with higher breast cancer grade (P < 0.01). Higher pSmad2 expression [HR (95 % CI):1.48 (1.07–2.04), P = 0.02] and cytoplasmic predominant TGF-βRII expression [HR (95 % CI): 1.80 (1.08–3.00), P = 0.02] were significantly associated with reduced cancer-free survival. Our data suggest that TGF-βRII and pSmad2 expressions are associated with certain clinical and pathologic features of breast cancer. A cytoplasmic predominant TGF-βRII expression pattern and a higher pSmad2 expression were associated with decreased breast cancer survival. Our study provides additional evidence to support the important role of TGF-β signaling in breast cancer prognosis.



Similar content being viewed by others
Abbreviations
- BMI:
-
Body mass index
- CI:
-
Confidence interval
- DFS:
-
Disease-free survival
- ER:
-
Estrogen receptor
- HER2:
-
Human epidermal growth factor receptor 2
- HR:
-
Hazard ratio
- PR:
-
Progesterone receptor
- pSmad2:
-
Phosphorylated Smad2
- SBCS:
-
Shanghai Breast Cancer Study
- TGF-β:
-
Transforming growth factor-beta
- TGF-βRI:
-
Transforming growth factor-beta receptor I
- TGF-βRII:
-
Transforming growth factor-beta receptor II
- TMA:
-
Tissue microarray
References
Ikushima H, Miyazono K (2010) TGFbeta signalling: a complex web in cancer progression. Nat Rev Cancer 10:415–424
Massague J (2012) TGFbeta signalling in context. Nat Rev Mol Cell Biol 13:616–630
Tsuchida K, Lewis KA, Mathews LS, Vale WW (1993) Molecular characterization of rat transforming growth factor-beta type II receptor. Biochem. Biophys. Res Commun 191:790–795
Takumi T, Moustakas A, Lin HY, Lodish HF (1995) Molecular characterization of a type I serine-threonine kinase receptor for TGF-beta and activin in the rat pituitary tumor cell line GH3. Exp Cell Res 216:208–214
Feng XH, Derynck R (2005) Specificity and versatility in tgf-beta signaling through Smads. Annu Rev Cell Dev Biol 21:659–693
Massague J, Blain SW, Lo RS (2000) TGFbeta signaling in growth control, cancer, and heritable disorders. Cell 103:295–309
Massague J (1998) TGF-beta signal transduction. Annu Rev Biochem 67:753–791
Wrana JL, Attisano L, Carcamo J, Zentella A, Doody J, Laiho M, Wang XF, Massague J (1992) TGF beta signals through a heteromeric protein kinase receptor complex. Cell 71:1003–1014
Chowdhury S, Ammanamanchi S, Howell GM (2009) Epigenetic targeting of transforming growth factor beta receptor II and implications for cancer therapy. Mol Cell Pharmacol 1:57–70
Grady WM, Myeroff LL, Swinler SE, Rajput A, Thiagalingam S, Lutterbaugh JD, Neumann A, Brattain MG, Chang J, Kim SJ, Kinzler KW, Vogelstein B, Willson JK, Markowitz S (1999) Mutational inactivation of transforming growth factor beta receptor type II in microsatellite stable colon cancers. Cancer Res 59:320–324
Markowitz S, Wang J, Myeroff L, Parsons R, Sun L, Lutterbaugh J, Fan RS, Zborowska E, Kinzler KW, Vogelstein B et al (1995) Inactivation of the type II TGF-beta receptor in colon cancer cells with microsatellite instability. Science 268:1336–1338
Izumoto S, Arita N, Ohnishi T, Hiraga S, Taki T, Tomita N, Ohue M, Hayakawa T (1997) Microsatellite instability and mutated type II transforming growth factor-beta receptor gene in gliomas. Cancer Lett 112:251–256
Macias-Silva M, Abdollah S, Hoodless PA, Pirone R, Attisano L, Wrana JL (1996) MADR2 is a substrate of the TGFbeta receptor and its phosphorylation is required for nuclear accumulation and signaling. Cell 87:1215–1224
Nakao A, Imamura T, Souchelnytskyi S, Kawabata M, Ishisaki A, Oeda E, Tamaki K, Hanai J, Heldin CH, Miyazono K, ten Dijke P (1997) TGF-beta receptor-mediated signalling through Smad2, Smad3 and Smad4. EMBO J 16:5353–5362
Shepherd RD, Kos SM, Rinker KD (2011) Flow-dependent Smad2 phosphorylation and TGIF nuclear localization in human aortic endothelial cells. Am J Physiol Heart Circ Physiol 301:H98–H107
Wu G, Chen YG, Ozdamar B, Gyuricza CA, Chong PA, Wrana JL, Massague J, Shi Y (2000) Structural basis of Smad2 recognition by the Smad anchor for receptor activation. Science 287:92–97
Wu JW, Hu M, Chai J, Seoane J, Huse M, Li C, Rigotti DJ, Kyin S, Muir TW, Fairman R, Massague J, Shi Y (2001) Crystal structure of a phosphorylated Smad2. Recognition of phosphoserine by the MH2 domain and insights on Smad function in TGF-beta signaling. Mol Cell 8:1277–1289
Inman GJ, Nicolas FJ, Hill CS (2002) Nucleocytoplasmic shuttling of Smads 2, 3, and 4 permits sensing of TGF-beta receptor activity. Mol Cell 10:283–294
Grau AM, Wen W, Ramroopsingh DS, Gao YT, Zi J, Cai Q, Shu XO, Zheng W (2008) Circulating transforming growth factor-beta-1 and breast cancer prognosis: results from the Shanghai Breast Cancer Study. Breast Cancer Res Treat 112:335–341
Zheng W (2009) Genetic polymorphisms in the transforming growth factor-beta signaling pathways and breast cancer risk and survival. Methods Mol Biol 472:265–277
Gao YT, Shu XO, Dai Q, Potter JD, Brinton LA, Wen W, Sellers TA, Kushi LH, Ruan Z, Bostick RM, Jin F, Zheng W (2000) Association of menstrual and reproductive factors with breast cancer risk: results from the Shanghai Breast Cancer Study. Int J Cancer 87:295–300
Zheng W, Long J, Gao YT, Li C, Zheng Y, Xiang YB, Wen W, Levy S, Deming SL, Haines JL, Gu K, Fair AM, Cai Q, Lu W, Shu XO (2009) Genome-wide association study identifies a new breast cancer susceptibility locus at 6q25.1. Nat Genet 41:324–328
Su Y, Zheng Y, Zheng W, Gu K, Chen Z, Li G, Cai Q, Lu W, Shu XO (2011) Distinct distribution and prognostic significance of molecular subtypes of breast cancer in Chinese women: a population-based cohort study. BMC Cancer 11:292
Lakhani S, Ellis I, Schnitt S, Tan P, van de Vijver M (2012) WHO classification of tumours of breast. International Agency for Research on Cancer, France
Mohsin SK, Weiss H, Havighurst T, Clark GM, Berardo M, Roanh lD, To TV, Qian Z, Love RR, Allred DC (2004) Progesterone receptor by immunohistochemistry and clinical outcome in breast cancer: a validation study. Mod Pathol 17:1545–1554
Zhang X, Loberiza FR, Klein JP, Zhang MJ (2007) A SAS macro for estimation of direct adjusted survival curves based on a stratified Cox regression model. Comput Methods Programs Biomed 88:95–101
Koli KM, Arteaga CL (1997) Predominant cytosolic localization of type II transforming growth factor beta receptors in human breast carcinoma cells. Cancer Res 57:970–977
Ewan KB, Shyamala G, Ravani SA, Tang Y, Akhurst R, Wakefield L, Barcellos-Hoff MH (2002) Latent transforming growth factor-beta activation in mammary gland: regulation by ovarian hormones affects ductal and alveolar proliferation. Am J Pathol 160:2081–2093
Derynck R, Akhurst RJ, Balmain A (2001) TGF-beta signaling in tumor suppression and cancer progression. Nat Genet 29:117–129
Massague J, Gomis RR (2006) The logic of TGFbeta signaling. FEBS Lett 580:2811–2820
Buck MB, Fritz P, Dippon J, Zugmaier G, Knabbe C (2004) Prognostic significance of transforming growth factor beta receptor II in estrogen receptor-negative breast cancer patients. Clin Cancer Res 10:491–498
Gobbi H, Arteaga CL, Jensen RA, Simpson JF, Dupont WD, Olson SJ, Schuyler PA, Plummer WD Jr, Page DL (2000) Loss of expression of transforming growth factor beta type II receptor correlates with high tumour grade in human breast in situ and invasive carcinomas. Histopathology 36:168–177
Paiva CE, Drigo SA, Rosa FE, Moraes Neto FA, Caldeira JR, Soares FA, Domingues MA, Rogatto SR (2010) Absence of transforming growth factor-beta type II receptor is associated with poorer prognosis in HER2-negative breast tumours. Ann Oncol 21:734–740
Figueroa JD, Flanders KC, Garcia-Closas M, Anderson WF, Yang XR, Matsuno RK, Duggan MA, Pfeiffer RM, Ooshima A, Cornelison R, Gierach GL, Brinton LA, Lissowska J, Peplonska B, Wakefield LM, Sherman ME (2010) Expression of TGF-beta signaling factors in invasive breast cancers: relationships with age at diagnosis and tumor characteristics. Breast Cancer Res Treat 121:727–735
Acknowledgments
The authors thank study participants and research staff for their contributions and commitment to this project. We thank Regina Courtney for technical assistance and Jacqueline Stern for assistance with editing and manuscript preparation. The immunofluorescence staining was performed at the Survey and Biospecimen Shared Resource, which is supported in part by the Vanderbilt-Ingram Cancer Center (P30CA068485). This research was supported by research grants from the National Institutes of health (R01CA064277, R01CA090899, R01CA118229, and R01CA122756).
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standards
All data collection was conducted with approval of appropriate institutional review boards to protect human subjects with consent and data protection systems in place. Data analysis for this manuscript was conducted on de-identified data sets.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Qiu, Q., Su, Y., Zheng, Y. et al. Increased pSmad2 expression and cytoplasmic predominant presence of TGF-βRII in breast cancer tissue are associated with poor prognosis: results from the Shanghai Breast Cancer Study. Breast Cancer Res Treat 149, 467–477 (2015). https://doi.org/10.1007/s10549-014-3251-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-014-3251-9