Abstract
Background
Cerebrotendinous xanthomatosis (CTX) is an autosomal recessive lipid storage disorder characterized by a heterogeneous presentation and a broad spectrum of clinical manifestations. Since early diagnosis and replacement therapy with chenodeoxycholic acid can prevent clinical deterioration, our aim was to develop a diagnostic tool to identify and treat CTX patients at an initial stage of the disease.
Methods
We devised a suspicion index, composed of weighted scores assigned to indicators such as family history characteristics and common systemic and neurological features, on the basis of a pooled analysis of selected international CTX series. The indicators were classified as very strong (score 100), strong (50) or moderate (25). The suspicion index was then applied retrospectively to our CTX population.
Results
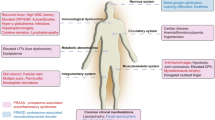
Early systemic signs such as cataract, diarrhea and neonatal cholestatic jaundice were considered strong indicators, together with neurological features such as intellectual impairment, psychiatric disturbances, ataxia, spastic paraparesis and dentate nuclei abnormalities at MRI. Tendon xanthomas were regarded as very strong indicators, as was an affected sibling. A total score ≥ 100 warranted serum cholestanol assessment. Elevated cholestanol or a total score ≥ 200, with one very strong or four strong indicators, warranted CYP27A1 gene analysis. In our patients, age at diagnosis was 35.5 ± 11.8 years (mean ± standard deviation), whereas with the diagnostic tool it became 10.6 ± 9.8 years (p < 0.01).
Conclusions
Our suspicion index provides a simple and inexpensive diagnostic tool allowing diagnosis and treatment of CTX before neurological disability occurs.




Similar content being viewed by others
References
Barkhof F, Verrips A, Wesseling P et al (2000) Cerebrotendinous xanthomatosis: the spectrum of imaging findings and the correlation with neuropathologic findings. Radiology 217:869–876
Batta AK, Shefer S, Batta M, Salen G (1985) Effect of chenodeoxycholic acid on biliary and urinary bile acids and bile alcohols in cerebrotendinous xanthomatosis; monitoring by high performance liquid chromatography. J Lipid Res 26:690–698
Berginer VM, Salen G, Shefer S (1984) Long-term treatment of cerebrotendinous xanthomatosis with chenodeoxycholic acid. N Engl J Med 311:1649–1652
Berginer VM, Shany S, Alkalay D et al (1993) Osteoporosis and increased bone fractures in cerebrotendinous xanthomatosis. Metabolism 42:69–74
Berginer VM, Gross B, Morad K et al (2009) Chronic diarrhea and juvenile cataracts: think cerebrotendinous xanthomatosis and treat. Pediatrics 123:143–147
Björkhem I, Hansson M (2010) Cerebrotendinous xanthomatosis: an inborn error in bile acid synthesis with defined mutations but still a challenge. Biochem Biophys Res Commun 396:46–49
Cali JJ, Russell DW (1991) Characterization of human sterol 27-hydroxylase. A mitochondrial cytochrome P-450 that catalyzes multiple oxidation reaction in bile acid biosynthesis. J Biol Chem 266:7774–7778
Clayton PT, Verrips A, Sistermans E, Mann A, Mieli-Vergani G, Wevers R (2002) Mutations in the sterol 27-hydroxylase gene (CYP27A) cause hepatitis of infancy as well as cerebrotendinous xanthomatosis. J Inherit Metab Dis 25:501–513
Cruysberg JR (2009) Children with cataract and chronic diarrhoea: cerebrotendinous xanthomatosis. J Inherit Metab Dis 32:309
Cruysberg JR, Wevers RA, Tolboom JJ (1991) Juvenile cataract associated with chronic diarrhea in pediatric cerebrotendinous xanthomatosis. Am J Ophthalmol 112:606–607
De Stefano N, Dotti MT, Mortilla M, Federico A (2001) Magnetic resonance imaging and spectroscopic changes in brains of patients with cerebrotendinous xanthomatosis. Brain 124:121–131
Federico A, Dotti MT (1996) Cerebrotendinous xanthomatosis. In: Moser HW (ed) Handbook of Clinical Neurology 22:599–613
Federico A, Dotti MT (2003) Cerebrotendinous xanthomatosis: clinical manifestations, diagnostic criteria, pathogenesis, and therapy. J Child Neurol 18:633–638
Fraidakis MJ (2013) Psychiatric manifestations in cerebrotendinous xanthomatosis. Transl Psychiatry 3:e302. doi:10.1038/tp.2013.76
Ginanneschi F, Mignarri A, Mondelli M et al (2013) Polyneuropathy in cerebrotendinous xanthomatosis and response to treatment with chenodeoxycholic acid. J Neurol 260:268–274
Koopman BJ, Wolthers BG, van der Molen JC, Waterreus RJ (1985) Bile acid therapies applied to patients suffering from cerebrotendinous xanthomatosis. Clin Chim Acta 152:115–122
Lee MH, Hazard S, Carpten JD et al (2001) Fine-mapping, mutation analyses, and structural mapping of cerebrotendinous xanthomatosis in U.S. pedigrees. J Lipid Res 42:159–169
Lorincz MT, Rainier S, Thomas D, Fink JK (2005) Cerebrotendinous xanthomatosis: possible higher prevalence than previously recognized. Arch Neurol 62:1459–1463
Martini G, Mignarri A, Ruvio M et al (2013) Long-term bone density evaluation in cerebrotendinous xanthomatosis: evidence of improvement after chenodeoxycholic acid treatment. Calcif Tissue Int 92:282–286
Mignarri A, Rossi S, Ballerini M et al (2011) Clinical relevance and neurophysiological correlates of spasticity in cerebrotendinous xanthomatosis. J Neurol 258:783–790
Mignarri A, Dotti MT, Del Puppo M et al (2012a) Cerebrotendinous xanthomatosis with progressive cerebellar vacuolation: six-year MRI follow-up. Neuroradiology 54:649–651
Mignarri A, Falcini M, Vella A et al (2012b) Parkinsonism as neurological presentation of late-onset cerebrotendinous xanthomatosis. Parkinsonism Relat Disord 18:99–101
Nakamura T, Matsuzawa Y, Takemura K, Kubo M, Miki H, Tarui S (1991) Combined treatment with chenodeoxycholic acid and pravastatin improves plasma cholestanol levels associated with marked regression of tendon xanthomas in cerebrotendinous xanthomatosis. Metabolism 40:741–746
Pierre G, Setchell K, Blyth J, Preece MA, Chakrapani A, McKiernan P (2008) Prospective treatment of cerebrotendinous xanthomatosis with cholic acid therapy. J Inherit Metab Dis 31:S241–S245
Pilo de la Fuente B, Ruiz I, Lopez de Munain A, Jimenez-Escrig A (2008) Cerebrotendinous xanthomatosis: neuropathological findings. J Neurol 255:839–842
Pilo de la Fuente B, Jimenez-Escrig A, Lorenzo JR et al (2011a) Cerebrotendinous xanthomatosis in Spain: clinical, prognostic, and genetic survey. Eur J Neurol 18:1203–1211
Pilo de la Fuente B, Sobrido MJ, Girós M et al (2011b) Usefulness of cholestanol levels in the diagnosis and follow-up of patients with cerebrotendinous xanthomatosis. Neurologia 26:397–404
Pilo B, de Blas G, Sobrido MJ et al (2011) Neurophysiological study in cerebrotendinous xanthomatosis. Muscle Nerve 43:531–536
Rubio-Agusti I, Kojovic M, Edwards MJ et al (2012) Atypical parkinsonism and cerebrotendinous xanthomatosis: report of a family with corticobasal syndrome and a literature review. Mov Disord 27:1769–1774
Salen G, Berginer V, Shore V et al (1987) Increased concentrations of cholestanol and apolipoprotein B in the cerebrospinal fluid of patients with cerebrotendinous xanthomatosis. Effect of chenodeoxycholic acid. N Engl J Med 316:1233–1238
Salen G, Batta AK, Tint GS, Shefer S (1994) Comparative effects of lovastatin and chenodeoxycholic acid on plasma cholestanol levels and abnormal bile acid metabolism in cerebrotendinous xanthomatosis. Metabolism 43:1018–1022
Samenuk P, Koffman BM (2001) Chenodeoxycholic treatment of cerebrotendinous xanthomatosis. Neurology 56:695–696
Siman-Tov T, Meiner V, Gadoth N (2006) Could steroids mask the diagnosis of cerebrotendinous xanthomatosis? J Neurol Sci 243:83–86
Su CS, Chang WN, Huang SH et al (2010) Cerebrotendinous xanthomatosis patients with and without parkinsonism: clinical characteristics and neuroimaging findings. Mov Disord 25:452–458
Van Heijst AF, Verrips A, Wevers RA, Cruysberg JR, Renier WO, Tolboom JJ (1998) Treatment and follow-up of children with cerebrotendinous xanthomatosis. Eur J Pediatr 157:313–316
Verrips A, Wevers RA, Van Engelen BG et al (1999) Effect of simvastatin in addition to chenodeoxycholic acid in patients with cerebrotendinous xanthomatosis. Metabolism 48:233–238
Verrips A, Hoefsloot LH, Steenbergen GC et al (2000a) Clinical and molecular genetic characteristics of patients with cerebrotendinous xanthomatosis. Brain 23:908–919
Verrips A, van Engelen BG, Wevers RA et al (2000b) Presence of diarrhea and absence of tendon xanthomas in patients with cerebrotendinous xanthomatosis. Arch Neurol 57:520–524
von Bahr S, Björkhem I, Van’t Hooft F et al (2005) Mutation in the sterol 27-hydroxylase gene associated with fatal cholestasis in infancy. J Pediatr Gastroenterol Nutr 40:481–486
Yahalom G, Tsabari R, Molshatzki N, Ephraty L, Cohen H, Hassin-Baer S (2013) Neurological outcome in cerebrotendinous xanthomatosis treated with chenodeoxycholic Acid: early versus late diagnosis. Clin Neuropharmacol 36:78–83
Acknowledgments
We thank Marina Del Puppo for serum cholestanol assessment, Federica Ginanneschi for statistical analysis, and all patients and families, as well as referring physicians.
Conflict of interest
None.
Funding
Andrea Mignarri, Gian Nicola Gallus, Maria Teresa Dotti and Antonio Federico declare no funding.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by: Ronald J.A. Wanders
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 111 kb)
Rights and permissions
About this article
Cite this article
Mignarri, A., Gallus, G.N., Dotti, M.T. et al. A suspicion index for early diagnosis and treatment of cerebrotendinous xanthomatosis. J Inherit Metab Dis 37, 421–429 (2014). https://doi.org/10.1007/s10545-013-9674-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10545-013-9674-3