Abstract
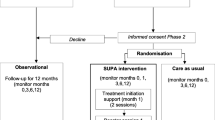
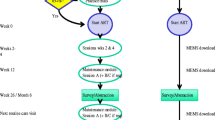
Concerns that standard didactic adherence counselling may be inadequate to maximise antiretroviral therapy (ART) adherence led us to evaluate more intensive individualised motivational adherence counselling. We randomised 297 HIV-positive ART-naïve patients in Durban, South Africa, to receive either didactic counselling, prior to ART initiation (n = 150), or an intensive motivational adherence intervention after initiating ART (n = 147). Study arms were similar for age (mean 35.8 years), sex (43.1 % male), CD4+ cell count (median 121.5 cells/μl) and viral load (median 119,000 copies/ml). Virologic suppression at 9 months was achieved in 89.8 % of didactic and 87.9 % of motivational counselling participants (risk ratio [RR] 0.98, 95 % confidence interval [CI] 0.90–1.07, p = 0.62). 82.9 % of didactic and 79.5 % of motivational counselling participants achieved >95 % adherence by pill count at 6 months (RR 0.96, 95 % CI 0.85–1.09, p = 0.51). Participants receiving intensive motivational counselling did not achieve higher treatment adherence or virological suppression than those receiving routinely provided didactic adherence counselling. These data are reassuring that less resource intensive didactic counselling was adequate for excellent treatment outcomes in this setting.
Resumen
La inquietud de que la terapia didáctica de adherencia estándar pudiera ser inadecuada para maximizar la adherencia al tratamiento antiretroviral (ART), nos llevó a evaluar la terapia motivacional individualizada. Aleatorizamos 297 pacientes HIV-positivos sin ART previo en Durban, Sudáfrica, para recibir, ya sea terapia didáctica antes del inicio del ART (n = 150), o terapia motivacional intensiva después de iniciado el ART (n = 147). Los brazos del estudio fueron similares en edad (promedio 35.8 años), sexo (43.1 % hombres), recuento de células CD4+ (mediana 121.5 células/μl) y carga viral (mediana 119,000 copias/ml). La supresión virológica a los nueves meses se logró en el 89.8 % de los participantes que recibieron terapia didáctica y en 87.9 % de aquellos en terapia motivacional (riesgo relativo [RR] 0.98, 95 % intervalo de confianza [CI] 0.90–1.07, p = 0.62). 82.9 % de los participantes bajo terapia didáctica y 79.5 % de los tratados con terapia motivacional alcanzaron >95 % de adherencia por cuenta de píldoras a los seis meses (RR 0.96, 95 % CI 0.85–1.09, p = 0.51). Los participantes que recibieron terapia motivacional intensiva no mostraron una mayor adherencia al tratamiento o supresión virológica que aquellos bajo terapia didáctica rutinaria. Estos resultados son tranquilizadores ya que muestran que la menos costosa terapia didáctica es adecuada en este escenario.


Similar content being viewed by others
Notes
We refer to patients in the treatment programme, and to participants when enrolled onto this study.
References
UNAIDS. AIDS epidemic update : november 2009. Geneva: WHO; 2009.
Nachega JB, Hislop M, Dowdy DW, Lo M, Omer SB, Regensberg L, et al. Adherence to highly active antiretroviral therapy assessed by pharmacy claims predicts survival in HIV-infected South African adults. J Acquir Immune Defic Syndr. 2006;43(1):78–84.
Broder S. The development of antiretroviral therapy and its impact on the HIV-1/AIDS pandemic. Antivir Res. 2010;85(1):1–18.
Jones R, Gazzard B. The cost of antiretroviral drugs and influence on prescribing policies. Int J STD AIDS. 2006;17(8):499–506.
Orrell C. Antiretroviral adherence in a resource-poor setting. Curr HIV/AIDS Rep. 2005;2(4):171–6.
Paterson DL, Swindells S, Mohr J, Brester M, Vergis EN, Squier C, et al. Adherence to protease inhibitor therapy and outcomes in patients with HIV infection. Ann Intern Med. 2000;133(1):21–30.
Simoni JM, Pearson CR, Pantalone DW, Marks G, Crepaz N. Efficacy of interventions in improving highly active antiretroviral therapy adherence and HIV-1 RNA viral load. A meta-analytic review of randomized controlled trials. J Acquir Immune Defic Syndr. 2006;43(1):S23–35.
Abdool Karim SS, Abdool Karim Q, Friedland G, Lalloo U, El-Sadr WM. Implementing antiretroviral therapy in resource-constrained settings: opportunities and challenges in integrating HIV and tuberculosis care. AIDS. 2004;18(7):975–9.
Shisana O, Simbayi L, editors. Nelson Mandela/HSRC Study of HIV/AIDS. South African national HIV prevalence, behavioural risks and mass media. Household survey 2002. Cape Town: Human Sciences Research Council; 2002.
Ammassari A, Trotta MP, Murri R, Castelli F, Narciso P, Noto P, et al. Correlates and predictors of adherence to highly active antiretroviral therapy: overview of published literature. J Acquir Immune Defic Syndr. 2002;31(3):S123–7.
Simoni JM, Frick PA, Pantalone DW, Turner BJ. Antiretroviral adherence interventions: a review of current literature and ongoing studies. Top HIV Med. 2003;11(6):185–98.
Amico KR, Harman JJ, Johnson BT. Efficacy of antiretroviral therapy adherence interventions: a research synthesis of trials, 1996 to 2004. J Acquir Immune Defic Syndr. 2006;41(3):285–97.
Gordon CM. Commentary on meta-analysis of randomized controlled trials for HIV treatment adherence interventions: research directions and implications for practice. J Acquir Immune Defic Syndr. 2006;43(1):S36–40.
Mannheimer SB, Morse E, Matts JP, Andrews L, Child C, Schmetter B, et al. Sustained benefit from a long-term antiretroviral adherence intervention: results of a large randomized clinical trial. J Acquir Immune Defic Syndr. 2006;43(1):S41–7.
Cote JK, Godin G. Efficacy of interventions in improving adherence to antiretroviral therapy. Int J STD AIDS. 2005;16(5):335–43.
Simoni JM, Amico KR, Pearson CR, Malow R. Strategies for promoting adherence to antiretroviral therapy: a review of the literature. Curr Infect Dis Rep. 2008;10(6):515–21.
DiIorio C, McCarty F, Resnicow K, McDonnell Holstad M, Soet J, Yeager K, et al. Using motivational interviewing to promote adherence to antiretroviral medications: a randomized controlled study. AIDS Care. 2008;20(3):273–83.
Davies G, Koenig LJ, Stratford D, Palmore M, Bush T, Golde M, et al. Overview and implementation of an intervention to prevent adherence failure among HIV-infected adults initiating antiretroviral therapy: lessons learned from Project HEART. AIDS Care. 2006;18(8):895–903.
Koenig LJ, Pals SL, Bush T, Pratt Palmore M, Stratford D, Ellerbrock TV. Randomized controlled trial of an intervention to prevent adherence failure among HIV-infected patients initiating antiretroviral therapy. Health Psychol. 2008;27(2):159–69.
Abdool Karim SS, Naidoo K, Grobler A, Padayatchi N, Baxter C, Gray A, et al. Timing of initiation of antiretroviral drugs during tuberculosis therapy. N Engl J Med. 2010;362(8):697–706.
Abdool Karim SS, Naidoo K, Grobler A, Padayatchi N, Baxter C, Gray AL, et al. Integration of antiretroviral therapy with tuberculosis treatment. N Engl J med. 2011;365(16):1492–501.
Department of Health. National antiretroviral treatment guideliness. Pretoria: National Department of Health; 2004.
WHO. Scaling up antiretroviral therapy in resource-limited settings: treatment guidelines for a public health approach (2003 revision). Geneva: World Health Organization; 2004.
DHHS. Guidelines for the use of antiretroviral agents in hiv-1-infected adults and adolescents. Washington: DHHS; 2004.
Fisher J, Fisher W, Bryan A, Misovich S. Information-motivation-behavioural skills model-based HIV risk behaviour change interventions for inner city high school youth. Health Psychol. 2002;21(2):177–86.
Fisher JD, Fisher WA. The information-motivation-behavioural skills model. In: DiClemente RJ, Crosby RA, Kegler MC, editors. Emerging theories in health promotion practice and research. San Francisco: Jossey-Bass; 2002. p. 40–70.
Fisher JD, Fisher WA, Amico KR, Harman JJ. An information-motivation-behavioral skills model of adherence to antiretroviral therapy. Health Psychol. 2006;25(4):462–73.
Fisher JD, Fisher WA, Cornman DH, Amico RK, Bryan A, Friedland GH. Clinician-delivered intervention during routine clinical care reduces unprotected sexual behavior among HIV-infected patients. J Acquir Immune Defic Syndr. 2006;41(1):44–52.
Rollnick S, Butler CC, McCambridge J, Kinnersley P, Elwyn G, Resnicow K. Consultations about changing behaviour. BMJ. 2005;331(7522):961–3.
Emmons KM, Rollnick S. Motivational interviewing in health care settings. Opportunities and limitations. Am J Prev Med. 2001;20(1):68–74.
Rubak S, Sandbaek A, Lauritzen T, Christensen B. Motivational interviewing: a systematic review and meta-analysis. Br J Gen Pract. 2005;55(513):305–12.
Lawn SD, Harries AD, Anglaret X, Myer L, Wood R. Early mortality among adults accessing antiretroviral treatment programmes in sub-Saharan Africa. AIDS. 2008;22(15):1897–908.
Lawn SD, Little F, Bekker LG, Kaplan R, Campbel E, Orrell C, et al. Changing mortality risk associated with CD4 cell response to antiretroviral therapy in South Africa. AIDS. 2009;23(3):335–42.
Zhang J, Yu KF. What’s the relative risk? A method of correcting the odds ratio in cohort studies of common outcomes. JAMA. 1998;280(19):1690–1.
Zou G. A modified poisson regression approach to prospective studies with binary data. Am J Epidemiol. 2004;159(7):702–6.
Barth RE, van der Meer JT, Hoepelman AI, Schrooders PA, van de Vijver DA, Geelen SP, et al. Effectiveness of highly active antiretroviral therapy administered by general practitioners in rural South Africa. Eur J Clin Microbiol Infect Dis. 2008;27(10):977–84.
Nachega JB, Hislop M, Nguyen H, Dowdy DW, Chaisson RE, Regensberg L, et al. Antiretroviral therapy adherence, virologic and immunologic outcomes in adolescents compared with adults in southern Africa. J Acquir Immune Defic Syndr. 2009;51(1):65–71.
Mutevedzi PC, Lessells RJ, Heller T, Barnighausen T, Cooke GS, Newell ML. Scale-up of a decentralized HIV treatment programme in rural KwaZulu-Natal, South Africa: does rapid expansion affect patient outcomes? Bull World Health Organ. 2010;88(8):593–600.
McCarney R, Warner J, Iliffe S, van Haselen R, Griffin M, Fisher P. The Hawthorne Effect: a randomised, controlled trial. BMC Med Res Methodol. 2007;7:30.
Simoni JM, Amico KR, Smith L, Nelson K. Antiretroviral adherence interventions: translating research findings to the real world clinic. Curr HIV/AIDS Rep. 2010;7(1):44–51.
Acknowledgements
This research was supported by the Doris Duke Charitable Foundation-funded Operations Research on AIDS Care and Treatment in Africa (ORACTA) Programme (Grant # 2005058). The Association of Commonwealth Universities funded PhD study for Francois van Loggerenberg at London School of Hygiene and Tropical Medicine. He was also supported by the Columbia University-Southern African Fogarty AIDS International Training and Research Programme (AITRP) funded by the Fogarty International Center, National Institutes of Health (Grant #D43TW00231). The National Institute of Allergy and infectious Disease (NIAID), National Institutes of Health (NIH) (Grant# AI51794) funded the infrastructure for this research. Alison Grant was supported by a Public Health Career Scientist award from the UK Department of Health. We would like to thank the clinic research support staff who provided the data collection, nursing services, as well as the administrative and counselling support for CAPRISA 058 study, Senzo Hlathi, Goodness Gumede, and Thandi Shezi. Dr Leila Mansoor provided advice and assisted with the training of the clinic counselling staff. Lise Werner, Anneke Grobler and Nonhlanhla Yende provided additional statistical guidance and support. Jayraj Ramota was the data manager, and data were entered and validated by Mfanafuthi Mthambela. Clive Govender provided data quality control. Members of the Center for Health, Intervention, and Prevention (CHIP), University of Connecticut, who developed the IMB model, were very helpful in the conceptualisation, conduct and analysis of this trial. Specifically, Paul Shuper and K. Rivet Amico provided on-going support and guidance. Katherine Fielding and Simon Lewin provided support as members of the PhD advisory committee. The intervention was based on one developed by Gerald Friedland (Yale University, USA), Marita Murrman, Patricia Torro, and Wafaa El-Sadr (all Columbia University, USA) in earlier work, and was generously shared; their support and guidance during the conceptualisation of this study conducted is acknowledged. We would like to especially acknowledge the participants who took part in this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
van Loggerenberg, F., Grant, A.D., Naidoo, K. et al. Individualised Motivational Counselling to Enhance Adherence to Antiretroviral Therapy is not Superior to Didactic Counselling in South African Patients: Findings of the CAPRISA 058 Randomised Controlled Trial. AIDS Behav 19, 145–156 (2015). https://doi.org/10.1007/s10461-014-0763-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-014-0763-6