Abstract
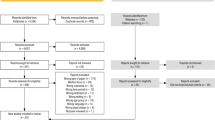
Early linkage to care and engagement in care are critical for initiation of medical interventions. However, over 50 % of newly diagnosed persons do not receive HIV-related care within 6 months of diagnosis. We evaluated a linkage to care and engagement in care initiative for HIV-positive adolescents in 15 U.S.-based clinics. Structural and client-level factors (e.g. demographic and behavioral characteristics, clinic staff and location) were evaluated as predictors of successful linkage and engagement. Within 32 months, 1,172/1,679 (69.8 %) of adolescents were linked to care of which 1,043/1,172 (89 %) were engaged in care. Only 62.1 % (1,043/1,679) of adolescents were linked and engaged in care. Linkage to care failure was attributed to adolescent, provider, and clinic-specific factors. Many adolescents provided incomplete data during the linkage process or failed to attend appointments, both associated with failure to linkage to care. Additional improvements in HIV care will require creative approaches to coordinated data sharing, as well as continued outreach services to support newly diagnosed adolescents.

Similar content being viewed by others
References
Ulett K, Willig J, Lin H, Routman J, Abroms S, Allison J, et al. The therapeutic implications of timely linkage and early retention in HIV care. AIDS Patient Care STDS. 2009;23(1):41–9.
Grangeiro A, Escuder MM, Menezes PR, Alencar R, de Ayres Castilho E. Late entry into HIV care: estimated impact on AIDS mortality rates in Brazil, 2003–2006. PLoS One. 2011;6(1):e14585.
Wanyenze RK, Hahn JA, Liechty CA, Ragland K, Ronald A, Mayanja-Kizza H, et al. Linkage to HIV care and survival following inpatient HIV counseling and testing. AIDS Behav. 2011;15(4):751–60.
CDC. HIV Surveillance report: Rates of diagnoses of HIV infection among adults and adolescents, by area of residence, 2011–United States and 6 dependent areas. 2011.
Hull MW, Wu Z, Montaner JSG. Optimizing the engagement of care cascade: a critical step to maximize the impact of HIV treatment as prevention. Curr Opin HIV AIDS. 2012;7(6):579–86.
Craw J, Gardner L, Rossman A, Gruber D, Noreen OD, Jordan D, et al. Structural factors and best practices in implementing a linkage to HIV care program using the ARTAS model. BMC Health Serv Res. 2010;10:246.
Craw JA, Gardner LI, Marks G, Rapp RC, Bosshart J, Duffus WA, et al. Brief strengths-based case management promotes entry into HIV medical care: results of the antiretroviral treatment access study-II. J Acquir Immune Defic Syndr. 2008;47:597–606.
Gardner LI, Metsch LR, Anderson-Mahoney P, Loughlin AM, del RC, Strathdee S, et al. Efficacy of a brief case management intervention to link recently diagnosed HIV-infected persons to care. AIDS. 2005;19:423–31.
Mugavero MJ, Norton WE, Saag MS. Health care system and policy factors influencing engagement in HIV medical care: piecing together the fragments of a fractured health care delivery system. Clin Infect Dis. 2011;52(suppl 2):S238.
Mugavero MJ, Davila JA, Nevin CR, Giordano TP. From access to engagement: measuring retention in outpatient HIV clinical care. AIDS Patient Care STDS. 2010;24:607–13.
Fleishman JA, Yehia BR, Moore RD, Korthuis PT, Gebo KA. Establishment, retention, and loss to follow-up in outpatient HIV care. J Acquir Immune Defic Syndr. 2012;60(3):249–59.
Hall HI, Gray KM, Tang T, Li J, Shouse L, Mermin J. Retention in care of adults and adolescents living with HIV in 13 US areas. J Acquir Immune Defic Syndr. 2012;60(1):77.
Giordano T, Gifford A, Suarez-Almazor M, Rabeneck L, Hartman C, Backus L, et al. Retention in care: a challenge to survival with HIV infection. Clin Infect Dis. 2007;44(11):1493–9.
Mugavero MJ, Lin HY, Willig JH, Westfall AO, Ulett KB, Routman JS, et al. Missed visits and mortality in patients establishing initial outpatient HIV treatment. Clin Infect Dis: an official publication of the Infectious Diseases Society of America. 2009;48(2):248.
CDC. HIV among youth in the US. 2013.
Centers for Disease C, prevention. Results of the Expanded HIV Testing Initiative–25 jurisdictions, United States, 2007–2010. MMWR Morb Mortal Wkly Rep. 2011;60(24):805–10.
Martinez J, Bell D, Dodds S, Shaw K, Siciliano C, LE Walker, et al. Transitioning youths into care: linking identified HIV-infected youth at outreach sites in the community to hospital-based clinics and or community-based health centers. J Adolesc Health. 2003;33(Suppl-30):23–30.
Minniear TD, Gaur AH, Thridandapani A, Sinnock C, Tolley EA, Flynn PM. Delayed Entry into and Failure to Remain in HIV Care Among HIV-Infected Adolescents. AIDS Res Hum Retroviruses. 2012;29:99–104.
Castle PE, Rodriguez AC, Burk RD, Herrero R, Wacholder S, Hildesheim A, et al. Long-term persistence of prevalently detected human papillomavirus infections in the absence of detectable cervical precancer and cancer. J Infect Dis. 2011;203(6):814–22.
Grant AM, Jamieson DJ, Elam-Evans LD, Beck-Sague C, Duerr A, Henderson SL. Reasons for testing and clinical and demographic profile of adolescents with non-perinatally acquired HIV infection. Pediatrics. 2006;117:468–75.
Hosek SG, Harper GW, Lemos D, Martinez J. The adolescent medicine trials network for HIVAI. An ecological model of stressors experienced by youth newly diagnosed with HIV. J HIV AIDS Prev Child Youth. 2008;9:192–218.
Wiehe SE, Aalsma MC, Liu GC, Fortenberry JD. Gender differences in the association between perceived discrimination and adolescent smoking. Am J Public Health. 2010;100(3):510–6.
Ryscavage PA, Anderson EJ, Sutton SH, Reddy S, Taiwo B. Clinical outcomes of adolescents and young adults in adult HIV care. J Acquir Immune Defic Syndr. 2011;58(2):193–7.
Elo IT, Culhane JF. Variations in health and health behaviors by nativity among pregnant black women in philadelphia. Am J Public Health. 2010;100(11):2185–92.
Gardner LI, Marks G, Craw J, Metsch L, Strathdee S, Anderson-Mahoney P, et al. Demographic, psychological, and behavioral modifiers of the Antiretroviral Treatment Access Study (ARTAS) intervention. AIDS Patient Care STDS. 2009;23:735–42.
ONAP. National HIV/AIDS Strategy: Update of the 2011–2012 Federal Efforts to Implement the National HIV/AIDS Strategy. http://www.aids.gov/federal-resources/national-hiv-aids-strategy/documents/index.html—progress-reports: 2012.
Tanner A, Philbin MM, DuVal A, Ellen J, Kapogiannis B, Fortenberry JD, editors. Models of Relationships between local health departments and adolescent medicine clinics: Implications for identifying a best-practice approach for linkage HIV-infected adolescents to care. International AIDS Society Conference; 2012; Washington DC.
Philbin MM, Tanner A, Duval A, Ellen J, Kapogiannis B, Fortenberry JD. Linking HIV-positive adolescents to care in 15 different clinics across the United States: creating solutions to address structural barriers for linkage to care. AIDS Care. 2013. doi:10.1080/09540121.2013.808730.
Tanner A, Philbin MM, DuVal A, Ellen J, Kapogiannis B, Fortenberry JD, editors. Linkinge HIV postiive adolescents to care: the role and process of youth friendly clinical environments American Public Health Association Conference; 2012; San Francisco, CA.
CDC. HIPAA privacy rule and public health guidance from CDC and the U.S. Department of Health and Human Service. In: CDC Surveillance Summaries. MMWR; 2003; 52(No. SS-l):1–12.
Hightow-Weidman LB, Jones K, Wohl AR, Futterman D, Outlaw A, Phillips G, et al. Early linkage and retention in care: findings from the outreach, linkage, and retention in care initiative among young men of color who have sex with men. AIDS Patient Care STDS. 2011;25(S1):31–8.
Omi J, Hamilton T, Casey E, editors. From testing to primary care: impact of the HIV testing expansion initiative of a large public hospital system on linking and retaining patients in HIV primary care. International AIDS Society Conference; 2010; Vienna, Austria.
Mugavero M, Norton WE, Saag M. Health care system and policy factors influencing engagement in HIV medical care: piecing together the fragments of a fractured health care delivery system. Clin Infect Dis. 2011;52(2):S238–46.
Fortenberry JD, Martinez J, Rudy BJ, Monte D. Linkage to care for HIV-positive adolescents: a multisite study of the adolescent medicine trials units of the adolescent trials network. J Adolesc Health. 2012;51:551–6.
Straub DM, Deeds BG, Willard N, Castor J, Peralta L, Francisco VT, et al. Partnership selection and formation: a case study of developing adolescent health community-researcher partnerships in fifteen US communities. J Adolesc Health. 2007;40(6):489–98.
Ziff MA, Harper GW, Chutuape KS, Deeds BG, Futterman D, Francisco VT, et al. Laying the foundation for connect to protect®: a multi-site community mobilization intervention to reduce HIV/AIDS incidence and prevalence among urban youth. J Urban Health. 2006;83(3):506–22.
Gardner EM, McLees MP, Steiner JF, del Rio C, Burman WJ. The spectrum of engagement in HIV care and its relevance to test-and-treat strategies for prevention of HIV infection. Clin Infect Dis. 2011;52(6):793.
Cohen MS, Chen YQ, McCauley M, Gamble T, Hosseinipour MC, Kumarasamy N, et al. Prevention of HIV-1 infection with early antiretroviral therapy. N Engl J Med. 2011;365:493–505.
Acknowledgments
The Adolescent Medicine Trials Network for HIV/AIDS Interventions is funded by grants 5 U01 HD 40533 and 5 U01 HD 40474 from the National Institutes of Health through the National Institute of Child Health and Human Development (Bill Kapogiannis, MD) with supplemental funding from the National Institutes on Drug Abuse (Nicolette Borek, PhD) and Mental Health (Susannah Allison, PhD; Pim Brouwers, PhD). Additional support was provided by an administrative supplement awarded through funds from the American Recovery and Reinvestment Act (ARRA) of 2009. The study was scientifically reviewed by the Adolescent Trials Network Community Prevention Leadership Group. Network, scientific, and logistical support was provided by the Adolescent Trials Network Coordinating Center (Craig Wilson, MD; Cynthia Partlow, MEd). Project support and coordination was provided by the Adolescent Trials Network Data and Operations Center at Westat, Inc. (Jim Korelitz, PhD; Barbara Driver RN, MS). We acknowledge the investigators and staff at the of the Adolescent Trials Network sites that participated in the study: Children’s Diagnostic and Treatment Center, Fort Lauderdale, FL (Ana Puga, MD, Esmine Leonard, RN, Amy Inman, BS); Children’s Hospital of Los Angeles, Los Angeles, CA (Marvin Belzer, MD, Diane Tucker, RN, MSN); Children’s Hospital of Philadelphia (Bret Rudy, MD, Mary Tanney, RN, MSN, CRNP, Adrienne DiBenedetto, BSN), Children’s Memorial Hospital, Chicago, IL (Robert Garofalo, MD, Julia Brennan, RN, MSN, ANP-C, Jennifer Kershaw, CPNP); Children’s National Medical Center, Washington, DC (Lawrence J. D’Angelo, MD, Connie Trexler, RN, CPN, BSN, Rita Hagler, CPNP, Amy Klamberg, CPNP); John H. Stroger Jr. Hospital of Cook County and the Ruth M. Rothstein CORE Center, Chicago, IL (Jaime Martinez, MD, Lisa Henry-Reid, MD, Kelly Bojan, DNP, RN, CFNP, Rachel Jackson, MSN, APN, CFNP); Montefiore Medical Center, Bronx, NY (Donna Futterman, MD, Elizabeth Enriquez-Bruce, MD, Maria Campos, RN); Mount Sinai Medical Center, New York, NY (John Steever, MD, Mary Geiger, RN); St. Jude Children’s Research Hospital, Memphis, TN (Pat Flynn, MD, Mary Dillard, RN, Carla McKinley, FNP); Tulane University Health Sciences Center, New Orleans, LA (Sue Ellen Abdalian, MD, Alyne Baker, RN, MN, Leslie Kozina, RN, CCRC); University of California at San Francisco, San Francisco, CA (Barbara Moscicki, MD, Lisa D. Irish, BSN, J. B. Molaghan, BA); University of Maryland, Baltimore, MD (Ligia Peralta, MD, Leonel Flores, MD, Reshma S. Gorle, MPH); University of Miami School of Medicine (Larry Friedman, MD, Donna Maturo, ARNP, Hanna Major-Wilson, ARNP), University of Puerto Rico, San Juan, PR (Irma L. Febo, MD, Hazel T Ayala-Flores, BSN, Anne T. F. Gomez, BA); University of South Florida, Tampa, FL (Patricia Emmanuel, MD, Diane M. Straub, MD, MPH, Silvia Callejas, BSN, ACRN, CCRC, Priscilla C. Julian, RN).
Author information
Authors and Affiliations
Consortia
Corresponding author
Rights and permissions
About this article
Cite this article
Philbin, M.M., Tanner, A.E., DuVal, A. et al. Factors Affecting Linkage to Care and Engagement in Care for Newly Diagnosed HIV-Positive Adolescents Within Fifteen Adolescent Medicine Clinics in the United States. AIDS Behav 18, 1501–1510 (2014). https://doi.org/10.1007/s10461-013-0650-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-013-0650-6