Abstract
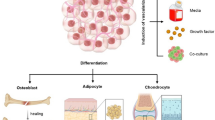
Tissue-engineered vessels offer options for autologous vascular grafts in cardiovascular repair and regeneration. The experiments aimed to construct functional arterial grafts by combining human hair follicle mesenchymal stem cells (HF-MSCs) with acellular umbilical arteries. We isolated mesenchymal stem cells from human hair follicles. Under appropriate culture conditions, these cells displayed CD44, CD90 and CD105, and exhibited the potential for differentiation to adipocytes, osteoblasts and chondrocytes. Very promisingly, HF-MSCs expressed the vascular smooth muscle specific markers in the presence of transforming growth factor-β. We created acellular arterial scaffolds by digesting human umbilical arteries with trypsin and sodium dodecyl sulfate. These acellular arterial scaffolds retained major components of the extracellular matrix. The mechanical properties of these acellular arterial scaffolds were very similar to those of native blood vessels. We then seeded HF-MSCs into acellular arterial scaffolds and found that they still expressed vascular smooth muscle specific markers. The arterial grafts derived from HF-MSCs demonstrated vasoreactivity in response to humoral constrictors. We constructed arterial grafts that are very close to native blood vessels in their structures and physiological functions. These properties suggest that these arterial grafts could be used as small diameter arterial grafts for cardiovascular repair and regeneration.








Similar content being viewed by others
References
Allaire, E., P. Bruneval, C. Mandet, J. P. Becquemin, and J. B. Michel. The immunogenicity of the extracellular matrix in arterial xenografts. Surgery 122:73–81, 1997.
Amiel, G. E., M. Komura, O. Shapira, J. J. Yoo, S. Yazdani, J. Berry, S. Kaushal, J. Bischoff, A. Atala, and S. Soker. Engineering of blood vessels from acellular collagen matrices coated with human endothelial cells. Tissue Eng. 12:2355–2365, 2006.
Baim, D. S. Percutaneous treatment of saphenous vein graft disease: the ongoing challenge. J. Am. Coll. Cardiol. 42:1370–1372, 2003.
Birchall, M., and G. Hamilton. Tissue-engineered vascular replacements for children. Lancet 380:197–198, 2012.
Bitter, T., and H. M. Muir. A modified uronic acid carbazole reaction. Anal. Biochem. 4:330–334, 1962.
Cervera, R. P., and M. Stojkovic. Commentary: somatic cell nuclear transfer-progress and promise. Stem Cells 26:494–495, 2008.
Chou, M. T., S. N. Chang, C. Ke, H. I. Chang, M. L. Sung, H. C. Kuo, and C. N. Chen. The proliferation and differentiation of placental-derived multipotent cells into smooth muscle cells on fibrillar collagen. Biomaterials 31:4367–4375, 2010.
Dahl, S. L., J. Koh, V. Prabhakar, and L. E. Niklason. Decellularized native and engineered arterial scaffolds for transplantation. Cell Transplant. 12:659–666, 2003.
Daniel, J., K. Abe, and P. S. McFetridge. Development of the human umbilical vein scaffold for cardiovascular tissue engineering applications. ASAIO J. 51:252–261, 2005.
Dardik, H. The second decade of experience with the umbilical vein graft for lower-limb revascularization. Cardiovasc. Surg. 3:265–269, 1995.
Dardik, H., N. Miller, A. Dardik, I. Ibrahim, B. Sussman, S. M. Berry, F. Wolodiger, M. Kahn, and I. Dardik. A decade of experience with the glutaraldehyde-tanned human umbilical cord vein graft for revascularization of the lower limb. J. Vasc. Surg. 7:336–346, 1988.
Dardik, H., K. Wengerter, F. Qin, A. Pangilinan, F. Silvestri, F. Wolodiger, M. Kahn, B. Sussman, and I. M. Ibrahim. Comparative decades of experience with glutaraldehydetanned human umbilical cord vein graft for lower limb revascularization: an analysis of 1275 cases. J. Vasc. Surg. 35:64–71, 2002.
de Valence, S., J. C. Tille, J. P. Giliberto, W. Mrowczynski, R. Gurny, B. H. Walpoth, and M. Möller. Advantages of bilayered vascular grafts for surgical applicability and tissue regeneration. Acta biomater. 8:3914–3920, 2012.
Eagle, K. A., R. A. Guyton, R. Davidoff, F. H. Edwards, G. A. Ewy, T. J. Gardner, J. C. Hart, H. C. Herrmann, L. D. Hillis, A. M. Hutter, Jr., B. W. Lytle, R. A. Marlow, W. C. Nugent, and T. A. Orszulak. ACC/AHA 2004 guideline update for coronary artery bypass graft surgery: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1999 Guidelines for Coronary Artery Bypass Graft Surgery). Circulation 110:e340–e437, 2004.
Elkins, R. C., M. M. Lane, S. B. Capps, C. McCue, and P. E. Dawson. Humoral immune response to allograft valve tissue pretreated with an antigen reduction process. Semin. Thorac. Cardiovasc. Surg. 13:82–86, 2001.
Gui, L., A. Muto, S. A. Chan, C. K. Breuer, and L. E. Niklason. Development of decellularized human umbilical arteries as small-diameter vascular grafts. Tissue Eng. Part A. 15:2665–2676, 2009.
Hochedlinger, K., and R. Jaenisch. Nuclear reprogramming and pluripotency. Nature 441:1061–1067, 2006.
Hoogduijn, M. J., E. Gorjup, and P. G. Genever. Comparative characterization of hair follicle dermal stem cells and bone marrow mesenchymal stem cells. Stem Cells Dev. 15:49–60, 2006.
Hoopes, C. W., and J. F. Platt. Molecular strategies for clinical xenotransplantation in cardiothoracic surgery. Semin. Thorac. Cardiovasc. Surg. 8:156–174, 1996.
Jahoda, C. A., J. Whitehouse, A. J. Reynolds, and N. Hole. Hair follicle dermal cells differentiate into adipogenic and osteogenic lineages. Exp. Dermatol. 12:849–859, 2003.
Krawiec, J. T., and D. A. Vorp. Adult stem cell-based tissue engineered blood vessels: a review. Biomaterials 33:3388–3400, 2012.
Krenning, G., J. R. Moonen, M. J. van Luyn, and M. C. Harmsen. Vascular smooth muscle cells for use in vascular tissue engineering obtained by endothelial-to-mesenchymal transdifferentiation (EnMT) on collagen matrices. Biomaterials 29:3703–3711, 2008.
Lako, M., L. Armstrong, P. M. Cairns, S. Harris, N. Hole, and C. A. Jahoda. Hair follicle dermal cells repopulate the mouse haematopoietic system. J. Cell Sci. 115:3967–3974, 2002.
Liu, J. Y., H. F. Peng, and S. T. Andreadis. Contractile smooth muscle cells derived from hair-follicle stem cells. Cardiovasc. Res. 79:24–33, 2008.
Liu, J. Y., H. F. Peng, S. Gopinath, J. Tian, and S. T. Andreadis. Derivation of functional smooth muscle cells from multipotent human hair follicle mesenchymal stem cells. Tissue Eng. Part A. 16:2553–2564, 2010.
Liu, X., L. Song, J. Liu, S. Wang, X. Tan, X. Bai, T. Bai, Y. Wang, M. Li, Y. Song, and Y. Li. miR-18b inhibits TGF-β1-induced differentiation of hair follicle stem cells into smooth muscle cells by targeting SMAD2. Biochem. Biophys. Res. Commun. 438:551–556, 2013.
Liu, J. Y., D. D. Swartz, H. F. Peng, S. F. Gugino, J. A. Russell, and S. T. Andreadis. Functional tissue-engineered blood vessels from bone marrow progenitor cells. Cardiovasc. Res. 75:618–628, 2007.
Meyer, S. R., J. Nagendran, L. S. Desai, G. R. Rayat, T. A. Churchill, C. C. Anderson, R. V. Rajotte, J. R. Lakey, and D. B. Ross. Decellularization reduces the immune response to aortic valve allografts in the rat. J. Thorac. Cardiovasc. Surg. 130:469–476, 2005.
Peng, H. F., J. Y. Liu, S. T. Andreadis, and D. D. Swartz. Hair follicle-derived smooth muscle cells and small intestinal submucosa for engineering mechanically robust and vasoreactive vascular media. Tissue Eng. Part A. 17:981–990, 2011.
Rashid, S. T., B. Fuller, G. Hamilton, and A. M. Seifalian. Tissue engineering of a hybrid bypass graft for coronary and lower limb bypass surgery. FASEB J. 22:2084–2089, 2008.
Rieder, E., A. Nigisch, B. Dekan, M. T. Kasimir, F. Mühlbacher, E. Wolner, P. Simon, and G. Weigel. Granulocyte-based immune response against decellularized or glutaraldehyde cross-linked vascular tissue. Biomaterials 27:5634–5642, 2006.
Robotin-Johnson, M. C., P. E. Swanson, D. C. Johnson, R. B. Schuessler, and J. L. Cox. An experimental model of small intestinal submucosa as a growing vascular graft. J. Thorac. Cardiovasc. Surg. 116:805–811, 1998.
Rodolfa, K. T., and K. Eggan. A transcriptional logic for nuclear reprogramming. Cell 126:652–655, 2006.
Sandusky, G. E., G. C. Lantz, and S. F. Badylak. Healing comparison of small intestine submucosa and ePTFE grafts in the canine carotid artery. J. Surg. Res. 58:415–420, 1995.
Schaner, P. J., N. D. Martin, T. N. Tulenko, I. M. Shapiro, N. A. Tarola, R. F. Leichter, R. A. Carabasi, and P. J. Dimuzio. Decellularized vein as a potential scaffold for vascular tissue engineering. J. Vasc. Surg. 40:146–153, 2004.
Shinoka, T., D. Shum-Tim, P. X. Ma, R. E. Tanel, N. Isogai, R. Langer, J. P. Vacanti, and J. E. Mayer, Jr. Creation of viable pulmonary artery autografts through tissue engineering. J. Thorac. Cardiovasc. Surg. 115:536–545, 1998.
Torikai, K., H. Ichikawa, K. Hirakawa, G. Matsumiya, T. Kuratani, S. Iwai, A. Saito, N. Kawaguchi, N. Matsuura, and Y. Sawa. A self-renewing, tissue-engineered vascular graft for arterial reconstruction. J. Thorac. Cardiovasc. Surg. 136:37–45, 2008.
Tschoeke, B., T. C. Flanagan, A. Cornelissen, S. Koch, A. Roehl, M. Sriharwoko, J. S. Sachweh, T. Gries, T. Schmitz-Rode, and S. Jockenhoevel. Development of a composite degradable/nondegradable tissue-engineered vascular graft. Artif. Organs 32:800–809, 2008.
Tu, J. V., C. L. Pashos, C. D. Naylor, E. Chen, S. L. Normand, J. P. Newhouse, and B. J. McNeil. Use of cardiac procedures and outcomes in elderly patients with myocardial infarction in the United States and Canada. N. Engl. J. Med. 336:1500–1505, 1997.
Wang, K., Y. Guan, Y. Liu, M. Zhu, T. Li, D. An, L. Ou, Y. Che, G. Zhang, J. Zhang, X. L. Zheng, and D. Kong. Fibrin glue with autogenic bone marrow mesenchymal stem cells for urethral injury repair in rabbit model. Tissue Eng. Part A. 18:23–24, 2012.
Wang, Y., J. Liu, X. Tan, G. Li, Y. Gao, X. Liu, L. Zhang, and Y. Li. Induced pluripotent stem cells from human hair follicle mesenchymal stem cells. Stem Cell Rev. 9:451–460, 2012.
Weinberg, C. B., and E. Bell. A blood vessel model constructed from collagen and cultured vascular cells. Science 231:397–400, 1986.
Wells, W., M. Malas, C. J. Baker, S. M. Quardt, and M. L. Barr. Depopulated vena caval homograft: a new venous conduit. J. Thorac. Cardiovasc. Surg. 126:498–503, 2003.
Woessner, Jr., J. F. The determination of hydroxyproline in tissue and protein samples containing small proportions of this imino acid. Arch. Biochem. Biophys. 93:440–447, 1961.
Yu, H., D. Fang, S. M. Kumar, L. Li, T. K. Nguyen, G. Acs, M. Herlyn, and X. Xu. Isolation of a novel population of multipotent adult stem cells from human hair follicles. Am. J. Pathol. 168:1879–1888, 2006.
Zhang, X., Y. Wang, Y. Gao, X. Liu, T. Bai, M. Li, L. Li, G. Chi, H. Xu, F. Liu, J. Y. Liu, and Y. Li. Maintenance of high proliferation and multipotent potential of human hair follicle -derived mesenchymal stem cells by growth factors. Int. J. Mol. Med. 31:913–921, 2013.
Acknowledgments
We appreciate the help of Dr. F William Orr, Department of Pathology, University of Manitoba, Canada, for revising this manuscript. The present study was supported by grants from the State Key Development Program of Basic Research of China (no. 211CB606200), the National Natural Science Foundation of China (no. 30930026/C100101), the Science and Technology Planning Project of Jilin Province, China (no. 20100947, no. 20120935), the Frontier Interdiscipline Program of Norman Bethune Health Science Center of Jilin University (2013101007) and the Specialized Research Fund for the Doctoral Program of Higher Education (20130061110077).
Author information
Authors and Affiliations
Corresponding authors
Additional information
Associate Editor Jennifer West oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Gao, Y., Liu, F., Zhang, L. et al. Acellular Blood Vessels Combined Human Hair Follicle Mesenchymal Stem Cells for Engineering of Functional Arterial Grafts. Ann Biomed Eng 42, 2177–2189 (2014). https://doi.org/10.1007/s10439-014-1061-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-014-1061-1