Abstract
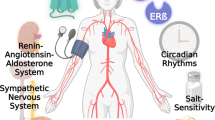
Cardiovascular disease (CVD) remains a worldwide public health concern despite decades of research and the availability of numerous targeted therapies. While the intrinsic physiological mechanisms regulating cardiovascular function are similar between males and females, marked sex differences have been established in terms of CVD onset, pathophysiology, manifestation, susceptibility, prevalence, treatment responses and outcomes in animal models and clinical populations. Premenopausal females are generally protected from CVD in comparison to men of similar age, with females tending to develop cardiovascular complications later in life following menopause. Emerging evidence suggests this cardioprotection in females is, in part, attributed to sex differences in hormonal regulators, such as the renin–angiotensin system (RAS). To date, research has largely focused on canonical RAS pathways and shown that premenopausal females are protected from cardiovascular derangements produced by activation of angiotensin II pathways. More recently, a vasodilatory arm of the RAS has emerged that is characterized by angiotensin-(1-7) [(Ang-(1-7)], angiotensin-converting enzyme 2 and Mas receptors. Emerging studies provide evidence for a shift towards these cardioprotective Ang-(1-7) pathways in females, with effects modulated by interactions with estrogen. Despite well-established sex differences, female comparison studies on cardiovascular outcomes are lacking at both the preclinical and clinical levels. Furthermore, there are no specific guidelines in place for the treatment of cardiovascular disease in men versus women, including therapies targeting the RAS. This review summarizes current knowledge on sex differences in the cardiovascular actions of the RAS, focusing on interactions with gonadal hormones, emerging data for protective Ang-(1-7) pathways and potential clinical implications for established and novel therapies.



Similar content being viewed by others
References
Benjamin EJ, Blaha MJ, Chiuve SE, Cushman M, Das SR, Deo R, de Ferranti SD, Floyd J, Fornage M, Gillespie C, Isasi CR, Jimenez MC, Jordan LC, Judd SE, Lackland D, Lichtman JH, Lisabeth L, Liu S, Longenecker CT, Mackey RH, Matsushita K, Mozaffarian D, Mussolino ME, Nasir K, Neumar RW, Palaniappan L, Pandey DK, Thiagarajan RR, Reeves MJ, Ritchey M, Rodriguez CJ, Roth GA, Rosamond WD, Sasson C, Towfighi A, Tsao CW, Turner MB, Virani SS, Voeks JH, Willey JZ, Wilkins JT, Wu JH, Alger HM, Wong SS, Muntner P, American Heart Association Statistics C, Stroke Statistics S (2017) Heart disease and stroke statistics—2017 update: a report from the American heart association. Circulation 135(10):e146–e603. https://doi.org/10.1161/CIR.0000000000000485
Kjeldsen SE (2018) Hypertension and cardiovascular risk: general aspects. Pharmacol Res 129:95–99. https://doi.org/10.1016/j.phrs.2017.11.003
Regitz-Zagrosek V, Kararigas G (2017) Mechanistic pathways of sex differences in cardiovascular disease. Physiol Rev 97(1):1–37. https://doi.org/10.1152/physrev.00021.2015
Colafella KMM, Denton KM (2018) Sex-specific differences in hypertension and associated cardiovascular disease. Nat Rev Nephrol 14(3):185–201. https://doi.org/10.1038/nrneph.2017.189
Komukai K, Mochizuki S, Yoshimura M (2010) Gender and the renin–angiotensin–aldosterone system. Fundam Clin Pharmacol 24(6):687–698. https://doi.org/10.1111/j.1472-8206.2010.00854.x
White MC, Fleeman R, Arnold AC (2019) Sex differences in the metabolic effects of the renin–angiotensin system. Biol Sex Differ 10(1):31. https://doi.org/10.1186/s13293-019-0247-5
Fernandez-Atucha A, Izagirre A, Fraile-Bermudez AB, Kortajarena M, Larrinaga G, Martinez-Lage P, Echevarria E, Gil J (2017) Sex differences in the aging pattern of renin–angiotensin system serum peptidases. Biol Sex Differ 8:5. https://doi.org/10.1186/s13293-017-0128-8
Dasinger JH, Alexander BT (2016) Gender differences in developmental programming of cardiovascular diseases. Clin Sci (Lond) 130(5):337–348. https://doi.org/10.1042/CS20150611
Kurtz A (2011) Renin release: sites, mechanisms, and control. Annu Rev Physiol 73:377–399. https://doi.org/10.1146/annurev-physiol-012110-142238
Miller AJ, Arnold AC (2019) The renin–angiotensin system in cardiovascular autonomic control: recent developments and clinical implications. Clin Auton Res 29(2):231–243. https://doi.org/10.1007/s10286-018-0572-5
Lemarie CA, Schiffrin EL (2010) The angiotensin II type 2 receptor in cardiovascular disease. J Renin Angiotensin Aldosterone Syst 11(1):19–31. https://doi.org/10.1177/1470320309347785
Medina D, Arnold AC (2019) Angiotensin-(1-7): translational avenues in cardiovascular control. Am J Hypertens 32(12):1133–1142. https://doi.org/10.1093/ajh/hpz146
Santos RAS, Sampaio WO, Alzamora AC, Motta-Santos D, Alenina N, Bader M, Campagnole-Santos MJ (2018) The ACE2/angiotensin-(1-7)/MAS axis of the renin–angiotensin system: focus on angiotensin-(1-7). Physiol Rev 98(1):505–553. https://doi.org/10.1152/physrev.00023.2016
Stocco C (2012) Tissue physiology and pathology of aromatase. Steroids 77(1–2):27–35. https://doi.org/10.1016/j.steroids.2011.10.013
Fischer M, Baessler A, Schunkert H (2002) Renin angiotensin system and gender differences in the cardiovascular system. Cardiovasc Res 53(3):672–677. https://doi.org/10.1016/s0008-6363(01)00479-5
Schunkert H, Danser AH, Hense HW, Derkx FH, Kurzinger S, Riegger GA (1997) Effects of estrogen replacement therapy on the renin–angiotensin system in postmenopausal women. Circulation 95(1):39–45. https://doi.org/10.1161/01.cir.95.1.39
De Lignieres B, Basdevant A, Thomas G, Thalabard JC, Mercier-Bodard C, Conard J, Guyene TT, Mairon N, Corvol P, Guy-Grand B Mauvais-Jarvis P, Sitruk-Ware R (1986) Biological effects of estradiol-17β in postmenopausal women: oral versus percutaneous administration. J Clin Endocrinol Metab 62(3):536–541. https://doi.org/10.1210/jcem-62-3-536
Hassager C, Riis BJ, Strom V, Guyene TT, Christiansen C (1987) The long-term effect of oral and percutaneous estradiol on plasma renin substrate and blood pressure. Circulation 76(4):753–758. https://doi.org/10.1161/01.cir.76.4.753
Roesch DM, Tian Y, Zheng W, Shi M, Verbalis JG, Sandberg K (2000) Estradiol attenuates angiotensin-induced aldosterone secretion in ovariectomized rats. Endocrinology 141(12):4629–4636. https://doi.org/10.1210/endo.141.12.7822
Wu Z, Maric C, Roesch DM, Zheng W, Verbalis JG, Sandberg K (2003) Estrogen regulates adrenal angiotensin AT1 receptors by modulating AT1 receptor translation. Endocrinology 144(7):3251–3261. https://doi.org/10.1210/en.2003-0015
Ichiki T, Usui M, Kato M, Funakoshi Y, Ito K, Egashira K, Takeshita A (1998) Downregulation of angiotensin II type 1 receptor gene transcription by nitric oxide. Hypertension 31(1 Pt 2):342–348. https://doi.org/10.1161/01.hyp.31.1.342
Brosnihan KB, Li P, Ganten D, Ferrario CM (1997) Estrogen protects transgenic hypertensive rats by shifting the vasoconstrictor–vasodilator balance of RAS. Am J Physiol 273(6):R1908–1915. https://doi.org/10.1152/ajpregu.1997.273.6.R1908
Xu X, Xiao JC, Luo LF, Wang S, Zhang JP, Huang JJ, Liu ML, Liu CG, Xu KQ, Li YJ, Song HP (2008) Effects of ovariectomy and 17β-estradiol treatment on the renin–angiotensin system, blood pressure, and endothelial ultrastructure. Int J Cardiol 130(2):196–204. https://doi.org/10.1016/j.ijcard.2007.08.041
Chao HH, Chen JJ, Chen CH, Lin H, Cheng CF, Lian WS, Chen YL, Juan SH, Liu JC, Liou JY, Chan P, Cheng TH (2005) Inhibition of angiotensin II induced endothelin-1 gene expression by 17-β-oestradiol in rat cardiac fibroblasts. Heart 91(5):664–669. https://doi.org/10.1136/hrt.2003.031898
Ichikawa J, Sumino H, Ichikawa S, Ozaki M (2006) Different effects of transdermal and oral hormone replacement therapy on the renin–angiotensin system, plasma bradykinin level, and blood pressure of normotensive postmenopausal women. Am J Hypertens 19(7):744–749. https://doi.org/10.1016/j.amjhyper.2005.10.006
Gupte M, Thatcher SE, Boustany-Kari CM, Shoemaker R, Yiannikouris F, Zhang X, Karounos M, Cassis LA (2012) Angiotensin converting enzyme 2 contributes to sex differences in the development of obesity hypertension in C57BL/6 mice. Arterioscler Thromb Vasc Biol 32(6):1392–1399. https://doi.org/10.1161/ATVBAHA.112.248559
Sullivan JC, Rodriguez-Miguelez P, Zimmerman MA, Harris RA (2015) Differences in angiotensin (1-7) between men and women. Am J Physiol Heart Circ Physiol 308(9):H1171–1176. https://doi.org/10.1152/ajpheart.00897.2014
Mompeon A, Lazaro-Franco M, Bueno-Beti C, Perez-Cremades D, Vidal-Gomez X, Monsalve E, Gironacci MM, Hermenegildo C, Novella S (2016) Estradiol, acting through ERα, induces endothelial non-classic renin–angiotensin system increasing angiotensin 1-7 production. Mol Cell Endocrinol 422:1–8. https://doi.org/10.1016/j.mce.2015.11.004
Bukowska A, Spiller L, Wolke C, Lendeckel U, Weinert S, Hoffmann J, Bornfleth P, Kutschka I, Gardemann A, Isermann B, Goette A (2017) Protective regulation of the ACE2/ACE gene expression by estrogen in human atrial tissue from elderly men. Exp Biol Med (Maywood) 242(14):1412–1423. https://doi.org/10.1177/1535370217718808
Lee SH, Lee YH, Jung SW, Kim DJ, Park SH, Song SJ, Jeong KH, Moon JY, Ihm CG, Lee TW, Kim JS, Sohn IS, Lee SY, Kim DO, Kim YG (2019) Sex-related differences in the intratubular renin–angiotensin system in two-kidney, one-clip hypertensive rats. Am J Physiol Renal Physiol 317(3):F670–F682. https://doi.org/10.1152/ajprenal.00451.2018
Baiardi G, Macova M, Armando I, Ando H, Tyurmin D, Saavedra JM (2005) Estrogen upregulates renal angiotensin II AT1 and AT2 receptors in the rat. Regul Pept 124(1–3):7–17. https://doi.org/10.1016/j.regpep.2004.06.021
Macova M, Armando I, Zhou J, Baiardi G, Tyurmin D, Larrayoz-Roldan IM, Saavedra JM (2008) Estrogen reduces aldosterone, upregulates adrenal angiotensin II AT2 receptors and normalizes adrenomedullary Fra-2 in ovariectomized rats. Neuroendocrinology 88(4):276–286. https://doi.org/10.1159/000150977
Yoshimura Y, Karube M, Aoki H, Oda T, Koyama N, Nagai A, Akimoto Y, Hirano H, Nakamura Y (1996) Angiotensin II induces ovulation and oocyte maturation in rabbit ovaries via the AT2 receptor subtype. Endocrinology 137(4):1204–1211. https://doi.org/10.1210/endo.137.4.8625890
Vargas-Castillo A, Tobon-Cornejo S, Del Valle-Mondragon L, Torre-Villalvazo I, Schcolnik-Cabrera A, Guevara-Cruz M, Pichardo-Ontiveros E, Fuentes-Romero R, Bader M, Alenina N, Vidal-Puig A, Hong E, Torres N, Tovar AR (2019) Angiotensin-(1-7) induces beige fat thermogenesis through the Mas receptor. Metabolism 103:154048. https://doi.org/10.1016/j.metabol.2019.154048
Costa-Fraga FP, Goncalves GK, Souza-Neto FP, Reis AM, Capettini LA, Santos RA, Fraga-Silva RA, Stergiopulos N, da Silva RF (2018) Age-related changes in vascular responses to angiotensin-(1-7) in female mice. J Renin Angiotensin Aldosterone Syst 19(3):1470320318789332. https://doi.org/10.1177/1470320318789332
Novella S, Perez-Cremades D, Mompeon A, Hermenegildo C (2019) Mechanisms underlying the influence of oestrogen on cardiovascular physiology in women. J Physiol 597(19):4873–4886. https://doi.org/10.1113/JP278063
Ellison KE, Ingelfinger JR, Pivor M, Dzau VJ (1989) Androgen regulation of rat renal angiotensinogen messenger RNA expression. J Clin Invest 83(6):1941–1945. https://doi.org/10.1172/JCI114102
Chen YF, Naftilan AJ, Oparil S (1992) Androgen-dependent angiotensinogen and renin messenger RNA expression in hypertensive rats. Hypertension 19(5):456–463. https://doi.org/10.1161/01.hyp.19.5.456
Baltatu O, Cayla C, Iliescu R, Andreev D, Bader M (2003) Abolition of end-organ damage by antiandrogen treatment in female hypertensive transgenic rats. Hypertension 41(3 Pt 2):830–833. https://doi.org/10.1161/01.HYP.0000048702.55183.89
Chinnathambi V, More AS, Hankins GD, Yallampalli C, Sathishkumar K (2014) Gestational exposure to elevated testosterone levels induces hypertension via heightened vascular angiotensin II type 1 receptor signaling in rats. Biol Reprod 91(1):6. https://doi.org/10.1095/biolreprod.114.118968
Freshour JR, Chase SE, Vikstrom KL (2002) Gender differences in cardiac ACE expression are normalized in androgen-deprived male mice. Am J Physiol Heart Circ Physiol 283(5):H1997–2003. https://doi.org/10.1152/ajpheart.01054.2001
Leung PS, Wong TP, Chung YW, Chan HC (2002) Androgen dependent expression of AT1 receptor and its regulation of anion secretion in rat epididymis. Cell Biol Int 26(1):117–122. https://doi.org/10.1006/cbir.2001.0830
Mishra JS, More AS, Gopalakrishnan K, Kumar S (2019) Testosterone plays a permissive role in angiotensin II-induced hypertension and cardiac hypertrophy in male rats. Biol Reprod 100(1):139–148. https://doi.org/10.1093/biolre/ioy179
Mishra JS, Hankins GD, Kumar S (2016) Testosterone downregulates angiotensin II type-2 receptor via androgen receptor-mediated ERK1/2 MAP kinase pathway in rat aorta. J Renin Angiotensin Aldosterone Syst 17(4):1470320316674875. https://doi.org/10.1177/1470320316674875
Douglas GC, O'Bryan MK, Hedger MP, Lee DK, Yarski MA, Smith AI, Lew RA (2004) The novel angiotensin-converting enzyme (ACE) homolog, ACE2, is selectively expressed by adult Leydig cells of the testis. Endocrinology 145(10):4703–4711. https://doi.org/10.1210/en.2004-0443
Kang NN, Fu L, Xu J, Han Y, Cao JX, Sun JF, Zheng M (2012) Testosterone improves cardiac function and alters angiotensin II receptors in isoproterenol-induced heart failure. Arch Cardiovasc Dis 105(2):68–76. https://doi.org/10.1016/j.acvd.2011.12.002
dos Santos RL, da Silva FB, Ribeiro RF Jr, Stefanon I (2014) Sex hormones in the cardiovascular system. Horm Mol Biol Clin Investig 18(2):89–103. https://doi.org/10.1515/hmbci-2013-0048
Kang AK, Duncan JA, Cattran DC, Floras JS, Lai V, Scholey JW, Miller JA (2001) Effect of oral contraceptives on the renin angiotensin system and renal function. Am J Physiol Regul Integr Comp Physiol 280(3):R807–813. https://doi.org/10.1152/ajpregu.2001.280.3.R807
Zakheim RM, Molteni A, Mattioli L, Mullis KB (1976) Angiotensin I-converting enzyme and angiotensin II levels in women receiving an oral contraceptive. J Clin Endocrinol Metab 42(3):588–589. https://doi.org/10.1210/jcem-42-3-588
Nickenig G, Strehlow K, Wassmann S, Baumer AT, Albory K, Sauer H, Bohm M (2000) Differential effects of estrogen and progesterone on AT(1) receptor gene expression in vascular smooth muscle cells. Circulation 102(15):1828–1833. https://doi.org/10.1161/01.cir.102.15.1828
Donadio MV, Gomes CM, Sagae SC, Franci CR, Anselmo-Franci JA, Lucion AB, Sanvitto GL (2006) Estradiol and progesterone modulation of angiotensin II receptors in the arcuate nucleus of ovariectomized and lactating rats. Brain Res 1083(1):103–109. https://doi.org/10.1016/j.brainres.2006.02.018
Seltzer A, Tsutsumi K, Shigematsu K, Saavedra JM (1993) Reproductive hormones modulate angiotensin II AT1 receptors in the dorsomedial arcuate nucleus of the female rat. Endocrinology 133(2):939–941. https://doi.org/10.1210/endo.133.2.8344227
Chesley LC, Tepper IH (1967) Effects of progesterone and estrogen on the sensitivity to angiotensin II. J Clin Endocrinol Metab 27(4):576–581. https://doi.org/10.1210/jcem-27-4-576
Johnson MC, Vega M, Vantman D, Troncoso JL, Devoto L (1997) Regulatory role of angiotensin II on progesterone production by cultured human granulosa cells. Expression of angiotensin II type-2 receptor. Mol Hum Reprod 3(8):663–668. https://doi.org/10.1093/molehr/3.8.663
Shefer G, Marcus Y, Knoll E, Dolkart O, Foichtwanger S, Nevo N, Limor R, Stern N (2016) Angiotensin 1-7 is a negative modulator of aldosterone secretion in vitro and in vivo. Hypertension 68(2):378–384. https://doi.org/10.1161/HYPERTENSIONAHA.116.07088
Funder JW (2013) Mineralocorticoid receptor antagonists: emerging roles in cardiovascular medicine. Integr Blood Press Control 6:129–138. https://doi.org/10.2147/IBPC.S13783
Szmuilowicz ED, Adler GK, Williams JS, Green DE, Yao TM, Hopkins PN, Seely EW (2006) Relationship between aldosterone and progesterone in the human menstrual cycle. J Clin Endocrinol Metab 91(10):3981–3987. https://doi.org/10.1210/jc.2006-1154
Stachenfeld NS, Taylor HS (2005) Progesterone increases plasma volume independent of estradiol. J Appl Physiol (1985) 98(6):1991–1997. https://doi.org/10.1152/japplphysiol.00031.2005
Faulkner JL, Kennard S, Huby AC, Antonova G, Lu Q, Jaffe IZ, Patel VS, Fulton DJR, Belin de Chantemele EJ (2019) Progesterone predisposes females to obesity-associated leptin-mediated endothelial dysfunction via upregulating endothelial MR (mineralocorticoid receptor) expression. Hypertension 74(3):678–686. https://doi.org/10.1161/HYPERTENSIONAHA.119.12802
Cheng Y, Li Q, Zhang Y, Wen Q, Zhao J (2015) Effects of female sex hormones on expression of the Ang-(1-7)/Mas-R/nNOS pathways in rat brain. Can J Physiol Pharmacol 93(11):993–998. https://doi.org/10.1139/cjpp-2015-0087
Samuel CS, Unemori EN, Mookerjee I, Bathgate RA, Layfield SL, Mak J, Tregear GW, Du XJ (2004) Relaxin modulates cardiac fibroblast proliferation, differentiation, and collagen production and reverses cardiac fibrosis in vivo. Endocrinology 145(9):4125–4133. https://doi.org/10.1210/en.2004-0209
Phie J, Haleagrahara N, Newton P, Constantinoiu C, Sarnyai Z, Chilton L, Kinobe R (2015) Prolonged subcutaneous administration of oxytocin accelerates angiotensin II-induced hypertension and renal damage in male rats. PLoS ONE 10(9):e0138048. https://doi.org/10.1371/journal.pone.0138048
Massiera F, Bloch-Faure M, Ceiler D, Murakami K, Fukamizu A, Gasc JM, Quignard-Boulange A, Negrel R, Ailhaud G, Seydoux J, Meneton P, Teboul M (2001) Adipose angiotensinogen is involved in adipose tissue growth and blood pressure regulation. FASEB J 15(14):2727–2729. https://doi.org/10.1096/fj.01-0457fje
Yiannikouris F, Gupte M, Putnam K, Thatcher S, Charnigo R, Rateri DL, Daugherty A, Cassis LA (2012) Adipocyte deficiency of angiotensinogen prevents obesity-induced hypertension in male mice. Hypertension 60(6):1524–1530. https://doi.org/10.1161/HYPERTENSIONAHA.112.192690
Yiannikouris F, Karounos M, Charnigo R, English VL, Rateri DL, Daugherty A, Cassis LA (2012) Adipocyte-specific deficiency of angiotensinogen decreases plasma angiotensinogen concentration and systolic blood pressure in mice. Am J Physiol Regul Integr Comp Physiol 302(2):R244–251. https://doi.org/10.1152/ajpregu.00323.2011
Moreno C, Hoffman M, Stodola TJ, Didier DN, Lazar J, Geurts AM, North PE, Jacob HJ, Greene AS (2011) Creation and characterization of a renin knockout rat. Hypertension 57(3):614–619. https://doi.org/10.1161/HYPERTENSIONAHA.110.163840
Gradman AH, Weir MR, Wright M, Bush CA, Keefe DL (2010) Efficacy, safety and tolerability of aliskiren, a direct renin inhibitor, in women with hypertension: a pooled analysis of eight studies. J Hum Hypertens 24(11):721–729. https://doi.org/10.1038/jhh.2010.11
Gatineau E, Cohn DM, Poglitsch M, Loria AS, Gong M, Yiannikouris F (2019) Losartan prevents the elevation of blood pressure in adipose-PRR deficient female mice while elevated circulating sPRR activates the renin–angiotensin system. Am J Physiol Heart Circ Physiol 316(3):H506–H515. https://doi.org/10.1152/ajpheart.00473.2018
Krege JH, John SW, Langenbach LL, Hodgin JB, Hagaman JR, Bachman ES, Jennette JC, O'Brien DA, Smithies O (1995) Male–female differences in fertility and blood pressure in ACE-deficient mice. Nature 375(6527):146–148. https://doi.org/10.1038/375146a0
Toering TJ, van der Graaf AM, Visser FW, Buikema H, Navis G, Faas MM, Lely AT (2015) Gender differences in response to acute and chronic angiotensin II infusion: a translational approach. Physiol Rep 3(7):e12434. https://doi.org/10.14814/phy2.12434
Sampson AK, Moritz KM, Denton KM (2012) Postnatal ontogeny of angiotensin receptors and ACE2 in male and female rats. Gend Med 9(1):21–32. https://doi.org/10.1016/j.genm.2011.12.003
Xue B, Pamidimukkala J, Hay M (2005) Sex differences in the development of angiotensin II-induced hypertension in conscious mice. Am J Physiol Heart Circ Physiol 288(5):H2177–2184. https://doi.org/10.1152/ajpheart.00969.2004
Brosnihan KB, Hodgin JB, Smithies O, Maeda N, Gallagher P (2008) Tissue-specific regulation of ACE/ACE2 and AT1/AT2 receptor gene expression by oestrogen in apolipoprotein E/oestrogen receptor-alpha knock-out mice. Exp Physiol 93(5):658–664. https://doi.org/10.1113/expphysiol.2007.041806
Silva-Antonialli MM, Tostes RC, Fernandes L, Fior-Chadi DR, Akamine EH, Carvalho MH, Fortes ZB, Nigro D (2004) A lower ratio of AT1/AT2 receptors of angiotensin II is found in female than in male spontaneously hypertensive rats. Cardiovasc Res 62(3):587–593. https://doi.org/10.1016/j.cardiores.2004.01.020
Sampson AK, Hilliard LM, Moritz KM, Thomas MC, Tikellis C, Widdop RE, Denton KM (2012) The arterial depressor response to chronic low-dose angiotensin II infusion in female rats is estrogen dependent. Am J Physiol Regul Integr Comp Physiol 302(1):R159–165. https://doi.org/10.1152/ajpregu.00256.2011
Xue B, Zhao Y, Johnson AK, Hay M (2008) Central estrogen inhibition of angiotensin II-induced hypertension in male mice and the role of reactive oxygen species. Am J Physiol Heart Circ Physiol 295(3):H1025–H1032. https://doi.org/10.1152/ajpheart.00021.2008
Xue B, Pamidimukkala J, Lubahn DB, Hay M (2007) Estrogen receptor-alpha mediates estrogen protection from angiotensin II-induced hypertension in conscious female mice. Am J Physiol Heart Circ Physiol 292(4):H1770–1776. https://doi.org/10.1152/ajpheart.01011.2005
Xue B, Zhang Z, Beltz TG, Guo F, Hay M, Johnson AK (2014) Estrogen regulation of the brain renin–angiotensin system in protection against angiotensin II-induced sensitization of hypertension. Am J Physiol Heart Circ Physiol 307(2):H191–198. https://doi.org/10.1152/ajpheart.01012.2013
Bundalo MM, Zivkovic MD, Romic S, Tepavcevic SN, Koricanac GB, Djuric TM, Stankovic AD (2016) Fructose-rich diet induces gender-specific changes in expression of the renin–angiotensin system in rat heart and upregulates the ACE/AT1R axis in the male rat aorta. J Renin Angiotensin Aldosterone Syst 17(2):1470320316642915. https://doi.org/10.1177/1470320316642915
Ramirez LA, Sullivan JC (2018) Sex differences in hypertension: where we have been and where we are going. Am J Hypertens 31(12):1247–1254. https://doi.org/10.1093/ajh/hpy148
Cohall DH, Scantlebury-Manning T, James S, Hall K, Ferrario CM (2015) Renin–angiotensin–aldosterone system gender differences in an Afro-Caribbean population. J Renin Angiotensin Aldosterone Syst 16(3):539–546. https://doi.org/10.1177/1470320314523659
Reyes-Engel A, Morcillo L, Aranda FJ, Ruiz M, Gaitan MJ, Mayor-Olea A, Aranda P, Ferrario CM (2006) Influence of gender and genetic variability on plasma angiotensin peptides. J Renin Angiotensin Aldosterone Syst 7(2):92–97. https://doi.org/10.3317/jraas.2006.015
Chappell MC, Marshall AC, Alzayadneh EM, Shaltout HA, Diz DI (2014) Update on the Angiotensin converting enzyme 2-Angiotensin (1-7)–MAS receptor axis: fetal programing, sex differences, and intracellular pathways. Front Endocrinol (Lausanne) 4:201. https://doi.org/10.3389/fendo.2013.00201
Taylor LE, Sullivan JC (2016) Sex differences in obesity-induced hypertension and vascular dysfunction: a protective role for estrogen in adipose tissue inflammation? Am J Physiol Regul Integr Comp Physiol 311(4):R714–R720. https://doi.org/10.1152/ajpregu.00202.2016
Xue B, Zhang Z, Johnson RF, Guo F, Hay M, Johnson AK (2013) Central endogenous angiotensin-(1–7) protects against aldosterone/NaCl-induced hypertension in female rats. Am J Physiol Heart Circ Physiol 305(5):H699–705. https://doi.org/10.1152/ajpheart.00193.2013
Shoemaker R, Tannock LR, Su W, Gong M, Gurley SB, Thatcher SE, Yiannikouris F, Ensor CM, Cassis LA (2019) Adipocyte deficiency of ACE2 increases systolic blood pressures of obese female C57BL/6 mice. Biol Sex Differ 10(1):45. https://doi.org/10.1186/s13293-019-0260-8
Chen YY, Zhang P, Zhou XM, Liu D, Zhong JC, Zhang CJ, Jin LJ, Yu HM (2018) Relationship between genetic variants of ACE2 gene and circulating levels of ACE2 and its metabolites. J Clin Pharm Ther 43(2):189–195. https://doi.org/10.1111/jcpt.12625
Walther T, Wessel N, Kang N, Sander A, Tschope C, Malberg H, Bader M, Voss A (2000) Altered heart rate and blood pressure variability in mice lacking the Mas protooncogene. Braz J Med Biol Res 33(1):1–9. https://doi.org/10.1590/s0100-879x2000000100001
Wang Y, Shoemaker R, Powell D, Su W, Thatcher S, Cassis L (2017) Differential effects of Mas receptor deficiency on cardiac function and blood pressure in obese male and female mice. Am J Physiol Heart Circ Physiol 312(3):H459–H468. https://doi.org/10.1152/ajpheart.00498.2016
Hilliard LM, Mirabito KM, Denton KM (2013) Unmasking the potential of the angiotensin AT2 receptor as a therapeutic target in hypertension in men and women: what we know and what we still need to find out. Clin Exp Pharmacol Physiol 40(8):542–550. https://doi.org/10.1111/1440-1681.12067
Prabhushankar R, Krueger C, Manrique C (2014) Membrane estrogen receptors: their role in blood pressure regulation and cardiovascular disease. Curr Hypertens Rep 16(1):408. https://doi.org/10.1007/s11906-013-0408-6
Robinet P, Milewicz DM, Cassis LA, Leeper NJ, Lu HS, Smith JD (2018) Consideration of sex differences in design and reporting of experimental arterial pathology studies-statement from ATVB council. Arterioscler Thromb Vasc Biol 38(2):292–303. https://doi.org/10.1161/ATVBAHA.117.309524
Henriques T, Zhang X, Yiannikouris FB, Daugherty A, Cassis LA (2008) Androgen increases AT1a receptor expression in abdominal aortas to promote angiotensin II-induced AAAs in apolipoprotein E-deficient mice. Arterioscler Thromb Vasc Biol 28(7):1251–1256. https://doi.org/10.1161/ATVBAHA.107.160382
Lo RC, Schermerhorn ML (2016) Abdominal aortic aneurysms in women. J Vasc Surg 63(3):839–844. https://doi.org/10.1016/j.jvs.2015.10.087
Thatcher SE, Zhang X, Woody S, Wang Y, Alsiraj Y, Charnigo R, Daugherty A, Cassis LA (2015) Exogenous 17-beta estradiol administration blunts progression of established angiotensin II-induced abdominal aortic aneurysms in female ovariectomized mice. Biol Sex Differ 6:12. https://doi.org/10.1186/s13293-015-0030-1
Daugherty A, Manning MW, Cassis LA (2001) Antagonism of AT2 receptors augments angiotensin II-induced abdominal aortic aneurysms and atherosclerosis. Br J Pharmacol 134(4):865–870. https://doi.org/10.1038/sj.bjp.0704331
Li W, Li J, Hao P, Chen W, Meng X, Li H, Zhang Y, Zhang C, Yang J (2016) Imbalance between angiotensin II and angiotensin-(1-7) in human coronary atherosclerosis. J Renin Angiotensin Aldosterone Syst. https://doi.org/10.1177/1470320316659618
Thatcher SE, Zhang X, Howatt DA, Yiannikouris F, Gurley SB, Ennis T, Curci JA, Daugherty A, Cassis LA (2014) Angiotensin-converting enzyme 2 decreases formation and severity of angiotensin II-induced abdominal aortic aneurysms. Arterioscler Thromb Vasc Biol 34(12):2617–2623. https://doi.org/10.1161/ATVBAHA.114.304613
Stegbauer J, Thatcher SE, Yang G, Bottermann K, Rump LC, Daugherty A, Cassis LA (2019) Mas receptor deficiency augments angiotensin II-induced atherosclerosis and aortic aneurysm ruptures in hypercholesterolemic male mice. J Vasc Surg 70(5):1658–1668.e1. https://doi.org/10.1016/j.jvs.2018.11.045
Bihl JC, Zhang C, Zhao Y, Xiao X, Ma X, Chen Y, Chen S, Zhao B, Chen Y (2015) Angiotensin-(1-7) counteracts the effects of Ang II on vascular smooth muscle cells, vascular remodeling and hemorrhagic stroke: role of the NFsmall ka, CyrillicB inflammatory pathway. Vascul Pharmacol 73:115–123. https://doi.org/10.1016/j.vph.2015.08.007
Rosenkranz S (2004) TGF-beta1 and angiotensin networking in cardiac remodeling. Cardiovasc Res 63(3):423–432. https://doi.org/10.1016/j.cardiores.2004.04.030
Keller KM, Howlett SE (2016) Sex differences in the biology and pathology of the aging heart. Can J Cardiol 32(9):1065–1073. https://doi.org/10.1016/j.cjca.2016.03.017
Mathieu S, El Khoury N, Rivard K, Paradis P, Nemer M, Fiset C (2018) Angiotensin II overstimulation leads to an increased susceptibility to dilated cardiomyopathy and higher mortality in female mice. Sci Rep 8(1):952. https://doi.org/10.1038/s41598-018-19436-5
Kratky V, Kikerlova S, Huskova Z, Sadowski J, Kolar F, Cervenka L (2019) Enhanced renal vascular responsiveness to angiotensin II and Norepinephrine: a unique feature of female rats with congestive heart failure. Kidney Blood Press Res 44(5):1128–1141. https://doi.org/10.1159/000502379
Jessup M, Brozena S (2003) Heart failure. N Engl J Med 348(20):2007–2018. https://doi.org/10.1056/NEJMra021498
Aurigemma GP, Silver KH, McLaughlin M, Mauser J, Gaasch WH (1994) Impact of chamber geometry and gender on left ventricular systolic function in patients > 60 years of age with aortic stenosis. Am J Cardiol 74(8):794–798. https://doi.org/10.1016/0002-9149(94)90437-5
Cramariuc D, Rogge BP, Lonnebakken MT, Boman K, Bahlmann E, Gohlke-Barwolf C, Chambers JB, Pedersen TR, Gerdts E (2015) Sex differences in cardiovascular outcome during progression of aortic valve stenosis. Heart 101(3):209–214. https://doi.org/10.1136/heartjnl-2014-306078
Olivetti G, Melissari M, Capasso JM, Anversa P (1991) Cardiomyopathy of the aging human heart. Myocyte loss and reactive cellular hypertrophy. Circ Res 68(6):1560–1568. https://doi.org/10.1161/01.res.68.6.1560
Gerdts E, Okin PM, de Simone G, Cramariuc D, Wachtell K, Boman K, Devereux RB (2008) Gender differences in left ventricular structure and function during antihypertensive treatment: the Losartan Intervention for Endpoint Reduction in Hypertension Study. Hypertension 51(4):1109–1114. https://doi.org/10.1161/HYPERTENSIONAHA.107.107474
Hudson M, Rahme E, Behlouli H, Sheppard R, Pilote L (2007) Sex differences in the effectiveness of angiotensin receptor blockers and angiotensin converting enzyme inhibitors in patients with congestive heart failure–a population study. Eur J Heart Fail 9(6–7):602–609. https://doi.org/10.1016/j.ejheart.2007.02.001
Ferreira AJ, Jacoby BA, Araujo CA, Macedo FA, Silva GA, Almeida AP, Caliari MV, Santos RA (2007) The nonpeptide angiotensin-(1-7) receptor Mas agonist AVE-0991 attenuates heart failure induced by myocardial infarction. Am J Physiol Heart Circ Physiol 292(2):H1113–1119. https://doi.org/10.1152/ajpheart.00828.2006
Grobe JL, Mecca AP, Lingis M, Shenoy V, Bolton TA, Machado JM, Speth RC, Raizada MK, Katovich MJ (2007) Prevention of angiotensin II-induced cardiac remodeling by angiotensin-(1-7). Am J Physiol Heart Circ Physiol 292(2):H736–742. https://doi.org/10.1152/ajpheart.00937.2006
Yamamoto K, Ohishi M, Katsuya T, Ito N, Ikushima M, Kaibe M, Tatara Y, Shiota A, Sugano S, Takeda S, Rakugi H, Ogihara T (2006) Deletion of angiotensin-converting enzyme 2 accelerates pressure overload-induced cardiac dysfunction by increasing local angiotensin II. Hypertension 47(4):718–726. https://doi.org/10.1161/01.HYP.0000205833.89478.5b
Wang J, Li N, Gao F, Song R, Zhu S, Geng Z (2015) Balance between angiotensin converting enzyme and angiotensin converting enzyme 2 in patients with chronic heart failure. J Renin Angiotensin Aldosterone Syst 16(3):553–558. https://doi.org/10.1177/1470320315576257
Sama IE, Ravera A, Santema BT, van Goor H, Ter Maaten JM, Cleland JGF, Rienstra M, Friedrich AW, Samani NJ, Ng LL, Dickstein K, Lang CC, Filippatos G, Anker SD, Ponikowski P, Metra M, van Veldhuisen DJ, Voors AA (2020) Circulating plasma concentrations of angiotensin-converting enzyme 2 in men and women with heart failure and effects of renin–angiotensin-aldosterone inhibitors. Eur Heart J 41(19):1810–1817. https://doi.org/10.1093/eurheartj/ehaa373
Mosca L, Barrett-Connor E, Wenger NK (2011) Sex/gender differences in cardiovascular disease prevention: what a difference a decade makes. Circulation 124(19):2145–2154. https://doi.org/10.1161/CIRCULATIONAHA.110.968792
Rabi DM, Khan N, Vallee M, Hladunewich MA, Tobe SW, Pilote L (2008) Reporting on sex-based analysis in clinical trials of angiotensin-converting enzyme inhibitor and angiotensin receptor blocker efficacy. Can J Cardiol 24(6):491–496. https://doi.org/10.1016/s0828-282x(08)70624-x
Sullivan JC (2008) Sex and the renin–angiotensin system: inequality between the sexes in response to RAS stimulation and inhibition. Am J Physiol Regul Integr Comp Physiol 294(4):R1220–1226. https://doi.org/10.1152/ajpregu.00864.2007
Kostis WJ, Shetty M, Chowdhury YS, Kostis JB (2018) ACE inhibitor-induced angioedema: a review. Curr Hypertens Rep 20(7):55. https://doi.org/10.1007/s11906-018-0859-x
Song JJ, Ma Z, Wang J, Chen LX, Zhong JC (2020) Gender differences in hypertension. J Cardiovasc Transl Res 13(1):47–54. https://doi.org/10.1007/s12265-019-09888-z
Miller JA, Cherney DZ, Duncan JA, Lai V, Burns KD, Kennedy CR, Zimpelmann J, Gao W, Cattran DC, Scholey JW (2006) Gender differences in the renal response to renin–angiotensin system blockade. J Am Soc Nephrol 17(9):2554–2560. https://doi.org/10.1681/ASN.2005101095
Wang H, Chen H (2016) Gender difference in the response to valsartan/amlodipine single-pill combination in essential hypertension (China Status II): an observational study. J Renin Angiotensin Aldosterone Syst 17(2):1470320316643903. https://doi.org/10.1177/1470320316643903
Calhoun DA, Sharma K (2010) The role of aldosteronism in causing obesity-related cardiovascular risk. Cardiol Clin 28(3):517–527. https://doi.org/10.1016/j.ccl.2010.04.001
Goodfriend TL, Kelley DE, Goodpaster BH, Winters SJ (1999) Visceral obesity and insulin resistance are associated with plasma aldosterone levels in women. Obes Res 7(4):355–362. https://doi.org/10.1002/j.1550-8528.1999.tb00418.x
Shukri MZ, Tan JW, Manosroi W, Pojoga LH, Rivera A, Williams JS, Seely EW, Adler GK, Jaffe IZ, Karas RH, Williams GH, Romero JR (2018) Biological sex modulates the adrenal and blood pressure responses to angiotensin II. Hypertension 71(6):1083–1090. https://doi.org/10.1161/HYPERTENSIONAHA.117.11087
Bangalore S, Kumar S, Messerli FH (2010) Angiotensin-converting enzyme inhibitor associated cough: deceptive information from the Physicians’ Desk Reference. Am J Med 123(11):1016–1030. https://doi.org/10.1016/j.amjmed.2010.06.014
Loloi J, Miller AJ, Bingaman SS, Silberman Y, Arnold AC (2018) Angiotensin-(1-7) contributes to insulin-sensitizing effects of angiotensin-converting enzyme inhibition in obese mice. Am J Physiol Endocrinol Metab 315(6):E1204–E1211. https://doi.org/10.1152/ajpendo.00281.2018
Schuchard J, Winkler M, Stolting I, Schuster F, Vogt FM, Barkhausen J, Thorns C, Santos RA, Bader M, Raasch W (2015) Lack of weight gain after angiotensin AT1 receptor blockade in diet-induced obesity is partly mediated by an angiotensin-(1–7)/Mas-dependent pathway. Br J Pharmacol 172(15):3764–3778. https://doi.org/10.1111/bph.13172
Benter IF, Yousif MH, Anim JT, Cojocel C, Diz DI (2006) Angiotensin-(1-7) prevents development of severe hypertension and end-organ damage in spontaneously hypertensive rats treated with L-NAME. Am J Physiol Heart Circ Physiol 290(2):H684–691. https://doi.org/10.1152/ajpheart.00632.2005
Acknowledgements
ACA is supported by NIH Grants R00HL122507 and UL1TR002014.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Medina, D., Mehay, D. & Arnold, A.C. Sex differences in cardiovascular actions of the renin–angiotensin system. Clin Auton Res 30, 393–408 (2020). https://doi.org/10.1007/s10286-020-00720-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10286-020-00720-2