Abstract
Background
Chronic smoking adversely affects peripheral vasculature. The aim of the present study was to investigate the effect of chronic cigarette smoking on rectal microvascular blood flow.
Methods
Rectal mucosal blood flow (MBF) was measured in 80 subjects (44 smokers and 36 non-smokers). The MBF was measured in the four quadrants of the rectum by laser Doppler flowmetry.
Results
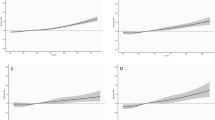
Rectal perfusion was found to be significantly lower in posterior midline compared to the other sites. In chronic smokers the observed MBF measured at the posterior and ventral sites was significantly lower compared to non-smokers (P = 0.04 and P = 0.03, respectively).
Conclusions
Our results suggest that rectal mucosal blood flow is reduced in chronic smokers.

Similar content being viewed by others
References
Price JF, Mowbray PI, Lee AJ, Rumley A, Lowe GD, Fowkes FG (1999) Relationship between smoking and cardiovascular risk factors in the development of peripheral arterial disease and coronary artery disease: Edinburgh Artery Study. Eur Heart J 20:344–353
Fowkes FG, Housley E, Cawood EH, Macintyre CC, Ruckley CV, Prescott RJ (1991) Edinburgh Artery Study: prevalence of asymptomatic and symptomatic peripheral arterial disease in the general population. Int J Epidemiol 20:384–392
Emmanuel AV, Kamm MA (1999) Laser Doppler measurement of rectal mucosal blood flow. Gut 45:64–69
van Adrichem LN, Hovius SE, van Strik R, van der Meulen JC (1992) Acute effects of cigarette smoking on microcirculation of the thumb. Br J Plast Surg 45:9–11
Tottrup A, Frost L (2005) Pelvic sepsis after extended Hartmann’s procedure. Dis Colon Rectum 48:251–255
Sørensen LT, Jørgensen T, Kirkeby LT, Skovdal J, Vennits B, Wille-Jørgensen P (1999) Smoking and alcohol abuse are major risk factors for anastomotic leakage in colorectal surgery. Br J Surg 86:927–931
Fawcett A, Shembekar M, Church JS, Vashisht R, Springall RG, Nott DM (1996) Smoking, hypertension, and colonic anastomotic healing: a combined clinical and histopathological study. Gut 38:714–718
Zimmerman DD, Gosselink MP, Mitalas LE et al (2005) Smoking impairs rectal mucosal bloodflow—a pilot study: possible implications for transanal advancement flap repair. Dis Colon Rectum 48:1228–1232
Klosterhalfen B, Vogel P, Rixen H, Mittermayer C (1989) Topography of the inferior rectal artery: a possible cause of chronic, primary anal fissure. Dis Colon Rectum 32:43–52
Schouten WR, Briel JW, Auwerda JJ (1994) Relationship between anal pressure and anodermal blood flow. The vascular pathogenesis of anal fissures. Dis Colon Rectum 37:664–669
Collins EE, Lund JN (2007) A review of chronic anal fissure management. Tech Coloproctol 11:209–223
Matzel KE, Stadelmaier U, Muehldorfer S, Hohenberger W (1997) Continence after colorectal reconstruction following resection: impact of level of anastomosis. Int J Colorectal Dis 12:82–87
Montesani C, Pronio A, Santella S et al (2004) Rectal cancer surgery with sphincter preservation: functional results related to the level of anastomosis. Clinical and instrumental study. Hepatogastroenterology 51:718–721
Matthiessen P, Hallböök O, Andersson M, Rutegård J, Sjödahl R (2004) Risk factors for anastomotic leakage after anterior resection of the rectum. Colorectal Dis 6:462–469
Eriksen MT, Wibe A, Norstein J et al (2005) Anastomotic leakage following routine mesorectal excision for rectal cancer in a national cohort of patients. Colorectal Dis 7:51–57
Walker KG, Bell SW, Rickard MJ et al (2004) Anastomotic leakage is predictive of diminished survival after potentially curative resection for colorectal cancer. Ann Surg 240:255–259
Kruschewski M, Rieger H, Pohlen U, Hotz HG, Buhr HJ (2007) Risk factors for clinical anastomotic leakage and postoperative mortality in elective surgery for rectal cancer. Int J Colorectal Dis 22:919–927
Rullier E, Laurent C, Garrelon JL, Michel P, Saric J, Parneix M (1998) Risk factors for anastomotic leakage after resection of rectal cancer. Br J Surg 85:355–358
Prins HA, Gosselink MP, Mitales LE et al (2005) The effect of oral administration of l-arginine on anal resting pressure and anodermal blood flow in healthy volunteers. Tech Coloproctol 9:229–232 (discussion 232–233)
Buise MP, Ince C, Tilanus HW, Klein J, Gommers D, van Bommel J (2005) The effect of nitroglycerin on microvascular perfusion and oxygenation during gastric tube reconstruction. Anesth Analg 100:1107–1111
Monfrecola G, Riccio G, Savarese C, Posteraro G, Procaccini EM (1998) The acute effect of smoking on cutaneous microcirculation blood flow in habitual smokers and nonsmokers. Dermatology 197:115–118
Petschke FT, Engelhardt TO, Ulmer H, Piza-Katzer H (2006) Effect of cigarette smoking on skin perfusion of the hand. Chirurg 77:1022–1026
Mavropoulos A, Aars H, Brodin P (2003) Hyperaemic response to cigarette smoking in healthy gingiva. J Clin Periodontol 30:214–221
Meekin TN, Wilson RF, Scott DA, Ide M, Palmer RM (2000) Laser Doppler flowmeter measurement of relative gingival and forehead skin blood flow in light and heavy smokers during and after smoking. J Clin Periodontol 27:236–242
Pellaton C, Kubli S, Feihl F, Waeber B (2002) Blunted vasodilatory responses in the cutaneous microcirculation of cigarette smokers. Am Heart J 144:269–274
Tur E, Yosipovitch G, Oren-Vulfs S (1992) Chronic and acute effects of cigarette smoking on skin blood flow. Angiology 43:328–335
Vignali A, Gianotti L, Braga M, Radaelli G, Malvezzi L, Di Carlo V (2000) Altered microperfusion at the rectal stump is predictive for rectal anastomotic leak. Dis Colon Rectum 43:76–82
Hallbook O, Johansson K, Sjodahl R (1996) Laser Doppler blood flow measurement in rectal resection for carcinoma—comparison between the straight and colonic J pouch reconstruction. Br J Surg 83:389–392
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
De Bruin, A.F.J., Schouten, S.B., de Kort, P.P.S. et al. The impact of chronic smoking on rectal mucosal blood flow. Tech Coloproctol 13, 269–272 (2009). https://doi.org/10.1007/s10151-009-0529-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-009-0529-8