Abstract
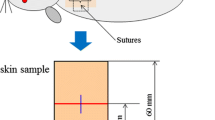
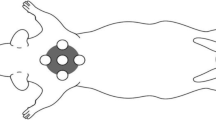
A 980-nm diode laser is proposed to be an alternative welding laser in dermatology due to its optimal penetration in tissue. An in vivo predosimetry study was done to estimate the optimal laser energy delivery conditions (6 W, 400 ms). Next, in vivo experiments were comparatively performed to examine healing of wounds closed either with suture or laser welding. One-centimeter-long, full-thickness incisions were done on the dorsal side of Wistar rats. Wounds were surgically removed at 1, 4, 7, 14, and 21 days postoperatively. Macroscopic examinations showed that welding had minimal scarring and a fine quality healing. According to histological (hematoxylin and eosin staining) results, change of epidermal thickness and granulation tissue formation through 21 days of healing period showed similarities in both methods. Epidermal thickness of welded wounds decreased from 62.46±6.87 μm (first day) to 36.49±0.92 μm (21st day) and that of sutured wounds decreased from 62.94±13.53 μm (first day) to 37.88±7.41 μm (21st day). At day 14, epidermal thickness of sutured wounds (61.20±6.60 μm) were higher than welded wounds (49.69±6.31 μm) (p<0.05). Besides, granulation values were greater for the sutured wounds but the difference was statistically significant (p<0.05) only for the seventh day (197,190.29±.89,554.96 μm2 for sutured wounds, 138,433.1±51,077.17 μm2 for welded wounds). Those differences indicate a faster recovery with laser welding. It is concluded that tissue welding with a 980-nm diode laser can be a good candidate for tissue welding applications with accelerated and improved healing, but further investigations are in progress for clinical use.





Similar content being viewed by others
References
Welch AJ, Torres JH, Cheong WF (1989) Laser physics and laser-tissue interaction. Texas Heart Inst J 16:141–149
Bleustein CB, Walker CN, Felsen D, Poppas DP (2000) Semi-solid albumin solder improved mechanical properties for laser tissue welding. Lasers Surg Med 27:140–146
Schober R, Ulrich F, Sander T, Dürselen H, Hessel S (1986) Laser-induced alteration of collagen substructure allows microsurgical tissue welding. Science 232:1421–1422
Tang J, Godlewski G, Rouy S, Delacretaz G (1997) Morphologic changes in collagen fibers after 830-nm diode laser welding. Lasers Surg Med 21:438–443
Bass LS, Treat MR (1995) Laser tissue welding: a comprehensive review of current and future clinical applications. Lasers Surg Med 17:315–349
Talmor M, Bleustein CB, Poppas DP (2001) Laser tissue welding: a biotechnological advance for the future. Arch Facial Plast Surg 3:207–213
McNally KM, Sorg BS, Chan EK, Welch AJ, Dawes JM, Owen ER (1999) Optimal parameters for laser tissue soldering. Part I: tensile strength and scanning electron microscopy analysis. Lasers Surg Med 24:319–331
McNally KM, Sorg BS, Chan EK, Welch AJ, Dawes JM, Owen ER (2000) Optimal parameters for laser tissue soldering: II. Premixed versus separate dye-solder techniques. Lasers Surg Med 26:346–356
Duck FA (1990) Physical properties of tissue: a comprehensive reference book. Academic, Cambridge
Niemz MH (1996) Laser-tissue interactions. Springer, Berlin Heidelberg New York
Prasad PN (2003) Introduction to biophotonics. Wiley Interscience, USA
Çilesiz I, Thomsen S, Welch AJ, Chan EK (1997) Controlled temperature tissue fusion: Ho:YAG laser welding of rat intestine in vivo, part two. Lasers Surg Med 21:278–286
Ott B, Züger BJ, Erni D, Banic A, Schaffner T, Weber HP, Frenz M (2001) Comparative in vitro study of tissue welding using a 808 nm diode laser and a Ho:YAG laser. Lasers Med Sci 16:260–266
Simhon D, Ravid A, Halpern M, Cilesiz I, Brosh T, Kariv N, Leviav A, Katzir A (2001) Laser soldering of rat skin, using fiberoptic temperature controlled system. Lasers Surg Med 29:265–273
Simhon D, Brosh T, Halpern M, Ravid A, Vasilyev T, Kariv N, Katzir A, Nevo Z (2004) Closure of skin incisions in rabbits by laser soldering: I: wound healing pattern. Lasers Surg Med 35:1–11
Brosh T, Simhon D, Halpern M, Ravid A, Vasilyev T, Kariv N, Katzir A, Nevo Z (2004) Closure of skin incisions in rabbits by laser soldering: II: tensile strength. Lasers Surg Med 35:12–17
Forer B, Vasilyev T, Brosh T, Kariv N, Gil Z, Fliss DM, Katzir A (2005) Repair of pig dura in vivo using temperature controlled CO2 laser soldering. Lasers Surg Med 37(4):286–292
Peavy GM (2002) Lasers and laser-tissue interaction. Vet Clin North Am Small Anim Pract 32(3):517–534
Fried NM, Walsh JT (2000) Laser skin welding: in vivo tensile strength and wound healing results. Lasers Surg Med 27:55–65
Bleustein CB, Felsen D, Poppas DP (2000) Welding characteristics of different albumin species with and without fatty acids. Lasers Surg Med 27:82–86
Small W 4th, Heredia NJ, Maitland DJ, Da Silva LB, Matthews DL (1997) Dye-enhanced protein solders and patches in laser-assisted tissue welding. J Clin Laser Med Surg 15(5):205–208
DeCoste SD, Farinelli W, Flotte T, Anderson RR (1992) Dye-enhanced laser welding for skin closure. Lasers Surg Med 12:25–32
Bozkulak O, Tabakoglu HO, Aksoy A, Kurtkaya O, Sav A, Canbeyli R, Gulsoy M (2004) The 980-nm diode laser for brain surgery: histopathology and recovery period. Lasers Med Sci 19:41–47
Gulsoy M, Celikel TA, Kurtkaya O, Sav A, Kurt A, Canbeyli R, Cilesiz I (1999) Application of the 980-nm diode laser in stereotaxic surgery. IEEE J Sel Top Quantum Electron 5(2):1090–1094
Capon A, Souil E, Gauthier B, Sumian C, Bachelet M, Buys B, Polla BS, Mordon S (2001) Laser assisted skin closure (LASC) by using a 815-nm diode laser system accelerates and improves wound healing. Lasers Surg Med 28:168–175
Kirsch AJ, Duckett JW, Snyder HM, Canning DA, Harshaw DW, Howard P, Macarak EJ, Zderic SA (1997) Skin flap closure by dermal laser soldering: a wound healing model for sutureless hypospadias repair. Urology 50(2):263–272
Acknowledgements
This work is supported by TUBITAK project 104M428 (to Murat Gulsoy). Rats were obtained from Psychobiology Laboratory, Bogazici University and histological examinations were done at Oruc Pathology Laboratory, Istanbul, Turkey. The experiments were conducted under a protocol approved by the Institutional Animal Research and Care Ethic Committee at Bogazici University. The 980-nm diode laser was borrowed from Dr. Inci.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gulsoy, M., Dereli, Z., Tabakoglu, H.O. et al. Closure of skin incisions by 980-nm diode laser welding. Lasers Med Sci 21, 5–10 (2006). https://doi.org/10.1007/s10103-006-0375-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-006-0375-0