Abstract
Introduction
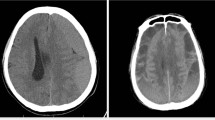
Chronic subdural haematoma (CSDH) is one of the most common neurosurgical pathologies. The recurrence of chronic subdural haematomas is an important concern, considering that elderly patients are the most affected and reoperations in these patients may represent a risk of neurological and clinical complications. In accordance with the inflammatory theory regarding CSDH and its recurrence, we aimed to evaluate the role of an inflammatory marker, neutrophil-to-lymphocyte ratio (NLR), as a risk factor and prognostic variable for CSDH recurrence.
Methods
We performed a cohort study of adult patients operated for post-traumatic CSDH traumatic CSDH between January 2015 and December 2019 in our neurotrauma unit, whose data was retrospectively retrieved. We excluded patients with previous inflammatory or infectious diseases as well as use of anticoagulant/antiplatelet medications. Neutrophil and lymphocyte counts were obtained 24 h preoperatively and 48–72 h postoperatively. The primary endpoint was symptomatic recurrence of CSDH up to 1 year after the surgery. An independent sample was used to validate the findings.
Results
The testing sample comprised 160 patients (59.4% male, mean age 69.3 ± 14.3 years, recurrence rate 22.5%). Postoperative neutrophil count and NLR were higher in those who recurred, as well as the neutrophils (median 1.15 vs 0.96, p = 0.022) and NLR (median 1.29 vs 0.79, p = 0.001) postoperative-to-preoperative ratios. Preoperative laboratory parameters or other baseline variables were not associated with recurrence. Postoperative NLR ratio (each additional unit, OR 2.53, 95% CI 1.37–4.67, p = 0.003) was independently associated with recurrence. The best cut-off for the postoperative NLR ratio was 0.995 (AUC-ROC 0.67, sensitivity 63.9%, specificity 76.6%). Postoperative NLR ratio ≥ 1 (i.e. a post-operative NLR that does not decrease compared to the preoperative value) was associated with recurrence (OR 4.59, 95% CI 2.00–10.53, p < 0.001). The validation sample analysis (66 patients) yielded similar results (AUC-ROC 0.728, 95% CI 0.594–0.862, p = 0.002) and similar cut-off (≥ 1.05, sensitivity 77.8%, specificity 66.7%).
Conclusion
NLR ratio can be a useful parameter for the prediction of post-traumatic CSDH recurrence. This hypothesis was validated in an independent sample and the accuracy was moderate.






Similar content being viewed by others
References
Miranda LB, Braxton E, Hobbs J, Quigley MR (2011) Chronic subdural hematoma in the elderly: not a benign disease. J Neurosurg 114(1):72–76
Kolias AG, Chari A, Santarius T, Hutchinson PJ (2014) Chronic subdural haematoma: modern management and emerging therapies. Nat Rev Neurol 10(10):570–578
Mori K, Maeda M (2001) Surgical treatment of chronic subdural hematoma in 500 consecutive cases: clinical characteristics, surgical outcome, complications, and recurrence rate. Neurol Med Chir 41(8):371–381
Balser D, Farooq S, Mehmood T, Reyes M, Samadani U (2015) Actual and projected incidence rates for chronic subdural hematomas in United States Veterans Administration and civilian populations. J Neurosurg 123(5):1209–1215
Karibe H, Kameyama M, Kawase M, Hirano T, Kawaguchi T, Tominaga T (2011) Epidemiology of chronic subdural hematoma. No Shinkei Geka 39(12):1149–1153
Kageyama H, Toyooka T, Tsuzuki N, Oka K (2013) Nonsurgical treatment of chronic subdural hematoma with tranexamic acid. J Neurosurg 119(2):332–337
Guha D, Coyne S, Macdonald RL (2016) Timing of the resumption of antithrombotic agents following surgical evacuation of chronic subdural hematomas: a retrospective cohort study. J Neurosurg 124(3):750–759
Almenawer, S.A., Farrokhyar, F., Hong, C., Alhazzani, W., Manoranjan, B., Yarascavitch, B., Arjmand, P., Baronia, B., Reddy, K., Murty, N. and Singh, S., (2014) Chronic subdural hematoma management: a systematic review and meta-analysis of 34829 patients
Glancz LJ, Poon MTC, Hutchinson PJ, Kolias AG, Brennan PM, Collaborative BNTR (2020) Drains result in greater reduction of subdural width and midline shift in burr hole evacuation of chronic subdural haematoma. Acta Neurochir 162(6):1455–1466
Tao C, Wang J, Hu X, Ma J, Li H, You C (2017) Clinical value of neutrophil to lymphocyte and platelet to lymphocyte ratio after aneurysmal subarachnoid hemorrhage. Neurocrit Care 26(3):393–401
Trotter W (1914) Chronic subdural haemorrhage of traumatic origin, and its relation to pachymeningitis haemorrhagica interna. Br J Surg 2(6):271–291
Edlmann E, Giorgi-Coll S, Whitfield PC, Carpenter KL, Hutchinson PJ (2017) Pathophysiology of chronic subdural haematoma: inflammation, angiogenesis and implications for pharmacotherapy. J Neuroinflammation 14(1):1–13
Sato S, Suzuki J (1975) Ultrastructural observations of the capsule of chronic subdural hematoma in various clinical stages. J Neurosurg 43(5):569–578
Dilektasli E, Inaba K, Haltmeier T, Wong MD, Clark D, Benjamin ER, Lam L, Demetriades D (2016) The prognostic value of neutrophil-to-lymphocyte ratio on mortality in critically ill trauma patients. J Trauma Acute Care Surg 81(5):882–888
Dong CH, Wang ZM, Chen SY (2018) Neutrophil to lymphocyte ratio predict mortality and major adverse cardiac events in acute coronary syndrome: A systematic review and meta-analysis. Clin Biochem 52:131–136
Chen W, Yang J, Li B, Peng G, Li T, Li L, Wang S (2018) Neutrophil to lymphocyte ratio as a novel predictor of outcome in patients with severe traumatic brain injury. J Head Trauma Rehabil 33(1):E53–E59
Tao C, Hu X, Wang J, Ma J, Li H, You C (2017) Admission neutrophil count and neutrophil to lymphocyte ratio predict 90-day outcome in intracerebral hemorrhage. Biomark Med 11(1):33–42
Torihashi K, Sadamasa N, Yoshida K, Narumi O, Chin M, Yamagata S (2008) Independent predictors for recurrence of chronic subdural hematoma: a review of 343 consecutive surgical cases. Neurosurgery 63(6):1125–1129
Yang W, Huang J (2017) Chronic subdural hematoma: epidemiology and natural history. Neurosurg Clin 28(2):205–210
Edlmann E, Holl DC, Lingsma HF, Bartek J, Bartley A, Duerinck J, Jensen TSR, Soleman J, Shanbhag NC, Devi BI, Laeke T (2020) Systematic review of current randomised control trials in chronic subdural haematoma and proposal for an international collaborative approach. Acta Neurochir 1–14
Edlmann E, Thelin EP, Caldwell K, Turner C, Whitfield P, Bulters D, Holton P, Suttner N, Owusu-Agyemang K, Al-Tamimi YZ, Gatt D (2019) Dex-CSDH randomised, placebo-controlled trial of dexamethasone for chronic subdural haematoma: report of the internal pilot phase. Sci Rep 9(1):1–13
Guthrie GJ, Charles KA, Roxburgh CS, Horgan PG, McMillan DC, Clarke SJ (2013) The systemic inflammation-based neutrophil–lymphocyte ratio: experience in patients with cancer. Crit Rev Oncol Hematol 88(1):218–230
Zhang Y, Yang Y, Long S, Li G (2020) Assessment of peripheral blood cell inflammatory markers in patients with chronic subdural hematoma. Clin Neurol Neurosurg 191:105738
Frati A, Salvati M, Mainiero F, Ippoliti F, Rocchi G, Raco A, Caroli E, Cantore G, Delfini R (2004) Inflammation markers and risk factors for recurrence in 35 patients with a posttraumatic chronic subdural hematoma: a prospective study. J Neurosurg 100(1):24–32
Kocaturk O, Besli F, Gungoren F, Kocaturk M, Tanriverdi Z (2019) The relationship among neutrophil to lymphocyte ratio, stroke territory, and 3-month mortality in patients with acute ischemic stroke. Neurol Sci 40(1):139–146
Inci I, Kusbeci OY, Eskut N (2020) The neutrophil-to-lymphocyte ratio as a marker of peripheral inflammation in progressive supranuclear palsy: a retrospective study. Neurol Sci 41(5):1233–1237
Ying A, Cheng Y, Lin Y, Yu J, Wu X, Lin Y (2020) Dynamic increase in neutrophil levels predicts parenchymal hemorrhage and function outcome of ischemic stroke with r-tPA thrombolysis. Neurol Sci 1–9
Deng QW, Gong PY, Chen XL, Liu YK, Jiang T, Zhou F et al (2020) Admission blood cell counts are predictive of stroke-associated infection in acute ischemic stroke patients treated with endovascular therapy. Neurol Sci 1–13
de Morais ANLR, Baylão VMR, Silva TM, Dos Santos AG, Azevedo M, de Oliveira AJ (2021) Is neutrophil-lymphocyte ratio a useful tool for predicting outcome in subarachnoid hemorrhage? A systematic review. Neurosurg Rev 1–6
Faria SS, Fernandes PC Jr, Silva MJB, Lima VC, Fontes W, Freitas-Junior R, Eterovic AK, Forget P (2016) The neutrophil-to-lymphocyte ratio: a narrative review. ecancermedicalscience 10
Hara M, Tamaki M, Aoyagi M, Ohno K (2009) Possible role of cyclooxygenase-2 in developing chronic subdural hematoma. J Med Dent Sci 56(3):101–106
Kudo H, Kuwamura K, Izawa I, Sawa H, Tamaki N (1992) Chronic subdural hematoma in elderly people: present status on Awaji Island and epidemiological prospect. Neurol Med Chir 32(4):207–209
Sarti C, Tuomilehto J, Salomaa V, Sivenius J, Kaarsalo E, Narva EV, Salmi K, Torppa J (1991) Epidemiology of subarachnoid hemorrhage in Finland from 1983 to 1985. Stroke 22(7):848–853
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
For this type of study, formal consent is not required.
Informed consent
Due to its observational nature and retrospective data collection, informed consent is waived for this study.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
de Oliveira, A.J.M., Solla, D.J.F., de Oliveira, K.F. et al. Postoperative neutrophil-to-lymphocyte ratio variation is associated with chronic subdural hematoma recurrence. Neurol Sci 43, 427–434 (2022). https://doi.org/10.1007/s10072-021-05241-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-021-05241-y