Abstract
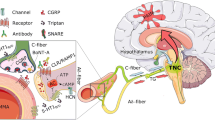
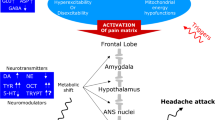
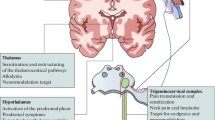
Here, in this review, we present our hypothesis of the migraine pathogenesis. We believe that migraine attacks derive from a top-down dysfunctional process that initiates in a hyperexcitable and hypoenergetic brain in the frontal lobe and downstream in abnormally activated nuclei of the pain matrix. This hypothesis derived from the results of the biochemical studies, mainly generated from our laboratory, on the possible metabolic shifts of tyrosine toward an activation of decarboxylase enzyme activity with an increased synthesis of traces amines, i.e. tyr, oct and syn, and an unphysiological synthesis of noradrenalin and dopamine. This metabolic shift is possibly favored by the reduced mitochondrial energy and high levels of glutamate in CNS of migraine patients. The unbalanced levels of neurotransmitters (DA and NE) and neuromodulators (tyr, oct and syn) in the synaptic dopaminergic and noradrenergic clefts of the pain matrix may activate, downstream, the trigeminal system that releases calcitonin gene-related G peptide. This induces the formation of an inflammatory soup, the sensitization of first trigeminal neuron and the migraine attack.
Similar content being viewed by others
References
Launer LJ, Terwindt GM, Ferrari MD (1999) The prevalence and characteristics of migraine in a population based cohort: the GEM study. Neurology 53:537–542
Welch KMA (1987) Migraine a biobehavioral disorder. Arch Neurol 44:323–327
Skinner JE, Molnar M (1983) Event related extracellular potassium ions activity changes in the frontal cortex of conscious rat. J Neurophysiol 49:204–215
Montagna P (2008) Migraine: a genetic disease? Neurol Sci 29(Suppl 1):S47–S51
Ziegler DK, Paolo AM (1995) Headache symptoms and psychological profile of headache-prone individuals: a comparison of clinic patients and controls. Arch Neurol 52:602–606
D’Andrea G, Perini F, Terrazzino S, Nordera GP (2004) Contributions of biochemistry to the pathogenesis of primary headaches. Neurol Sci 3(Suppl 3):589–592
D’Andrea G, Cananzi AR, Ferro Milone F, JosephR GrunfeldS, Welch KMA (1989) Platelet levels of glutamate and aspartate in normal subjects. Stroke 20(2):299–300
Millan MJ (2002) Descending control of pain. Prog Neurobiol 66:355–474
D’Andrea G, Nordera GP, Perini F, Allais G, Granella F (2007) Biochemistry of neuro-modulation in primary headaches: focus on tyrosine metabolism. Neurol Sci 28(Suppl 2):S94–S96
D’Andrea G, Terrazzino S, Fortin D, Cocco P, Balbi T (2003) Elusive amines and primary headaches: historical background and prospectives. Neurol Sci 24:S65–S67
Axelrod J, Saavedra JM (1977) Octopamine. Nature 265:501–504
Sever PS (1979) False transmitters and migraine. Lancet 1(8111):333
Borowsky B, Adham N, Jones KA et al (2001) Trace amines: identification of a family of mammalian G protein-coupled receptors. Proc Natl Acad Sci USA 98:933–941
Berry DB (2004) Mammalian central nervous system trace amines. Pharmacologic amphetamines, physiologic neuromodulators. J Neurochem 90:257–271
(2004) The international classification of headache disorders. Cephalalgia 24:1–160
Lashley KS (1941) Patterns of cerebral integration indicated by the scotomatas of migraine. Arch Neurol Psychiatry 46:331–339
Olesen J, Larsen B, Luritzen M (1981) Focal hyperemia followed by spreading olegimia an impaired activation of rCBF in classic migraine. Ann Neurol 9:344–352
Lauritzen M, Skyhoj E, Olesen J et al (1983) The role of spreading depression in acute brain disorders. Ann Neurol 14:569–572
Leao AAP (1944) Spreading depression of activity in cerebral cortex. J Neurophysiol 7:359–390
Cao Y, Welch KMA, Aurora S, Vikinsgtad EM (1999) Functional MRI-BOLD of visual triggered headache in patients with migraine. Arch Neurol 56:548–554
Welch KMA, D’Andrea G, Tepley N, Barkley G, Ramadan NM (1990) The concept of migraine as a state of central neuronal hyperexcitability. Neurol Clin 8:817–828
Van Gelder N (1987) Calcium mobility and release associated with EEG abnormalities, migraine and epilepsy. In: Andermann F, Lugaresi E (eds) Migraine and epilepsy. Butterworths, Boston, pp 367–378
Freeman M (2006) Reconsidering the effect of monosodium glutamate: a literature review. J Am Acad Nurse Pract 18(10):482–486
Mangano RM, Schwarcz R (1981) The human platelet as a model for the glutamatergic neuron. Platelet uptake of l-glutamate. J Neurochem 36(3):1067–1976
D’Andrea G, Cananzi AR, Joseph R, Morra M, Zamberaln F, Ferro Milone F, Grunfeld S, Welch KMA (1991) Platelet glycine, glutamate, and aspartate in primary headache. Cephalalgia 11:197–200
Ferrari MD, Odink J, Bos KD, Maleny MS, Bruin GW (1990) Neuroexcitatatory plasma amino acids are elevated in migraine. Neurology 40(10):1582–1586
Cananzi AR, D’Andrea G, Perini F, Zamberaln F, Welch KMA (1995) Platelet plasma levels of glutamate and glutamine in migraine with and without aura. Cephalalgia 15(2):132–135
Vaccaro M, Riva C, Tremolizzo L, Aliprandi A et al (2007) Platelet glutamate uptake and release on migraine with and without aura. Cephalalgia 27(1):35–40
Peres MF, Zukermann E, Senne Soares CA, Alonso EO, Santos BF, Faulhaber MH (2004) Cerebrospinal fluid glutamate levels in chronic migraine. Cephalalgia 24(9):735–739
Aurora SK, Ahmad BK, Welch KM, Bhardhwaj P, Ramadan NM (1998) Transcranial magnetic stimulation confirms hyperexcitability of occipital cortex in migraine. Neurology 50(4):1111–1114
Khedr EM, Ahmed MA, Mohamed KA (2006) Motor and visual cortical excitability in migraineurs patients with and without aura: transcranial magnetic stimulation. Neurophysiol Clin 36(1):13–18
Schoenen J (2006) Neurophysiological features of the migrainous brain. Neurol Sci 27(Suppl 2):S77–S81
Ramadan NM, halvorson H, Vande-Linde A, Levine SR, helpern JA, Welch KM (1989) Low brain magnesium and migraine. Headache 29(7):416–419
Van Harreveld A (1984) The nature of chick’s magnesium sensitive retinal spreading depression. J Neurobiol 15:333–334
Lees G, Leach MJ (1993) Studies on the mechanism of action of novel anticonvulsant lamotrigine (lamictal) using primary neuroglia cultures from rat cortex. Brain Res 612:190–199
Leach MJ, Lees G, Riddall DR (1995) Lamotrigine. Mechanisms of action. In: Levy RH, Mattson RH, Meldrum BS (eds) Antiepileptic drugs, 4th edn. Raven Press, New York, pp 851–859
D’Andrea G, Granella F, Cadaldini M, Manzoni GC (1999) Effectiveness of lamotrigine in the prophylaxis. Cephalalgia 19:64–66
Lampl C, Buzath A, Klinger D, Neumann K (1999) Lamotrigine in the prophylactic treatment of migraine with aura: a pilot study. Cephalalgia 19:58–63
Chen WT, Fuh JL, Wang SJ (2001) Persistent migrainous visual phenomena might be responsive to lamotrigine. Headache 41(8):823–825
Lampl C, Katsarava Z, Diener HC, Limmroth V (2005) Lamotrigine reduces migraine aura and migraine attacks in patients with migraine with aura. J Neurol Neurosurg Psychiatry 76:1730–1732
D’Andrea G, Nordera GP, Allais G (2006) Treatment of the aura: solving the puzzle. Neurol Sci 27(Suppl 2):S96–S99
Steiner TJ, Findley LJ, Yuen AW (1997) Lamotrigine versus placebo in the prophylaxis of migraine with and without aura. Cephalalgia 17(2):109–112
Bogdanov VB, Multon S, Chauvel V, Bogdanova OV, Makarchuk MY, Schoenen J (2009) Cortical spreading depression and associated neuronal Fos expression in rats are affected differentially by chronic treatment with lamotrigine, valproate or riboflavin. Cephalalgia 29(Suppl 1):10
Griffin NJ, Ruggiero L, Lipton RB, Silberstein SD et al (2003) Premonitory symptoms in migraine: an electronic diary study. Neurology 60(6):935–940
Demarquay G, Royet JP, Giroud P, Chazot G, Valade D, Ryvlin P (2006) Rating of olfactory judgement in migraine patients. Cephalalgia 26:1123–1130
Denuelle M, Fabre N, Payoux P, Chollet F, Geroud G (2007) Hypothalamic activation in spontaneous migraine attacks. Headache 47(10):1418–1426
Cologno D, Cicarelli G, Petretta V, D’Onofrio F, Bussne G (2008) High prevalence of dopaminergic premonitory symptoms in migraine patients with restless legs syndrome: a pathogenetic link? Neurol Sci 29(Suppl 1):S166–S168
D’Andrea G, Terrazzino S, Leon A, Fortin D, Perini F, Granella F, Bussone G (2204) Elevated levels of circulating trace amines in primary headaches. Neurology 62:1701–1705
D’Andrea G, Granella F, Leone M, Perini F, Farruggio A, Bussone G (2006) Abnormal platelet trace amine profiles in migraine with and without aura. Cephalalgia 26(8):968–972
Villalon CM, Olesen J (2009) The role of CGRP in the pathophysiology of migraine and efficacy of CGRP receptor antagonists as acute antimigraine drugs. Pharmacol Ther 124(3):309–323
Perini F, D’Andrea G, Galloni E, Pignatelli F, Billo G, Alba S, Bussone G, Toso V (2005) Plasma cytokine levels in migraineurs and controls. Headache 45:926–931
D’Andrea G, Cananzi AR, Perini F, Hasselmark L (1995) Platelet models and their possible usefulness in the study of migraine pathogenesis. Cephalalgia 15(4):265–271
Fusayasu E, Kowa H, Takeshima T, Nasako K, Nakashima K (2007) Increased plasma substance P and CGRP levels, and high ACE activity in migraineurs during headache free periods. Pain 128(3):209–214
Bolay N, Reuter U, Dunn AK, Huang Z, Boas DA, Moskowitz MA (2002) Intrinsic brain activity triggers trigeminal meningeal afferent in migraine model. Nat Med 8(2):136–142
Dalkara T, Zervas NT, Moskovitz MA (2006) From spreading depression to trigeminovascular system. Neurol Sci 27(Suppl 2):S86–S90
Moulton EA, Burstein R, Tully S, Hargreaves R, Becerra l, Borsok D (2008) Interictal dysfunction descending modulatory center in migraine patients. PLoS One 3(11):e3799
Fumal A, Laureys S, Di Clemente L, Boly M, Bohotin V, Vandenheede M, Coppola GL, Salmon E, Kupers R, Shoenen J (2006) Orbitofrontal cortex involvement in chronic analgesic-overuse headache evolving from episodic migraine. Brain 129:543–550
Welch KMA, Cao Y, Aurora SK, Wiggins G, Vikingstad EM (1998) MRI of the occipital cortex, red nucleus and substantia nigra during visual aura of migraine. Neurology 51:1465–1469
Willer C, May A, Limmroth V, Juptner M, Kaube H, Schayck RV, Coenen HH, Diener HC (1995) Brain stem activation in spontaneous human migraine attacks. Nat Med 1(7): 658–660
Rudling EJ, Richardson J, Evans DP (2000) A comparison of agonist-specific coupling of cloned human α2-adrenoreceptors subtypes. Br J Pharmacol 131:933–941
Altier N, Stewart J (1999) The tachinin NK-1 receptor antagonist RP-67580, infused into Ventral tegmental area prevents stress-induced analgesia in the formalin test. Physiol Behav 66:717–721
D’Andrea G, Terrazzino S, Fortin D, Farruggio A, Rinaldi L, Leon A (2003) HPLC electrochemical detection of trace amines in human plasma and platelets and expression of mRNA transcripts of trace amines receptors in circulating leukocytes. Neurosci Lett 346(1–2):89–92
Danielson TJ, Boulton AA, Robertson HS (1977) m-Octopamine, p-octopamine and phenylethylamine in mammalian brain: a sensitive, specific assay anf effects of drugs. J Neurochem 29:1131–1135
D’Andrea G, Granella F, Perini F, Farruggio A, Leone M, Bussone G (2006) Platelet levels of dopamine are increased in migraine and cluster headache. Headache 46(4):585–591
Magos A, Brincat M, Zilkha KJ, Studd JW (1985) Serum dopamine β-hydroxylase activity in menstrual migraine. J Neurol Neurosurg Psychiatry 48(4):328–331
Gallai V, Gaiti A, Sarchielli P, Coata G, Trequattrini A, Paciaroni M (1992) Evidence for an altered dopamine β-hydroxylase activity in migraine and tension type headache. Acta Neurol Scand 86:403–446
D’Andrea G, Cananzi AR, Morra M, Fornasiero S, Zamberlan F, Welch KMA et al (1989) Platelet as model to test autonomic function in migraine. Funct Neurol 4(1):79–83
Martignoni F, Blandini F, D’Andrea G et al (1990) Platelet and plasma catecholamines in migraine patients. Evidences of menstrual-related variability of the noradrenergic tone. Biogenic Amines 10:227–237
Nagel-Leiby S, D’Andrea G, Grunfeld S, Welch KMA (1990) Ovarian steroid levels in migraine with and without aura. Cephalalgia 10:147–152
Fernandez F, Lea RA, Colson NJ, Bellis C, Quinlan S, Griffits LR (2006) Association between a 19 bp deletion polymorphism at dopamine beta-hydroxylase (DBH) locus and migraine with aura. J Neurol Sci 251(1–2):118–123
Peres MFP, Sanchez del Rio M, seabra MLV, Tufik S, Abucham J, Cipolla-Neto J, Siberstein SD, Zuckermann E (2007) Hypothalamic involvement in chronic migraine. J Neurol Neurosurg Psychiatry 71:747–751
Shimazu S, Miklya I (2004) Pharmacological studies with endogenous enhancer substances: Β-phenylethylamine, tryptamine, and their synthetic derivatives. Prog Neuropsychopharmacol Biol Psychiatry 28:421–427
Sicuteri F, Testi A, Anselmi B (1961) Biochemical investigations in headache: increase of hydroyindoleacetic acid excretion during migraine attack. Int Arch Allergy 19:265–271
D’Andrea G, Hasselmark L, Cananzi AR, Alecci M, Perini F, Zamberlan F, Welch KMA (1995) Metabolism and menstrual cycle rhytmicity of serotonin in primary headaches. Headache 35(4):216–221
Fioroni L, D’Andrea G, Alecci M, Cananzi AR, Facchinetti F (1996) Platelet serotonin pathway in mestrual migraine. Cephalalgia 16(6):427–430
Andreou AP, Shields KG, Goadsby PJ (2009) GABA and valproate modulate trigeminovascular nociceptive transmission in the thalamus. Neurobiol Dis 37(2):314–323
Casucci G, Villani V, Frediani F (2008) Central Mechanism of action of antimigraine prophylactic drugs. Neurol Sci May 29(Suppl 1):S123–S126
Welch KMA, Chabi E, Nell JH, Bartosh K, Achar VS, Meyer JS (1975) Cerebrospinal fluid gamma aminobutyric acid levels and migraine. Br Med J 3(5882):516–517
Joseph R, D’Andrea G, Grunfeld S, Welch KMA (1988) Cytosolic ionized calcium homeostasis in platelet: an abnormal sensitivity to PAF-activation in migraine. Headache 28(6):396–402
D’Andrea G, Welch KMA, Riddle JM, Grunfeld S, Joseph R (1989) Platelet serotonin metabolism and ultrastructure in migraine. Arch Neurol 46(11):1187–1189
Joseph R, Welch KMA, Levine S, D’Andrea G (1986) ATP hyposecretion from platelet dense bodies—evidence for the purinergic hypothesis and a marker of migraine. Headache 26:403–410
D’Andrea G, Hasselmark L, Perini F, Alecci M, Cananzi AR, Welch KMA (1994) Platelet secretion from dense and alpha granules in vitro in migraine with and without aura. J Neurol Neurosurg Psychiatry 57(5):557–561
Sangiorgi S, Mochi M, Riva R, Cortelli P, Monari L, Pierangeli G, Montagna P (1994) Abnormal platelet mithocondrial function in patients affected by migraine with and without aura. Cephalalgia 14:31–230
Welch KMA, Ramadan MN (1995) Mitochondria, magnesium and migraine. J Neurol Sci 134(1–2):9–14
Barbiroli B, Montagna P, Cortelli P, Funicello R, Iotti S, Monari L, Pierangeli G, Zaniol P, Lugaresi E (1992) Abnormal brain and muscle energy metabolism shown by 31P magnetic resonance spectroscopy in patients affected by migraine with aura. Neurology 42(6):12091214
Yang SP, Pau KY, Spies HG (1997) Gonadectomy alters tyrosine hydroxylase and norepinephrine transporter mRNA levels in the locus coeruleus of the rabbit. J Neuroendocrinol 9(10):763–768
Virmani A, Gaetani F, Imam S, Binienda Z, Ali S (2002) The protective role of l-carnitine against neurotoxicity evoked by drug abuse, methamphetamine, could be related to mitochondrial dysfunction. Ann N Y Acad Sci 965:225–232
Balbi T, Fusco M, Vasapollo D, Boschetto R, Cocco P, Leon A, Farruggio A (2005) The presence of trace amines in postmortem cerebrospinal fluid in humans. J Forensic Sci 50(3):630–632
Welch KMA, Nagesh V, Aurora SK, Gelman N (2001) Periacqueductal gray matter dysfunction in migraine: cause or burden of illness? Headache 41:629–637
Welch KMA (2009) Iron in the migraine brain: a resilient hypothesis. Cephalalgia 29(3):283–285
Aridon P, D’Andrea G, Rigamonti A, Leone M, Casari G, Bussone G (2004) Elusive amines and cluster headache: mutational analysis of trace amine receptor cluster on chromosome 6q23. Neurol Sci 25(Suppl 3):S279–S280
David JC, Coulon JF (1985) Octopamine in invertebrates and vertebrates. Prog Neurobiol 24:141–185
Lindemann L, Ebeling M, Kratochwil NA, Bunzow JR, Grandy DK, Hoener MC (2005) Trace amine-associated receptors from structurally and functionally distinct subfamilies of novel G protein-coupled receptors. Genomics 85(3):372–385
Prescot A, Becerra L, Pendse G, Tully S, Burstein R et al (2009) Excitatory neurotransmitters in brain regions in interictal migraine patients. Mol Pain 5:34
Conflict of interest statement
The authors declare that they have no conflict of interest related to the publication of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
D’Andrea, G., Leon, A. Pathogenesis of migraine: from neurotransmitters to neuromodulators and beyond. Neurol Sci 31 (Suppl 1), 1–7 (2010). https://doi.org/10.1007/s10072-010-0267-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-010-0267-8