Abstract
Background
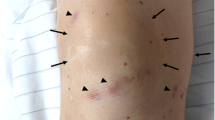
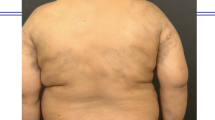
Weber-Christian disease (WCD) is an uncommon, idiopathic disease that is challenging to diagnose and has an unclear treatment protocol. We reviewed thirteen patients with WCD and analyzed their clinical characteristics. The purpose of this article was to improve the understanding of this rare disorder.
Methods
Thirteen cases of WCD were analyzed retrospectively regarding their clinical manifestation, laboratory results, misdiagnoses, therapy, and outcome.
Results
Of the thirteen patients diagnosed with WCD, the majority were female (male to female ratio, 2:11), with a mean patient age of 50.1 years. Subcutaneous nodules were the most commonly reported symptom, followed by fever, arthralgias/arthritis, and myalgia. The laboratory results were typically nonspecific. In total, 61.5% patients were misdiagnosed before pathology confirmed the diagnosis of WCD. Most patients were treated with corticosteroids and/or immunosuppressants. Two patients were treated surgically. While long-term remission was successfully achieved in some patients, others had recurrent symptoms.
Conclusion
WCD was predominantly observed in female patients in our cohort. Subcutaneous nodules and fever were the most common clinical characteristics. In addition, the patients’ laboratory test results were nonspecific, which led to a high misdiagnosis rate. In this study population, corticosteroid and/or immunosuppressant treatments were efficacious therapeutic interventions for WCD.
Key Points •Subcutaneous nodules and fever were the most common clinical characteristics in Weber-Christian panniculitis. •Misdiagnosis rate was higher in Weber-Christian panniculitis patient; tumors, bacterial infections and rheumatic diseases were the most common misdiagnoses. •Corticosteroid and/or immunosuppressant therapy was effective in most Weber-Christian panniculitis patients. |


Similar content being viewed by others
References
Wu F, Zou CC (2007) Childhood Weber-Christian disease: clinical investigation and virus detection. Acta Paediatr 96(11):1665–1669. https://doi.org/10.1111/j.1651-2227.2007.00498.x
Weber FP (1925) A case of relapsing nonsuppurative pannicultis showing phagocytosis of subcutaneous fat cells by macrophages. Br J Dermatol 37:301–311
Christian HA (1928) Relapsing febrile nodular nonsuppurative panniculitis. Arch Intern Med 42:338–351
Bailey RJ (1937) Relapsing febrile nodular nonsuppurative panniculitis (Weber-Christian disease). JAMA 109:1419–1425
Mavrikakis I, Georgiadis T, Fragiadaki K, Sfikakis PP (2010) Orbital lobular panniculitis in Weber-Christian disease: sustained response to anti-TNF treatment and review of the literature. Surv Ophthalmol 55(6):584–589. https://doi.org/10.1016/j.survophthal.2010.05.001
Panush RS, Yonker RA, Dlesk A, Longley S, Caldwell JR (1985) Weber-Christian disease, analysis of 15 cases and review of the literature. Medicine 64(3):181–191. https://doi.org/10.1097/00005792-198501000-00005
Moraes AJ, Soares PM, Zapata AL, Lotito AP, Sallum AM, Silva CA (2006) Panniculitis in childhood and adolescence. Pediatr Int 48(1):48–53. https://doi.org/10.1111/j.1442-200X.2006.02169.x
White JW, Winkelmann RK (1998) Weber-Christian panniculitis:a review of 30 cases with this diagnosis. J Am Acad Dermatol 39(1):56–62. https://doi.org/10.1016/S0190-9622(98)70402-5
Jin O, Sun LY, Lau CS (2004) Weber-Christian disease and pituitary dysfunction in a patient with polymyositis. Clin Exp Rheumatol 22(2):792. https://doi.org/10.1002/art.20755
Sugihara T, Koike R, Nosaka Y, Ogawa J, Hagiyama H, Nagasaka K, Nonomura Y, Nishio J, Nanki T, Kohsaka H, Kubota T, Miyasaka N (2002) Case of subcutaneous and mesenteric acute panniculitis with Sjogren syndrome. Nihon Rinsho Meneki Gakkai Kaishi 25(3):277–284. https://doi.org/10.2177/jsci.25.277
Wasserman JM, Thung SN, Berman R, Bodenheimer HC Jr, Sigal SH (2001) Hepatic Weber-Christian disease. Semin Liver Dis 21(1):115–118. https://doi.org/10.1055/s-2001-12934
Usuki K, Kitamura K, Urabe A, Takaku F (1998) Successful treatment of Weber-Christian disease by cyclosporin A. Am J Med 85(2):276–278. https://doi.org/10.1016/S0002-9343(88)80368-1
Ostrov BE, Athreya BH, Eichenfield AH, Goldsmith DP (1996) Successful treatment of severe cytophagic histiocytic panniculitis with cyclosporine A. Semin Athritis Rheum 25(6):404–413. https://doi.org/10.1016/S0049-0172(96)80005-9
Acknowledgments
We would like to thank Lili Yu (Department of Pathology, Zhejiang Provincial People’s Hospital, People’s Hospital of Hangzhou Medical College, Hangzhou, China) for his assistance in identifying Weber-Christian panniculitis for the present study.
Author information
Authors and Affiliations
Contributions
Wei Zheng had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Wei Zheng, Wen yuan Song, and Hongying Pan were involved in the design of the study; authors Wei Zheng and Wen yuan Song jointly completed the writing, and Qingqing Wu, Qiaoqiao Yin, and Chaolan Pan were substantially involved in revising the article.
Corresponding author
Ethics declarations
Because this study was based on the retrospective analysis of existing administrative and clinical data, the need to obtain informed patient consent was waived by the Ethics Review Committee of Zhejiang Provincial People’s Hospital.
Disclosures
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zheng, W., Song, W., Wu, Q. et al. Analysis of the clinical characteristics of thirteen patients with Weber-Christian panniculitis. Clin Rheumatol 38, 3635–3641 (2019). https://doi.org/10.1007/s10067-019-04722-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-019-04722-y