Abstract
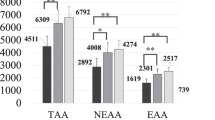
In this study, we investigated differences in amino acid losses between HD and pre-dilution on-line HDF with equal Kt/V for urea to determine which modality removes less amino acids from extravascular pools and ensures better nutrition. The subjects were patients receiving pre-dilution on-line HDF (n = 10) or HD (n = 10) at this hospital. Dialysis time was 4 h for all patients. In patients on HD, the blood flow rate was 200 mL/min and the dialysate flow rate was 463 ± 29.3 mL/min. In patients on pre-dilution on-line HDF, the blood flow rate was 240 ± 20 mL/min, the dialysate flow rate was 565.0 ± 42.5 mL/min, and the substitution flow rate (substitution volume) was 252.8 ± 26.4 mL/min (57.0 ± 6.0 L). Kt/V for urea was comparable between patients on HD and patients on pre-dilution on-line HDF (1.46 ± 0.25 vs. 1.46 ± 0.31). Amino acid loss and clear space were evaluated. Patients on pre-dilution on-line HDF lost significantly less glutamine and arginine (p < 0.01 and p = 0.032) and significantly less nonessential amino acids (NEAAs) than patients on HD (p = 0.013). They also had significantly lower clear space of total amino acids (TAAs), NEAAs, essential amino acids (EAAs), and branched-chain amino acids (BCAAs) than patients on HD (Total AA p = 0.019, NEAA p = 0.018, EAA p = 0.024, BCAA p = 0.042). When Kt/V for urea is equal, pre-dilution on-line HDF ensures better nutrition than does HD.


Similar content being viewed by others
References
Kikuchi K, Hamano T, Wada A, Nakai S, Masakane I. Predilution online hemodiafiltration is associated with improved survival compared with hemodialysis. Kidney Int. 2019;95:929–38.
Ikizler TA, Hakim RM. Nutrition in end-stage renal disease. Kidney Int. 1996;50:343–57.
Kopple JD, Greene T, Chumlea WC, Hollinger D, Maroni BJ, Merrill D, et al. Relationship between nutritional status and the glomerular filtration rate: results from the MDRD study. Kidney Int. 2000;57:1688–703.
Fouque D, Kalantar-Zadeh K, Kopple J, Cano N, Chauveau P, Cuppari L, et al. A proposed nomenclature and diagnostic criteria for protein-energy wasting in acute and chronic kidney disease. Kidney Int. 2008;73:391–8.
Acchiardo SR, Moore LW, Latour PA. Malnutrition as the main factor in morbidity and mortality of hemodialysis patients. Kidney Int Suppl. 1983;16:S199–203.
Stenvinkel P, Barany P, Chung SH, Lindholm B, Heimbürger O. A comparative analysis of nutritional parameters as predictors of outcome in male and female ESRD patients. Nephrol Dial Transplant. 2002;17:1266–74.
Carrero JJ, Stenvinkel P, Cuppari L, Ikizler TA, Kalantar-Zadeh K, Kaysen G, et al. Etiology of the protein-energy wasting syndrome in chronic kidney disease: a consensus statement from the International Society of Renal Nutrition and Metabolism (ISRNM). J Ren Nutr. 2013;23:77–90.
Löfberg E, Essén P, McNurlan M, Wernerman J, Garlick P, Anderstam B, et al. Effect of hemodialysis on protein synthesis. Clin Nephrol. 2000;54:284–94.
Mokrzycki MH, Kaplan AA. Protein losses in continuous renal replacement therapies. J Am Soc Nephrol. 1996;7:2259–63.
Davies SP, Reaveley DA, Brown EA, Kox WJ. Amino acid clearances and daily losses in patients with acute renal failure treated by continuous arteriovenous hemodialysis. Crit Care Med. 1991;19:1510–5.
Schepky AG, Bensch KW, Schulz-Knappe P, Forssmann WG. Human hemofiltrate as a source of circulating bioactive peptides: determination of amino acids, peptides and proteins. Biomed Chromatogr. 1994;8:90–4.
Ikizler TA, Pupim LB, Brouillette JR, et al. Hemodialysis stimulates muscle and whole body protein loss and alters substrate oxidation. Am J Physiol Endocrinol Metab. 2002;282:e107–e116116.
Raj DS, Zager P, Shah VO, Dominic EA, Adeniyi O, Blandon P, et al. Protein turnover and amino acid transport kinetics in end-stage renal disease. Am J Physiol Endocrinol Metab. 2004;286:E136–E143143.
Kotani G, Usami M, Kasahara H, Saitoh Y. The relationship of IL-6 to hormonal mediators, fuel utilization, and systemic hypermetabolism after surgical trauma. Kobe J Med Sci. 1996;42:187–205.
Wolfson M, Jones MR, Kopple JD. Amino acid losses during hemodialysis with infusion of amino acids and glucose. Kidney Int. 1982;21:500–6.
Ikizler TA, Flakoll PJ, Parker RA, Hakim RM. Amino acid and albumin losses during hemodialysis. Kidney Int. 1994;46:830–7.
Navarro JF, Marcén R, Teruel JL, Martin del Río R, Gámez C, Mora C, et al. Effect of different membranes on amino-acid losses during haemodialysis. Nephrol Dial Transplant. 1998;13:113–7.
Navarro JF, Mora C, León C, Martín-Del Río R, Macía ML, Gallego E, et al. Amino acid losses during hemodialysis with polyacrylonitrile membranes: effect of intradialytic amino acid supplementation on plasma amino acid concentrations and nutritional variables in nondiabetic patients. Am J Clin Nutr. 2000;71:765–73.
Yamashita AC. The clear space index. Contrib Nephrol. 2017;189:197–203.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Urabe, S., Hyodo, T., Hosono, T. et al. Amino acid losses are lower during pre-dilution on-line HDF than HD of the same Kt/V for urea. J Artif Organs 23, 342–347 (2020). https://doi.org/10.1007/s10047-020-01174-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10047-020-01174-z