Abstract
Purpose
Endoscopic totally extraperitoneal (TEP) hernia repair with polypropylene mesh has become a well-established technique. However, since the mesh is placed in close contact with the spermatic cord, mesh-induced inflammation may affect its structures, possibly resulting in impaired fertility. The aim of this observational prospective cohort study was to assess fertility after bilateral endoscopic TEP inguinal hernia repair in male patients.
Methods
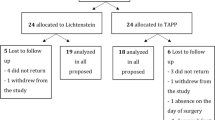
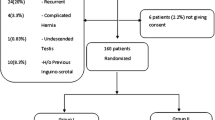
Fifty-seven male patients (22–60 years old) with primary, reducible, bilateral inguinal hernias underwent elective bilateral endoscopic TEP hernia repair with use of polypropylene mesh. The primary outcome was testicular perfusion; secondary outcomes were testicular volume, endocrinological status, and semen quality. All patients were assessed preoperatively and 6 months postoperatively.
Results
Follow-up was completed in 44 patients. No statistically significant differences in measurements of testicular blood flow parameters or testicular volume were found. Postoperative LH levels were significantly higher [preoperative median 4.3 IU/L (IQR 3.4–5.3) versus postoperative median 5.0 IU/L (IQR 3.6–6.5), p = 0.03]. Levels of inhibin B were significantly lower postoperatively [preoperative median 139.0 ng/L (IQR 106.5–183.0) versus postoperative median 27.0 ng/L (IQR 88.3–170.9), p = 0.01]. No significant changes in FSH or testosterone levels were observed. There were no differences in semen quality.
Conclusions
Our data suggest that bilateral endoscopic TEP hernia repair with polypropylene mesh does not impair fertility, as no differences in testicular blood flow, testicular volume, or semen quality were observed. Postoperative levels of LH and inhibin B differed significantly from preoperative measurements, yet no clinical relevance could be ascribed to these findings.
Similar content being viewed by others
References
Simons MP, Aufenacker T, Bay-Nielsen M et al (2009) European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13(4):343–403
Bay-Nielsen M, Kehlet H, Strand L et al (2001) Quality assessment of 26 304 herniorrhaphies in Denmark: a prospective nationwide study. Lancet 358(9288):1124–1128
Kehlet H (2008) Chronic pain after groin hernia repair. Br J Surg 95(2):135–136
Kuhry E, Van Veen RN, Langeveld HR et al (2007) Open or endoscopic total extraperitoneal inguinal hernia repair? A systematic review. Surg Endosc 21(2):161–166
O’Reilly EA, Burke JP, O’Connell PR (2012) A meta-analysis of surgical morbidity and recurrence after laparoscopic and open repair of primary unilateral hernia. Ann Surg 255(5):846–853
Fitzgibbons RJ (2005) Can we be sure polypropylene mesh causes infertility? Ann Surg 241(4):559–561
Maciel LC, Glina S, Palma PCR et al (2007) Histopathological alterations of the vas deferens in rats exposed to polypropylene mesh. BJU Int 100(1):187–190
Peiper C, Junge K, Klinge U et al (2006) Is there a risk of infertility after inguinal mesh repair? Experimental studies in the pig and the rabbit. Hernia 10(1):7–12
Shin D, Lipshultz LI, Goldstein M et al (2005) Herniorrhaphy with polypropylene mesh causing inguinal vasal obstruction. Ann Surg 241(4):553–558
Yamaguchi K, Ishikawa T, Nakano Y et al (2008) Rapidly progressing, late-onset obstructive azoospermia linked to herniorrhaphy with mesh. Fertil Steril 90(5):2018–2020
Kordzadeh A, Liu MO, Jayanthi NV (2016) Male infertility following inguinal hernia repair: a systematic review and pooled analysis. Hernia. doi:10.1007/s10029-016-1560-0
Goruroglu Ozturk O (2012) Using biological variation data for reference change values in clinical laboratories. Biochem Anal Biochem 1(4):1–2
Bellón JM, Contreras LA, Buján J et al (1998) Tissue response to polypropylene meshes used in the repair of abdominal wall defects. Biomaterials 19(7–9):669–675
Ridgway PF, Shah J, Darzi A (2002) Male genital tract injuries after contemporary inguinal hernia repair. BJU Int 90(3):272–276
Dilek ON (2014) Hernioplasty and testicular perfusion. SpringerPlus 21(3):107
Middleton W, Thorne D, Melson G (1989) Color Doppler ultrasound of the testis. AJR Am J Roentgenol 152(2):293–297
Stula I, Druzijanic N, Srsen D et al (2015) Influence of inguinal hernia mesh repair on testicular flow and sperm autoimmunity. Hernia 16(4):417–424
Lal P, Bansal B, Sharma R et al (2016) Laparoscopic TEP repair of inguinal hernia does not alter testicular perfusion. Hernia 20(3):429–434
Ersin S, Aydin U, Makay O (2006) Is testicular perfusion influenced during laparoscopic inguinal hernia surgery? Surg Endosc 20:685–689
Gurbulak EK, Gurbulak B, Akgun IE et al (2015) Effects of totally extraperitoneal (TEP) and Lichtenstein hernia repair on testicular blood flow and volume. Surgery 158(5):1297–1303
Peeters E, Spiessens C, Oyen R et al (2010) Laparoscopic inguinal hernia repair in men with lightweight meshes may significantly impair sperm motility: a randomized controlled trial. Ann Surg 252(2):240
Skawran S, Weyhe D, Schmitz B et al (2011) Bilateral endoscopic total extraperitoneal (TEP) inguinal hernia repair does not induce obstructive azoospermia: data of a retrospective and prospective trial. World J Surg 35(7):1643–1648
Peeters E, Spiessens C, Oyen R et al (2014) Sperm motility after laparoscopic inguinal hernia repair with lightweight meshes: 3-year follow-up of a randomised clinical trial. Hernia 18:361–367
Akbulut G, Serteser M, Yucel A et al (2003) Can laparoscopic hernia repair alter function and volume of testis? Randomized clinical trial. Surg Laparosc Ednosc Percutan Tech 13(6):377–381
Wantz GE (1982) Testicular atrophy as a risk inguinal hernioplasty. Surg Gynecol Obstet 154(4):570–571
Sucullu I, Filiz AI, Sen B et al (2010) The effects of inguinal hernia repair on testicular function in young adults: a prospective randomized study. Hernia 14(2):165–169
Schouten N, Van Dalen T, Smakman N et al (2012) Male infertility after endoscopic totally extraperitoneal (TEP) hernia repair (Main): rationale and design of a prospective observational cohort study. BMS Surg 21(12):7
Kehlet H, Roumen RM, Reinpold W et al (2013) Invited commentary: persistent pain after inguinal hernia repair: what do we know and what do we need to know? Hernia 17:293–297
Author information
Authors and Affiliations
Contributions
MR: data collection, analysis and interpretation of data, drafting of manuscript. GJC: study conception and design, critical revision, EJV: study conception and design, critical revision. PD: study conception and design, critical revision. CW: study conception and design (clinical chemistry), interpretation of data (clinical chemistry), critical revision. RS: study conception and design (urology), interpretation of data (urology), critical revision. LSM: study conception and design (radiology), interpretation of data (radiology), critical revision. IB: study conception and design, drafting of manuscript, critical revision.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interests.
Ethical approval
Ethical approval was obtained by the Regional Medical Ethics Committee and the hospitals EthicsBoard.
Human and animal rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
All subjects signed informed consent.
Rights and permissions
About this article
Cite this article
Roos, M.M., Clevers, G.J., Verleisdonk, E.J. et al. Bilateral endoscopic totally extraperitoneal (TEP) inguinal hernia repair does not impair male fertility. Hernia 21, 887–894 (2017). https://doi.org/10.1007/s10029-017-1657-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-017-1657-0