Abstract
Purpose
The two most common procedures for open tension-free groin hernia repair with prosthetic mesh are the Lichtenstein operation and the mesh plug (Rutkow–Robbins) technique. Our study evaluated these two techniques on testicular blood flow and volume, and sperm function in young adults.
Methods
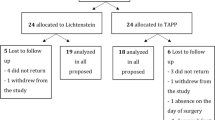
We randomized operation types with a systematic sampling method, and handled consecutive patients of age 20–30 years having unilateral inguinal hernia repair at our institution from March to August 2008. The study subjects were divided into the Lichtenstein group (LG) and the mesh plug group (MPG). All subjects received color Doppler ultrasonography to determine testicular volume and resistive index (RI) the day before surgery and 3 months postoperatively by a physician blinded for the type of planned or performed operation. Spermiograms done preoperatively and at 3 months postoperatively measured sperm concentration and the rate of progressive motility.
Results
Sixty-four patients met the study criteria, with 32 patients each in the LG and MPG. RI levels were elevated postoperatively in both the LG (P = 0.027) and MPG (P = 0.012); there was no significant alteration in terms of testicular volume and spermiogram in the LG and MPG.
Conclusion
The Lichtenstein and mesh plug techniques in unilateral inguinal hernia increase the RI level significantly in the early postoperative period, but do not have a significant effect on sperm concentration and the rate of progressive motility.
Similar content being viewed by others
References
Rutkow IM (1998) Epidemiologic, economic, and sociologic aspects of hernia surgery in the United States in the 1990s. Surg Clin North Am 78:941–951
Frey DM, Wildisen A, Hamel CT, Zuber M, Oertli D, Metzger J (2007) Randomized clinical trial of Lichtenstein’s operation versus mesh plug for inguinal hernia repair. Br J Surg 94:36–41
Rutkow IM, Robbins AW (1995) Mesh plug hernia repair: a follow-up report. Surgery 117:597–598
Neumayer L, Giobbie-Hurder A, Jonasson O, Fitzgibbons R Jr, Dunlop D, Gibbs J et al (2004) Open mesh versus laparoscopic mesh repair of inguinal hernia. N Engl J Med 350:1819–1827
Wantz GE (1993) Testicular atrophy and chronic residual neuralgia as risks of inguinal hernioplasty. Surg Clin North Am 73:571–581
Phillips EH, Arregui M, Carroll BJ, Corbitt J, Crafton WB, Fallas MJ et al (1995) Incidence of complications following laparoscopic hernioplasty. Surg Endosc 9:16–21
Aydede H, Erhan Y, Sakarya A, Kara E, Ilkgül O, Can M (2003) Effect of mesh and its localisation on testicular flow and spermatogenesis in patients with groin hernia. Acta Chir Belg 103:607–610
Sheynkin YR, Hendin BN, Schlegel PN, Goldstein M (1998) Microsurgical repair of iatrogenic injury to the vas deferens. J Urol 159:139–141
Amid PK, Shulman AG, Lichtenstein IL (1996) Open “tension-free” repair of inguinal hernias: the Lichtenstein technique. Eur J Surg 162:447–453
Robbins AW, Rutkow IM (1998) Mesh plug repair and groin hernia surgery. Surg Clin North Am 78:1007–1023
Klinge U, Klosterhalfen B, Müller M, Schumpelick V (1999) Foreign body reaction to meshes used for the repair of abdominal wall hernias. Eur J Surg 165:665–673
Amid PK (1997) Classification of biomaterials and their related complications in abdominal wall hernia surgery. Hernia 1:15–21
Skandalakis JE, Skandalakis LJ, Colborn GL (1996) Testicular atrophy and neuropathy in herniorrhaphy. Am Surg 62:775–782
Uzzo RG, Lemack GE, Morrissey KP, Goldstein M (1999) The effects of mesh bioprosthesis on the spermatic cord structures: a preliminary report in a canine model. J Urol 161:1344–1399
Pinggera GM, Mitterberger M, Bartsch G, Strasser H, Gradl J, Aigner F et al (2008) Assessment of the intratesticular resistive index by colour Doppler ultrasonography measurements as a predictor of spermatogenesis. BJU Int 101:722–726
Valenti G, Baldassarre E, Torino G (2006) Vas deferens obstruction due to fibrosis after plug hernioplasty. Am Surg 72:137–138
Pavlica P, Barozzi L (2001) Imaging of the acute scrotum. Eur Radiol 11:220–228
Iles JD (1965) Specialisation in elective herniorrhaphy. Lancet 1:751–755
Yavetz H, Harash B, Yogev L, Homonnai ZT, Paz G (1991) Fertility of men following inguinal hernia repair. Andrologia 23:443–446
Beddy P, Ridgway PF, Geoghegan T, Peirce C, Govender P, Keane FB et al (2006) Inguinal hernia repair protects testicular function: a prospective study of open and laparoscopic herniorraphy. J Am Coll Surg 203:17–23
Lima Neto EV, Goldenberg A, Jucá MJ (2007) Prospective study on the effects of a polypropylene prosthesis on testicular volume and arterial flow in patients undergoing surgical correction for inguinal hernia. Acta Cir Bras 22:266–271
Silich RC, McSherry CK (1996) Spermatic granuloma. An uncommon complication of the tension-free hernia repair. Surg Endosc 10:537–539
Fitzgibbons RJ Jr, Salerno GM, Filipi CJ, Hunter WJ, Watson P (1994) A laparoscopic intraperitoneal onlay mesh technique for the repair of an indirect inguinal hernia. Ann Surg 219:144–156
Taylor SG, Hair A, Baxter GM, O’Dwyer PJ (2001) Does contraction of mesh following tension free hernioplasty effect testicular or femoral vessel blood flow? Hernia 5:13–15
Ramadan SU, Gokharman D, Tuncbilek I, Ozer H, Kosar P, Kacar M et al (2009) Does the presence of a mesh have an effect on the testicular blood flow after surgical repair of indirect inguinal hernia? J Clin Ultrasound 37:78–81
Akbulut G, Serteser M, Yücel A, Değirmenci B, Yilmaz S, Polat C et al (2003) Can laparoscopic hernia repair alter function and volume of testis? Randomized clinical trial. Surg Laparosc Endosc Percutan Tech 13:377–381
Homonnai ZT, Fainman N, Paz GF, David MP (1980) Testicular function after herniotomy. Herniotomy and fertility. Andrologia 12:115–120
Acknowledgment
The authors thank Marilyn Carlson for her editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sucullu, I., Filiz, A.I., Sen, B. et al. The effects of inguinal hernia repair on testicular function in young adults: a prospective randomized study. Hernia 14, 165–169 (2010). https://doi.org/10.1007/s10029-009-0589-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-009-0589-8