Purpose
Abstract
A meta-analysis was performed to asses whether antibiotic prophylaxis is effective in reducing the incidence of surgical site infection (SSI) after open mesh repair of groin hernia.
Methods
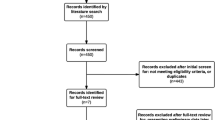
A literature search for randomized controlled trials (RCT) evaluating the effectiveness of antibiotic prophylaxis in adult patients undergoing open mesh repair of groin hernia was performed in November 2015. Incidence of overall and deep SSI was considered as primary and secondary outcome measures, respectively. Only studies with a clear definition of SSI and a follow-up of at least 1 month were included. Effect size from each RCT was computed as odds ratio (OR) and 95 % confidence interval (CI) and then data were pooled using a random-effects model.
Results
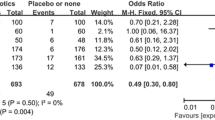
Sixteen RCTs with a total number of 5519 patients were included in the meta-analysis. Considering all the RCTs, antibiotic prophylaxis significantly reduced the overall incidence of SSI from 4.8 % to 3.2 % [OR 0.68, 95 % CI (0.51–0.91)]. However, after removal of two outlier studies, which were identified by evaluating the standardized residual, the result of the meta-analysis became non-significant [OR 0.76, 95 % CI (0.56–1.02)]. The incidence of deep SSI was very low (0–0.7 %) and the effect of antibiotic prophylaxis was not significant [OR 0.80, 95 % CI (0.32–1.99)].
Conclusions
The results of this meta-analysis do not support the routine use of antibiotic prophylaxis for the open mesh repair of groin hernia. In clinical settings with unexpectedly high rates of SSIs, the appropriateness of surgical asepsis should be carefully checked.




Similar content being viewed by others
References
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR (1999) Guideline for prevention of surgical site infection, 1999. Centers for Disease Control and Prevention (CDC) Hospital Infection Control Practices Advisory Committee. Am J Infect Control 27:97–132
Gaynes RP, Culver DH, Horan TC, Edwards JR, Richards C, Tolson JS (2001) Surgical site infection (SSI) rates in the United States, 1992–1998: the National Nosocomial Infections Surveillance System basic SSI risk index. Clin Infect Dis 33(Suppl 2):S69–S77
Edwards JR, Peterson KD, Mu Y, Banerjee S, Allen-Bridson K, Morrell G, Dudeck MA, Pollock DA, Horan TC (2009) National healthcare safety network (NHSN) report: data summary for 2006 through 2008, issued December 2009. Am J Infect Control 37:783–805
Mazaki T, Mado K, Masuda H, Shiono M, Tochikura N, Kaburagi M (2014) A randomized trial of antibiotic prophylaxis for the prevention of surgical site infection after open mesh-plug hernia repair. Am J Surg 207:476–484
Othman I (2011) Prospective randomized evaluation of prophylactic antibiotic usage in patients undergoing tension free inguinal hernioplasty. Hernia 15:309–313
Shankar VG, Srinivasan K, Sistla SC, Jagdish S (2010) Prophylactic antibiotics in open mesh repair of inguinal hernia: a randomized controlled trial. Int J Surg 8:444–447
Al-Fatah MA (2011) The role of antibiotic prophylaxis in prevention of wound infection after Lichtenstein repair of primary inguinal hernia. http://www.aamj.eg.net/journals/pdf/1355.pdf
Aufenacker TJ, van Geldere D, van Mesdag T, Bossers AN, Dekker B, Scheijde E, van Nieuwenhuizen R, Hiemstra E, Maduro JH, Juttmann JW, Hofstede D, van Der Linden CT, Gouma DJ, Simons MP (2004) The role of antibiotic prophylaxis in prevention of wound infection after Lichtenstein open mesh repair of primary inguinal hernia: a multicenter double-blind randomized controlled trial. Ann Surg 240:955–960
Celdrán A, Frieyro O, de la Pinta JC, Souto JL, Esteban J, Rubio JM, Señarís JF (2004) The role of antibiotic prophylaxis on wound infection after mesh hernia repair under local anesthesia on an ambulatory basis. Hernia 8:20–22
Ergul Z, Akinci M, Ugurlu C, Kulacoglu H, Yilmaz KB (2012) Prophylactic antibiotic use in elective inguinal hernioplasty in a trauma center. Hernia 16:145–151
Jain SK, Jayant M, Norbu C (2008) The role of antibiotic prophylaxis in mesh repair of primary inguinal hernias using prolene hernia system: a randomized prospective double-blind control trial. Trop Doct 38:80–82
Kochhar G, Andley M, Saha S, Kumar A, Pusuluri R, Saurabh G, A Kumar (2014) Randomized controlled trial to evaluate the role of antibiotic prophylaxis in lichtenstein hernia repair. https://www.researchgate.net/publication/268484354
Morales R, Carmona A, Pagán A, García Menéndez C, Bravo R, Hernández MJ, Llobera J (2000) Utilidad de la profilaxis antibiótica en la reducción de la infección de herida en la reparación de la hernia inguinal o crural mediante malla de polipropileno. Cir Esp 67:51–59
Oteiza F, Ciga MA, Ortiz H (2004) Profilaxis antibiótica en la hernioplastia inguinal. Cir Esp 75:69–71
Perez AR, Roxas MF, Hilvano SS (2005) A randomized, double-blind, placebo-controlled trial to determine effectiveness of antibiotic prophylaxis for tension-free mesh herniorraphy. J Am Coll Surg 200:393–397
Razack A, Kapoor KK, Tambat RM (2015) The role of single dose antibiotic prophylaxis in open mesh repair of inguinal hernia: a prospective, double blind randomized trial. J Evol Med Dent Sci 4:6017–6026
Tzovaras G, Delikoukos S, Christodoulides G, Spyridakis M, Mantzos F, Tepetes K, Athanassiou E, Hatzitheofilou C (2007) The role of antibiotic prophylaxis in elective tension-free mesh inguinal hernia repair: results of a single-centre prospective randomised trial. Int J Clin Pract 61:236–239
Wang J, Ji G, Yang Z, Xi M, Wu Y, Zhao P, Wang L, Yu W, Wen A (2013) Prospective randomized, double-blind, placebo controlled trial to evaluate infection prevention in adult patients after tension-free inguinal hernia repair. Int J Clin Pharmacol Ther 51:924–931
Yerdel MA, Akin EB, Dolalan S, Turkcapar AG, Pehlivan M, Gecim IE, Kuterdem E (2001) Effect of single-dose prophylactic ampicillin and sulbactam on wound infection after tension-free inguinal hernia repair with polypropylene mesh: the randomized, double-blind, prospective trial. Ann Surg 233:26–33
Sanabria A, Domínguez LC, Valdivieso E, Gómez G (2007) Prophylactic antibiotics for mesh inguinal hernioplasty: a meta-analysis. Ann Surg 245:392–396
Sanchez-Manuel FJ, Lozano-García J, Seco-Gil JL (2012) Antibiotic prophylaxis for hernia repair. Cochrane Database Syst Rev 2:CD003769
National Collaborating Centre for Women’s and Children’s Health (2008) Surgical site infection: prevention and treatment of surgical site infection. NICE, London. https://www.nice.org.uk/guidance/cg74/evidence/full-guideline-242005933
Bratzler DW, Dellinger EP, Olsen KM, Perl TM, Auwaerter PG, Bolon MK, Fish DN, Napolitano LM, Sawyer RG, Slain D, Steinberg JP, Weinstein RA; American Society of Health-System Pharmacists; Infectious Disease Society of America; Surgical Infection Society; Society for Healthcare Epidemiology of America (2013) Clinical practice guidelines for antimicrobial prophylaxis in surgery. Am J Health Syst Pharm 70:195–283
Scottish Intercollegiate Guidelines Network (SIGN) (2008) Antibiotic prophylaxis in surgery. SIGN, Edinburg (SIGN publication no. 104). http://www.sign.ac.uk/pdf/sign104.pdf
Sistema Nazionale per le Linee Guida (SNLG) (2008) Antibioticoprofilassi perioperatoria nell’adulto. SNLG, Milano (SNLG 17). http://www.snlg-iss.it/cms/files/LG_AntibioticoP_Unico_2008.pdf
Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, Conze J, de Lange D, Fortelny R, Heikkinen T, Kingsnorth A, Kukleta J, Morales-Conde S, Nordin P, Schumpelick V, Smedberg S, Smietanski M, Weber G, Miserez M (2009) European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13:343–403
Kingsnorth A, LeBlanc K (2003) Hernias: inguinal and incisional. Lancet 362:1561–1571
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700
Higgins JPT, Green S (eds) (2011) Cochrane handbook for systematic reviews of interventions Version 5.1.0 [updated March 2011]. In: The Cochrane Collaboration. http://www.cochrane-handbook.org
Borenstein M, Hedges LV, Higgins JPT, Rothstein HR (2009) Introduction to meta-analysis. Wiley, Chichester
Altman DG (1998) Confidence intervals for the number needed to treat. BMJ 317:1309–1312
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
Duval S, Tweedie R (2000) Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56:455–463
Scott NW, McCormack K, Graham P, Go PM, Ross SJ, Grant AM (2002) Open mesh versus non-mesh for repair of femoral and inguinal hernia. Cochrane Database Syst Rev 4:CD002197
Fawole AS, Chaparala RP, Ambrose NS (2006) Fate of the inguinal hernia following removal of infected prosthetic mesh. Hernia 10:58–61
Rehman S, Khan S, Pervaiz A, Perry EP (2012) Recurrence of inguinal herniae following removal of infected prosthetic meshes: a review of the literature. Hernia 16:123–126
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
EE, FM, GP, AN, and PGC declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Erdas, E., Medas, F., Pisano, G. et al. Antibiotic prophylaxis for open mesh repair of groin hernia: systematic review and meta-analysis. Hernia 20, 765–776 (2016). https://doi.org/10.1007/s10029-016-1536-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-016-1536-0