Abstract
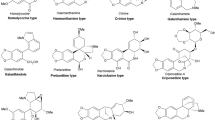
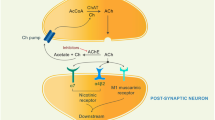
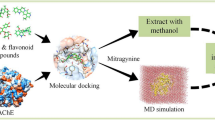
Acetylcholinesterase (AChE) inhibitors are currently in focus for the pharmacotherapy of Alzheimer’s disease (AD). These inhibitors increase the level of acetylcholine in the brain and facilitate cholinergic neurotransmission. AChE inhibitors such as rivastigmine, galantamine, physostigmine and huperzine are obtained from plants, indicating that plants can serve as a potential source for novel AChE inhibitors. We have performed a virtual screening of diverse natural products with distinct chemical structure against AChE. NDGA was one among the top scored compounds and was selected for enzyme kinetic studies. The IC50 of NDGA on AChE was 46.2 μM. However, NDGA showed very poor central nervous system (CNS) activity and blood–brain barrier (BBB) penetration. In silico structural modification on NDGA was carried out in order to obtain derivatives with better CNS activity as well as BBB penetration. The studies revealed that some of the designed compounds can be used as lead molecules for the development of drugs against AD

Inhibitory activity of NDGA against AChE




Similar content being viewed by others
References
Selkoe DJ, Schenk D (2003) Alzheimer’s disease: molecular understanding predicts amyloid-based therapeutics. Annu Rev Pharmacol Toxicol 43:545–584
Schliebs R (2005) Basal forebrain cholinergic dysfunction in Alzheimer’s disease–interrelationship with beta-amyloid, inflammation and neurotrophin signaling. Neurochem Res 30:895–908
Goedert M, Spillantini MG (2006) A century of Alzheimer’s disease. Science 314:777–781
Luttmann E, Linnemann E, Fels G (2002) Galantamine as bis-functional ligand for the acetylcholinesterase. J Mol Model 8:208–216
Schrattenholz A, Pereira EF, Roth U, Weber KH, Albuquerque EX, Maelicke A (1996) Agonist responses of neuronal nicotinic acetylcholine receptors are potentiated by a novel class of allosterically acting ligands. Mol Pharmacol 49:1–6
Coyle JT, Geerts H, Sorra K, Amatniek J (2007) Beyond in vitro data: a review of in vivo evidence regarding the allosteric potentiating effect of galantamine on nicotinic acetylcholine receptors in Alzheimer’s neuropathology. J Alzheimers Dis 11:491–507
Reyes AE, Chacon MA, Dinamarca MC, Cerpa W, Morgan C, Inestrosa NC (2004) Acetylcholinesterase—Abeta complexes are more toxic than Abeta fibrils in rat hippocampus: effect on rat beta-amyloid aggregation, laminin expression, reactive astrocytosis, and neuronal cell loss. Am J Pathol 164:2163–2174
Castro A, Martinez A (2006) Targeting beta-amyloid pathogenesis through acetylcholinesterase inhibitors. Curr Pharm Des 12:4377–4387
Kasa P, Papp H, Kasa P Jr, Torok I (2000) Donepezil dose-dependently inhibits acetylcholinesterase activity in various areas and in the presynaptic cholinergic and the postsynaptic cholinoceptive enzyme-positive structures in the human and rat brain. Neuroscience 101:89–100
Kurz A (1998) The therapeutic potential of tacrine. J Neural Transm Suppl 54:295–299
Sugimoto H (2001) Donepezil hydrochloride: a treatment drug for Alzheimer’s disease. Chem Rec 1(1):63–73
Zarotsky V, Sramek JJ, Cutler NR (2003) Galantamine hydrobromide: an agent for alzheimer’s disease. Am J Health Syst Pharm 60:446–452
Jann MW (2000) Rivastigmine, a new- generation cholinesterase inhibitor for the treatment of Alzheimer’s disease. Pharmacotherapy 20(1):1–12
Francis PT, Nordberg A, Arnold SE (2005) A preclinical view of cholinesterase inhibitors in neuroprotection: do they provide more than symptomatic benefits in Alzheimer’s disease? Trends Pharmacol Sci 26:104–111
Wang YE, Yue DX, Tang XC (1986) Anticholinesterase activity of huperzine A. Acta pharmacol Sin 7:110–113
Barak D, Ordentlich A, Stein D, Yu QS, Greig NH, Shafferman A (2009) Accommodation of physostigmine and its analogs by acetylcholinesterase is dominated by hydrophobic interactions. Biochem J 417(1):213–222
Arteaga S, Andrade-Cetto A, Cardenas R (2005) Larrea tridentate (creosote bush) an abundant palnt of Mexican and US-american desert and its metabolite nordihydroguairetic acid. J Ethnopharmol 98(3):231–239
Oliveto EP (1972) Nordihydroguaiaretic acid. A naturally occurring antioxidant. Chem Ind 17:677–679
Noor R, Mittal S, Iqbal J (2002) Superoxide dismutase-applications and relevance to human diseases. Med Sci Monit 8:RA210–RA215
Guzman-Beltran S, Espada S, Orozco-Ibarra M, Pedraza-Chaverri J, Cuadrado A (2008) Nordihydroguaiaretic acid activates the antioxidant pathway Nrf2/HO-1 and protects cerebellargranule neurons against oxidative stress. Neurosci Lett 447:167–171
Goodman Y, Steiner MR, Steiner SM, Mattson MP (1994) Nordihydroguaiaretic acid protects hippocampal neurons against amyloid beta-peptide toxicity, and attenuates free radical and calcium accumulation. Brain Res 654:171–176
Rothman SM, Yamada KA, Lancaster N (1993) Nordihydroguaiaretic acid attenuates NMDA neurotoxicity—action beyond the receptor. Neuropharmacology 32:1279–1288
Boston-Howes W, Williams EO, Bogush A, Scolere M, Pasinelli P, Trotti D (2008) Nordihydroguaiaretic acid increases glutamate uptake in vitro and in vivo: therapeutic implications for amyotrophic lateral sclerosis. Exp Neurol 213:229–237
Shishido Y, Furushiro M, Hashimoto S, Yokokura T (2001) Effect of nordihydroguaiaretic acid on behavioral impairment and neuronal cell death after forebrain ischemia. Pharmacol Biochem Behav 69:469–474
Majumdar DK, Govil JN, Singh VK (2003) Recent progress in medicinal plants. Vol 8 Phytochemistry and Pharmacology. Studium, Houston, TX
Ellman GL, Courtney KD, Andres V Jr, Featherstone RM (1961) Biochem Pharmacol 7:88–95
Sussman JL, Harel M, Frolow F, Oefner C, Goldman A, Toker L, Silman I (1991) Science 253:872–879
Bon S, Vigny M, Massoulie J (1979) Asymmetric and globular forms of acetylcholinesterase in mammals and birds. Proc Natl Acad Sci USA 76:2546–2550
Lipinski CA, Lombardo F, Dominy BW, Feeney PJ (2001) Experimental and computational approaches to estimate solubility and permeability in drug discovery and development settings. Adv Drug Deliv Rev 46:3–26
Ekins S, Waller CL, Swann PW, Cruciani G, Wrighton SA, Wikel JH (2000) J Pharmacol Toxicol 44:251–272
Alavijeh MS, Chishty M, Qaiser MZ, Palmer AM (2005) Drug metabolism and pharmacokinetics, the blood-brain barrier, and central nervous system drug discovery. NeuroRx 2:554–571
Clark DE (2003) In silico prediction of blood–brain barrier permeation. Drug Discov Today 8:927–933
Lloyd EJ, Andrews PR (1986) A common structural model for central nervous system drugs and their receptors. J Med Chem 29:453–462
Lemke TL, Williams DA, Roche VF, Zito SW (2008), Foye’s principles of medicinal chemistry. Wolters Kluwer/Lippincott Williams and Wilkins, Baltimore
Pajouhesh H, Lenz GR (2005) Medicinal chemical properties of successful central nervous system drugs. NeuroRx 2:541–553
Clark DE (1999) Rapid calculation of polar molecular surface area and its application to the prediction of transport phenomena. 2. Prediction of blood–brain barrier penetration. J Pharm Sci 88:815–821
Ajay, Bemis GW, Murcko MA (1999) Designing libraries with CNS activity. J Med Chem 42:4942–4951
Balon K, Riebesehl BU, Muller BW (1999) Determination of liposome partitioning of ionizable drugs by titration. J Pharm Sci 88:802–806
Bhal SK, Kassam K, Peirson IG, Pearl GM (2007) The rule of five revisited: applying log d in place of log p in drug-likeness filters. Mol Pharmaceut 4:556–560
Garberg P, Ball M, Borg N, Cecchelli R, Fenart L, Hurst RD, Lindmark T, Mabondzo A, Nilsson JE, Raub TJ, Stanimirovic D, Terasaki T, Oberg JO (2005) In vitro models for the blood–brain barrier. Toxicol In Vitro 19:299–334
Deli MA, Abraham CS, Kataoka Y, Niwa M (2005) Permeability studies on in vitro blood–brain barrier models: physiology, pathology, and pharmacology. Cell Mol Neurobiol 25:59–127
Reichel A, Begley DJ, Abbott NJ (2003) An overview of in vitro techniques for blood–brain barrier studies. Methods Mol Med 89:307–324
Doan KM, Humphreys JE, Webster LO, Wring SA, Shampine LJ, Serabjit-Singh CJ (2002) Passive permeability and P-glycoproteinmediated efflux differentiate central nervous system (CNS) and non-CNS marketed drugs. J Pharmacol Exp Ther 303:1029–1037
Acknowledgments
The authors gratefully acknowledge the use of computational facilities provided by Bioinformatics Infrastructure Facility (supported by DBT, Government of India) at Kannur University and BIOGENE cluster, Bioinformatics Resources and Application Facility at C-DAC (Center for Development of Advanced Computing) Pune, India.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Remya, C., Dileep, K.V., Tintu, I. et al. In vitro inhibitory profile of NDGA against AChE and its in silico structural modifications based on ADME profile. J Mol Model 19, 1179–1194 (2013). https://doi.org/10.1007/s00894-012-1656-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00894-012-1656-0