Abstract
Objectives
The purpose of this systematic review was to evaluate evidence about the prevalence of degenerative joint disease (DJD) of the temporomandibular joints (TMJ).
Materials and methods
We performed search on electronic databases and gray literature from their inception to January 2018. Studies reporting prevalence data of DJD on TMJ were included. DJD was assessed through clinical and imaging diagnosis. Studies risk of bias was evaluated using the Critical Appraisal Checklist for Studies Reporting Prevalence Data.
Results
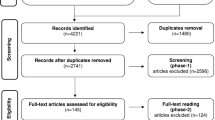
From 1082 studies, 32 were identified, and the sample size included 3435 subjects. They were clustered into two groups: the first comprised studies that reported prevalence of DJD in TMJ secondary to rheumatic systemic diseases like juvenile idiopathic arthritis (JIA) and rheumatoid arthritis (RA) and the second group comprised studies that reported prevalence of DJD on temporomandibular disorder patients. The prevalence of DJD on JIA patients ranged from 40.42% (n = 47) to 93.33% (n = 15) and on RA patients from 45.00% (n = 20) to 92.85% (n = 56). Among TMD patients, the prevalence of DJD reported according to patients ranged from 18.01% (n = 1038) to 84.74% (n = 118) and reported according to joints ranged from 17.97% (n = 178) to 77.23% (n = 224).
Conclusion
This review attempts to high prevalence of DJD in patients with systemic rheumatic disease and a less prevalent, but still high, occurrence in patients with TMD without systemic involvement.
Clinical relevance
Specialist doctors and dentists should be alert to not underestimate and to correctly diagnose DJD of the TMJ early in patients with rheumatic disease and TMD.

Similar content being viewed by others
References
Poole AR (2012) Osteoarthritis as a whole joint disease. HSS J 8(1):4–6. https://doi.org/10.1007/s11420-011-9248-6
Tanaka E, Detamore MS, Mercuri LG (2008) Degenerative disorders of the temporomandibular joint: etiology, diagnosis, and treatment. J Dent Res 87(4):296–307. https://doi.org/10.1177/154405910808700406
Leeuw RdK, Gary D. (2013) Orofacial pain: guidelines for assessment, Diagnosis and management, 5th edn
Kalladka M, Quek S, Heir G, Eliav E, Mupparapu M, Viswanath A (2014) Temporomandibular joint osteoarthritis: diagnosis and long-term conservative management: a topic review. J Indian Prosthodont Soc 14(1):6–15. https://doi.org/10.1007/s13191-013-0321-3
Helenius LM, Hallikainen D, Helenius I, Meurman JH, Kononen M, Leirisalo-Repo M, Lindqvist C (2005) Clinical and radiographic findings of the temporomandibular joint in patients with various rheumatic diseases. A case-control study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 99(4):455–463. https://doi.org/10.1016/j.tripleo.2004.06.079
Manfredini D, Guarda-Nardini L, Winocur E, Piccotti F, Ahlberg J, Lobbezoo F (2011) Research diagnostic criteria for temporomandibular disorders: a systematic review of axis I epidemiologic findings. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 112(4):453–462. https://doi.org/10.1016/j.tripleo.2011.04.021
Bracco P, Debernardi C, Piancino MG, Cirigliano MF, Salvetti G, Bazzichi L, De Feo F, Bosco M (2010) Evaluation of the stomatognathic system in patients with rheumatoid arthritis according to the research diagnostic criteria for temporomandibular disorders. Cranio 28(3):181–186. https://doi.org/10.1179/crn.2010.025
Bayar N, Kara SA, Keles I, Koç MC, Altinok D, Orkun S (2002) Temporomandibular joint involvement in rheumatoid arthritis: a radiological and clinical study. Cranio 20(2):105–110
Brooks SL, Westesson PL, Eriksson L, Hansson LG, Barsotti JB (1992) Prevalence of osseous changes in the temporomandibular joint of asymptomatic persons without internal derangement. Oral Surg Oral Med Oral Pathol 73(1):118–122
Lin YC, Hsu ML, Yang JS, Liang TH, Chou SL, Lin HY (2007) Temporomandibular joint disorders in patients with rheumatoid arthritis. J Chin Med Assoc 70(12):527–534
Arvidsson LZ, Smith HJ, Flato B, Larheim TA (2010) Temporomandibular joint findings in adults with long-standing juvenile idiopathic arthritis: CT and MR imaging assessment. Radiology 256(1):191–200
Schiffman E, Ohrbach R, Truelove E, Look J, Anderson G, Goulet JP, List T, Svensson P, Gonzalez Y, Lobbezoo F, Michelotti A, Brooks SL, Ceusters W, Drangsholt M, Ettlin D, Gaul C, Goldberg LJ, Haythornthwaite JA, Hollender L, Jensen R, John MT, De Laat A, de Leeuw R, Maixner W, van der Meulen M, Murray GM, Nixdorf DR, Palla S, Petersson A, Pionchon P, Smith B, Visscher CM, Zakrzewska J, Dworkin SF, International Rdc/Tmd Consortium Network IafDR, Orofacial Pain Special Interest Group IAftSoP (2014) Diagnostic criteria for temporomandibular disorders (DC/TMD) for clinical and research applications: recommendations of the international RDC/TMD consortium network* and orofacial pain special interest Groupdagger. J Oral Facial Pain Headache 28(1):6–27. https://doi.org/10.11607/jop.1151
Ahmad M, Hollender L, Anderson Q, Kartha K, Ohrbach R, Truelove EL, John MT, Schiffman EL (2009) Research diagnostic criteria for temporomandibular disorders (RDC/TMD): development of image analysis criteria and examiner reliability for image analysis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 107(6):844–860. https://doi.org/10.1016/j.tripleo.2009.02.023
Peck CC, Goulet JP, Lobbezoo F, Schiffman EL, Alstergren P, Anderson GC, de Leeuw R, Jensen R, Michelotti A, Ohrbach R, Petersson A, List T (2014) Expanding the taxonomy of the diagnostic criteria for temporomandibular disorders. J Oral Rehabil 41(1):2–23. https://doi.org/10.1111/joor.12132
Michelotti A, Alstergren P, Goulet JP, Lobbezoo F, Ohrbach R, Peck C, Schiffman E, List T (2016) Next steps in development of the diagnostic criteria for temporomandibular disorders (DC/TMD): recommendations from the international RDC/TMD consortium network workshop. J Oral Rehabil 43(6):453–467. https://doi.org/10.1111/joor.12378
Shamseer L, Moher D, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA, Group P-P (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015: elaboration and explanation. BMJ 349:g7647. https://doi.org/10.1136/bmj.g7647
Pantoja L L Q TIP, Pupo YM, Porporatti AL, Canto De GL , Zwir LF, Guerra ENS (2017) Prevalence of degenerative disease in temporomandibular joint: a systematic review. PROSPERO 2017:CRD42017060281. Available from http://www.crd.york.ac.uk/PROSPERO/display_recordasp?ID=CRD42017060281
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A (2016) Rayyan-a web and mobile app for systematic reviews. Syst Rev 5(1):210. https://doi.org/10.1186/s13643-016-0384-4
O'Connor D GS, Higgins JPT (2011) Cochrane handbook for systematic reviews of interventions. The Cochrane Collaboration
Munn Z, Moola S, Riitano D, Lisy K (2014) The development of a critical appraisal tool for use in systematic reviews addressing questions of prevalence. Int J Health Policy Manag 3(3):123–128. https://doi.org/10.15171/ijhpm.2014.71
Abramowicz S, Kim S, Susarla HK, Kaban LB (2013) Differentiating arthritic from myofascial pain in children with juvenile idiopathic arthritis: preliminary report. J Oral Maxillofac Surg 71(3):493–496
Bakke M, Petersson A, Wiese M, Svanholt P, Sonnesen L (2014) Bony deviations revealed by cone beam computed tomography of the temporomandibular joint in subjects without ongoing pain. J Oral Facial Pain Headache 28(4):331–337
Bauss O, Sadat-Khonsari R, Fenske C, Engelke W, Schwestka-Polly R (2004) Temporomandibular joint dysfunction in Marfan syndrome. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 97(5):592–598
Bernhardt O, Biffar R, Kocher T, Meyer G (2007) Prevalence and clinical signs of degenerative temporomandibular joint changes validated by magnetic resonance imaging in a non-patient group. Ann Anat 189(4):342–346
Bertram S, Rudisch A, Innerhofer K, PÜMpel E, Grub-Wieser G, Emshoff R (2001) Diagnosing TMJ internal derangement and osteoarthritis with magnetic resonance imaging. J Am Dent Assoc 132(6):753–761. https://doi.org/10.14219/jada.archive.2001.0272
Celiker R, Gokce-Kutsal Y, Eryilmaz M (1995) Temporomandibular joint involvement in rheumatoid arthritis. Relationship with disease activity. Scand J Rheumatol 24(1):22–25
Cordeiro PCFGJ, Souza VA, Dias IM, Silva JNN, Devito KL, Bonato LL (2016) Temporomandibular joitn involvement in rheumatoid arthritis patients: association between clinical and tomographic data. Acta Odontol Latinoam 29(3):219–224
Dias GM, Bonato LL, Guimarães JP, Nogueira Silva JN, Ferreira LA, Grossmann E, Pires Carvalho AC (2015) A study of the association between sleep bruxism, low quality of sleep, and degenerative changes of the temporomandibular joint. J Craniofac Surg 26(8):2347–2350
Eberhard L, Giannakopoulos NN, Rohde S, Schmitter M (2013) Temporomandibular joint (TMJ) disc position in patients with TMJ pain assessed by coronal MRI. Dentomaxillofac Radiol 42(6):20120199
Emshoff R, Brandimaier I, Bertram S, Rudisch A (2002) Magnetic resonance imaging findings of osteoarthrosis and effusion in patients with unilateral temporomandibular joint pain. Int J Oral Maxillofac Surg 31(6):598–602
Emshoff R, Brandlmaier I, Gerhard S, Strobl H, Bertram S, Rudisch A (2003) Magnetic resonance imaging predictors of temporomandibular joint pain. J Am Dent Assoc 134(6):705–714
Emshoff R, Innerhofer K, Rudisch A, Bertram S (2002) The biological concept of "internal derangement and osteoarthrosis": a diagnostic approach in patients with temporomandibular joint pain? Oral Surg Oral Med Oral Pathol Oral Radiol Endod 93(1):39–44
Emshoff R, Rudisch A, Bosch R, Strobl H (2003) Prognostic indicators of the outcome of arthrocentesis: a short-term follow-up study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 96(1):12–18
Emshoff R, Rudisch A, Innerhofer K, Bösch R, Bertram S (2001) Temporomandibular joint internal derangement type III: relationship to magnetic resonance imaging findings of internal derangement and osteoarthrosis. Int J Oral Maxillofac Surg 30(5):390–396
Ferraz Júnior AML, Devito KL, Guimarães JP (2012) Temporomandibular disorder in patients with juvenile idiopathic arthritis: clinical evaluation and correlation with the findings of cone beam computed tomography. Oral Surg Oral Med Oral Pathol Oral Radiol 114(3):e51–e57
Helenius LM, Tervahartiala P, Helenius I, Al-Sukhun J, Kivisaari L, Suuronen R, Kautiainen H, Hallikainen D, Lindqvist C, Leirisalo-Repo M (2006) Clinical, radiographic and MRI findings of the temporomandibular joint in patients with different rheumatic diseases. Int J Oral Maxillofac Surg 35(11):983–989. https://doi.org/10.1016/j.ijom.2006.08.001
Holmlund A, Axelsson S (1994) Temporomandibular joint osteoarthrosis; correlation of clinical and arthroscopic findings with degree of molar support. Acta Odontol Scand 52(4):214–218
Keller H, Muller LM, Markic G, Schraner T, Kellenberger CJ, Saurenmann RK (2015) Is early TMJ involvement in children with juvenile idiopathic arthritis clinically detectable? Clinical examination of the TMJ in comparison with contrast enhanced MRI in patients with juvenile idiopathic arthritis. Pediatr Rheumatol 13:56
Kim K, Wojczynska A, Lee JY (2016) The incidence of osteoarthritic change on computed tomography of Korean temporomandibular disorder patients diagnosed by RDC/TMD; a retrospective study. Acta Odontol Scand 74(5):337–342. https://doi.org/10.3109/00016357.2015.1136678
Kurita H, Kojima Y, Nakatsuka A, Koike T, Kobayashi H, Kurashina K (2004) Relationship between temporomandibular joint (TMJ)-related pain and morphological changes of the TMJ condyle in patients with temporomandibular disorders. Dentomaxillofac Radiol 33(5):329–333
Lamot U, Strojan P, Popovič KŠ (2013) Magnetic resonance imaging of temporomandibular joint dysfunction-correlation with clinical symptoms, age, and gender. Oral Surg Oral Med Oral Pathol Oral Radiol 116(2):258–263
Massilla Mani F, Sivasubramanian SS (2016) A study of temporomandibular joint osteoarthritis using computed tomographic imaging. Biom J 39(3):201–206. https://doi.org/10.1016/j.bj.2016.06.003
Mohammed Y, Saeed O, Zaghloul N, Samer S, Mahmud S, Abdulah A (2012) Juvenile idiopathic arthritis and the temporomandibular joint. Alex J Med 48(2):123–129. https://doi.org/10.1016/j.ajme.2011.11.004
Resnick CM, Dang R, Henderson LA, Zander DA, Daniels KM, Nigrovic PA, Kaban LB (2017) Frequency and morbidity of temporomandibular joint involvement in adult patients with a history of juvenile idiopathic arthritis. J Oral Maxillofac Surg 75(6):1191–1200. https://doi.org/10.1016/j.joms.2016.11.013
Schmitter M, Essig M, Seneadza V, Balke Z, Schroder J, Rammelsberg P (2010) Prevalence of clinical and radiographic signs of osteoarthrosis of the temporomandibular joint in an older persons community. Dentomaxillofac Radiol 39(4):231–234. https://doi.org/10.1259/dmfr/16270943
Svechtarov V, Nencheva-Svechtarova S, Uzunov T (2015) Analysis of chronic temporomandibular disorders based on the latest diagnostic criteria. Acta Med Bulg 42(1):49–55
Takahara N, Nakagawa S, Sumikura K, Kabasawa Y, Sakamoto I, Harada H (2017) Association of Temporomandibular Joint Pain According to magnetic resonance imaging findings in temporomandibular disorder patients. J Oral Maxillofac Surg 75:1848–1855. https://doi.org/10.1016/j.joms.2017.03.026
Weiss PF, Arabshahi B, Johnson A, Bilaniuk LT, Zarnow D, Cahill AM, Feudtner C, Cron RQ (2008) High prevalence of temporomandibular joint arthritis at disease onset in children with juvenile idiopathic arthritis, as detected by magnetic resonance imaging but not by ultrasound. Arthritis Rheum 58(4):1189–1196
Wiberg B, Wanman A (1998) Signs of osteoarthrosis of the temporomandibular joints in young patients - A clinical and radiographic study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 86(2):158–164
Dworkin SF, LeResche L (eds) (1992) Research diagnostic criteria for temporomandibular disorders: review, criteria, examinations and specifications, critique. J Craniomandib Disord Facial Oral Pain 6(4):301–355
Al-Shwaikh H, Urtane I, Pirttiniemi P, Pesonen P, Krisjane Z, Jankovska I, Davidsone Z, Stanevica V (2016) Radiologic features of temporomandibular joint osseous structures in children with juvenile idiopathic arthritis. Cone beam computed tomography study. Stomatologija 18(2):51–60
Sokolove J, Brennan MJ, Sharpe O, Lahey LJ, Kao AH, Krishnan E, Edmundowicz D, Lepus CM, Wasko MC, Robinson WH (2013) Brief report: citrullination within the atherosclerotic plaque: a potential target for the anti-citrullinated protein antibody response in rheumatoid arthritis. Arthritis Rheum 65(7):1719–1724. https://doi.org/10.1002/art.37961
Krishnamoorthy B, Mamatha N, Kumar VA (2013) TMJ imaging by CBCT: current scenario. Ann Maxillofac Surg 3(1):80–83. https://doi.org/10.4103/2231-0746.110069
Alexiou K, Stamatakis H, Tsiklakis K (2009) Evaluation of the severity of temporomandibular joint osteoarthritic changes related to age using cone beam computed tomography. Dentomaxillofac Radiol 38(3):141–147. https://doi.org/10.1259/dmfr/59263880
Navallas M, Inarejos EJ, Iglesias E, Cho Lee GY, Rodriguez N, Anton J (2017) MR imaging of the temporomandibular joint in juvenile idiopathic arthritis: technique and findings. Radiographics 37(2):595–612. https://doi.org/10.1148/rg.2017160078
McInnes IBSG (2011) The pathogenesis of rheumatoid arthritis. N Engl J Med 365(23):2205–2219
Al-Ekrish AA, Al-Juhani HO, Alhaidari RI, Alfaleh WM (2015) Comparative study of the prevalence of temporomandibular joint osteoarthritic changes in cone beam computed tomograms of patients with or without temporomandibular disorder. Oral Surg Oral Med Oral Pathol Oral Radiol 120(1):78–85. https://doi.org/10.1016/j.oooo.2015.04.008
Comert Kilic S, Kilic N, Sumbullu MA (2015) Temporomandibular joint osteoarthritis: cone beam computed tomography findings, clinical features, and correlations. Int J Oral Maxillofac Surg 44(10):1268–1274. https://doi.org/10.1016/j.ijom.2015.06.023
Silman AJ, Pearson JE (2002) Epidemiology and genetics of rheumatoid arthritis. Arthritis Res 4(Suppl 3):S265–S272. https://doi.org/10.1186/ar578
Funding
This work was not supported by any sources of consultants’ fees or other financial arrangements paid directly to investigators.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Pantoja, L.L.Q., de Toledo, I.P., Pupo, Y.M. et al. Prevalence of degenerative joint disease of the temporomandibular joint: a systematic review. Clin Oral Invest 23, 2475–2488 (2019). https://doi.org/10.1007/s00784-018-2664-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2664-y