Abstract
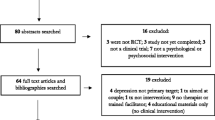
Postpartum depression (PPD) is a common complication of childbirth with prevalence estimated at 10–20% reported in many countries, including Israel. However, no data has been reported for Israeli Bedouin women, whose lifestyle is significantly different from that of the general population. This study aimed to determine the prevalence of PPD among Bedouin women in the southern Negev. The study included 104 women attending public health clinics for pregnancy and postpartum care. PPD symptoms were assessed using the Edinburgh Postnatal Depression Scale (EPDS). The rate of PPD symptoms was 43% at the EPDS cut-off score of 10, and 26% at the more stringent cut-off score of 13. This rate is considerably higher than reported rates among Israeli Jewish women. No significant difference was found between a score of ≥10 and maternal age, number of children, or level of education; however, at the EPDS score of ≥13, there was an inverse relationship between educational level and PPD symptoms. Lower rates were found among women whose pregnancies were planned and those who worked out of the home. The high rate of PPD among these Israeli Bedouin women challenges health authorities to find ways minimize the negative consequences for themselves, their children, and families.


Similar content being viewed by others
References
Abbot MW, Williams MM (2006) Postnatal depressive symptoms among Pacific mothers in Auckland: prevalence and risk factors. Aust NZ J Psychiatry 40:230–238
Abou-Saleh MT, Ghubash R (1997) The prevalence of early postpartum psychiatric morbidity in Dubai: a transcultural perspective. Acta Psychiatr Scand 95:428–432
Al-Krenawi A, Graham J (1999) Gender and biomedical/traditional mental health utilization among the Bedouin-Arabs of the Negev. Cult Med Psychiatr 23:219–243
Al-Krenawi A, Slonim-Nevo V (2008) The psychosocial profile of Bedouin Arab women lining in polygamous and monogamous marriages. J Contemp Soc Services 89:1
Bagedahl-Strindlund M, Monsen BK (1998) Postnatal depression: a hidden illness. Acta Psychiatr Scand 98:272–275
Ben-Gurion University of the Negev (2004) Statistical yearbook of the Negev Bedouin; In cooperation with Konrad Adenauer foundation. Be'er Sheva, Israel
Brockington I (2004) Postpartum psychiatric disorders. Lancet 363:303–310
Caspi Y, Slobodin O, Krammerer N, Enosh G, Shorer S, Klein E (2010) Bedouin wives on the home front: living with men serving in the Israel defense forces. J Trauma Stress 12:682–690
Central Bureau of Statistics: Population in Israel. Jerusalem http://www1.cbs.gov.il/reader/shnaton/templ_shnaton_e.html?num_tab=st02_01&CYear=2009, Accessed Jan. 24, 2011
Chaaya M, Campbell OM, El Kak F, Shaar D, Harb H, Kaddour A (2002) Postpartum depression: prevalence and determinants in Lebanon. Arch Womens Ment Health 5(2):65–72
Chaudron LH, Szilagyi PG, Kitzman HJ, Wadkins H, Conwell Y (2004) Detection of postpartum symptoms by screening at well-child visits. Pediatrics 113(3):551–558
Cooper P, Murray L (1997) Prediction, detection and treatment of postnatal depression. Arch Dis Child 77:97–101
Cox JL, Holden J (2003) A guide to the Edinburgh postnatal depression scale. Gaskell, London
Cwikel J, Barak N (2002) The health and welfare of Bedouin Arab women in the Negev. Center for women's health studies and promotion. The center for Bedouin studies and development, Be'er Sheva, Israel
Diego MA, Field T, Hernandez-Reif M, Cullen C, Schanberg S, Kuhn C (2004) Prepartum, postpartum and chronic depression effects on newborns. Psychiatry 67:63–80
Edhborg M, Friberg M, Lundh W, Widstrom AM (2005) “Struggling with life”: narratives from women with signs of postpartum depression. Scand J Public Health 33(4):261–267
Eilat-Tsanani S, Merom A, Romano S, Reshef A, Lavi I, Tabenkin H (2006) The effect of postpartum depression on women's consultations with physicians. Isr Med Assoc J 8(6):406–410
El-Khoury N, Karam EG, Melhem NM (1999) Depression and pregnancy. J Med Liban 47(3):169–174, May-Jun
Evins GG, Theofrastous JP, Galvin SL (2000) Postpartum depression: a comparison of screening and routine clinical evaluation. American J Obstetric Gynecol 182:1080–1082
Felice E, Saliba J, Grech V, Cox J (2004) Prevalence rates and psychosocial characteristics associated with depression pregnancy and postpartum in Maltese women. J Affect Disord 82:297–301
Gaynes BN, Gavin N, Meltzer-Brody S, Lohr KN, Swinson T, Gartlehner G, Brody S, Miller WC (2005) Perinatal depression: prevalence, screening accuracy and screening outcomes. Evidence Report/Technology Assessment: Number 119. AHRQ Pub. No. 05-E006-1
Ghubash R, Abou-Saleh MT, Daradkeh TK (1997) The validity of the Arabic Edinburgh postnatal depression scale. Soc Psychiatry Psychiatr Epidemiol 32(8):474–476
Glasser S, Barell V, Shoham A, Ziv A, Boyko V, Lusky A, Hart S (1998) Prospective study of postpartum depression in an Israeli cohort: prevalence, incidence and demographic risk factors. J Psychosom Obstet Gynaecol 19:155–164
Glasser S, Barell V (1999) Depression scale for research and identification of postpartum depression. Harefuah 136:764–768 (in Hebrew)
Goldbort J (2006) Transcultural analysis of postpartum depression. MCN Am J Matern Child Nurs 31:121–126
Green K, Broome H, Mirabella J (2006) Postnatal depression among mothers in the United Arab Emirates: socio-cultural and physical factors. Psychol Health Med 11(4):425–431
Hackney M (1996) The effect of postnatal depression on older siblings. Marce' Society Bulletin March:12–13
Hay DF, Pawlby S, Sharp D, Asten P, Mills A, Kumar R (2001) Intellectual problems shown by 11-year-old children whose mothers had postnatal depression. J Child Psychol Psychiatr 42:871–889
Hearn G, Iliff A, Jones I, Kirby A, Ormiston P, Parr P, Rout J, Wardman L (1998) Postnatal depression in the community. Br J Gen Pract 48:1064–1066
Kandel-Katznelson S, Maisel S, Zilber N, Lerner J (2000) Validation of the Hebrew translation of the Edinburgh postnatal depression scale: background, methods and findings. Tenth Annual Conference of the Israeli Psychiatric Association, Jerusalem, Hebrew
Kaplan G, Glasser S, Murad H, Atamna A, Alpert G, Goldbourt U, Kalter-Leibovici O (2010) Depression among Arabs and Jews in Israel: a population-based study. Soc Psychiatry Psychiatr Epidemiol 45:931–939
Kheirabadi GR, Maracy MR, Barekatain M, Salehi M, Sadri GH, Kelishadi M, Cassy P (2009) Risk factors of postpartum depression in rural areas of Isfahan Province, Iran. Arch Iran Med 12(5):461–467
Knesset (2010) Bedouins in the State of Israel. Jerusalem http://www.knesset.gov.il/lexicon/eng/bedouim_eng.htm, Accessed April 3, 2011
Lee D, Yip A, Chiu H, Leung T, Chung T (2001) A psychiatric epidemiological study of postpartum Chinese women. Am J Psychiatry 158:220–226
Lodgson MC, Wisner KL, Pinto-Foltz MD (2006) The impact of postpartum depression on mothering. JOGGN 35:652–658
Murray L, Sinclair D, Cooper P, Ducournau P, Turner P, Stein A (1999) The socioemotional development of 5-year-old children of postnatally depressed mothers. J Child Psychol Psychiatry 40:1259–1271
Pessate-Schubert A (2003) Changing from the margins: Bedouin women and higher education in Israel. Women's Studies International Forum 26:285–298
Rubertsson C, Wickberg B, Gustavsson P, Radestad I (2005) Depressive symptoms in early pregnancy, two months and one year postpartum—prevalence and psychosocial risk factors in a national Swedish sample. Arch Womens Ment Health 8:97–104
Wisner KL, Chambers C, Sit DK (2006) Postpartum depression: a major public health problem. JAMA 296(21):2616–2618
Whitton A, Warner R, Appleby L (1996) The pathway to care in postnatal depression: women's attitudes to post-depression and its treatment. Br J Gen Pract 46:427–428
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Glasser, S., Stoski, E., Kneler, V. et al. Postpartum depression among Israeli Bedouin women. Arch Womens Ment Health 14, 203–208 (2011). https://doi.org/10.1007/s00737-011-0216-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00737-011-0216-4