Abstract
Purpose
To compare the predictive validity of the Edinburgh Postnatal Depression Scale (EPDS) and other tools for screening depression in pregnant and postpartum women through a systematic review and meta-analysis.
Methods
An electronic search of MEDLINE, EMBASE, CINAHL, and PsycArticles databases was conducted using the following keywords: depression, perinatal-related terms, and EPDS. Quality Assessment of Diagnostic Accuracy Studies-2 was used to assess the risk of bias in diagnostic studies.
Results
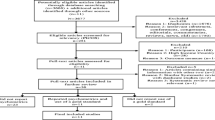
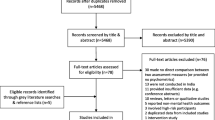
The search identified 823 articles, of which 17 studies met the inclusion criteria. In 1831 pregnant women from nine studies, pooled sensitivity and specificity of the EPDS were 0.81 and 0.87, respectively, with summary receiver operating characteristic (sROC) curve of 0.90. In 515 postpartum women from six studies, pooled sensitivity, specificity, and sROC were 0.79, 0.92, and 0.90, respectively. We then compared the EPDS with other tools using three or more studies. The sROC curve of the Patient Health Questionnaire-9 was 0.74, which was lower than that (0.86) of the EPDS. The sROC curve of the Beck Depression Inventory and the ten-item Kessler Psychological Distress Scale was 0.91, similar to that of the EPDS (0.90 and 0.87). However, in comparison with the Postpartum Depression Screening Scale (0.98), the sROC curve of the EPDS was 0.54.
Conclusion
As a tool specialized for screening depression in pregnant and postpartum women, the EPDS showed excellent performance. Thus, the EPDS can be used in preference to other tools to screen for depression in perinatal women at a primary care setting or a midwifery center.




Similar content being viewed by others
Data availability
Yes.
References
Biaggi A, Conroy S, Pawlby S, Pariante CM (2016) Identifying the women at risk of antenatal anxiety and depression: a systematic review. J Affect Disord 191:62–77. https://doi.org/10.1016/j.jad.2015.11.014
Hay DF, Pawlby S, Waters CS, Sharp D (2008) Antepartum and postpartum exposure to maternal depression: different effects on different adolescent outcomes. J Child Psychol Psychiatry 49:1079–1088. https://doi.org/10.1111/j.1469-7610.2008.01959.x
Kingston D, Kehler H, Austin MP et al (2018) Trajectories of maternal depressive symptoms during pregnancy and the first 12 months postpartum and child externalizing and internalizing behavior at three years. PLoS One 13(4):e0195365. https://doi.org/10.1371/journal.pone.0195365
Guintivano J, Manuck T, Meltzer-Brody S (2018) Predictors of postpartum depression: a comprehensive review of the last decade of evidence. Clin Obstet Gynecol 61(3):591–603. https://doi.org/10.1097/GRF.0000000000000368
Leigh B, Milgrom J (2008) Risk factors for antenatal depression, postnatal depression and parenting stress. BMC Psychiatry 8(1):24. https://doi.org/10.1186/1471-244X-8-24
ACOG committee on practice bulletins-obstetrics (2018) ACOG Practice Bulletin: Clinical management guidelines for obstetrician-gynecologists number 92, April 2008 (replaces practice bulletin number 87, November 2007) use of psychiatric medications during pregnancy and lactation. Obstet Gynecol 111:1001–1020. https://doi.org/10.1097/AOG.0b013e31816fd910 (Reaffirmed Obstet Gynecol 131:185. Reaffirmed 2020)
Stewart DE (2011) Clinical practice depression during pregnancy. N Engl J Med 365(17):1605–1611. https://doi.org/10.1056/NEJMcp1102730
Fitelson E, Kim S, Baker AS, Leight K (2010) Treatment of postpartum depression: clinical, psychological and pharmacological options. Int J Womens Health 3:1–14. https://doi.org/10.2147/IJWH.S6938
Horowitz JA, Goodman JH (2005) Identifying and treating postpartum depression. JOGNN 34(2):264–273. https://doi.org/10.1177/0884217505274583
Szegedi A, Jansen WT, van Willigenburg AP, van der Meulen E, Stassen HH, Thase ME (2009) Early improvement in the first 2 weeks as a predictor of treatment outcome in patients with major depressive disorder: a meta-analysis including 6562 patients. J Clin Psychiatry 70(3):344–353. https://doi.org/10.4088/JCP.07m03780
Ren Y, Yang H, Browning C, Thomas S, Liu M (2015) Performance of screening tools in detecting major depressive disorder among patients with coronary heart disease: a systematic review. Med Sci Monit 21:646–653. https://doi.org/10.12659/MSM.892537
Buist A, Bilszta J, Barnett B et al (2005) Recognition and management of perinatal depression in general practice: a survey of GPs and postnatal women. Aust Fam Phys 34:787–790
Callister LC, Beckstrand RL, Corbett C (2011) Postpartum depression and help-seeking behaviors in immigrant hispanic women. JOGNN 40(4):440–449
ACOG (2018) ACOG committee opinion no. 757 summary: screening for perinatal depression. Obstet Gynecol 132:1314–1316. https://doi.org/10.1097/AOG.0000000000002928
Cox JL, Holden JM, Sagovsky R (1987) Detection of postnatal depression. development of the 10-item Edinburgh postnatal depression scale. Br J Psychiatry 150:782–786. https://doi.org/10.1192/bjp.150.6.782
Rachel E (2015) Perinatal mental health: the Edinburgh postnatal depression scale, Manual 2nd edn. In: Cox J, Holden JM, Henshaw CM (eds) RCPsych, vol 25. Primary Health Care, London, p 12
Lyubenova A et al (2021) Depression prevalence based on the Edinburgh postnatal depression scale compared to structured clinical interview for DSM disorders classification: systematic review and individual participant data meta-analysis. Int J Methods Psychiatr Res 30(1):1–13. https://doi.org/10.1002/mpr.1860
Levis B, Yan XW, He C, Sun Y, Benedetti A, Thombs BD (2019) Comparison of depression prevalence estimates in meta-analyses based on screening tools and rating scales versus diagnostic interviews: a meta-research review. BMC Med 17(1):65–65. https://doi.org/10.1186/s12916-019-1297-6
Levis B, Negeri A, Sun Y et al (2020) Accuracy of the Edinburgh postnatal depression scale (EPDS) for screening to detect major depression among pregnant and postpartum women: systematic review and meta-analysis of individual participant data. BMJ 371:m4022. https://doi.org/10.1136/bmj.m4022
Thombs BD, Benedetti A, Kloda LA et al (2015) Diagnostic accuracy of the Edinburgh postnatal depression scale (EPDS) for detecting major depression in pregnant and postnatal women: protocol for a systematic review and individual patient data meta-analyses. BMJ Open 5(10):e009742. https://doi.org/10.1136/bmjopen-2015-009742
Bossuyt PM, Davenport C, Deeks JJ et al. (2013) Cochrane handbook for systematic reviews of diagnostic test accuracy. The cochrane training. https://training.cochrane.org/resource/cochrane-handbook-systematic-reviews-diagnostic-test-accuracy. Accessed 15 May 2021
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Whiting PF, Rutjes AW, Westwood ME et al (2011) QUADAS-2: a revised tool for the quality assessment of diagnostic accuracy studies. Ann Intern Med 155:529–536. https://doi.org/10.7326/0003-4819-155-8-201110180-00009
Negeri ZF, Shaikh M, Beyene J (2018) Bivariate random-effects meta-analysis models for diagnostic test accuracy studies using arcsine-based transformations. Biom J 60:827–844. https://doi.org/10.1002/bimj.201700101
Zamora J, Abraira V, Muriel A et al (2006) Meta-DiSc: a software for meta-analysis of test accuracy data. BMC Med Res Methodol 6(1):31–31. https://doi.org/10.1186/1471-2288-6-31
Patel A, Cooper N, Freeman S et al (2021) Graphical enhancements to summary receiver operating characteristic plots to facilitate the analysis and reporting of meta-analysis of diagnostic test accuracy data. Res Synth Methods 12:34–44. https://doi.org/10.1002/jrsm.1439
Freeman SC, Kerby CR, Patel A et al (2019) Development of an interactive web-based tool to conduct and interrogate meta-analysis of diagnostic test accuracy studies: MetaDTA. BMC Med Res Methodol 19:81
Greiner M, Pfeiffer D, Smith RD (2000) Principles and practical application of the receiver-operating characteristic analysis for diagnostic tests. Prev Vet Med 45:23–41. https://doi.org/10.1016/S0167-5877(00)00115-X
Walter SD (2002) Properties of the summary receiver operating characteristic (SROC) curve for diagnostic test data. Stat Med 21:1237–1256
Matthey S, Souter K, Valenti B, Ross-Hamid C (2019) Validation of the MGMQ in screening for emotional difficulties in women during pregnancy. J Affect Disord 256:156–163. https://doi.org/10.1016/j.jad.2019.05.037
Naja S, Al Kubaisi N, Chehab M, Al Dahshan A, Abuhashem N, Bougmiza I (2019) Psychometric properties of the Arabic version of EPDS and BDI-II as a screening tool for antenatal depression: evidence from Qatar. BMJ Open 9(9):e030365. https://doi.org/10.1136/bmjopen-2019-030365
Sasaki Y, Baba T, Oyama R, Fukumoto K, Haba G, Sasaki M (2019) Re-evaluation of the Edinburgh postnatal depression scale as screening for post-partum depression in Iwate prefecture, Japan. J Obstet Gynaecol Res 45(9):1876–1883. https://doi.org/10.1111/jog.14042
Chorwe-Sungani G, Chipps J (2018) Validity and utility of instruments for screening of depression in women attending antenatal clinics in Blantyre district in Malawi. S Afr Fam Pract 60:114–120. https://doi.org/10.4102/safp.v60i4.4888
Green EP, Tuli H, Kwobah E, Menya D, Chesire I, Schmidt C (2018) Developing and validating a perinatal depression screening tool in Kenya blending Western criteria with local idioms: a mixed methods study. J Affect Disord 228:49–59. https://doi.org/10.1016/j.jad.2017.11.027
van Heyningen T, Honikman S, Tomlinson M, Field S, Myer L (2018) Comparison of mental health screening tools for detecting antenatal depression and anxiety disorders in South African women. PLoS One [Electronic Res] 13(4):e0193697. https://doi.org/10.1371/journal.pone.0193697
Castro CT, Martins Brancaglion MY, Nogueira CM, Bergo PA, Duarte GF, Nicolato R, Lopes PAR, Vitor LH, Correa H (2015) What is the best tool for screening antenatal depression? J Affect Disord 178:12–17. https://doi.org/10.1016/j.jad.2015.02.003
Gawlik S, Waldeier L, Muller M, Szabo A, Sohn C, Reck C (2013) Subclinical depressive symptoms during pregnancy and birth outcome–a pilot study in a healthy German sample. Arch Womens Ment Health 16(2):93–100. https://doi.org/10.1007/s00737-012-0320-0
Tandon SD, Cluxton-Keller F, Leis J, Le HN, Perry DFA (2012) Comparison of three screening tools to identify perinatal depression among low-income African American women. J Affect Disord 136(1–2):155–162. https://doi.org/10.1016/j.jad.2011.07.014
Fernandes MC, Srinivasan K, Stein AL, Menezes G, Sumithra R, Ramchandani PG (2011) Assessing prenatal depression in the rural developing world: a comparison of two screening measures. Arch Womens Ment Health 14(3):209–216. https://doi.org/10.1007/s00737-010-0190-2
Flynn HA, Sexton M, Ratliff S, Porter K, Zivin K (2011) Comparative performance of the Edinburgh postnatal depression scale and the patient health questionnaire-9 in pregnant and postpartum women seeking psychiatric services. Psychiatry Res 187(1–2):130–134. https://doi.org/10.1016/j.psychres.2010.10.022
Tran TD, Tran T, La B, Lee D, Rosenthal D, Fisher J (2011) Screening for perinatal common mental disorders in women in the North of Vietnam: a comparison of three psychometric instruments. J Affect Disord 133(1–2):281–293. https://doi.org/10.1016/j.jad.2011.03.038
Tesfaye M, Hanlon C, Wondimagegn D, Alem A (2010) Detecting postnatal common mental disorders in Addis Ababa, Ethiopia: validation of the Edinburgh postnatal depression scale and kessler scales. J Affect Disord 122(1–2):102–108. https://doi.org/10.1016/j.jad.2009.06.020
Hanusa BH, Scholle SH, Haskett RF, Spadaro K, Wisner KL (2008) Screening for depression in the postpartum period: a comparison of three instruments. J Womens Health 17(4):585–596. https://doi.org/10.1016/j.jmwh.2008.07.005
White G. (2008) A comparison of the postpartum depression screening scale (PDSS) with the Edinburgh postnatal depression scale (EPDS). New Zealand college of midwives journal 10(39):28–32. https://link.gale.com/apps/doc/A206107529/HRCA?u=anon~2d3f0f29&sid=googleScholar&xid=3b00c4bb. Accessed 7 Aug 2021
Su KP, Chiu TH, Huang CL, Ho M, Lee CC, Wu PL, Lin CY, Liau CH, Liao CC, Chiu WC, Pariante CM (2007) Different cutoff points for different trimesters? the use of Edinburgh postnatal depression scale and beck depression inventory to screen for depression in pregnant Taiwanese women. Gen Hosp Psychiatry 29(5):436–441. https://doi.org/10.1016/j.genhosppsych.2007.05.005
Beck CT, Gable RK (2001) Comparative analysis of the performance of the postpartum depression screening scale with two other depression instruments. Nurs Res 50(4):242–250. https://doi.org/10.1097/00006199-200107000-00008
Payne JL (2016) Recent advances and controversies in peripartum depression. Curr Obstet Gynecol Rep 5(3):250–256. https://doi.org/10.1007/s13669-016-0167-x
O’Connor E, Rossom RC, Henninger M et al. (2016) Screening for depression in adults: an updated systematic evidence review for the US preventive services task force. evidence synthesis No. 128. AHRQ publication No. 14-05208-EF-1. Rockville, MD: Agency for healthcare research and quality. http://lps3.www.ncbi.nlm.nih.gov.libproxy.snu.ac.kr/books/NBK349027/?report=reader. Accessed 13 Nov 2021
Nelson HD, Cantor A, Pappas M, Weeks C (2020) Screening for anxiety in adolescent and adult women: a systematic review for the women’s preventive services initiative. Ann Intern Med 173(1):29–41. https://doi.org/10.7326/M20-0579
Reuland D, Cherrington A, Watkins GS, Bradford DW, Blanco RA, Gaynes BN (2009) Diagnostic accuracy of Spanish language depression-screening instruments. Ann Fam Med 7(5):455–462. https://doi.org/10.1370/afm.981
Wang L, Kroenke K, Stump TM, Monahan PO (2021) Screening for perinatal depression with the patient health questionnaire depression scale (PHQ-9): a systematic review and meta-analysis. Gen Hosp Psychiatry 68:74–78. https://doi.org/10.1016/j.genhosppsych.2020.12.007
Beck CT, Gable RK (2000) Postpartum depression screening scale: development and psychometric testing. Nurs Res 49(5):272–282. https://doi.org/10.1097/00006199-200009000-00006
Fellmeth G, Harrison S, Opondo C, Nair M, Kurinczuk JJ, Alderdice F (2021) Validated screening tools to identify common mental disorders in perinatal and postpartum women in India: a systematic review and meta-analysis. BMC Psychiatry 21(1):200–209. https://doi.org/10.1186/s12888-021-03190-6
Funding
This work was supported by the Soonchunhyang University Research Fund. And this study was accomplished relating to searching causes of preterm birth by a grant by a grant (NRF 2019R1F1A104579912) of the Basic Science Research Program through the National Research Foundation (NRF) funded by the Ministry of Education, Republic of Korea. The funder had no further role in the conduct of the research.
Author information
Authors and Affiliations
Contributions
All authors (SHP and JIK) contributed to the study’s conception and design, material preparation, data collection and analysis. Advanced analysis was performed by SHP. All authors have written the first draft of the manuscript and commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest or any competing interests to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Park, SH., Kim, JI. Predictive validity of the Edinburgh postnatal depression scale and other tools for screening depression in pregnant and postpartum women: a systematic review and meta-analysis. Arch Gynecol Obstet 307, 1331–1345 (2023). https://doi.org/10.1007/s00404-022-06525-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06525-0