Abstract
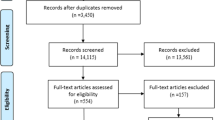
Tumor necrosis factor-alpha inhibitor (TNFi) treatment is effective for ulcerative colitis (UC) and Crohn’s disease (CD). Although several meta-analyses have been performed to evaluate the association between TNFi treatment and surgical morbidity, the results are controversial. We conducted a systematic review and meta-analysis of the prevention of surgical site infection (SSI) after surgery for UC and CD in patients on TNFis, based on literature published between January 2000 and May 2019 (registered on PROSPERO, No. CRD42019134156). Overall, 2175 UC patients in 13 observational studies (OBSs) and 7084 CD patients in 16 OBSs were included. The incidences of incisional (INC) SSI and organ/space (O/S) SSI after surgery for UC were 179/1985 (9.0%) and 176/2175 (8.1%), respectively. TNFi use was not associated with the incidences of INC SSI (odds ratio (OR) 1.04, 95% confidence interval (CI) (0.47–2.32) or O/S SSI (OR 1.85, 95% CI (0.82–4.20)) after surgery for UC. The INC SSI and O/S SSI incidences after surgery for CD were 289/3089 (9.4%) and 526/7,084 (7.4%), respectively. Preoperative TNFi use was not associated with INC SSI (OR 0.98, 95% CI (0.52–1.83)) or O/S SSI incidence (OR 1.09, 95% CI (0.78–1.52)) after surgery for CD. We did not find a significant association between preoperative TNFi use and SSI in surgery for UC or CD.




Similar content being viewed by others
References
Van Assche G, Rutgeerts P. Anti-TNF agents in Crohn’s disease. Expert Opin Investig Drugs. 2000;9:103–11.
Hanauer SB, Feagan BG, Lichtenstein GR, Mayer LF, Schreiber S, Colombel JF, et al. Maintenance infliximab for Crohn’s disease: the ACCENT I randomised trial. Lancet. 2002;359:1541–9.
Rutgeerts P, Sandborn WJ, Feagan BG, Reinisch W, Olson A, Johanns J, et al. Infliximab for induction and maintenance therapy for ulcerative colitis. N Engl J Med. 2005;353:2462–76.
Stidham RW, Lee TC, Higgins PD, Deshpande AR, Sussman DA, Singal AG, et al. Systematic review with network meta-analysis: the efficacy of anti-TNF agents for the treatment of Crohn’s disease. Aliment Pharmacol Ther. 2014;39:1349–62.
Narula N, Charleton D, Marshall JK. Meta-analysis: peri-operative anti-TNFα treatment and post-operative complications in patients with inflammatory bowel disease. Aliment Pharmacol Ther. 2013;37:1057–64.
Selvaggi F, Pellino G, Canonico S, Sciaudone G. Effect of preoperative biologic drugs on complications and function after restorative proctocolectomy with primary ileal pouch formation: systematic review and meta-analysis. Inflamm Bowel Dis. 2015;21:79–92.
Xu Y, Yang L, An P, Zhou B, Liu G. Meta-analysis: the influence of preoperative infliximab use on postoperative complications of Crohn's disease. Inflamm Bowel Dis. 2019;25:261–9.
Lin YS, Cheng SW, Wang YH, Chen KH, Fang CJ, Chen C. Systematic review with meta-analysis: risk of post-operative complications associated with pre-operative exposure to anti-tumor necrosis factor agents for Crohn’s Disease. Aliment Pharmacol Ther. 2019;49:966–77.
Culver DH, Horan TC, Gaynes RP, Martone WJ, Jarvis WR, Emori TG, et al. Surgical wound infection rates by wound class, operative procedure, and patient risk index. National nosocomial infections surveillance system. Am J Med. 1991;91:152S–S158158.
Horan TC, Gaynes RP, Martone WJ, Jarvis WR, Emori TG. CDC definitions of nosocomial surgical site infections, 1992: a modification of CDC definitions of surgical wound infections. Infect Control Hosp Epidemiol. 1992;13:606–8.
Higgins JP, Altman DG, Gøtzsche PC, Jüni P, Moher D, Oxman AD, et al. The Cochrane collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2019;343:5928.
Guyatt G, Oxman AD, Akl EA, Kunz R, Vist G, Brozek J, et al. GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. J Clin Epidemiol. 2011;64:383–94.
Kanda Y. Investigation of the freely available easy-to-use software 'EZR' for medical statistics. Bone Marrow Transplant. 2013;48:452–8.
Selvasekar CR, Cima RR, Larson DW, Dozois EJ, Harrington JR, Harmsen WS, et al. Effect of infliximab on short-term complications in patients undergoing operation for chronic ulcerative colitis. J Am Coll Surg. 2007;204:956–62.
Mor IJ, Vogel JD, da Luz MA, Shen B, Hammel J, Remzi FH. Infliximab in ulcerative colitis is associated with an increased risk of postoperative complications after restorative proctocolectomy. Dis Colon Rectum. 2008;51:1202–7.
Ferrante M, D'Hoore A, Vermeire S, Declerck S, Noman M, Van Assche G, et al. Corticosteroids but not infliximab increase short-term postoperative infectious complications in patients with ulcerative colitis. Inflamm Bowel Dis. 2009;15:1062–70.
Coquet-Reinier B, Berdah SV, Grimaud JC, Birnbaum D, Cougard PA, Barthet M, et al. Preoperative infliximab treatment and postoperative complications after laparoscopic restorative proctocolectomy with ileal pouch-anal anastomosis: a case-matched study. Surg Endosc. 2010;24:1866–71.
Gainsbury ML, Chu DI, Howard LA, Coukos JA, Farraye FA, Stucchi AF, et al. Preoperative infliximab is not associated with an increased risk of short-term postoperative complications after restorative proctocolectomy and ileal pouch-anal anastomosis. J Gastrointest Surg. 2011;15:397–403.
Bregnbak D, Mortensen C, Bendtsen F. Infliximab and complications after colectomy in patients with ulcerative colitis. J Crohns Colitis. 2012;6:281–6.
Schaufler C, Lerer T, Campbell B, Weiss R, Cohen J, Sayej W, et al. Preoperative immunosuppression is not associated with increased postoperative complications following colectomy in children with colitis. J Pediatr Gastroenterol Nutr. 2012;55:421–4.
Uchino M, Ikeuchi H, Matsuoka H, Bando T, Ichiki K, Nakajima K, et al. Infliximab administration prior to surgery does not increase surgical site infections in patients with ulcerative colitis. Int J Colorectal Dis. 2013;28:1295–306.
Gu J, Remzi FH, Shen B, Vogel JD, Kiran RP. Operative strategy modifies risk of pouch-related outcomes in patients with ulcerative colitis on preoperative anti-tumor necrosis factor-α therapy. Dis Colon Rectum. 2013;56:1243–52.
Eshuis EJ, Al Saady RL, Stokkers PC, Ponsioen CY, Tanis PJ, Bemelman WA. Previous infliximab therapy and postoperative complications after proctocolectomy with ileum pouch anal anastomosis. J Crohns Colitis. 2013;7:142–9.
Nelson R, Liao C, Fichera A, Rubin DT, Pekow J. Rescue therapy with cyclosporine or infliximab is not associated with an increased risk for postoperative complications in patients hospitalized for severe steroid-refractory ulcerative colitis. Inflamm Bowel Dis. 2014;20:14–20.
Uchino M, Ikeuchi H, Bando T, Hirose K, Hirata A, Chohno T, et al. Does pre-operative multiple immunosuppressive therapy associate with surgical site infection in surgery for ulcerative colitis. Digestion. 2015;92:121–9.
Uchino M, Ikeuchi H, Bando T, Chohno T, Sasaki H, Horio Y, et al. Associations between multiple immunosuppressive treatments before surgery and surgical morbidity in patients with ulcerative colitis during the era of biologics. Int J Colorectal Dis. 2019;34:699–710.
Marchal L, D'Haens G, Van Assche G, Vermeire S, Noman M, Ferrante M, et al. The risk of post-operative complications associated with infliximab therapy for Crohn's disease: a controlled cohort study. Aliment Pharmacol Ther. 2004;19:749–54.
Appau KA, Fazio VW, Shen B, Church JM, Lashner B, Remzi F, et al. Use of infliximab within 3 months of ileocolonic resection is associated with adverse postoperative outcomes in Crohn's patients. J Gastrointest Surg. 2008;12:1738–44.
Nasir BS, Dozois EJ, Cima RR, Pemberton JH, Wolff BG, Sandborn WJ, et al. Perioperative anti-tumor necrosis factor therapy does not increase the rate of early postoperative complications in Crohn's disease. J Gastrointest Surg. 2010;14:1859–65.
Canedo J, Lee SH, Pinto R, Murad-Regadas S, Rosen L, Wexner SD. Surgical resection in Crohn's disease: is immunosuppressive medication associated with higher postoperative infection rates? Colorectal Dis. 2011;13:1294–8.
Syed A, Cross RK, Flasar MH. Anti-tumor necrosis factor therapy is associated with infections after abdominal surgery in Crohn's disease patients. Am J Gastroenterol. 2013;108:583–93.
Nørgård BM, Nielsen J, Qvist N, Gradel KO, de Muckadell OB, Kjeldsen J. Pre-operative use of anti-TNF-α agents and the risk of post-operative complications in patients with Crohn's disease—a nationwide cohort study. Aliment Pharmacol Ther. 2013;37:214–24.
Serradori T, Germain A, Scherrer ML, Ayav C, Perez M, Romain B, et al. The effect of immune therapy on surgical site infection following Crohn's Disease resection. Br J Surg. 2013;100:1089–93.
Uchino M, Ikeuchi H, Matsuoka H, Bando T, Ichiki K, Nakajima K, et al. Risk factors for surgical site infection and association with infliximab administration during surgery for Crohn's disease. Dis Colon Rectum. 2013;56:1156–65.
Yamamoto T, Spinelli A, Suzuki Y, Saad-Hossne R, Teixeira FV, de Albuquerque IC, et al. Risk factors for complications after ileocolonic resection for Crohn's disease with a major focus on the impact of preoperative immunosuppressive and biologic therapy: a retrospective international multicentre study. United Eur Gastroenterol J. 2016;4:784–93.
Kotze PG, Saab MP, Saab B, da Silva Kotze LM, Olandoski M, Pinheiro LV, et al. Tumor necrosis factor alpha inhibitors did not influence postoperative morbidity after elective surgical resections in Crohn's disease. Dig Dis Sci. 2017;62:456–64.
Brouquet A, Maggiori L, Zerbib P, Lefevre JH, Denost Q, Germain A, et al. Anti-TNF therapy is associated with an increased risk of postoperative morbidity after surgery for ileocolonic Crohn disease: results of a prospective nationwide cohort. Ann Surg. 2018;267:221–8.
Jouvin I, Lefevre JH, Creavin B, Pitel S, Chafai N, Tiret E, et al. Postoperative morbidity risks following ileocolic resection for Crohn's disease treated with Anti-TNF alpha therapy: a retrospective study of 360 Patients. Inflamm Bowel Dis. 2018;24:422–32.
Lightner AL, McKenna NP, Tse CS, Hyman N, Smith R, Ovsepyan G, et al. Postoperative outcomes in ustekinumab-treated patients undergoing abdominal operations for Crohn's disease. J Crohns Colitis. 2018;12:402–7.
Schad CA, Haac BE, Cross RK, Syed A, Lonsako S, Bafford AC. Early postoperative anti-TNF therapy does not increase complications following abdominal surgery in Crohn's disease. Dig Dis Sci. 2019. https://doi.org/10.1007/s10620-019-5476-2.
Yu CS, Jung SW, Lee JL, Lim SB, Park IJ, Yoon YS, et al. The influence of preoperative medications on postoperative complications in patients after intestinal surgery for Crohn's disease. Inflamm Bowel Dis. 2019. https://doi.org/10.1093/ibd/izz010.
Lightner AL, McKenna NP, Alsughayer A, Loftus EV Jr, Raffals LE, Faubion WA, et al. Anti-TNF biologic therapy does not increase postoperative morbidity in pediatric Crohn's patients. J Pediatr Surg. 2019. https://doi.org/10.1016/j.jpedsurg.2019.01.006.
Clay M, Mazouyes A, Gilson M, Gaudin P, Baillet A. Risk of postoperative infections and the discontinuation of TNF inhibitors in patients with rheumatoid arthritis: a meta-analysis. Joint Bone Spine. 2016;83:701–5.
Goodman SM, Menon I, Christos PJ, Smethurst R, Bykerk VP. Management of perioperative tumour necrosis factor α inhibitors in rheumatoid arthritis patients undergoing arthroplasty: a systematic review and meta-analysis. Rheumatol (Oxf). 2016;55:573–82.
Global guidelines for the prevention of surgical site infection. 2019. https://apps.who.int/iris/bitstream/10665/250680/1/9789241549882-eng.pdf. Accessed 1 Dec 2016
Berríos-Torres SI, Umscheid CA, Bratzler DW, Leas B, Stone EC, Kelz RR, et al. Centers for disease control and prevention guideline for the prevention of surgical site infection, 2017. JAMA Surg. 2017;152:784–91.
Cornillie F, Shealy D, D'Haens G, Geboes K, Van Assche G, Ceuppens J, et al. Infliximab induces potent anti-inflammatory and local immunomodulatory activity but no systemic immune suppression in patients with Crohn's disease. Aliment Pharmacol Ther. 2001;15:463–73.
Funding
This work was partially supported by the Japan Surgical Infection Society.
Author information
Authors and Affiliations
Contributions
Conception and design: MY, TM, and HI. Literature search: MK, TM, YM, and CY. Analysis and interpretation: MU and JS. Literature assessment and review: HO, SH, JS, YM, CY, YK, KS, MK, MK, FS, HI, and YT. Writing of the article: MU. Critical revision of the article: HI, YT, and KH. Final approval of the article: MU, TM, HO, SH, JS, YM, CY, YK, KS, MK, MK, FS, MY, TM, HI, YT, and KH.
Corresponding author
Ethics declarations
Conflicts of interest
This work was supported in part by the Japan Surgical Infection Society. We have no potential conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
595_2020_2003_MOESM6_ESM.pptx
Supplemental Figure Funnel plot for the rate of incisional surgical site infection in patients undergoing surgery for A) ulcerative colitis and B) Crohn’s disease. Funnel plot for the rate of organ/space surgical site infection in patients undergoing surgery for C) ulcerative colitis and D) Crohn’s disease. The estimated effect measure is plotted on the x-axis, and the standard error is plotted on the y-axis (PPTX 57 kb)
Rights and permissions
About this article
Cite this article
Uchino, M., Ikeuchi, H., Shimizu, J. et al. Association between preoperative tumor necrosis factor alpha inhibitor and surgical site infection after surgery for inflammatory bowel disease: a systematic review and meta-analysis. Surg Today 51, 32–43 (2021). https://doi.org/10.1007/s00595-020-02003-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-020-02003-9