Abstract
Aims
To investigate the correlation of impairment in skeletal muscle and heart in spontaneous type 2 diabetes mellitus (T2DM) rhesus monkeys using magnetic resonance image (MRI).
Methods
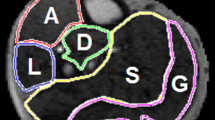
Fifteen T2DM monkeys and fourteen healthy control (HC) monkeys were included. The microcirculation of skeletal muscle [skeletal muscle blood flow (SMBF), skeletal muscle oxygen extraction fraction (SMOEF)] and the function and strain of heart were evaluated by MRI. Three regions of interests were chosen on the soleus muscle (SOL), gastrocnemius muscle (GAS) and tibialis anterior muscle (TA) for image analysis.
Results
Eight T2DM monkeys and eight HC monkeys were obtained the full data. The SMBF reserves and SMOEF reserves were found significantly decreased in T2DM during inflation in SOL, GAS and TA muscles (all p < 0.05), and the SMBF reserves decreased during hyperemia in GAS and TA muscles (all p < 0.05). In these monkeys, the global peak longitudinal strain (longitudinal PS), peak systolic longitudinal strain rate (longitudinal PSSR) and peak diastolic longitudinal strain rate (longitudinal PDSR) were seen significantly different in T2DM compared to HC monkeys (all p < 0.05). The longitudinal PSSR was found negatively correlated with SMBF reserves in SOL, GAS and TA during inflation in all monkeys.
Conclusions
The impaired microcirculation of skeletal muscle and the myocardial deformation were found in T2DM monkeys with normal ejection fraction. And a negative correlation was existed in the longitudinal PSSR and the SMBF reserves.



Similar content being viewed by others
References
Strain WD, Paldanius PM (2018) Diabetes, cardiovascular disease and the microcirculation. Cardiovasc Diabetol 17(1):57. https://doi.org/10.1186/s12933-018-0703-2
Nathan DM (2015) Diabetes: advances in diagnosis and treatment. JAMA 314(10):1052–1062. https://doi.org/10.1001/jama.2015.9536
Bigagli E, Lodovici M (2019) Circulating oxidative stress biomarkers in clinical studies on type 2 diabetes and its complications. Oxidative Med Cell Longev 2019:5953685. https://doi.org/10.1155/2019/5953685
Baltzis D, Eleftheriadou I, Veves A (2014) Pathogenesis and treatment of impaired wound healing in diabetes mellitus: new insights. Adv Ther 31(8):817–836. https://doi.org/10.1007/s12325-014-0140-x
Nichols GA, Gullion CM, Koro CE, Ephross SA, Brown JB (2004) The incidence of congestive heart failure in type 2 diabetes: an update. Diabetes Care 27(8):1879–1884. https://doi.org/10.2337/diacare.27.8.1879
Zaccardi F, Webb DR, Yates T, Davies MJ (2016) Pathophysiology of type 1 and type 2 diabetes mellitus: a 90-year perspective. Postgrad Med J 92(1084):63–69. https://doi.org/10.1136/postgradmedj-2015-133281
Piepoli MF, Crisafulli A (2014) Pathophysiology of human heart failure: importance of skeletal muscle myopathy and reflexes. Exp Physiol 99(4):609–615. https://doi.org/10.1113/expphysiol.2013.074310
Hirai DM, Copp SW, Holdsworth CT et al (2014) Skeletal muscle microvascular oxygenation dynamics in heart failure: exercise training and nitric oxide-mediated function. Am J Physiol Heart Circ Physiol 306(5):H690–H698. https://doi.org/10.1152/ajpheart.00901.2013
Lavine KJ, Sierra OL (2017) Skeletal muscle inflammation and atrophy in heart failure. Heart Fail Rev 22(2):179–189. https://doi.org/10.1007/s10741-016-9593-0
Liu X, Yang ZG, Gao Y et al (2018) Left ventricular subclinical myocardial dysfunction in uncomplicated type 2 diabetes mellitus is associated with impaired myocardial perfusion: a contrast-enhanced cardiovascular magnetic resonance study. Cardiovasc Diabetol 17(1):139. https://doi.org/10.1186/s12933-018-0782-0
Qian C, Gong L, Yang Z et al (2015) Diastolic dysfunction in spontaneous type 2 diabetes rhesus monkeys: a study using echocardiography and magnetic resonance imaging. BMC Cardiovasc Disord 15:59. https://doi.org/10.1186/s12872-015-0046-9
Zhu T, Zeng W, Chen Y et al (2018) 2D/3D CMR tissue tracking versus CMR tagging in the assessment of spontaneous T2DM rhesus monkeys with isolated diastolic dysfunction. BMC Med Imaging 18(1):47. https://doi.org/10.1186/s12880-018-0288-y
Zheng J, An H, Coggan AR et al (2014) Noncontrast skeletal muscle oximetry. Magn Reson Med 71(1):318–325. https://doi.org/10.1002/mrm.24669
Zheng J, Hastings MK, Muccigross D et al (2015) Non-contrast MRI perfusion angiosome in diabetic feet. Eur Radiol 25(1):99–105. https://doi.org/10.1007/s00330-014-3337-0
Zheng J, Hasting MK, Zhang X et al (2014) A pilot study of regional perfusion and oxygenation in calf muscles of individuals with diabetes with a noninvasive measure. J Vasc Surg 59(2):419–426. https://doi.org/10.1016/j.jvs.2013.07.115
Haddad JA, Haddad AN (2018) The past decade in type 2 diabetes and future challenges. Hormones (Athens, Greece) 17(4):451–459. https://doi.org/10.1007/s42000-018-0080-y
Rayner JO, Kalkeri R, Goebel S et al (2018) Comparative pathogenesis of Asian and African-Lineage Zika virus in Indian Rhesus Macaque’s and development of a non-human primate model suitable for the evaluation of new drugs and vaccines. Viruses. https://doi.org/10.3390/v10050229
Zhang Y, Zeng W, Chen W et al (2019) MR extracellular volume mapping and non-contrast T1rho mapping allow early detection of myocardial fibrosis in diabetic monkeys. Eur Radiol 29(6):3006–3016. https://doi.org/10.1007/s00330-018-5950-9
Wang C, Zhang R, Zhang X et al (2016) Noninvasive measurement of lower extremity muscle oxygen extraction fraction under cuff compression paradigm. J Magn Reson Imaging JMRI 43(5):1148–1158. https://doi.org/10.1002/jmri.25074
Scheuermann-Freestone M, Madsen PL, Manners D et al (2003) Abnormal cardiac and skeletal muscle energy metabolism in patients with type 2 diabetes. Circulation 107(24):3040–3046. https://doi.org/10.1161/01.Cir.0000072789.89096.10
Attar R, Wester A, Koul S, Eggert S, Andell P (2019) Peripheral artery disease and outcomes in patients with acute myocardial infarction. Open Heart 6(1):e001004. https://doi.org/10.1136/openhrt-2018-001004
Keng BMH, Gao F, Teo LLY et al (2019) Associations between skeletal muscle and myocardium in aging: a syndrome of “cardio-sarcopenia”? J Am Geriatr Soc. https://doi.org/10.1111/jgs.16132
Morris DR, Skalina TA, Singh TP, Moxon JV, Golledge J (2018) Association of computed tomographic leg muscle characteristics with lower limb and cardiovascular events in patients with peripheral artery disease. J Am Heart Assoc 7(20):e009943. https://doi.org/10.1161/jaha.118.009943
Zheng Y, Ley SH, Hu FB (2018) Global aetiology and epidemiology of type 2 diabetes mellitus and its complications. Nat Rev Endocrinol 14(2):88–98. https://doi.org/10.1038/nrendo.2017.151
Schrauwen-Hinderling VB, Kooi ME, Schrauwen P (2016) Mitochondrial function and diabetes: consequences for skeletal and cardiac muscle metabolism. Antioxid Redox Signal 24(1):39–51. https://doi.org/10.1089/ars.2015.6291
Lindner JR (2018) Cause or effect? Microvascular dysfunction in insulin-resistant states. Circ Cardiovasc Imaging 11(4):e007725. https://doi.org/10.1161/circimaging.118.007725
Leermakers PA, Gosker HR (2016) Skeletal muscle mitophagy in chronic disease: implications for muscle oxidative capacity? Curr Opin Clin Nutr Metab Care 19(6):427–433. https://doi.org/10.1097/mco.0000000000000319
Schulte AC, Aschwanden M, Bilecen D (2008) Calf muscles at blood oxygen level-dependent MR imaging: aging effects at postocclusive reactive hyperemia. Radiology 247(2):482–489. https://doi.org/10.1148/radiol.2472070828
Fitts RH, Bodine SC, Romatowski JG, Widrick JJ (1985) Velocity, force, power, and Ca2+ sensitivity of fast and slow monkey skeletal muscle fibers. J Appl Physiol 84(5):1776–1787. https://doi.org/10.1152/jappl.1998.84.5.1776
Kalam K, Otahal P, Marwick TH (2014) Prognostic implications of global LV dysfunction: a systematic review and meta-analysis of global longitudinal strain and ejection fraction. Heart (Br Card Soc) 100(21):1673–1680. https://doi.org/10.1136/heartjnl-2014-305538
Mochizuki Y, Tanaka H, Matsumoto K et al (2017) Impact of left ventricular longitudinal functional mechanics on the progression of diastolic function in diabetes mellitus. Int J Cardiovasc Imaging 33(12):1905–1914. https://doi.org/10.1007/s10554-017-1198-8
Hatani Y, Tanaka H, Mochizuki Y et al (2019) Association of body fat mass with left ventricular longitudinal myocardial systolic function in type 2 diabetes mellitus. J Cardiol. https://doi.org/10.1016/j.jjcc.2019.07.013
Funding
This study was funded by the National Natural Science Foundation of China (Grant Numbers 81520108014, 81771800, 81829003) and the State’s Key Project of Research and Development Plan of China (2016YFA0201402).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard statement
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed. The study was been approved by the Institutional Animal Care and Use Committee of Sichuan PriMed Group Co., Ltd and Sichuan University.
Informed consent
For this type of study, formal consent is not required.
Additional information
Managed By Antonio Secchi.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, Y., Zeng, W., Chen, W. et al. Evaluating the correlation of the impairment between skeletal muscle and heart using MRI in a spontaneous type 2 diabetes mellitus rhesus monkey model. Acta Diabetol 57, 673–679 (2020). https://doi.org/10.1007/s00592-019-01460-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-019-01460-0