Abstract
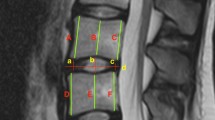
The L4/5 disc inter-space is commonly believed to be represented by a line drawn between the two highest points of the iliac crests. This line is frequently used as a pre-operative guide for incision placement, in patients undergoing spinal surgery. We reviewed the antero-posterior and lateral lumbar spine films of 450 patients, ranging in age from 20 to 90 years, measuring the distance from the supracristal plane to the midpoint of the L4/5 disc interspace. The plane intersected the spine at the L4/5 interspace in only 31.9% of cases and was found to lie at the lower half of the body of L4 or above in 49.5% of cases. There was significant variation in the position of the supracristal plane between the different patient age groups studied (P≤0.05). The use of additional imaging, along with plain radiography is advised when attempting identification of this spinal level, as reliance on palpation of the iliac crests alone to identify this landmark may lead to unintentional cranial placement of a surgical incision during spinal procedures, or cannulation at a level above the intended interspace, during epidural and spinal anaesthesia.
Résumé
L’espace discal L4–L5 est communément censé être placé sur une ligne passant entre les deux plus hauts points des crêtes iliaques. Cette ligne est fréquemment utilisée pour le repérage chez des patients installés pour une intervention chirurgicale vertébrale. Nous avons revu les radiographies d’incidences antéro-postérieures et de profil de 450 patients avec des âges extrêmes entre 20 et 90 ans et avons mesuré la distance entre le plan passant au dessus des crêtes iliaques et l’espace discal L4-L5. Ce plan ne traverse la colonne vertébrale en L4–L5 que chez 31.9% des cas et fut trouvé dans une position différente, soit dans la moitié inférieure du corps de L4, soit dans la supérieure dans 49.5% des cas. La variation du plan des crêtes iliaques chez les différents patients était significative (< ou = 005). L’utilisation d’imagerie additionnelle, en sus des radiographies conventionnelles est conseillée lorsque l’on veut identifier ce niveau vertébral, alors que la seule palpation des crêtes iliaques peut conduire à réaliser une incision trop crâniale lors d’une intervention chirurgicale ou à cathétériser un niveau supérieur lors d’une anesthésie épidurale ou d’une rachi-anesthésie.


Similar content being viewed by others
References
Aitkenhead AR, Rowbotham DJ, Smith G (eds) (2001) Textbook of anaesthesia, 4th edn. Churchill Livingstone, Edinburgh, pp 636–637
Kubota Y, Toyoda Y, Kubota H (1992) Jacoby’s line rather than Tuffier’s line as a guide to lumbar puncture. Anesth Analg 74(6):939
Standring S (ed) (2005) Gray’s anatomy: the anatomical basis of clinical practise, 39th edn. Churchill Livingstone, Edinburgh, pp 727–731
Render CA (1996) The reproducibility of the iliac crest as a marker of lumbar spine level. Anaesthesia 51(11):1070–1071
Thavasothy M (1997) The reproducibility of the iliac crest as a marker of lumbar spinal level. Anaesthesia 52(8):811
Broadbent CR, Maxwell WB, Ferrie R, Wilson DJ, Gawne-Cain M, Russell R (2000) Ability of anaesthetists to identify a marked lumber interspace. Anaesthesia 55(11):1122–1126
Furness G, Reilly MP, Kuchi S (2002) An evaluation of ultrasound imaging for identification of lumbar intervertebral level. Anaesthesia 57(3):277–280
Ievins FA (1991) Accuracy of placement of extradural catheters in the L3–4 interspace: comparison of two methods of identifying L4. Br J Anaesth 66(3):381–382
Reynolds F (2000) Logic in the safe practise of spinal anaesthesia. Anaesthesia 55(11):1045–1046
Van Gessel EF, Forster A, Gamulin Z (1993) Continuous spinal anaesthesia: where do spinal catheters go? Anesth Analg 76(5):1004–1007
Hogan QH (1994) Tuffier’s line: the normal distribution of anatomic parameters. Anesth Analg 78(1):194–195
Parry H (2001) Spinal cord damage. Anaesthesia 56(3):290
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Walsh, J.C., Quinlan, J.F., Butt, K. et al. Variation in position of the L4/5 disc inter-space from the anatomical landmark: review of 450 radiographs and clinical applications. Eur J Orthop Surg Traumatol 16, 203–206 (2006). https://doi.org/10.1007/s00590-005-0075-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-005-0075-7