Abstract
Purpose
This study aims to: (a) quantify and evaluate normal relationships between neighboring spinal units using MR imaging indices, (b) propose an easy-to-apply-and-reproduce method of estimating the correct amount of distraction when surgically restoring a collapsed intervertebral disc, based on individualized measurements.
Methods
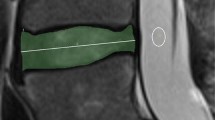
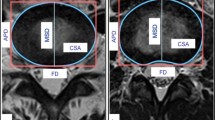
This is a retrospective cross-sectional MR imaging study of 119 adult subjects, aged 18–54, asymptomatic for low back pain. Each of the examinees should demonstrate two or more consecutive intervertebral discs classified as Pfirrmann grade I or II to be included. We measured and studied the relationships of disc height index, Dabbs index, Farfan index, disc convexity index and mean and posterior disc height per spinal level using multiple regression analysis. All measurements were tested for intra- and interobserver agreement by two raters.
Results
DHI, Dabbs, Farfan, and mean disc height had a statistically significant correlation with the spinal level and age. Our results were highly reproducible, with excellent inter- and intraobserver agreement and reliability between two raters (ICC = 0.992 and 0.994, respectively). Furthermore, we expressed each intervertebral space as a percentage of its adjacent space, introducing the coefficient α factor for every intervertebral space.
Conclusions
Our results suggest that a normal values’ database to refer during preoperative planning of correction of a degenerated intervertebral disc is feasible. Our study offers new anatomical and radiological insight in terms of spinal measurements and their potential correlation with current surgical techniques. A new approach for calculating disc space as an expression of its adjacent disc has been introduced with various potential applications.




Similar content being viewed by others
References
Adams MA, Dolan P (2012) Intervertebral disc degeneration: evidence for two distinct phenotypes. J Anat 221:497–506
Billy GG, Lemieux SK, Chow MX (2014) Changes in lumbar disk morphology associated with prolonged sitting assessed by magnetic resonance imaging. PM R 6:790–795. https://doi.org/10.1016/j.pmrj.2014.02.014
Boody BS, Rosenthal BD, Jenkins TJ, Patel AA, Savage JW, Hsu WK (2017) Iatrogenic flatback and flatback syndrome: evaluation, management, and prevention. Clin Spine Surg 30(4):142–149. https://doi.org/10.1097/BSD.0000000000000522
Dabbs VM, Dabbs LG (1990) Correlation between disc height narrowing and low-back pain. Spine (Phila Pa 1976) 15:1366–1369
Dreischarf M, Schmidt H, Putzier M, Zander T (2015) Biomechanics of the L5–S1 motion segment after total disc replacement—influence of iatrogenic distraction, implant positioning and preoperative disc height on the range of motion and loading of facet joints. J Biomech 48:3283–3291. https://doi.org/10.1016/j.jbiomech.2015.06.023
Farfan HF, Cossette JW, Robertson GH, Wells RV, Kraus H (1970) The effects of torsion on the lumbar intervertebral joints: the role of torsion in the production of disc degeneration. J Bone Joint Surg Am 52:468–497
Fleiss J (1986) The design and analysis of clinical experiments. Wiley, New York
Frobin W, Brinckmann P, Biggemann M, Tillotson M, Burton K (1997) Precision measurement of disc height, vertebral height and sagittal plane displacement from lateral radiographic views of the lumbar spine. Clin Biomech (Bristol Avon) 12(Suppl 1):S1–S63
Froholdt A, Brox JI, Reikerås O, Leivseth G (2013) Disc height and sagittal alignment in operated and non-operated levels in the lumbar spine at long-term follow-up: a case-control study. Open Orthop J 7:258–263
Haefeli M, Kalberer F, Saegesser D, Nerlich AG, Boos N, Paesold G (2006) The course of macroscopic degeneration in the human lumbar intervertebral disc. Spine (Phila Pa 1976) 31:1522–1531
Hassett G, Hart DJ, Manek NJ, Doyle DV, Spector TD (2003) Risk factors for progression of lumbar spine disc degeneration: the Chingford Study. Arthritis Rheum 48:3112–3117
Jarman JP, Arpinar VE, Baruah D, Klein AP, Maiman DJ, Tugan Muftuler L (2015) Intervertebral disc height loss demonstrates the threshold of major pathological changes during degeneration. Eur Spine J 24:1944–1950
Kaito T, Hosono N, Mukai Y, Makino T, Fuji T, Yonenobu K (2010) Induction of early degeneration of the adjacent segment after posterior lumbar interbody fusion by excessive distraction of lumbar disc space. J Neurosurg Spine 12:671–679
Kanayama M, Togawa D, Takahashi C, Terai T, Hashimoto T (2009) Cross-sectional magnetic resonance imaging study of lumbar disc degeneration in 200 healthy individuals. J Neurosurg Spine 11:501–507. https://doi.org/10.3171/2009.5.SPINE08675
Kepler CK, Rihn JA, Radcliff KE, Patel AA, Anderson DG, Vaccaro AR, Hilibrand AS, Albert TJ (2012) Restoration of lordosis and disk height after single-level transforaminal lumbar interbody fusion. Orthop Surg 4(1):15–20. https://doi.org/10.1111/j.1757-7861.2011.00165.x
Kerttula LI, Serlo WS, Tervonen OA, Pääkkö EL, Vanharanta HV (2000) Post-traumatic findings of the spine after earlier vertebral fracture in young patients: clinical and MRI study. Spine (Phila Pa 1976) 25:1104–1108
Lee JC, Choi SW (2015) Adjacent segment pathology after lumbar spinal fusion. Asian Spine J 9:807–817
Leivseth G, Braaten S, Frobin W, Brinckmann P (2006) Mobility of lumbar segments instrumented with a ProDisc II prosthesis: a two-year follow-up study. Spine (Phila Pa 1976) 31:1726–1733
Mannion AF, Leivseth G, Brox JI, Fritzell P, Hägg O, Fairbank JC (2014) ISSLS Prize winner: Long-term follow-up suggests spinal fusion is associated with increased adjacent segment disc degeneration but without influence on clinical outcome: results of a combined follow-up from 4 randomized controlled trials. Spine (Phila Pa 1976) 39:1373–1383
Meijer GJ, Homminga J, Veldhuizen AG, Verkerke GJ (2011) Influence of interpersonal geometrical variation on spinal motion segment stiffness: implications for patient-specific modeling. Spine (Phila Pa 1976) 36:E929–E935. https://doi.org/10.1097/BRS.0b013e3181fd7f7f
Pfirrmann CW, Metzdorf A, Elfering A, Hodler J, Boos N (2006) Effect of aging and degeneration on disc volume and shape: a quantitative study in asymptomatic volunteers. J Orthop Res 24:1086–1094
Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N (2001) Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine (Phila Pa 1976) 26:1873–1878
Radcliff KE, Kepler CK, Jakoi A, Sidhu GS, Rihn J, Vaccaro AR, Albert TJ, Hilibrand AS (2013) Adjacent segment disease in the lumbar spine following different treatment interventions. Spine J 13:1339–1349
Siepe CJ, Hitzl W, Meschede P, Sharma AK, Khattab MF, Mayer MH (2009) Interdependence between disc space height, range of motion and clinical outcome in total lumbar disc replacement. Spine (Phila Pa 1976) 34:904–916
Siepe CJ, Korge A, Grochulla F, Mehren C, Mayer HM (2008) Analysis of post-operative pain patterns following total lumbar disc replacement: results from fluoroscopically guided spine infiltrations. Eur Spine J 17:44–56
Siepe CJ, Mayer HM, Heinz-Leisenheimer M, Korge A (2007) Total lumbar disc replacement: different results for different levels. Spine (Phila Pa 1976) 32:782–790
Strube P, Hoff EK, Schürings M, Schmidt H, Dreischarf M, Rohlmann A, Putzier M (2013) Parameters influencing the outcome after total disc replacement at the lumbosacral junction. Part 2: distraction and posterior translation lead to clinical failure after a mean follow-up of 5 years. Eur Spine J 22:2279–2287
Teraguchi M, Yoshimura N, Hashizume H, Muraki S, Yamada H, Minamide A, Oka H, Ishimoto Y, Nagata K, Kagotani R, Takiguchi N, Akune T, Kawaguchi H, Nakamura K, Yoshida M (2014) Prevalence and distribution of intervertebral disc degeneration over the entire spine in a population-based cohort: the Wakayama Spine Study. Osteoarthr Cartil 22:104–110. https://doi.org/10.1016/j.joca.2013.10.019
Videman T, Battié MC, Parent E, Gibbons LE, Vainio P, Kaprio J (2008) Progression and determinants of quantitative magnetic resonance imaging measures of lumbar disc degeneration: a five-year follow-up of adult male monozygotic twins. Spine (Phila Pa 1976) 33:1484–1490
Wang H, Chen W, Jiang J, Lu F, Ma X, Xia X (2016) Analysis of the correlative factors in the selection of interbody fusion cage height in transforaminal lumbar interbody fusion. BMC Musculoskelet Disord 17:9
Zhong W, Driscoll SJ, Wu M, Wang S, Liu Z, Cha TD, Wood KB, Li G (2014) In vivo morphological features of human lumbar discs. Medicine (Baltimore) 93:e333. https://doi.org/10.1097/MD.0000000000000333
Author information
Authors and Affiliations
Contributions
AHF: Data analysis, manuscript writing. DLA: Project development, manuscript writing. AHK: Manuscript editing. SEV: Manuscript writing and editing. MH: Data collection and manuscript editing. AHZ: Project development, data collection, manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Fyllos, A.H., Arvanitis, D.L., Karantanas, A.H. et al. Magnetic resonance morphometry of the adult normal lumbar intervertebral space. Surg Radiol Anat 40, 1055–1061 (2018). https://doi.org/10.1007/s00276-018-2048-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-018-2048-7