Abstract
Purpose
This prospective randomised control study is to demonstrate whether or not there is a clinical benefit from inserting a Wallis implant on the functional recovery of patients who have undergone lumbar decompression surgery.
Method
Sixty consecutive patients with an average age of 58 years (34–81) who were selected for primary lumbosacral decompression were randomly assigned into two groups with equal number of patients, decompression alone or decompression with Wallis implant. The patients had an average follow-up of 40 months. Patients were assessed by visual analogue scale (VAS) (Boonstra et al., Int J Rehabil Res 31:165–169, 2008; Price et al., Pain 17:45–56, 1983) pain score for back and leg pain, and the Oswestry Disability Index questionnaire (ODI) (Smeets et al., Arthritis Care Res (Hoboken) 63:S158–S173, 2011).
Results
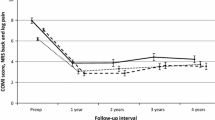
The results in both the groups did not reveal a significant difference in the clinical outcome assessment of back pain score or ODI. With the Wilcoxon two-sample test, no difference in median values was achieved (p value 0.0787 for ODI and p value 0.1926 for back pain). The average ODI in the Wallis group dropped from 50.93 to 29.11. The average VAS for the Wallis group back pain dropped from 7.79 to 4.22.
Conclusion
The Wallis implant is a safe medical device. This study revealed a reduction in pain and functional disability in patients treated with decompression surgery for lumbar stenosis, with or without Wallis. The Wallis group improved more, but it was not statistically significant. The risk of complications is lower than other interspinous devices [18, 19].

Similar content being viewed by others
References
Bono CM, Vaccaro AR (2007) Interspinous process devices in the lumbar spine. J Spinal Disord Tech 20(3):255–261
Robaina-Padrón FJ (2007) Controversies about instrumented surgery and pain relief in degenerative lumbar spine pain. Results of scientific evidence. Neurocirugia (Astur) 18(5):406–413
Korovessis P, Repantis T, Zacharatos S, Zafiropoulos A (2009) Wallis implant reduce adjacent segment degeneration above lumbosacral instrumented fusion? Eur Spine J 18(6):830–840
Floman Y, Millgram MA, Smorgick Y, Rand N, Ashkenazi EJ (2007) Failure of the Wallis interspinous implant to lower the incidence of recurrent lumbar disc herniations in patients undergoing primary disc excision. Spinal Disord Tech 20(5):337–341
Boonstra AM, Schiphorst Preuper HR, Reneman MF, Posthumus JB, Stewart RE (2008) Reliability and validity of the visual analogue scale for disability in patients with chronic musculoskeletal pain. Int J Rehabil Res 31(2):165–169
Price DD, McGrath PA, Rafii A, Buckingham B (1983) The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain 17(1):45–56
Smeets R, Köke A, Lin CW, Ferreira M, Demoulin C (2011) Measures of function in low back pain/disorders: low back pain rating scale (LBPRS), oswestry disability index (ODI), progressive isoinertial lifting evaluation (PILE), quebec back pain disability scale (QBPDS), and Roland-Morris disability questionnaire (RDQ). Arthritis Care Res (Hoboken) 63(suppl 11):S158–S173
Beyer F, Yagdiran A, Neu P, Kaulhausen T, Eysel P, Sobottke R (2013) Percutaneous interspinous spacer versus open decompression: a 2-year follow-up of clinical outcome and quality of life. Eur Spine J 22:2015–2021
Sun HL, Li CD, Liu XY, Yi XD, Lin JR, Liu H, Lu HL, Li H, Yu ZR (2013) Retrospective study of complication of interspinous implants for degenerative lumbar disease. Zhonghua Wai Ke Za Zhi 51(1):35–39
Hicks GE, Gaines JM, Shardell M, Simonsick EM (2008) Associations of back and leg pain with health status and functional capacity of older adults: findings from the retirement community back pain study. Arthritis Rheum 59(9):1306–1313
Genevay S, Atlas SJ (2010) Lumbar spinal stenosis. Best Pract Res Clin Rheumatol 24(2):253–265
Kovacs FM, Urrútia G, Alarcón JD (2011) Surgery versus conservative treatment for symptomatic lumbar spinal stenosis: a systematic review of randomized controlled trials. Spine 36(20):E1335–E1351
Long William D, Whang Peter G (2011) Interspinous spacers for lumbar spinal stenosis. Oper Tech Orthop 21(3):208–212
Burnett MG, Stein SC, Bartels RH (2010) Cost-effectiveness of current treatment strategies for lumbar spinal stenosis: nonsurgical care, laminectomy, and X-STOP. J Neurosurg Spine 13(1):39–46
Boonstra AM, Schiphorst Preuper HR, Reneman MF, Posthumus JB, Stewart RE (2008) Reliability and validity of the visual analogue scale for disability in patients with chronic musculoskeletal pain. Int J Rehabil Res 31(2):165–169
Price DD, McGrath PA, Rafii A, Buckingham B (1983) The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain 17(1):45–56
Smeets R, Köke A, Lin CW, Ferreira M, Demoulin C (2011) Measures of function in low back pain/disorders: low back pain rating scale (LBPRS), oswestry disability index (ODI), progressive isoinertial lifting evaluation (PILE), quebec back pain disability scale (QBPDS), and Roland-Morris disability questionnaire (RDQ). Arthritis Care Res (Hoboken) 63(suppl 11):S158–S173
Kim DH, Albert TJ (2007) Interspinous process spacers. J Am Acad Orthop Surg 15:200–207
Sénégas J, Vital JM, Guérin J, Bernard P, M’Barek M, Loreiro M, Bouvet R (1995) Stabilisation lombaire souple. GIEDA—Instabilités vertébrales lombaires. Expansion Scientifique Française, Paris, pp 122–132
Bono CM, Vaccaro AR (2007) Interspinous process devices in the lumbar spine. J Spinal Disord Tech 20:255–261
Senegas J (2002) Mechanical supplementation by non-rigid fixation in degenerative intervertebral lumbar segments: the Wallis system. Eur Spine J 11(2):164–169
Wildermuth S, Zanetti M, Duewell S et al (1998) Lumbar spine: quantitative and qualitative assessment of positional (upright flexion and extension) MR imaging and myelography. Radiology 207:391–398
Anjarwalla NK, Brown LC, McGregor AH (2007) The outcome of spinal decompression surgery 5 years on. Eur Spine J 16:1842–1847
Atlas SJ, Keller RB, Wu YA et al (2005) Long-term outcomes of surgical and nonsurgical management of lumbar spinal stenosis: 8 to 10 year results from the maine lumbar spine study. Spine 30:936–943
Mardjetko SM, Connolly PJ, Shott S (1994) Degenerative lumbar spondylolisthesis. A meta-analysis of literature 1970–1993. Spine 19:2256S–2265S
Gibson JN, Waddell G (2005) Surgery for degenerative lumbar spondylosis: updated Cochrane review. Spine 30:2312–2320
Wurgler-Hauri CC, Kalbarczyk A, Wiesli M et al (2008) Dynamic neutralization of the lumbar spine after microsurgical decompression in acquired lumbar spinal stenosis and segmental instability. Spine 33:66–72
Smorgick Y, Park DK, Baker KC, Lurie JD, Tosteson TD, Zhao W, Herkowitz HN, Fischgrund JS, Weinstein JN (2013) Single- versus multilevel fusion for single-level degenerative spondylolisthesis and multilevel lumbar stenosis: four-year results of the spine patient outcomes research trial. Spine (Phila Pa 1976) 38(10):797–805
Conflict of interest
No funds were received in support of this study. No benefits in any form have been received from a commercial party related directly or indirectly to the subject of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Marsh, G.D.J., Mahir, S. & Leyte, A. A prospective randomised controlled trial to assess the efficacy of dynamic stabilisation of the lumbar spine with the Wallis ligament. Eur Spine J 23, 2156–2160 (2014). https://doi.org/10.1007/s00586-014-3487-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3487-4