Abstract
Objectives
The aim of this study was to systematically describe the nature and context of subjective sexual well-being and sexual behavior in young women with breast cancer.
Methods
Data on sexual behavior and subjective sexual well-being were collected through an internet questionnaire. Respondents were included if they had been diagnosed with breast cancer within the past 6 years and were currently 45 years of age or younger. Results were compared with a representative sample of the general Dutch population.
Results
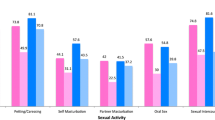
In comparison with the general Dutch population of women, young women still undergoing breast cancer treatment are less sexually active and have a more negative experience of sexuality. While women who had already finished their treatment had more or less the same amount of sexual activity as the general Dutch population, there were still major differences in their experience of sexuality. Particularly strong associations were found between these women’s sexual well-being in relation to their relationship satisfaction, and sexual interaction competence.
Conclusion
In the wake of breast cancer treatment, young women have difficulty enjoying sex; it is evidently hard for them to resume their sex lives after breast cancer. In particular, women who find it hard to discuss sexual wishes and the possibilities and impossibilities associated with breast cancer with their partner experience negative consequences when trying to resume their sex lives.
Similar content being viewed by others
References
Dutch Association of Comprehensive Cancer Centers (2010) Borstkanker in Nederland, cijfers uit de kankerregistratie [Breast Cancer in the Netherlands, data from the cancer registry]. Vereniging Integrale Kankercentra, Utrecht
Dutch Scientific Network Comprehensive Cancer Centers (2011). Available from URL: http://www.iknl.nl/cijfers Accessed on April 24, 2011
Graf MC, Geller PA (2003) Treating hot flashes in breast cancer survivors: a review of alternative treatments to hormone replacement therapy. Clin J Oncol Nurs 7:637–640
Massie MJ (2004) Prevalence of depression in patients with cancer. J Natl Cancer 32:57–71
Burwell SR, Case LD, Kaelin C, Avis NE (2006) Sexual problems in younger women after breast cancer surgery. J Clin Oncol 24:2815–2821
Hopwood P, Haviland J, Mills J, Sumo G (2007) The impact of age and clinical factors on quality of life in early breast cancer: an analysis of 2208 women recruited to the UK START Trial (Standardisation of Breast Radiotherapy Trial). Breast 16:241–251
Kedde H, Van de Wiel HBM, Weijmar Schultz WCM, Wijsen C (2012) Sexual dysfunction in young women with breast cancer. Support Care Cancer 21:271–280
Alder J, Zanetti R, Wight E et al (2008) Sexual dysfunction after premenopausal stage I and II breast cancer: do androgens play a role? J Sex Med 5:1898–1906
Eeltink C, Hahn D (eds) (2009) 80 vragen over kanker en seksualiteit [80 questions about cancer and sexuality]. Academic Pharmaceutical Productions, Utrecht
Fobair P, Stewart S, Chang S, D’Onofrio C, Banks P, Bloom S (2006) Body image and sexual problems in young women with breast cancer. Psychooncol 5:579–594
Henson H (2002) Breast cancer and sexuality. Sex Disabil 20:261–275
Derogatis LR (1980) Breast and gynaecological cancers: their unique body image and sexual identity in women. Front Radiat Ther On 14:1–11
Schain WS, Wellisch DK, Pasnau RO, Landsverk J (1985) The sooner the better: a study of psychological factors in women undergoing immediate versus delayed reconstruction of the breast. Am J Psychiat 142:40–46
Bakewell RT, Volker DL (2005) Sexual dysfunction related to the treatment of young women with breast cancer. Clin J Oncol Nurs 9:697–702
Kunkel E, Chen E (2003) Psychiatric aspects of women with breast cancer. Psychiat Clin N Am 26:713–724
Wilmoth MC, Coleman EA, Smith SC, Davis C (2004) Fatigue, weight gain, and altered sexuality in patients with breast cancer: exploration of a symptom cluster. Oncol Nurs Forum 31:1069–1075
Ghizzani A, Pirtoli L, Bellezza A, Velicogna F (1995) The evaluation of some factors influencing the sexual life of women affected by breast cancer. J Sex Marital Ther 21:57–63
Van Lankveld J, Laan E (2009) Wetenschappelijk onderzoek naar seksualiteit [Scientific research on sexuality]. In: Gijs L, Gianotten W, Vanwesenbeeck I, Weijenborg P (eds) Seksuologie [Sexology]. Bohn Stafleu van Loghum, Houten, pp 45–67
Pool G, Van de Wiel HBM, Jaspers JPC, Weijmar Schultz WCM, Van Driel MF (2008) Kanker [Cancer]. In: Gianotten WL, Meihuizen-de Regt MJ, Van Son-Schoones N (eds) Seksualiteit bij ziekte en lichamelijke beperking [Sexuality with disease and physical disability]. Van Gorcum, Assen, pp 325–339
Enzlin P (2008) Seksualiteit, een plaatsbepaling [Sexuality, orientation and definition]. In: Gianotten WL, Meihuizen-de Regt MJ, Van Son-Schoones N (eds) Seksualiteit bij ziekte en lichamelijke beperking [Sexuality with disease and physical disability]. Van Gorcum, Assen, pp 16–20
Oberg K, Fugl-Meyer KS, Fugl-Meyer AR (2002) On sexual well-being in sexually abused Swedish women: epidemiological aspects. Sex Relat Ther 17:329–341
Laumann EO, Paik A, Glasser DB et al (2006) A cross-national study of subjective sexual well-being among older women and men: findings from the global study of sexual attitudes and behaviors. Arch Sex Behav 35:145–161
Ofman U, Kingsberg SA, Nelson CJ (2008) Sexual problems and cancer. In: DeVita VT, Hellman S, Rosenberg SA (eds) Cancer: principles and practice of oncology. Lippincott Williams & Wilkins, Philadelphia, PA, pp 2804–2815
Panjari M, Bell R, Davis S (2011) Sexual function after breast cancer. J Sex Med 8:294–302
Malinovszky KM, Gould A, Foster E et al (2006) Quality of life and sexual function after high-dose or conventional chemotherapy for high-risk breast cancer. Br J Cancer 95:1626–1631
Markopoulos C, Tsaroucha AK, Kouskos E et al (2009) Impact of breast cancer surgery on the self-esteem and sexual life of female patients. J Int Med Res 37:182–188
Evers AWM, Kraaimaat FW, Van Lankveld W, Jongen PJH, Jacobs JWG, Bijlsma JWJ (1998) Beyond unfavorable thinking: the illness cognition questionnaire for chronic diseases. J Consult Clin Psych 69:1026–1036
Hagger MS, Orbell S (2003) A meta-analytic review of the common-sense model of illness representations. Psychol Heal 18:141–184
Leventhal H, Nerenz DR, Steele DS (1984) Illness representations and coping with health threats. In: Baum A, Singer J (eds) A handbook of psychology and health. Erlbaum, Hillsdale, pp 219–252
Weinman J, Petrie KJ, Moss-Morri R, Horne R (1996) The Illness perception questionnaire: a new method for assessing illness perceptions. Psychol Health 11:431–446
Heijmans MJWM (1998) Cognitive representations of chronic disease: an empirical study among patients with chronic fatigue syndrome and Addison’s disease. Universiteit Utrecht, Utrecht
Burman B, Margolin G (1992) Analysis of the association between marital relationships and health problems: an interactional perspective. Psychol Bull 112:39–63
Gottman JM (1993) A theory of marital dissolution and stability. J Fam Psychol 7:57–75
Horwitz AV, McLaughlin J, White HR (1998) How the negative and positive aspects of partner relationships affect the mental health of young married people. J Health Soc Behav 39:124–136
De Graaf H, Höing M, Zaagsma M, Vanwesenbeeck I (2007) Tienerseks: vormen van instrumentele seks onder tieners [Teenage sex: variations in instrumental sex among teenagers]. Rutgers Nisso Groep, Utrecht
Savelkoul M (2012) Sociale steun samengevat [Social support summarized]. Available from URL: http://www.nationaalkompas.nl/gezondheidsdeterminanten/omgeving/leefomgeving/sociale-steun/sociale-steun-samengevat. Accessed on March 9, 2012
Garssen B (2004) Psychological factors and cancer development: evidence after 30 years of research. Clin Psychol Rev 24:315–338
Edelman S (2005) Relationship between psychological factors and cancer: an update of the evidence. Clin Psychol 9:45–53
Chida Y, Hamer M, Wardle J, Steptoe A (2008) Do stress-related psychosocial factors contribute to cancer incidence and survival? Nat Rev Clin Oncol 5:466–475
Pinquart M, Duberstein PR (2010) Associations of social networks with cancer mortality: a meta-analysis. Crit Rev Oncol Hemat 75:122–137
Nausheen B, Gidron Y, Peveler R, Moss-Morris R (2009) Social support and cancer progression: a systematic review. J Psychosom Res 67:403–415
Salonen P, Tarkka MT, Kellokumpu-Lehtinen PL et al (2012) Effect of social support on changes in quality of life in early breast cancer patients: a longitudinal study. Scand J Caring Sci. doi:10.1111/j.1471-6712.2012.01050.x, Advance online publication
Vroege JA (1994) Vragenlijst voor het signaleren van seksuele dysfuncties (VSD). 5de versie [Questionnaire on screening for sexual dysfunctions (QSD). 5th version]. Academisch Ziekenhuis Utrecht, Afdeling Medische seksuologie/Nederlands Instituut voor Sociaal Sexuologisch Onderzoek: Utrecht
Taleporos G, McCabe M (2002) Development and validation of the physical disability sexual and body esteem scale. Sex Disabil 20:159–176
Vanwesenbeeck I, Bakker F, Gesell S (2010) Sexual health in the Netherlands. Main results of a population survey among Dutch adults. Int J Sex Health 22:55–71
Lawrance K, Byers ES (1998) Interpersonal exchange model of sexual satisfaction questionnaire. In: Davis CM, Yarber WL, Bauserman R, Schreer G, Davis L (eds) Sexuality-related measures: a compendium, 2nd edn. Sage, Thousand Oaks, CA, pp 514–519
Janda LH, O’Grady KE (1980) Development of a sex anxiety inventory. J Consult Clin Psych 48:169–175
Fisher WA, Byrne D, White LA (1983) Emotional Barriers to contraception. In: Byrne D, Fisher WA (eds) Adolescents, sex and contraception. Lawrence Erlbaum Associates, Hillsdale, NJ, pp 207–239
Bancroft J, Loftus J, Scott Long J (2003) Distress about sex: a national survey of women in heterosexual relationships. Arch Sex Behav 32:193–208
Ware JE, Kosinski MA (2001) SF-36: Physical and mental health summary scales. A manual for users of Version 1, 2nd edn. Quality Metric Inc, Lincoln, RI
Arrindell W, Schaap C (1985) The Maudsley marital questionnaire (MMQ): an extension of its construct validity. Br J Psychiat 147:295–299
Cohen J (1992) A power primer. Psychol Bull 112:155–159
McLean C, Campbell C (2003) Locating research informants in a multi-ethnic community: ethnic identities, social networks and recruitment methods. Ethn Health 8:41–61
Berglund G, Bolund C, Gustafsson U, Sjoden P (1997) Is the wish to participate in a cancer rehabilitation program an indicator of the need? Comparisons of participants and non-participants in a randomized study. Psychooncology 6:46
Acknowledgement
This study was financed by the Dutch Ministry of Public Health, Welfare, and Sports. This study was commissioned by the Dutch Breast Cancer Association (BVN) and the Amazon Foundation — an organisation specifically aimed at young women with breast cancer. This study did not require the approval of an institutional review board.
Conflict of interest
Rutgers WPF and the University of Groningen, University Medical Center Groningen do not a have a financial relationship with the organizations that sponsored this research. Rutgers WPF is in full control of all primary data, which can be reviewed by the Journal of Supportive Care in Cancer if requested. The authors certify that they have no commercial associations that may pose a conflict of interests in connection with the submitted article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kedde, H., van de Wiel, H.B.M., Weijmar Schultz, W.C.M. et al. Subjective sexual well-being and sexual behavior in young women with breast cancer. Support Care Cancer 21, 1993–2005 (2013). https://doi.org/10.1007/s00520-013-1750-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-013-1750-6