Abstract
Background
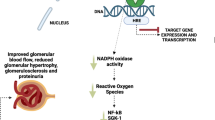
Alport syndrome (AS) is a progressive hereditary glomerular disease. Recent data indicate that aldosterone promotes fibrosis mediated by the transforming growth factor-β1 (TGF-β1) pathway, which may worsen proteinuria. Spironolactone (SP) antagonizes aldosterone and this study aimed to evaluate the efficacy of SP in reducing proteinuria and urinary TGF-β1 excretion in proteinuric AS patients.
Methods
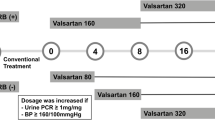
The study involved ten children with AS, normal renal function, and persistent proteinuria (>6 months; uPr/uCr ratio >1). SP 25 mg once a day for 6 months was added to existing ACE inhibitor treatment with or without angiotensin-II receptor blockade. Urine and blood samples were examined monthly. Urinary TGF-β1 levels were measured twice before and three times during SP treatment. Plasma renin activity (PRA) and serum aldosterone levels were also measured. In eight patients, uProt/uCreat was also assessed after 9 months and 12 months of SP treatment.
Results
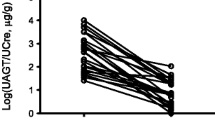
After beginning SP therapy, all patients showed significant decrease in mean uProt/uCreat ratio (1.77 ± 0.8 to 0.86 ± 0.6; p < 0.001) and mean urinary TGF-β1 levels (104 ± 54 to 41 ± 20 pg/mgCreatinine; p < 0.01), beginning after 30 days of treatment and remaining stable throughout SP administration. PRA remain unchanged, and mean serum aldosterone increased from 105 ± 72 pg/ml to 303 ± 156 pg/ml (p < 0.001). The only side effect was gynecomastia in an obese boy. After 1 year of therapy, mean uProt/uCreat remains low (0.82 ± 0.48).
Conclusions
Addition of SP to ACE-I treatment with or without angiotensin II receptor blokers (ARB) significantly reduced proteinuria. This was mediated by decreased urinary TGF-β1 levels and not associated with major side effects.






Similar content being viewed by others
References
Barker DF, Hostikka SL, Zhou J, Chow LT, Oliphant AR, Gerken SC, Gregory MC, Skolnick MH, Atkin CL, Tryggvason K (1990) Identification of mutations in the COL4A5 collagen gene in Alport syndrome. Science 248:1224–1227
Gubler MC, Knebelmann B, Beziau A, Broyer M, Pirson Y, Haddoum F, Kleppel MM, Antignac C (1995) Autosomal recessive Alport syndrome: immunohistochemical study of type IV collagen chain distribution. Kidney Int 47:38–44
Guney I, Selcuk YN, Altintepe L, Atalay H, Başarali KM, Büyükbaş S (2009) Antifibrotic effects of aldosterone receptor blocker (Spironolactone) in patients with chronic kidney disease. Ren Fail 31:779–784
Lai L, Chen J, Hao CM, Lin S, Gu Y (2006) Aldosterone promotes fibronectin production through a Smad2-dependent TGF-β1 pathway in mesangial cells. Biochem Biophys Res Commun 348:70–75
Goumenos DS, Tsakas S, El Nahas AM, Alexandri S, Oldroyd S, Kalliakmani P, Vlachojannis JG (2002) Transforming growth factor-β1 in the kidney and urine of patients with glomerular disease and proteinuria. Nephrol Dial Transplant 17:2145–2152
Jais JP, Knebelmann B, Giartis I, De Marchi M, Rizzoni G, Renieri A, Weber M, Gross O, Netzer KO, Flinter F, Pirson Y, Dahan K, Wieslander J, Persson U, Tryggvason K, Martin P, Hertz JM, Schröder C, Sanak M, Carvalho MF, Saus J, Antignac C, Smeets H, Gubler MC (2003) X-linked Alport syndrome: natural history and genotype-phenotype correlations in girls and women belonging to 195 families: a “European Community Alport Syndrome Concerted Action” study. J Am Soc Nephrol 14:2603–2610
Gross O, Kashtan CE (2009) Treatment of Alport syndrome: beyond animal models. Kidney Int 76:599–603
Chen D, Jefferson B, Harvey SJ, Gartley CJ, Jacobs RM, Thorner PS (2003) Cyclosporine A slows the progressive renal disease of Alport syndrome (X-linked Hereditary Nephritis): results from a canine model. J Am Soc Nephrol 14:690–698
Massella L, Onetti Muda A, Legato A, Di Zazzo G, Giannakakis K, Emma F (2010) Cyclosporine A treatment in patients with Alport syndrome: a single-center experience. Pediatr Nephrol 25:1269–1275
Charbit M, Gubler MC, Dechaux M, Gagnadoux MF, Grünfeld JP, Niaudet P (2007) Cyclosporine therapy in patients with Alport syndrome. Pediatr Nephrol 22:57–63
Proesmans W, Van Dyck M (2004) Enalapril in children with Alport syndrome. Pediatr Nephrol 19:271–275
Webb NJ, Lam C, Shahinfar S (2011) Efficacy and safety of losartan in children with Alport syndrome – results from a subgroup analysis of prospective, randomized, placebo- or amlodipine-controlled trial. Nephrol Dial Transplant 26:2521–2526
Gross O, Licht C, Anders HJ (2012) Early angiotensin-converting enzyme inhibition in Alport syndrome delays renal failure and improves life expectancy. Kidney Int 81:494–501
Nakao N, Yoshimura A (2003) Combination treatment of angiotensin II receptor blocker and angiotensin-converting-enzyme inhibitor in non diabetic renal disease. Lancet 361:117–124
Furumatsu Y, Nagasawa Y, Tomida K, Mikami S, Kaneko T, Okada N, Tsubakihara Y, Imai E, Shoji T (2008) Effect of Renin-Angiotensin-Aldosterone system triple blockade on non-diabetic renal disease: addition of aldosterone blocker, Spironolactone, to combination treatment with an angiotensin-converting enzyme inhibitor and angiotensin II receptor blocker. Hypertens Res 31:59–67
González Monte E, Andrés A, Polanco N, Toribio ML, Santana R, Gutiérrez Martínez E, González J, Ramírez E, Hernández A, Morales E, Praga M, Morales JM (2010) Addition of spironolactone to dual blockade of renina angiotensin system dramatically reduces severe proteinuria in renal transplant patients: an uncontrolled pilot study at 6 months. Transplant Proc 42:2899–2901
Kaito H, Nozu K, Iijima K, Nakanishi K, Yoshiya K, Kanada K, Przybyslaw Krol R, Yoshikawa N, Matsuo M (2006) The effect of aldosterone blockade in patients with Alport syndrome. Pediatr Nephrol 21:1824–1829
Kashtan CE, Ding J, Gregory M, Gross O, Heidet L, Knebelmann B, Rheault M, Licht C (2013) Clinical practice recommendations for the treatment of Alport syndrome: a statement of the Alport Syndrome Research Collaborative. Pediatr Nephrol 28:5–11
Schwartz GJ, Brion LP, Spitzer A (1987) The use of plasma creatinine concentration for estimating glomerular filtration rate in infants, children, and adolescents. Pediatr Clin North Am 34:571–590
Bianchi S, Bigazzi R, Campese VM (2006) Long-term effects of spironolactone on proteinuria and kidney function in patients with chronic kidney disease. Kidney Int 70:2116–2123
Park HC, Xu ZG, Choi S, Goo YS, Kang SW, Choi KH, Ha SK, Lee HY, Han DS (2003) Effect of losartan and amlodipine on proteinuria and transforming growth factor-β1 in patients with IgA nephropathy. Nephrol Dial Transplant 18:1115–1121
Struthers AD (1995) Aldosterone escape during ACE inhibitor therapy in chronic heart failure. Eur Heart J 16:103–106
Nishiyama A, Abe Y (2006) Molecular mechanisms and therapeutic strategies of chronic renal injury: renoprotective effects of aldosterone blockade. J Pharmacol Sci 100:9–16
Tsakas S, Goumenos DS (2006) Accurate measurement and clinical significance of urinary transforming growth factor-beta1. Am J Nephrol 26:186–193
Cheon Park H, Gao Xu Z, Choi S, Young SG, Wook Kang S, Hun Choi K, Kyu Ha S, Lee Y, Suk Han D (2003) Effect of losartan and amlodipine on proteinuria and transforming growth factor-β1 in patients with IgA nephropathy. Nephrol Dial Transplant 18:1115–1121
Sayers R, Kalluri R, Rogers KD, Shiel CF, Meehan DT, Cosgrove D (1999) Role for transforming growth factor-beta1 in Alport renal disease progression. Kidney Int 56:1662–1673
Cosgrove D, Rodgers K, Meehan D, Miller C, Bovard K, Gilroy A, Gardner H, Kotelianski V, Gotwals P, Amatucci A, Kalluri R (2000) Integrin alpha1beta1 and transforming growth factor-beta1 play distinct roles in Alport glomerular pathogenesis and serve as dual targets for metabolic therapy. Am J Pathol 157:1649–1659
Adler L, Mathew R, Futterweit S, Frank R, Gauthier BG, Kashtan CE, Trachtman H (2002) Angiotensin converting enzyme inhibitor therapy in children with Alport syndrome: effect on urinary albumin, TGF-β, and nitrite excretion. BMC Nephrol 3:2–7
Bobadilla NA, Gamba G (2007) New insights into the pathophysiology of cyclosporine nephrotoxicity: a role of aldosterone. Am J Physiol Renal Physiol 293:F2–F9
Cosgrove D (2012) Glomerular pathology in Alport syndrome: a molecular prospective. Pediatr Nephrol 27:885–890
Acknowledgments
We thank Prof. A. Renieri and F Mari (Genetica Medica, Università di Siena) for the genetic analysis.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Giani, M., Mastrangelo, A., Villa, R. et al. Alport syndrome: the effects of spironolactone on proteinuria and urinary TGF-β1. Pediatr Nephrol 28, 1837–1842 (2013). https://doi.org/10.1007/s00467-013-2490-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-013-2490-z