Abstract
Purpose
To investigate the effectiveness and clinical significance of thoracolaparoscopic esophagectomy with mesoesophagus excision.
Materials and methods
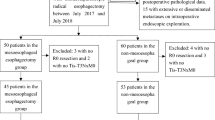
Patients who underwent en bloc mesoesophageal esophagectomy through thoracoscopy combined with laparoscopy were retrospectively enrolled. Carbon nanoparticles were used in some patients to label the esophageal drainage lymph nodes. The clinical data were analyzed.
Results
En bloc mesoesophageal esophagectomy was successfully performed in 135 patients (100%). The carbon nanoparticles were used in 10 patients, among which the left gastric arterial lymph nodes were labeled in all patients and excised together with the left gastric mesentery, mesoesophagus, esophageal cancer, lymph nodes, vessels, nerves, and adipose tissues as one intact package. The mean operation time was 182.5 ± 26.4 min, intraoperative blood loss 45.9 ± 17.6 ml, mean number of lymph nodes dissected 20.9 ± 8.12, extubation time of drainage tubes 7.5 ± 3.8 days, first oral feeding time 7.5 ± 1.8 days, and postoperative hospital stay 13 ± 5.11 days. Postoperatively, anastomotic leakage occurred in six patients (4.4%), anastomotic stenosis in eight (5.9%), hoarseness in seven (5.2%), and inflammation of the remnant stomach in four (3.0%), with a complication rate of 18.5%. Patients were followed up for 13–34 months (median 23). Eighteen patients presented with organ metastasis. No local recurrence or death during follow-up.
Conclusion
Based on the membrane anatomy or mesoesophagus theory, thoracolaparoscopic en bloc mesoesophageal esophagectomy is safe, with decreased blood loss, and it is necessary to resect the left gastric artery lymph nodes together with the left gastric mesentery and its contents to completely remove the cancer.




Similar content being viewed by others
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61:69–90
Mao WM, Zheng WH, Ling ZQ (2011) Epidemiologic risk factors for esophageal cancer development. Asian Pac J Cancer Prev 12:2461–2466
Izon AS, Jose P, Hayden JD, Grabsch HI (2013) Significant variation of resected meso-esophageal tissue volume in two-stage subtotal esophagectomy specimens: a retrospective morphometric study. Ann Surg Oncol 20:788–797
Birkmeyer JD, Siewers AE, Finlayson EV, Stukel TA, Lucas FL, Batista I, Welch HG, Wennberg DE (2002) Hospital volume and surgical mortality in the United States. N Engl J Med 346:1128–1137
D’Amico TA (2011) Improving outcomes after esophagectomy: the importance of preventing postoperative pneumonia. Zhonghua Wei Chang Wai Ke Za Zhi 14:660–666
Guo W, Ma X, Yang S, Zhu X, Qin W, Xiang J, Lerut T, Li H (2016) Combined thoracoscopic-laparoscopic esophagectomy versus open esophagectomy: a meta-analysis of outcomes. Surg Endosc 30:3873–3881
Maas KW, Biere SS, Scheepers JJ, Gisbertz SS, van-der-Peet DL, Cuesta MA (2012) Laparoscopic versus open transhiatal esophagectomy for distal and junction cancer. Rev Esp Enferm Dig 104:197–202
Cuesta MA, Weijs TJ, Bleys RL, van Hillegersberg R, van Berge Henegouwen MI, Gisbertz SS, Ruurda JP, Straatman J, Osugi H, van der Peet DL (2015) A new concept of the anatomy of the thoracic oesophagus: the meso-oesophagus. Observational study during thoracoscopic esophagectomy. Surg Endosc 29:2576–2582
Merritt RE, Kneuertz PJ, D’Souza DM, Perry KA (2019) Total laparoscopic and thoracoscopic Ivor Lewis esophagectomy after neoadjuvant chemoradiation with minimal overall and anastomotic complications. J Cardiothorac Surg 14:123
Murakami M, Otsuka K, Goto S, Ariyoshi T, Yamashita T, Aoki T (2017) Thoracoscopic and hand assisted laparoscopic esophagectomy with radical lymph node dissection for esophageal squamous cell carcinoma in the left lateral decubitus position: a single center retrospective analysis of 654 patients. BMC Cancer 17:748
Wan J, Che Y, Kang N, Zhang R (2016) Surgical method, postoperative complications, and gastrointestinal motility of thoraco-laparoscopy 3-field esophagectomy in treatment of esophageal cancer. Med Sci Monit 22:2056–2065
Heald RJ (1995) Total mesorectal excision is optimal surgery for rectal cancer: a Scandinavian consensus. Br J Surg 82:1297–1299
Heald RJ, Ryall RD (1986) Recurrence and survival after total mesorectal excision for rectal cancer. Lancet 1:1479–1482
Hohenberger W, Weber K, Matzel K, Papadopoulos T, Merkel S (2009) Standardized surgery for colonic cancer: complete mesocolic excision and central ligation–technical notes and outcome. Colorectal Dis 11:354–364 (discussion 364–355)
Tachimori Y (2014) Total mesoesophageal esophagectomy. Chin Med J (Engl) 127:574–579
Cuesta MA (2019) Minimally invasive mesoesophageal resection. J Thorac Dis 11:S728–S734
Hwang SE, Kim JH, Bae SI, Rodriguez-Vazquez JF, Murakami G, Cho BH (2014) Mesoesophagus and other fascial structures of the abdominal and lower thoracic esophagus: a histological study using human embryos and fetuses. Anat Cell Biol 47:227–235
Weijs TJ, Goense L, van Rossum PSN, Meijer GJ, van Lier AL, Wessels FJ, Braat MN, Lips IM, Ruurda JP, Cuesta MA, van Hillegersberg R, Bleys RL (2017) The peri-esophageal connective tissue layers and related compartments: visualization by histology and magnetic resonance imaging. J Anat 230:262–271
Rizzetto C, DeMeester SR, Hagen JA, Peyre CG, Lipham JC, DeMeester TR (2008) En bloc esophagectomy reduces local recurrence and improves survival compared with transhiatal resection after neoadjuvant therapy for esophageal adenocarcinoma. J Thorac Cardiovasc Surg 135:1228–1236
Escrig Sos J, Gomez Quiles L, Maiocchi K (2019) The 8th edition of the AJCC-TNM classification: new contributions to the staging of esophagogastric junction cancer. Cir Esp 97:432–437
Luketich JD, Pennathur A, Awais O, Levy RM, Keeley S, Shende M, Christie NA, Weksler B, Landreneau RJ, Abbas G, Schuchert MJ, Nason KS (2012) Outcomes after minimally invasive esophagectomy: review of over 1000 patients. Ann Surg 256:95–103
van Workum F, Berkelmans GH, Klarenbeek BR, Nieuwenhuijzen GAP, Luyer MDP, Rosman C (2017) McKeown or Ivor Lewis totally minimally invasive esophagectomy for cancer of the esophagus and gastroesophageal junction: systematic review and meta-analysis. J Thorac Dis 9:S826–S833
Akhtar NM, Chen D, Zhao Y, Dane D, Xue Y, Wang W, Zhang J, Sang Y, Chen C, Chen Y (2020) Postoperative short-term outcomes of minimally invasive versus open esophagectomy for patients with esophageal cancer: an updated systematic review and meta-analysis. Thorac Cancer 11:1465–1475
Yamashita K, Watanabe M, Mine S, Toihata T, Fukudome I, Okamura A, Yuda M, Hayami M, Ishizuka N, Imamura Y (2018) Minimally invasive esophagectomy attenuates the postoperative inflammatory response and improves survival compared with open esophagectomy in patients with esophageal cancer: a propensity score matched analysis. Surg Endosc 32:4443–4450
Gong J (2015) D2 gastrectomy and complete mesentery excision based on metastasis IIIII( and membrane anatomy. Zhonghua Wei Chang Wai Ke Za Zhi 18:121–122
Gong JP (2013) The fifth metastasis route of gastric cancer and the third principle of radical operation. Zhonghua Wei Chang Wai Ke Za Zhi 16:109–110
Chai N, Du C, Gao Y, Niu X, Zhai Y, Linghu E, Liu Y, Yang B, Lu Z, Li Z, Wang X, Tang P (2018) Comparison between submucosal tunneling endoscopic resection and video-assisted thoracoscopic enucleation for esophageal submucosal tumors originating from the muscularis propria layer: a randomized controlled trial. Surg Endosc 32:3364–3372
Peng W, Tan S, Huang S, Ren Y, Li H, Peng Y, Fu X, Tang X (2019) Efficacy and safety of submucosal tunneling endoscopic resection for upper gastrointestinal submucosal tumors with more than 1-year’ follow-up: a systematic review and meta-analysis. Scand J Gastroenterol 54:397–406
Wadhwa V, Franco FX, Erim T (2020) Submucosal tunneling endoscopic resection. Surg Clin North Am 100:1201–1214
Zhang M, Wu S, Xu H (2019) Comparison between submucosal tunneling endoscopic resection (STER) and other resection modules for esophageal muscularis propria tumors: a retrospective study. Med Sci Monit 25:4560–4568
Liu CL, Yang TL, Chen BF (2003) Sentinel lymph node mapping with emulsion of activated carbon particles in patients with pre-mastectomy diagnosis of intraductal carcinoma of the breast. J Chin Med Assoc 66:406–410
Wang LY, Li JH, Zhou X, Zheng QC, Cheng X (2017) Clinical application of carbon nanoparticles in curative resection for colorectal carcinoma. Onco Targets Ther 10:5585–5589
Wang Q, Chen E, Cai Y, Chen C, Jin W, Zheng Z, Jin Y, Chen Y, Zhang X, Li Q (2016) Preoperative endoscopic localization of colorectal cancer and tracing lymph nodes by using carbon nanoparticles in laparoscopy. World J Surg Oncol 14:231
Huang K, Luo D, Huang M, Long M, Peng X, Li H (2013) Protection of parathyroid function using carbon nanoparticles during thyroid surgery. Otolaryngol Head Neck Surg 149:845–850
Jiang Y, Lin N, Huang S, Lin C, Jin N, Zhang Z, Ke J, Yu Y, Zhu J, Wang Y (2015) Tracking nonpalpable breast cancer for breast-conserving surgery with carbon nanoparticles: implication in tumor location and lymph node dissection. Medicine (Baltimore) 94:e605
Liu BR, Ahmed MR, He D, Zhao L, Yang W, Zhang X, Shi Y, Zhou Y, Zhang D, Chen Y, Cao Z, He D, Yuan Y, Li D (2019) Endoscopic mediastinal lymph node identification and resection using carbon nanoparticles in a porcine model. Gastroenterology 156(1250–1252):e1251
Yan J, Xue F, Chen H, Wu X, Zhang H, Chen G, Lu J, Cai L, Xiang G, Deng Z, Zheng Y, Zheng X, Li G (2014) A multi-center study of using carbon nanoparticles to track lymph node metastasis in T1–2 colorectal cancer. Surg Endosc 28:3315–3321
Funding
This study was supported by the Key Research, Development, and Promotion Projects of Henan Province in 2020 (202102310117) and Key Scientific Research Projects of Colleges and Universities in Henan Province 20B320029.
Author information
Authors and Affiliations
Contributions
Study concept and design: G-JW and B-LG. Acquisition of data: X-MD, T-YZ, R-XL, and Y-FZ. Analysis and interpretation of data: X-MD, G-JW, and B-LG. Drafting of the manuscript: T-YZ and X-MD. Critical revision of the manuscript for important intellectual content: B-LG. Statistical analysis: None. Obtained funding: G-J W. Technical or material support: G-JW. Study supervision: Y-FZ.
Corresponding author
Ethics declarations
Disclosures
Tian-Yu Zhu, Xiu-Mei Deng, Guo-Jun Wang, Bu-Lang Gao, Rui-Xin Li, Yun-Fei Zhang, and Jing-Tao Wang have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhu, TY., Deng, XM., Wang, GJ. et al. En bloc mesoesophageal esophagectomy through thoracoscopy combined with laparoscopy based on the mesoesophageal theory. Surg Endosc 36, 5784–5793 (2022). https://doi.org/10.1007/s00464-022-09175-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09175-0