Abstract
Background
Placement of self-expanding metal stents has been increasingly adopted as a bridge to surgery in patients presenting with obstructed left-sided colorectal cancers. The optimal bridging time has yet to be widely established, hence this retrospective study aims to determine the optimal bridging time to elective surgery post endoluminal stenting.
Patients and methods
All patients who underwent colorectal stenting for large bowel obstruction in a single, tertiary hospital in Singapore between January 2003 and December 2017 were retrospectively identified. Patients’ baseline demographics, tumour characteristics, stent-related complications, intra-operative details, post-operative complications and oncological outcomes were analysed.
Results
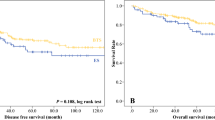
Of the 53 patients who successfully underwent colonic stenting for malignant left sided obstruction, 33.96% of patients underwent surgery within two weeks of stent placement while 66.04% of patients underwent surgery after 2 weeks of stent placement. Univariate analysis between both groups did not demonstrate significant differences in postoperative complications and stoma formation. Significant differences were observed between both groups for stent complications (38.89% vs 8.57%, p = 0.022), on-table decompression (38.89% vs 2.86%, p = 0.001) and systemic recurrence (11.11% vs 40.00%, p = 0.030). Increased bridging interval to surgery (OR 13.16, CI 1.37–126.96, p = 0.026) was a significant risk factor for systemic recurrence on multivariate analysis.
Conclusions
Patients undergoing definitive surgery within 2 weeks of colonic stenting may have better oncological outcomes without compromising on postoperative outcomes. Further prospective studies are required to compare outcomes between emergency surgery and different bridging intervals.



Similar content being viewed by others
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68:394–424
Keum N, Giovannucci E (2019) Global burden of colorectal cancer: emerging trends, risk factors and prevention strategies. Nat Rev GastroenterolHepatol 16:713–732
Deans GT, Krukowski ZH, Irwin ST (1994) Malignant obstruction of the left colon. Br J Surg 81:1270–1276
McArdle CS, Hole DJ (2004) Emergency presentation of colorectal cancer is associated with poor 5-year survival. Br J Surg 91:605–609
Tan KK, Sim R (2010) Surgery for obstructed colorectal malignancy in an Asian population: predictors of morbidity and comparison between left- and right-sided cancers. J GastrointestSurg 14:295–302
Tejero E, Mainar A, Fernández L, Tobío R, De Gregorio MA (1994) New procedure for the treatment of colorectal neoplastic obstructions. Dis Colon Rectum 37:1158–1159
Watt AM, Faragher IG, Griffin TT, Rieger NA, Maddern GJ (2007) Self-expanding metallic stents for relieving malignant colorectal obstruction: a systematic review. Ann Surg 246:24–30
Jiménez-Pérez J, Casellas J, García-Cano J, Vandervoort J, García-Escribano OR, Barcenilla J, Delgado AA, Goldberg P, Gonzalez-Huix F, Vázquez-Astray E, Meisner S (2011) Colonic stenting as a bridge to surgery in malignant large-bowel obstruction: a report from two large multinational registries. Am J Gastroenterol 106:2174–2180
Jain SR, Yaow CYL, Ng CH, Neo VSQ, Lim F, Foo FJ, Wong NW, Chong CS (2020) Comparison of colonic stents, stomas and resection for obstructive left colon cancer: a meta-analysis. Tech Coloproctol 24:1121–1136
Saito S, Yoshida S, Isayama H, Matsuzawa T, Kuwai T, Maetani I, Shimada M, Yamada T, Tomita M, Koizumi K, Hirata N, Kanazawa H, Enomoto T, Sekido H, Saida Y (2016) A prospective multicenter study on self-expandable metallic stents as a bridge to surgery for malignant colorectal obstruction in Japan: efficacy and safety in 312 patients. SurgEndosc 30:3976–3986
Pirlet IA, Slim K, Kwiatkowski F, Michot F, Millat BL (2011) Emergency preoperative stenting versus surgery for acute left-sided malignant colonic obstruction: a multicenter randomized controlled trial. SurgEndosc 25:1814–1821
van Hooft JE, Bemelman WA, Oldenburg B, Marinelli AW, LutkeHolzik MF, Grubben MJ, Sprangers MA, Dijkgraaf MG, Fockens P (2011) Colonic stenting versus emergency surgery for acute left-sided malignant colonic obstruction: a multicentre randomised trial. Lancet Oncol 12:344–352
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Valenzuela C (1993) 2 solutions for estimating odds ratios with zeros. Rev Med Chil 121:1441–1444
van Hooft JE, van Halsema EE, Vanbiervliet G, Beets-Tan RG, DeWitt JM, Donnellan F, Dumonceau JM, Glynne-Jones RG, Hassan C, Jiménez-Perez J, Meisner S, Muthusamy VR, Parker MC, Regimbeau JM, Sabbagh C, Sagar J, Tanis PJ, Vandervoort J, Webster GJ, Manes G, Barthet MA, Repici A (2014) Self-expandable metal stents for obstructing colonic and extracolonic cancer: European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline. Gastrointest Endosc 80:747–761.e741–775
Lee H, Bae SU, Baek SK, Jeong WK (2017) Comparison of early and late surgery following colonic stenting for obstructive colorectal cancer. Korean J Clin Oncol 13:96–101
Matsuda A, Miyashita M, Matsumoto S, Sakurazawa N, Kawano Y, Yamada T, Matsutani T, Uchida E (2018) Optimal interval from placement of a self-expandable metallic stent to surgery in patients with malignant large bowel obstruction: a preliminary study. SurgLaparoscEndoscPercutanTechnol 28:239–244
van Hooft JE, Veld JV, Arnold D, Beets-Tan RGH, Everett S, Götz M, van Halsema EE, Hill J, Manes G, Meisner S, Rodrigues-Pinto E, Sabbagh C, Vandervoort J, Tanis PJ, Vanbiervliet G, Arezzo A (2020) Self-expandable metal stents for obstructing colonic and extracolonic cancer: European Society of Gastrointestinal Endoscopy (ESGE) Guideline - Update 2020. Endoscopy 52:389–407
Kam MH, Tang CL, Chan E, Lim JF, Eu KW (2009) Systematic review of intraoperative colonic irrigation vs. manual decompression in obstructed left-sided colorectal emergencies. Int J Colorectal Dis 24:1031–1037
Dudley HA, Racliffe AG, McGeehan D (1980) Intraoperative irrigation of the colon to permit primary anastomosis. Br J Surg 67:80–81
Broholm M, Kobborg M, Frostberg E, Jeppesen M, Gögenür I (2017) Delay of surgery after stent placement for resectable malignant colorectal obstruction is associated with higher risk of recurrence. Int J Colorectal Dis 32:513–516
Arezzo A, Balague C, Targarona E, Borghi F, Giraudo G, Ghezzo L, Arroyo A, Sola-Vera J, De Paolis P, Bossotti M, Bannone E, Forcignanò E, Bonino MA, Passera R, Morino M (2017) Colonic stenting as a bridge to surgery versus emergency surgery for malignant colonic obstruction: results of a multicentre randomised controlled trial (ESCO trial). SurgEndosc 31:3297–3305
Ceresoli M, Allievi N, Coccolini F, Montori G, Fugazzola P, Pisano M, Sartelli M, Catena F, Ansaloni L (2017) Long-term oncologic outcomes of stent as a bridge to surgery versus emergency surgery in malignant left side colonic obstructions: a meta-analysis. J Gastrointest Oncol 8:867–876
Lim TZ, Chan DKH, Tan KK (2018) Endoscopic stenting should be advocated in patients with stage IV colorectal cancer presenting with acute obstruction. J Gastrointest Oncol 9:785–790
Foo CC, Poon SHT, Chiu RHY, Lam WY, Cheung LC, Law WL (2019) Is bridge to surgery stenting a safe alternative to emergency surgery in malignant colonic obstruction: a meta-analysis of randomized control trials. SurgEndosc 33:293–302
Sloothaak DA, van den Berg MW, Dijkgraaf MG, Fockens P, Tanis PJ, van Hooft JE, Bemelman WA (2014) Oncological outcome of malignant colonic obstruction in the Dutch Stent-In 2 trial. Br J Surg 101:1751–1757
Maruthachalam K, Lash GE, Shenton BK, Horgan AF (2007) Tumour cell dissemination following endoscopic stent insertion. Br J Surg 94:1151–1154
Yamashita S, Tanemura M, Sawada G, Moon J, Shimizu Y, Yamaguchi T, Kuwai T, Urata Y, Kuraoka K, Hatanaka N, Yamashita Y, Taniyama K (2018) Impact of endoscopic stent insertion on detection of viable circulating tumor cells from obstructive colorectal cancer. Oncol Lett 15:400–406
Kye B-H, Kim J-H, Kim H-J, Lee YS, Lee I-K, Kang WK, Cho H-M, Ahn C-H, Oh S-T (2020) The optimal time interval between the placement of self-expandable metallic stent and elective surgery in patients with obstructive colon cancer. Sci Rep 10:9502
Cserni G (2003) Nodal staging of colorectal carcinomas and sentinel nodes. J ClinPathol 56:327–335
Sekimoto M, Takemasa I, Mizushima T, Ikeda M, Yamamoto H, Doki Y, Mori M (2011) Laparoscopic lymph node dissection around the inferior mesenteric artery with preservation of the left colic artery. SurgEndosc 25:861–866
Malassagne B, Valleur P, Serra J, Sarnacki S, Galian A, Hoang C, Hautefeuille P (1993) Relationship of apical lymph node involvement to survival in resected colon carcinoma. Dis Colon Rectum 36:645–653
Tsai HL, Chen YT, Yeh YS, Huang CW, Ma CJ, Wang JY (2019) Apical lymph nodes in the distant metastases and prognosis of patients with stage III colorectal cancer with adequate lymph node retrieval following FOLFOX adjuvant chemotherapy. Pathol Oncol Res 25:905–913
Yi JW, Lee TG, Lee HS, Heo SC, Jeong SY, Park KJ, Kang SB (2012) Apical-node metastasis in sigmoid colon or rectal cancer: is it a factor that indicates a poor prognosis after high ligation? Int J Colorectal Dis 27:81–87
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
All authors—Drs Tammy Lim, Hui Yu Tham, Mr Clyve Yaow, Drs Ian Tan, Dedrick Chan, Ridzuan Farouk, Kuok Chung Lee, Bettina Lieske, Ker-Kan Tan, Choon Seng Chong have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lim, T., Tham, H.Y., Yaow, C.Y.L. et al. Early surgery after bridge-to-surgery stenting for malignant bowel obstruction is associated with better oncological outcomes. Surg Endosc 35, 7120–7130 (2021). https://doi.org/10.1007/s00464-020-08232-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-08232-w