Abstract
Background
Concomitant common bile duct (CBD) stone in the setting of acute calculous cholecystitis (ACC) should be suspected once abnormal liver indices are noticed.
Aim
We aimed to identify predictors of CBD stone in patients hospitalized with ACC.
Methods
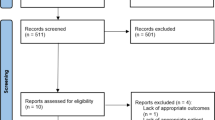
We performed a retrospective multi-center, case-controlled, study from 1st of January 2016 until the 31th of December 2018. Inclusion criteria included patients with an established diagnosis of ACC based on clinical, laboratory and radiological criteria and who had an endoscopic ultrasound (EUS) for suspected CBD stone. One-hundred and twelve patients were included, of these fifty-three patients (47.3%) were diagnosed with CBD stone by EUS.
Results
In univariate analysis, Age (OR 1.038, P = 0.001), total bilirubin (mg/dl) (OR 1.429, P = 0.02) and CBD width (mm) by US (OR 1.314, P = 0.01) were statistically significant in predicting CBD stone and remained significant in multivariate regression analysis. We developed a diagnostic score that included these three parameters, with assignment of weights for each variable according to the coefficient estimate. A low cut-off score of 0 was associated with sensitivity of 100% for CBD stone, whereas a high cut-off score of 3 was associated with sensitivity of 10% and specificity of 96.6% with a positive predictive value of 67% (ROC of 0.7558). We validated this score with an independent cohort (ROC of 0.7416) with a sensitivity of 46.6%, a specificity of 91.5% and a PPV of 87.1%.
Conclusion
We recommend incorporating this score as an aid for stratifying patients with ACC into low or high probability for concomitant CBD stone.

Similar content being viewed by others
Abbreviations
- ACC:
-
Acute calculus cholecystitis
- CBD:
-
Common bile duct
- EUS:
-
Endoscopic ultrasound
- MRCP:
-
Magnetic resonance cholangiopancreatography
- ASGE:
-
American Society for Gastrointestinal Endoscopy
- US:
-
Ultrasound
- ESGE:
-
European Society of Gastrointestinal Endoscopy
- ALT:
-
Alanine aminotransferase
- AST:
-
Aspartate transaminase
- ALP:
-
Alkaline phosphatase
- GGT:
-
Gamma-glutamyl transferase
- WBC:
-
White blood cells
- OR:
-
Odds ratio
- ROC:
-
Receiver operating characteristics
- PPV:
-
Positive predictive value
- NPV:
-
Negative predictive value
- ERCP:
-
Endoscopic retrograde cholangiopancreatography
References
Strasberg SM (2008) Clinical practice. Acute calculous cholecystitis. N Engl J Med 358:2804–2811
Trowbridge RL, Rutkowski NK, Shojania KG (2003) Does this patient have acute cholecystitis? JAMA 289:80–86
Committee ASoP, Fisher L, Lee Krinsky M, Anderson MA, Appalaneni V, Banerjee S, Ben-Menachem T, Cash BD, Decker GA, Fanelli RD, Friis C, Fukami N, Harrison ME, Ikenberry SO, Jain R, Jue T, Khan K, Maple JT, Strohmeyer L, Sharaf R, Dominitz JA (2010) The role of endoscopy in the management of obscure GI bleeding. Gastrointest Endosc 72:471–479
Al-Jiffry BO, Elfateh A, Chundrigar T, Othman B, Almalki O, Rayza F, Niyaz H, Elmakhzangy H, Hatem M (2013) Non-invasive assessment of choledocholithiasis in patients with gallstones and abnormal liver function. World J Gastroenterol 19:5877–5882
Ward WH, Fluke LM, Hoagland BD, Zarow GJ, Held JM, Ricca RL (2015) The role of magnetic resonance cholangiopancreatography in the diagnosis of choledocholithiasis: do benefits outweigh the costs? Am Surg 81:720–725
Netinatsunton N, Attasaranya S, Sottisuporn J, Witeerungrot T, Jongboonyanuparp T, Piratvisuth T, Ovartlarnporn B (2016) Comparing cost-effectiveness between endoscopic ultrasound and endoscopic retrograde cholangiopancreatography in diagnosis of common bile duct stone in patients with predefined risks: a study from a developing country. Endosc Ultrasound 5:165–172
Adams MA, Hosmer AE, Wamsteker EJ, Anderson MA, Elta GH, Kubiliun NM, Kwon RS, Piraka CR, Scheiman JM, Waljee AK, Hussain HK, Elmunzer BJ (2015) Predicting the likelihood of a persistent bile duct stone in patients with suspected choledocholithiasis: accuracy of existing guidelines and the impact of laboratory trends. Gastrointest Endosc 82:88–93
Prachayakul V, Aswakul P, Bhunthumkomol P, Deesomsak M (2014) Diagnostic yield of endoscopic ultrasonography in patients with intermediate or high likelihood of choledocholithiasis: a retrospective study from one university-based endoscopy center. BMC Gastroenterol 14:165
Shah AP, Mourad MM, Bramhall SR (2018) Acute pancreatitis: current perspectives on diagnosis and management. J Inflamm Res 11:77–85
Manes G, Paspatis G, Aabakken L, Anderloni A, Arvanitakis M, Ah-Soune P, Barthet M, Domagk D, Dumonceau JM, Gigot JF, Hritz I, Karamanolis G, Laghi A, Mariani A, Paraskeva K, Pohl J, Ponchon T, Swahn F, Ter Steege RWF, Tringali A, Vezakis A, Williams EJ, van Hooft JE (2019) Endoscopic management of common bile duct stones: European Society of Gastrointestinal Endoscopy (ESGE) guideline. Endoscopy 51:472–491
Committee ASoP, Maple JT, Ben-Menachem T, Anderson MA, Appalaneni V, Banerjee S, Cash BD, Fisher L, Harrison ME, Fanelli RD, Fukami N, Ikenberry SO, Jain R, Khan K, Krinsky ML, Strohmeyer L, Dominitz JA (2010) The role of endoscopy in the evaluation of suspected choledocholithiasis. Gastrointest Endosc 71:1–9
Barkun AN, Barkun JS, Fried GM, Ghitulescu G, Steinmetz O, Pham C, Meakins JL, Goresky CA (1994) Useful predictors of bile duct stones in patients undergoing laparoscopic cholecystectomy. McGill Gallstone Treatment Group Ann Surg 220:32–39
Hauer-Jensen M, Karesen R, Nygaard K, Solheim K, Amlie EJ, Havig O, Rosseland AR (1993) Prospective randomized study of routine intraoperative cholangiography during open cholecystectomy: long-term follow-up and multivariate analysis of predictors of choledocholithiasis. Surgery 113:318–323
Prat F, Meduri B, Ducot B, Chiche R, Salimbeni-Bartolini R, Pelletier G (1999) Prediction of common bile duct stones by noninvasive tests. Ann Surg 229:362–368
Sethi S, Wang F, Korson AS, Krishnan S, Berzin TM, Chuttani R, Pleskow DK, Sawhney MS (2016) Prospective assessment of consensus criteria for evaluation of patients with suspected choledocholithiasis. Dig Endosc 28:75–82
Suarez AL, LaBarre NT, Cotton PB, Payne KM, Cote GA, Elmunzer BJ (2016) An assessment of existing risk stratification guidelines for the evaluation of patients with suspected choledocholithiasis. Surg Endosc 30:4613–4618
Chisholm PR, Patel AH, Law RJ, Schulman AR, Bedi AO, Kwon RS, Wamsteker EJ, Anderson MA, Elta GH, Govani SM, Prabhu A (2019) Preoperative predictors of choledocholithiasis in patients presenting with acute calculous cholecystitis. Gastrointest Endosc 89(977–983):e972
Narvaez Rivera RM, Gonzalez Gonzalez JA, Monreal Robles R, Garcia Compean D, Paz Delgadillo J, Garza Galindo AA, Maldonado Garza HJ (2016) Accuracy of ASGE criteria for the prediction of choledocholithiasis. Rev Esp Enferm Dig 108:309–314
Kaspy MS, Hassan GM, Paquin SC, Sahai AV (2019) An assessment of the yield of EUS in patients referred for dilated common bile duct and normal liver function tests. Endosc Ultrasound. 8:318
Verma D, Kapadia A, Eisen GM, Adler DG (2006) EUS vs MRCP for detection of choledocholithiasis. Gastrointest Endosc 64:248–254
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors
Author information
Authors and Affiliations
Contributions
TK and WS contributed to the design of the manuscript. TK, AK, MM, and WS contributed to data analysis and interpretation. All authors contributed to data collection and analysis. TK, AM and WS contributed to critical revision of the manuscript and all authors approved the final version to be published.
Corresponding author
Ethics declarations
Disclosures
Drs. Tawfik Khoury, Anas Kadah, Amir Mari, Itai Kalisky, Lior Katz, Mahmud Mahamid and Wisam Sbeit have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Khoury, T., Kadah, A., Mari, A. et al. A validated score predicting common bile duct stone in patients hospitalized with acute calculus cholecystitis: a multi-center retrospective study. Surg Endosc 35, 3709–3715 (2021). https://doi.org/10.1007/s00464-020-07853-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07853-5