Abstract
Background
ELRR by TEM is a valid alternative to TME in selected patients with early low rectal cancer, with similar long-term oncological results and better Quality of Life. The authors’ policy is to close the residual defect, with possibly a higher risk of dehiscence from tension on the suture line. Aim is to evaluate if a modified technique may reduce the risk of dehiscence.
Methods
The latest series of 50 patients undergoing ELRR was analyzed and patients were divided in two consecutive groups. In Group A, 25 patients underwent ELRR by TEM with the authors’ standard technique. In Group B, a subsequent series of 25 patients also underwent ELRR, but the perirectal residual cavity was filled with a hemostatic agent prior to rectal wall closure. After suture completion, the rectal ampulla was stuffed with gauzes to avoid the formation of a perirectal fluid collection, by enlarging the volume of the residual rectal ampulla. A transanal Foley catheter was positioned for gas evacuation.
Results
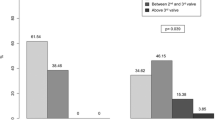
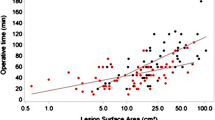
There were no significant differences in mean tumor distance from the anal verge, mean lesion diameter, mean operative time, and pathological staging between the two groups. Neoadjuvant radio-chemotherapy (n-RCT) in Groups A and B was performed in 6 and 2 patients, respectively. Suture line dehiscence in Group A occurred in 3 patients (12 %) and in group B it was nil. In patients who experienced a dehiscence, mean lesion diameter was 6.3 cm (range 6–7). None of these patients had undergone n-RCT.
Conclusion
After ELRR by TEM, suture line dehiscence is presumably related to the wider size of the residual cavity. Obliteration of the residual perirectal space with hemostatic agent and by gauzes’ introduction in the rectal ampulla may reduce the risk of postoperative perirectal abscess and thus reduce the suture line dehiscence rate.
Similar content being viewed by others
References
Lezoche E, Guerrieri M, Paganini AM, D’Ambrosio G, Baldarelli M, Lezoche G, Feliciotti F, De Sanctis A (2005) Transanal endoscopic versus total mesorectal laparoscopic resections of T2-N0 low rectal cancers after neoadjuvant treatment: a prospective randomized trial with a 3-years minimum follow-up period. Surg Endosc 19(6):751–756
Lezoche E, Guerrieri M, Paganini AM, Baldarelli M, De Sanctis A, Lezoche G (2005) Long-term results in patients with T2-3 N0 distal rectal cancer undergoing radiotherapy before transanal endoscopic microsurgery. Br J Surg 92(12):1546–1552
Lezoche E, Baldarelli M, Lezoche G, Paganini AM, Gesuita R, Guerrieri M (2012) Randomized clinical trial of endoluminal locoregional resection versus laparoscopic total mesorectal excision for T2 rectal cancer after neoadjuvant therapy. Br J Surg 99(9):1211–1218. doi:10.1002/bjs.8821
Lezoche E, Paganini AM, Fabiani B, Balla A, Vestri A, Pescatori L, Scoglio D, D’Ambrosio G, Lezoche G (2013) Quality-of-life impairment after endoluminal locoregional resection and laparoscopic total mesorectal excision. Surg Endosc 28(1):227–234
Buess G, Theiss R, Hutterer F, Pichlmaier H, Pelz C, Holfeld T, Said S, Isselhard W (1983) Transanal endoscopic surgery of the rectum-testing a new method in animal experiments. Leber Magen Darm 13(2):73–77
Buess G, Hutterer F, Theiss J, Böbel M, Isselhard W, Pichlmaier H (1984) A system for a transanal endoscopic rectum operation. Chirurg 55:677–680
Fujita F, Torashima Y, Kuroki T, Eguchi S (2013) The risk factors and predictive factors for anastomotic leakage after resection for colorectal cancer: reappraisal of the literature. Surg Today
Matthiessen P, Hallböök O, Andersson M, Rutegård J, Sjödahl R (2004) Risk factors for anastomotic leakage after anterior resection of the rectum. Colorectal Dis 6(6):462–469
Lim M, Akhtar S, Sasapu K, Harris K, Burke D, Sagar P, Finan P (2006) Clinical and subclinical leaks after low colorectal anastomosis: a clinical and radiologic study. Dis Colon Rectum 49(10):1611–1619
Kanellos I, Vasiliadis K, Angelopoulos S, Tsachalis T, Pramateftakis MG, Mantzoros I, Betsis D (2004) Anastomotic leakage following anterior resection for rectal cancer. Tech Coloproctol Suppl 1:s79–s81
Krarup PM, Jorgensen LN, Andreasen AH, Harling H, Danish Colorectal Cancer Group (2012) A nationwide study on anastomotic leakage after colonic cancer surgery. Colorectal Dis 14(10):e661–e667. doi:10.1111/j.1463-1318.2012.03079.x
Law WI, Chu KW, Ho JW, Chan CW (2000) Risk factors for anastomotic leakage after low anterior resection with total mesorectal excision. Am J Surg 179(2):92–96
Trencheva K, Morrissey KP, Wells M, Mancuso CA, Lee SW, Sonoda T, Michelassi F, Charlson ME, Milsom JW (2013) Identifying important predictors for anastomotic leak after colon and rectal resection: prospective study on 616 patients. Ann Surg 257(1):108–113. doi:10.1097/SLA.0b013e318262a6cd
Park JS, Choi GS, Kim SH, Kim HR, Kim NK, Lee KY, Kang SB, Kim JY, Lee KY, Kim BC, Bae BN, Son GM, Lee SI, Kang H (2013) Multicenter analysis of risk factors for anastomotic leakage after laparoscopic rectal cancer excision: the Korean laparoscopic colorectal surgery study group. Ann Surg 257(4):665–671. doi:10.1097/SLA.0b013e31827b8ed9
Alves A, Panis Y, Trancart D, Regimbeau JM, Pocard M, Valleur P (2002) Factors associated with clinically significant anastomotic leakage after large bowel resection: multivariate analysis of 707 patients. World J Surg 26(4):499–502
Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, Smith AM, Heath RM, Brown JM, MRC CLASICC trial group (2005) Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. Lancet 365(9472):1718–1726
Veldkamp R, Kuhry E, Hop WC, Jeekel J, Kazemier G, Bonjer HJ, Haglind E, Påhlman L, Cuesta MA, Msika S, Morino M, Lacy AM, COlon cancer Laparoscopic or Open Resection Study Group (COLOR) (2005) Laparoscopic surgery versus open surgery for colon cancer: short-term outcomes of a randomised trial. Lancet Oncol 6(7):477–484
Slim K, Vicaut E, Launay-Savary MV, Contant C, Chipponi J (2009) Updated systematic review and meta-analysis of randomized clinical trials on the role of mechanical bowel preparation before colorectal surgery. Ann Surg 249(2):203–209. doi:10.1097/SLA.0b013e318193425a
Van’t Sant HP, Weidema WF, Hop WC, Oostvogel HJ, Contant CM (2010) The influence of mechanical bowel preparation in elective lower colorectal surgery. Ann Surg 251(1):59–63. doi:10.1097/SLA.0b013e3181c0e75c
Chang JS, Keum KC, Kim NK, Baik SH, Min BS, Huh H, Lee CG, Koom WS (2013) Preoperative chemoradiotherapy effects on anastomotic leakage After rectal cancer resection: a propensity score matching analysis. Ann Surg 259(3):516–521
Park JS, Choi GS, Kim SH, Kim HR, Kim NK, Lee KY, Kang SB, Kim JY, Lee KY, Kim BC, Bae BN, Son GM, Lee SI, Kang H (2013) Multicenter analysis of risk factors for anastomotic leakage after laparoscopic rectal cancer excision: the Korean laparoscopic colorectal surgery study group. Ann Surg 257(4):665–671. doi:10.1097/SLA.0b013e31827b8ed9
Karanja ND, Corder AP, Bearn P, Heald RJ (1994) Leakage from stapled low anastomosis after total mesorectal excision for carcinoma of the rectum. Br J Surg 81(8):1224–1226
Ganai S, Kanumuri P, Rao RS, Alexander AI (2006) Local recurrence after transanal endoscopic microsurgery for rectal polyps and early cancers. Ann Surg Oncol 13(4):547–556
de Graaf EJ, Burger JW, van Ijsseldijk AL, Tetteroo GW, Dawson I, Hop WC (2011) Transanal endoscopic microsurgery is superior to transanal excision of rectal adenomas. Colorectal Dis 13(7):762–767. doi:10.1111/j.1463-1318.2010.02269.x
Allaix ME, Arezzo A, Caldart M, Festa F, Morino M (2009) Transanal endoscopic microsurgery for rectal neoplasms: experience of 300 consecutive cases. Dis Colon Rectum 52(11):1831–1836. doi:10.1007/DCR.0b013e3181b14d2d
Kreissler-Haag D, Schuld J, Lindemann W, König J, Hildebrandt U, Schilling M (2008) Complications after transanal endoscopic microsurgical resection correlate with location of rectal neoplasms. Surg Endosc 22(3):612–616
Allaix ME, Aresso A, Cassoni P, Famiglietti F, Morino M (2012) Recurrence after transanal endoscopic microsurgery for large rectal adenomas. Surg Endosc 26(9):2594–2600. doi:10.1007/s00464-012-2238-z
Bretagnol F, Merrie A, George B, Warren BF, Mortensen NJ (2007) Local excision of rectal tumours by transanal endoscopic microsurgery. Br J Surg 94(5):627–633
Marks JH, Valsdottir EB, DeNittis A, Yarandi SS, Newman DA, Nweze I, Mohiuddin M, Marks GJ (2009) Transanal endoscopic microsurgery for the treatment of rectal cancer: comparison of wound complications rates with and without neoadjuvant radiation therapy. Surg Endosc 23(5):1081–1087. doi:10.1007/s00464-009-0326-5
Marks JH, Marchionni C, Marks GJ (2003) Transanal endoscopic microsurgery in the treatment of select rectal cancers or tumours suspicious for cancer. Surg Endosc 17(7):1114–1117
Bignell MB, Ramwell A, Evans JR, Dastur N, Simson JN (2010) Complications of transanal endoscopic microsurgery (TEMS): a prospective audit. Colorectal Dis 12(7 Online):e99–103. doi:10.1111/j.1463-1318.2009.02071.x
Koebrugge B, Bosscha K, Ernst MF (2009) Transanal endoscopic microsurgery for local excision of rectal lesions: is there a learning curve? Dig Surg. 26(5):372–377. doi:10.1159/000257228
Maslekar S, Pillinger SH, Monson JR (2007) Transanal endoscopic microsurgery for carcinoma of the rectum. Surg Endosc 21(1):97–102
Disclosures
Prof. Alessandro M. Paganini, Dr. Andrea Balla, Dr. Silvia Quaresima, Dr. Giancarlo D’Ambrosio, Dr. Paolo Bruzzone, Prof. Emanuele Lezoche, have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Additional information
Presented at the SAGES 2014 Annual Meeting, April 2–5, 2014, Salt Lake City, Utah.
Rights and permissions
About this article
Cite this article
Paganini, A.M., Balla, A., Quaresima, S. et al. Tricks to decrease the suture line dehiscence rate during endoluminal loco-regional resection (ELRR) by transanal endoscopic microsurgery (TEM). Surg Endosc 29, 1045–1050 (2015). https://doi.org/10.1007/s00464-014-3776-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3776-3