Abstract
Background
Mesh repair may decrease the recurrence rate but bears risk of esophageal complications. This study aimed to analyze the long-term results of laparoscopic hiatal repair depending on hiatal surface area (HSA).
Methods
The results from 658 procedures were analyzed. Group 1 had 343 patients with HSA smaller than 10 cm2 (small hernias), for whom primary crural repair was performed. Group 2 had 261 patients with HSA size 10–20 cm2 (large hernias), for whom primary crural repair (subgroup A) or mesh repair (subgroup B) was performed. Group 3 had 54 patients with HSA larger than 20 cm2 (giant hernias), for whom only mesh repair was performed.
Results
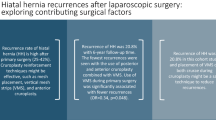
The mean follow-up period was 28.6 months (range, 10–48 months). Primary repair results in a higher recurrence rate for large hernias (11.9 %) than for small hernias (3.5 %) (p = 0.0016). For large hernias, the original method of sub-lay lightweight partially absorbable mesh repair provides a lower recurrence rate than primary repair (4.9 % vs 11.9 %; p = 0.0488) and a comparable dysphagia rate (2.1 % vs 2.2 %; p = 0.6533). For giant hernias, mesh repair results in a higher recurrence rate than for large hernias (20 % vs 4.9 %; p = 0.0028). The analysis of variance (ANOVA) HSA recurrence ratio confirmed the correctness of the chosen threshold levels (10 and 20 cm2) for subdividing hernias into three classes according to the new classification.
Conclusions
The authors advise routine measurement of HSA and use of relative classification, primary suturing as the optimal repair for small hernias, the original technique of sub-lay lightweight partially absorbable mesh repair as the apparent best treatment for large hernias, and the original technique for giant hernias, which provides results corresponding to those reported in the literature, although these results require improvement.




Similar content being viewed by others
References
Draaisma WA, Gooszen HG, Tournoij E, Broeders JA (2005) Controversies in paraesophageal hernia repair: a review of literature. Surg Endosc 19:1300–1308
Granderath FA, Schweiger UM, Kamolz T et al (2005) Laparoscopic Nissen fundoplication with prosthetic hiatal closure reduces postoperative intrathoracic wrap herniation: preliminary results of a prospective randomized functional and clinical study. Arch Surg 140:40–48
Rathore MA, Andrabi SI, Bhatti MI et al (2007) Metaanalysis of recurrence after laparoscopic repair of paraesophageal hernia. JSLS 11:456–460
Targarona EM, Bendahan G, Balague C et al (2004) Mesh in the hiatus: a controversial issue. Arch Surg 139:1286–1296
Andujar JJ, Papasavas PK, Birdas T, Robke J et al (2004) Laparoscopic repair of large paraesophageal hernia is associated with a low incidence of recurrence and reoperation. Surg Endosc 18:444–447
Frantzides CT, Madan AK, Carlson MA, Stavropoulos GP (2002) A prospective, randomized trial of laparoscopic polytetrafluoroethylene (PTFE) patch repair vs simple cruroplasty for large hiatal hernia. Arch Surg 137:649–652
Oelschlager BK, Pellegrini CA, Hunter JG et al (2011) Biologic prosthesis to prevent recurrence after laparoscopic paraesophageal hernia repair: long-term follow-up from a multicenter, prospective, randomized trial. J Am Coll Surg 213:461–468
Antoniou SA, Koch OO, Antoniou GA, Pointner R, Granderath FA (2012) Mesh-reinforced hiatal hernia repair: a review on the effect on postoperative dysphagia and recurrence. Langenbecks Arch Surg 397:19–27
Frantzides CT, Carlson MA, Loizides S et al (2010) Hiatal hernia repair with mesh: a survey of SAGES members. Surg Endosc 24:1017–1024
Granderath FA, Schweiger UM, Kamolz T et al (2005) Dysphagia after laparoscopic antireflux surgery: a problem of hiatal closure more than a problem of the wrap. Surg Endosc 19:1439–1446
Stadlhuber RJ, Shenf AE, Mittal SK, Fitzqibbons RJ et al (2009) Mesh complications after prosthetic reinforcement of hiatal closure: a 28-case series. Surg Endosc 23:1219–1926
Granderath FA, Schweiger UM, Pointner R (2007) Laparoscopic antireflux surgery: tailoring the hiatal closure to the size of hiatal surface area. Surg Endosc 21:542–548
Grubnik VV, Malynovskyy AV (2011) Actual questions of laparoscopic hiatal hernia repair: own experience and literature review. Ukr J Surg 5:95–99
Grubnik VV, Malynovskyy AV, Grubnik OV, Ilyashenko VV (2011) Effectiveness of different types of mesh for laparoscopic repair of large hiatal hernias. Abstracts of 18th International Congress of European Association for Endoscopic Surgery). Surg Endosc 25:S41
Grubnik VV, Malynovskyy AV, Ilyashenko VV (2011) Comparative study of different types of mesh for laparoscopic repair of large hiatal hernias Abstracts of 2011 scientific session of the Society of American Gastrointestinal and Endoscopic Surgeons). Surg Endosc 25:S315
Granderath FA, Carlson MA, Champion JK, Szold A, Basso N, Pointner R, Frantzides CT (2006) Prosthetic closure of the esophageal hiatus in large hiatal hernia repair and laparoscopic antireflux surgery. Surg Endosc 20:367–379
Johnson JM, Carbonell AM, Carmody BJ et al (2006) Laparoscopic mesh hiatoplasty for paraesophageal hernias and fundoplications: a critical analysis of available literature. Surg Endosc 20:362–366
Champion JK, McKernan JB (1998) Hiatal size and risk of recurrence after laparoscopic fundoplication (abstract). Surg Endosc 12:565–570
Dallemagne B, Weerts J, Markiewicz S et al (2006) Clinical results of laparoscopic fundoplication at ten years surgery. Surg Endosc 20:159–165
Disclosures
V. V. Grubnik and A. V. Malynovskyy have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Grubnik, V.V., Malynovskyy, A.V. Laparoscopic repair of hiatal hernias: new classification supported by long-term results. Surg Endosc 27, 4337–4346 (2013). https://doi.org/10.1007/s00464-013-3069-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-013-3069-2