Abstract
Background
Mesh-assisted hiatal closure during foregut surgery is increasing. Our aim was to evaluate the complications that follow revisional foregut surgery. Specifically, we compared surgical indications and perioperative outcomes between patients with and without prior hiatal mesh (PHM).
Methods
We conducted an institutional review board (IRB)-approved retrospective cohort study from a single tertiary-care referral center. Over 37 months, 91 patients underwent revisional foregut surgery. We excluded 13 cases including operations performed primarily for obesity or achalasia. Of the remaining 78 patients, 10 had PHM and 68 were nonmesh patients (NM).
Results
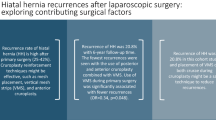
The groups were similar in terms of age, body mass index (BMI), American Society of Anesthesiologists (ASA) classification, and rates and types of anatomic failure. Compared with NM patients, PHM patients had increased estimated blood loss (410 vs. 127 ml, p < 0.01) and operative time (4.07 vs. 2.89 h, p < 0.01). The groups had no difference in perioperative blood transfusion or length of stay. Complete fundoplication was more commonly created in NM patients (2/10 vs. 42/68, p = 0.03). Three of the 10 PHM patients and 3 of the 68 NM patients required major resection. Therefore, PHM patients had 6.8-fold increased risk of major resection compared with NM patients [95% confidence interval (CI) = 1.585, 29.17; p = 0.05]. The NM patients with multiple prior hiatal operations had 4.6-fold increased risk of major resection compared with those with one prior operation (95% CI = 2.919, 7.384; p = 0.03). In PHM patients, however, the number of prior hiatal operations was not associated with major resection.
Conclusions
PHM is associated with increased risk of major resection at revision. The pattern of failure was not different in patients with hiatal mesh, suggesting that hiatal mesh does not eliminate the potential for revision. When performing hiatal herniorrhaphy, the increased risk of recurrence without mesh must be weighed against the potential risk for subsequent major resection when using mesh.
Similar content being viewed by others
References
Targarona EM, Bendahan G, Balague C, Garriga J, Trias M (2004) Mesh in the hiatus: a controversial issue. Arch Surg 139:1286–1296 (discussion 1296)
Cuschieri A, Shimi S, Nathanson LK (1992) Laparoscopic reduction, crural repair, and fundoplication of large hiatal hernia. Am J Surg 163:425–430
van der Peet DL, Klinkenberg-Knol EC, Alonso Poza A, Sietses C, Eijsbouts QA, Cuesta MA (2000) Laparoscopic treatment of large paraesophageal hernias: both excision of the sac and gastropexy are imperative for adequate surgical treatment. Surg Endosc 14:1015–1018
Jobe BA, Aye RW, Deveney CW, Domreis JS, Hill LD (2002) Laparoscopic management of giant type III hiatal hernia and short esophagus. Objective follow-up at three years. J Gastrointest Surg 6:181–188 (discussion 188)
Luketich JD, Raja S, Fernando HC, Campbell W, Christie NA, Buenaventura PO, Weigel TL, Keenan RJ, Schauer PR (2000) Laparoscopic repair of giant paraesophageal hernia: 100 consecutive cases. Ann Surg 232:608–618
Kuster GG, Gilroy S (1993) Laparoscopic technique for repair of paraesophageal hiatal hernias. J Laparoendosc Surg 3:331–338
Basso N, De Leo A, Genco A, Rosato P, Rea S, Spaziani E, Primavera A (2000) 360 degrees laparoscopic fundoplication with tension-free hiatoplasty in the treatment of symptomatic gastroesophageal reflux disease. Surg Endosc 14:164–169
Athanasakis H, Tzortzinis A, Tsiaoussis J, Vassilakis JS, Xynos E (2001) Laparoscopic repair of paraesophageal hernia. Endoscopy 33:590–594
Oelschlager BK, Barreca M, Chang L, Pellegrini CA (2003) The use of small intestine submucosa in the repair of paraesophageal hernias: initial observations of a new technique. Am J Surg 186:4–8
Kamolz T, Granderath FA, Bammer T, Pasiut M, Pointner R (2002) Dysphagia and quality of life after laparoscopic Nissen fundoplication in patients with and without prosthetic reinforcement of the hiatal crura. Surg Endosc 16:572–577
Horgan S, Eubanks TR, Jacobsen G, Omelanczuk P, Pellegrini CA (1999) Repair of paraesophageal hernias. Am J Surg 177:354–358
Huntington TR (1997) Laparoscopic mesh repair of the esophageal hiatus. J Am Coll Surg 184:399–400
Granderath FA, Schweiger UM, Kamolz T, Asche KU, Pointner R (2005) Laparoscopic Nissen fundoplication with prosthetic hiatal closure reduces postoperative intrathoracic wrap herniation: preliminary results of a prospective randomized functional and clinical study. Arch Surg 140:40–48
Frantzides CT, Madan AK, Carlson MA, Stavropoulos GP (2002) A prospective, randomized trial of laparoscopic polytetrafluoroethylene (PTFE) patch repair vs simple cruroplasty for large hiatal hernia. Arch Surg 137:649–652
Oelschlager BK, Pellegrini CA, Hunter J, Soper N, Brunt M, Sheppard B, Jobe B, Polissar N, Mitsumori L, Nelson J, Swanstrom L (2006) Biologic prosthesis reduces recurrence after laparoscopic paraesophageal hernia repair: a multicenter, prospective, randomized trial. Ann Surg 244:481–490
Hashemi M, Peters JH, DeMeester TR, Huprich JE, Quek M, Hagen JA, Crookes PF, Theisen J, DeMeester SR, Sillin LF, Bremner CG (2000) Laparoscopic repair of large type III hiatal hernia: objective followup reveals high recurrence rate. J Am Coll Surg 190:553–560 (discussion 560–561)
Luostarinen M, Rantalainen M, Helve O, Reinikainen P, Isolauri J (1998) Late results of paraoesophageal hiatus hernia repair with fundoplication. Br J Surg 85:272–275
Hunter JG, Smith CD, Branum GD, Waring JP, Trus TL, Cornwell M, Galloway K (1999) Laparoscopic fundoplication failures: patterns of failure and response to fundoplication revision. Ann Surg 230:595–604 (discussion 604–606)
Terry M, Smith CD, Branum GD, Galloway K, Waring JP, Hunter JG (2001) Outcomes of laparoscopic fundoplication for gastroesophageal reflux disease and paraesophageal hernia. Surg Endosc 15:691–699
Smith CD, McClusky DA, Rajad MA, Lederman AB, Hunter JG (2005) When fundoplication fails: redo? Ann Surg 241:861–869 (discussion 869–871)
Granderath FA, Kamolz T, Schweiger UM, Pointner R (2006) Impact of laparoscopic nissen fundoplication with prosthetic hiatal closure on esophageal body motility: results of a prospective randomized trial. Arch Surg 141:625–632
Luketich JD, Nason KS, Christie NA, Pennathur A, Jobe BA, Landreneau RJ, Schuchert MJ (2010) Outcomes after a decade of laparoscopic giant paraesophageal hernia repair. J Thorac Cardiovasc Surg 139:395–404, 404.e1
Griffith PS, Valenti V, Qurashi K, Martinez-Isla A (2008) Rejection of goretex mesh used in prosthetic cruroplasty: a case series. Int J Surg 6:106–109
Rumstadt B, Kahler G, Mickisch O, Schilling D (2008) Gastric mesh erosion after hiatoplasty for recurrent paraesophageal hernia. Endoscopy 40 Suppl 2:E70
Tatum RP, Shalhub S, Oelschlager BK, Pellegrini CA (2008) Complications of PTFE mesh at the diaphragmatic hiatus. J Gastrointest Surg 12:953–957
Stadlhuber RJ, Sherif AE, Mittal SK, Fitzgibbons RJ Jr, Brunt LM, Hunter JG, DeMeester TR, Swanstrom LL, Smith CD, Filipi CJ (2009) Mesh complications after prosthetic reinforcement of hiatal closure: a 28-case series. Surg Endosc 23:1219–1226
Iqbal A, Awad Z, Simkins J, Shah R, Haider M, Salinas V, Turaga K, Karu A, Mittal SK, Filipi CJ (2006) Repair of 104 failed anti-reflux operations. Ann Surg 244:42–51
Disclosures
Authors Parker, Bowers, Bray, Harris, Belli, Pfluke, Preissler, Asbun, and Smith, have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Parker, M., Bowers, S.P., Bray, J.M. et al. Hiatal mesh is associated with major resection at revisional operation. Surg Endosc 24, 3095–3101 (2010). https://doi.org/10.1007/s00464-010-1095-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-010-1095-x