Abstract
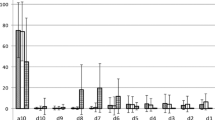
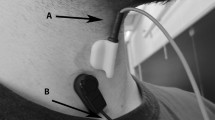
Cervical auscultation is the use of a listening device, typically a stethoscope in clinical practice, to assess swallow sounds and by some definitions airway sounds. Judgments are then made on the normality or degree of impairment of the sounds. Listeners interpret the sounds and suggest what might be happening with the swallow or causing impairment. A major criticism of cervical auscultation is that there is no evidence on what causes the sounds or whether the sounds correspond to physiologically important, health-threatening events. We sought to determine in healthy volunteers (1) if a definitive set of swallow sounds could be identified, (2) the order in which swallow sounds and physiologic events occur, and (3) if swallow sounds could be matched to the observed physiologic events. Swallow sounds were computer recorded via a Littmann stethoscope from 19 healthy volunteers (8 males, 11 females, age range = 18–73 years) during simultaneous fiberoptic laryngoscopy and respiration monitoring. Six sound components could be distinguished but none of these occurred in all swallows. There was a wide spread and a large degree of overlap of the timings of swallow sounds and physiologic events. No individual sound component was consistently associated with a physiologic event, which is a clinically significant finding. Comparisons of groups of sounds and events suggest associations between the preclick and the onset of apnea; the preclick and the start of epiglottic excursion; the click and the epiglottis returning to rest; the click and the end of the swallow apnea. There is no evidence of a causal link. The absence of a swallow sound in itself is not a definite sign of pathologic swallowing, but a repeated abnormal pattern may indicate impairment. At present there is no robust evidence that cervical auscultation of swallow sounds should be adopted in routine clinical practice. There are no data to support the inclusion of the technique into clinical guidelines or management protocols. More evaluation using imaging methods such as videofluoroscopy is required before this subjective technique is validated for clinical use by those assessing swallowing outside of a research context.



Similar content being viewed by others
References
Zenner PM, Losinski DS, Mills RH: Using cervical auscultation in the clinical dysphagia examination in long-term care. Dysphagia 10:27-31, 1995
Stroud A, Lawrie B, Wiles C: Inter- and intra-rater reliability of cervical auscultation to detect aspiration in patients with dysphagia. Clin Rehabil 16:640–645, 2002
Cichero JAY, Murdoch BE: The physiologic cause of swallowing sounds: answers from heart sounds and vocal tract acoustics. Dysphagia 13:39–52, 1998
Marks L, Rainbow D: Working with Dysphagia. Bicester: Speechmark Publishing Ltd, 2001, 251 pp
Hamlet S, Nelson RJ, Patterson RL: Interpreting the sounds of swallowing: fluid flow through the cricopharyngeus. Ann Otol Rhinol Laryngol 99:749–752, 1990
Boiron M, Rouleau P, Metman EH: Exploration of pharyngeal swallowing by audiosignal recording. Dysphagia 12:86–92, 1997
Cichero JAY, Murdoch BE: Acoustic signature of the normal swallow: characterization by age, gender, and bolus volume. Ann Otol Rhinol Laryngol 111:623–632, 2002
Leder SB, Sasaki CT: Comment on “Acoustic signature of the normal swallow characterization by age, gender and bolus volume”. Dysphagia 18:144, 2003
McKaig T: McKaignet: Dedicated to providing information regarding Cervical Auscultation (CA) ongoing research and educational opportunities. http://www.mckaignet.com/research.htm. Accessed 15 Dec 2005
Mackowiak RC, Brenman HS, Friedman MHF: Acoustic profile of deglutition. Proc Soc Exp Biol Med 125:1149–1152, 1967
Perlman AL, Ettema SL, Barkmeier J: Respiratory and acoustic signals associated with bolus passage during swallowing. Dysphagia 15:89–94, 2000
Takahashi K, Groher ME, Michi K: Methodology for detecting swallowing sounds. Dysphagia 9:54–62, 1994
McKaig N, Stroud A: The comparison of swallowing sounds with simultaneously recorded fluoroscopic imaging. Dysphagia 12: 30, 1997 [poster abstract]
Reddy NP, Canilang EP, Casterline J, Rane MB, Joshi AM, Thomas R, Candadai R: Noninvasive acceleration measurements to characterize the pharyngeal phase of swallowing. J Biomed Eng 13:379–383, 1991
Selley WG, Ellis RE, Flack FC, Bayliss SR, Pearce VR: The synchronization of respiration and swallow sounds with videofluoroscopy during swallowing. Dysphagia 9:162–167, 1994
Leslie P, Drinnan M, Finn P, Ford G, Wilson J: Reliability and validity of cervical auscultation: a controlled comparison using videofluoroscopy. Dysphagia 19:231–240, 2004
Hamlet S, Penney DG, Formolo J: Stethoscope acoustics and cervical auscultation of swallowing. Dysphagia 9:63–68, 1994
Cichero J, Murdoch B: Detection of swallowing sounds: methodology revisited. Dysphagia 17:40–49, 2002
Hibberd J, Taylor J: Cervical auscultation training course. Quest Training, UK: Birmingham, 2002
Stroud A: Cervical Auscultation: a one-day workshop. Western Infirmary, UK: Glasgow, 1999
Schulze-Delrieu K, Miller R: Clinical Assessment of Dysphagia. In: Perlman AL, Schulze-Delrieu K (eds.): Deglutition and its Disorders. San Diego: Singular Publishing Group, 1997, pp 125–152
Hiss SG, Treole K, Stuart A: Effects of age, gender, bolus volume, and trial on swallowing apnea duration and swallow/respiratory phase relationships of normal adults. Dysphagia 16:128–135, 2001
Leslie P, Drinnan M, Ford G, Wilson J: Swallow respiratory patterns and aging: presbyphagia or dysphagia? J Gerontol 60:391–395, 2005
Leslie P: Cervical auscultation: myths and magic – evidence and reliability. Study day. Freeman Hospital, UK: Newcastle upon Tyne, 2003
Finestone H, Foley N, Woodbury G, Greene-Finestone L: Quantifying fluid intake in dysphagic stroke patients: a preliminary comparison of oral and nonoral strategies. Arch Phys Med Rehabil 82:1744–1746, 2001
Harvey R: The judgement of urines. J Assoc Méd Can 159:1482–1484, 1998
McCullough G: Use of surface electromyography (EMG) to treat dysphagia in adults subsequent to stroke. Roanoke, VA: Speech and Hearing Association of Virginia, 2000
Barreca S, Wolf S, Fasoli S, Bohannon R: Treatment interventions for the paretic upper limb of stroke survivors: a critical review. Neurorehabil Neural Repair 17:220–226, 2004
Acknowledgments
The authors thank the volunteers who gave up their time and supported this work.
Author information
Authors and Affiliations
Corresponding author
Additional information
Study performed at the Freeman Hospital, Newcastle upon Tyne, UK. This project was supported by the Stroke Association (grant 11/98). Presented in part at the ASHA Convention, Chicago, Illinois, 13–15 November 2003
Rights and permissions
About this article
Cite this article
Leslie, P., Drinnan, M.J., Zammit-Maempel, I. et al. Cervical Auscultation Synchronized with Images from Endoscopy Swallow Evaluations. Dysphagia 22, 290–298 (2007). https://doi.org/10.1007/s00455-007-9084-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00455-007-9084-5