Abstract
Background
In the United States, cancer is the second leading cause of mortality, and millions more battle cancer worldwide. As such, primary prevention of cancer is a major interest globally. Aspirin has been studied as a primary prevention method for multiple diseases, mainly cardiovascular disease and various forms of cancer. The role of aspirin as a primary prevention of cancer is still controversial and may be more beneficial in certain cancers over others. With rapidly surfacing large randomized controlled trials (RCTs) studying this subject, we aimed to evaluate the efficacy and safety of aspirin as a primary prophylaxis for cancer.
Methods
A comprehensive electronic database search was conducted for all RCTs that compared aspirin versus placebo for the prevention of any type of disease, and where cancer incidence or mortality was reported. The primary outcome was cancerrelated mortality. Secondary outcomes were cancer incidence, all-cause mortality, major bleeding, any bleeding and gastrointestinal (GI) bleeding. We calculated risk ratios (RRs) and 95% confidence intervals (CIs) using a random-effects model at the longest follow-up period.
Results
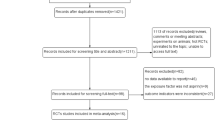
We included 16 RCTs with 104,018 total patients, mean age of 60.51 years, mean follow-up of 5.48 years, and a male percentage of 38.72%. We found that aspirin was not associated with a significant reduction of cancer-related mortality compared with placebo (RR 0.99; 95% CI: 0.87–1.12; P = 0.85: I2 = 41%). Compared with placebo, aspirin was not associated with significant reduction of all-cause mortality (RR 0.97; 95% CI: 0.92–1.02; P = 0.19; I2 = 13%) or cancer incidence (RR: 0.98; 95% CI: 0.92–1.04; P = 0.43; I2 = 16%). However, aspirin treatment was associated with significantly increased risks of any bleeding (RR 1.63; 95% CI: 1.31–2.03; P < 0.01), major bleeding (RR 1.41; 95% CI: 1.26–1.57; P < 0.01), and GI bleeding (RR 1.85; 95% CI: 1.38–2.48; P < 0.01) compared with placebo.
Conclusion
Our study did not find any significant reductions in cancer-related mortality or cancer incidence when compared aspirin use with placebo or no aspirin. Our study also highlights that the use of aspirin for primary prevention of cancer was found to cause higher rates of bleeding (any bleeding, major bleeding, and GI bleeding) compared to placebo or no aspirin at the longest follow-up period with no significant benefit in cancer primary prevention.









Similar content being viewed by others
References
Belch J, MacCuish A, Campbell I et al (2008) The prevention of progression of arterial disease and diabetes (POPADAD) trial: factorial randomised placebo controlled trial of aspirin and antioxidants in patients with diabetes and asymptomatic peripheral arterial disease. BMJ 337:a1840
Brighton TA, Eikelboom JW, Mann K et al (2012) Low-dose aspirin for preventing recurrent venous thromboembolism. N Engl J Med 367:1979–1987
Chubak J, Whitlock EP, Williams SB, Kamineni A, Burda BU, Buistand DS, Anderson ML (2016) Annals of internal medicine aspirin for the prevention of cancer incidence and mortality : systematic evidence reviews for the U.S. Preventive Services. Ann Int Med 164(12):814–825
Collaborative Group of the Primary Prevention Project (2001) Low-dose aspirin and vitamin E in people at cardiovascular risk: a randomised trial in general practice. Lancet 357:89–95
Cook NR, Lee IM, Zhang SM et al (2013) Alternate-day, low-dose aspirin and cancer risk: long-term observational follow-up of a randomized trial. Ann Intern Med 159:77–85
ETDRS Investigators (1992) Aspirin effects on mortality and morbidity in patients with diabetes mellitus. Early treatment diabetic retinopathy study report 14. JAMA 268:1292–1300
Farrell B, Godwin J, Richards S, Warlow C (1991) The United Kingdom transient ischaemic attack (UK-TIA) aspirin trial: final results. J Neurol Neurosurg Psychiatry 54:1044–1054
Fitzmaurice C et al (2017) Global Regional, and national cancer incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life-years for 32 cancer groups, 1990 to 2015 a systematic analysis for the global burden of disease study. JAMA Oncol. 98121(4):524–548
Ilbawi AM, Anderson BO (2015) Cancer in global health: how do prevention and early detection strategies relate? Global Health. 7(278):1–6
Juul-Möller S, Edvardsson N, Jahnmatz B et al (1992) Double-blind trial of aspirin in primary prevention of myocardial infarction in patients with stable chronic angina pectoris. The Swedish Angina Pectoris Aspirin Trial (SAPAT) group. Lancet 340:1421–1425
Krstic MN, Mijac DD, Popovic DD (2019) General aspects of primary cancer prevention. Dig Dis. 25:15. https://doi.org/10.1159/000497191
Ma X, Yu H (2006) Global burden of cancer. Yale J Biol Med 79:85–94
McNeil JJ, Nelson MR, Woods RL, Lockery JE et al (2018) Effect of aspirin on all-cause mortality in the healthy elderly. N Engl J Med 379(16):1519–1528
Medical Research Council's General Practice Research Framework (1998) Thrombosis prevention trial: randomised trial of low-intensity oral anticoagulation with warfarin and low-dose aspirin in the primary prevention of ischemic heart disease in men at increased risk. Lancet 351:233–241
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M et al (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev 4:1–9
Ogawa H, Nakayama M, Morimoto T et al (2008) Low-dose aspirin for primary prevention of atherosclerotic events in patients with type 2 diabetes: a randomized controlled trial. JAMA 300:2134–2142
Okada S, Morimoto T, Ogawa H, Sakuma M et al (2018) Effect of aspirin on cancer chemoprevention in japanese patients with type 2 diabetes : 10-year observational follow-up of a randomized controlled trial. Diabetes Care. 41:1757–1764
Rothwell PM, Fowkes FGR, Belch JFF, Ogawa H, Warlow CP, Meade TW (2011) Effect of daily aspirin on long-term risk of death due to cancer: analysis of individual patient data from randomised trials. The Lancet 377(9759):31–41
Seshasai SRK, Wijesuriya S, Sivakumaran R, Nethercott S, Erqou S, Sattar N, Ray KK (2012) Effect of aspirin on vascular and nonvascular outcomes. Arch Intern Med. 172(3):209–216
Stegeman I, Bossuyt PM, Yu T, Boyd C, Puhan MA (2015) Aspirin for primary prevention of cardiovascular disease and cancer, a benefit and harm analysis. Plos One. 2:1–12
The ASCEND study collaborative group (2018) Effects of aspirin for primary prevention in persons with diabetes mellitus. N Engl J Med 379(16):1529–1539
The DAMAD Study Group (1989) Effect of aspirin alone and aspirin plus dipyridamole in early diabetic retinopathy. A multicenter randomized controlled clinical trial. Diabetes 38:491–498
The Persantine-Aspirin Reinfarction Study Research Group (1980) Persantine and aspirin in coronary heart disease. Circulation 62:449–461
The SALT Collaborative Group (1991) Swedish aspirin low-dose trial (SALT) of 75 mg aspirin as secondary prophylaxis after cerebrovascular ischaemic events. Lancet 338:1345–1349
Tsoi KKF et al (2019) Long-term use of low-dose aspirin for cancer prevention : a 10-year population cohort study in Hong Kong. Int J Cancer
Vane JR, Meade TW (1997) Second European Stroke Prevention Study (ESPS 2): clinical and pharmacological implications. J Neurol Sci 145(2):123–125
Whitlock EP, Williams SB, Burda BU, Feightner A, Beil T (2015) Aspirin use in adults: cancer, all-cause mortality, and harms. A Systematic Evidence Review for the U.S. Preventive Services Task Force. Evidence Synthesis No. 132. AHRQ Publication No. 13-05193-EF-1. Rockville, MD: Agency for Healthcare Research and Quality
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Haykal, T., Barbarawi, M., Zayed, Y. et al. Safety and efficacy of aspirin for primary prevention of cancer: a meta-analysis of randomized controlled trials. J Cancer Res Clin Oncol 145, 1795–1809 (2019). https://doi.org/10.1007/s00432-019-02932-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-019-02932-0