Abstract
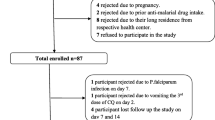
A rising incidence of imported acute malaria has been observed in non-immune traveller children returning from the tropics to France. Halofantrine efficacy has been poorly assessed in non-immune children. In order to assess halofantrine efficacy in non-immune children with acute uncomplicated Plasmodium falciparum malaria, we collected data of children with positive blood smears in an open prospective study. Children with neurological manifestations, vomiting and congenital long QT were excluded. All children were hospitalised and received halofantrine (24 mg/kg divided into three doses per day) on an empty stomach. Persistent fever after day 3 defined failure. Relapse was defined by a positive blood smear with or without systemic symptoms within a 1 month follow-up period. In total, 52 children were enrolled. No failure was observed, but relapses occurred in 14/52. On univariate analysis, the mean age of children with relapse was significantly lower (P<0.05). Moreover, diarrhoea was more frequently associated with relapses (P<0.04). Age and diarrhoea were significant independent factors contributing to relapses. Conclusion:this study shows that with a relapse rate of 27%, this regimen with a 1-day course of halofantrine is not to be recommended.
Similar content being viewed by others
References
Angles A, Bagheri H, Montastruc JL, Magnaval JF Le Réseau Français des Centres Régionaux de Pharmacovigilance (2003) Adverse drug reactions (ADRs) to antimalarial drugs. Analysis of spontaneous report from the French pharmacovigilance database (1996–2000). Presse Med 32: 106–113
Castot A, Rapoport P, LeCoz P (1993) Prolonged QT interval with halofantrine. Lancet 341: 1541
Conférence de Consensus (1999) Prise en charge et prévention du paludisme d’importation à Plasmodium falciparum. Bull Epidemiol Hebd 38: 157–161
Coulaud JP, LeBras J, Matheron S, Morinière B, Saimot AG, Rossignol JF (1986) Treatment of imported cases of falciparum malaria in France with halofantrine. Trans R Soc Trop Med Hyg 80: 615–616
Karbwang J, Milton KA, Bangchang K, Ward SA, Edwards G, Bunnag D (1991) Pharmacodynamics of halofantrine in Thai patients with acute complicated falciparum malaria. Br J Clin Pharmacol 31: 484–487
Legros F, Fromage M, Ancelle T, Burg E, Janot C, Maisonneuve P, Danis M (1999) Enquête nationale de recensement des cas de paludisme d’importation en France métropolitaine pour l’année 1997. Bull Epidemiol Hebd 11: 41–42
Piarroux R, Dumon H, Garnier JM, Lehmann M, Unal D, Quilici M (1993) Choice of therapy for imported cases of falciparum malaria in children: a retrospective study of 100 cases seen in Marseille, France. Trans R Soc Trop Med Hyg 87: 72–74
Ter Kuile FO, Dolan G, Nosten F, Edstein MD, Luxemburger C, Phaipun L, Chongsuphajaisiddhi T, Webster HK, White NJ (1993) Halofantrine versus mefloquine in treatment of multidrug-resistant falciparum malaria. Lancet 341: 1044–1049
Touze JE, Bernard J, Keundjian A, Imbert P, Viguier A, Chaudet H, Doury JC (1996) Electrocardiographic changes and halofantrine plasma level during acute falciparum malaria. Am J Trop Med Hyg 54: 255–258
Touze JE, Perret JL, Nicolas X, Fourcade L, Bernard J, Keundjian A, Doares JM, Doury JC (1997) Efficacy of low dose halofantrine for second treatment of uncomplicated falciparum malaria. Lancet 349: 255–256
Watkins WM, Oloo JA, Lury JD, Mosoba M, Kariuki D, Mjomba M, Koech DK, Gilles HM (1988) Efficacy of multiple-dose halofantrine in treatment of chloroquine-resistant falciparum malaria in children in Kenya. Lancet 2: 247–250
Weinke T, Loscher T, Fleischer K, Kretschmer H, Pohle HD, Kohler B, Schlunk T, Clemens R, Bock HL (1992) The efficacy of halofantrine in the treatment of acute malaria in nonimmune travellers. Am J Trop Med Hyg 47: 1–5
Wirima J, Khoromana C, Molyneux ME, Gilles HM (1988) Clinical trials with halofantrine hydrochloride in Malawi. Lancet 2: 250–252
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hau, I., Seringe, S., Aberrane, S. et al. Halofantrine efficacy in non-immune children with imported acute Plasmodium falciparum malaria Infection. Eur J Pediatr 163, 22–24 (2004). https://doi.org/10.1007/s00431-003-1316-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-003-1316-6