Abstract
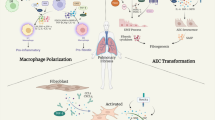
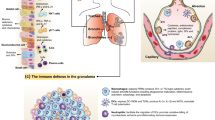
Oxygen tension affects local immune responses in inflammation and infection. In tuberculosis mycobacteria avoid hypoxic areas and preferentially persist and reactivate in the oxygen-rich apex of the lung. Oxygen restriction activates antimicrobial effector mechanisms in macrophages and restricts growth of intracellular Mycobacterium tuberculosis (M.Tb). The effect of oxygen restriction on T cell-mediated antimicrobial effector mechanisms is unknown. Therefore we determined the influence of hypoxia on the expression of granulysin, an antimicrobial peptide of lymphocytes. Hypoxia increased the antigen-specific up-regulation of granulysin mRNA and protein in human CD4+ and CD8+ T lymphocytes. This observation was functionally relevant, because oxygen restriction supported the growth-limiting effect of antigen-specific T cells against virulent M.Tb residing in primary human macrophages. Our results provide evidence that oxygen restriction promotes the expression of granulysin and suggest that this effect—in conjunction with additional T cell-mediated immune responses—supports protection against mycobacteria. The therapeutic modulation of oxygen availability may offer a new strategy for the host-directed therapy of infectious diseases with intracellular pathogens.







Similar content being viewed by others
References
McNamee EN, Korns Johnson D, Homann D, Clambey ET (2013) Hypoxia and hypoxia-inducible factors as regulators of T cell development, differentiation, and function. Immunol Res 55:58–70. doi:10.1007/s12026-012-8349-8
Leach RM, Treacher DF (1998) Oxygen transport-2. Tissue hypoxia. BMJ 317:1370–1373. doi:10.1136/bmj.317.7169.1370
Braun RD, Lanzen JL, Snyder SA, Dewhirst MW (2001) Comparison of tumor and normal tissue oxygen tension measurements using OxyLite or microelectrodes in rodents. Am J Physiol Heart Circ Physiol 280:H2533–H2544
Caldwell CC, Kojima H, Lukashev D, Armstrong J, Farber M, Apasov SG, Sitkovsky MV (2001) Differential effects of physiologically relevant hypoxic conditions on T lymphocyte development and effector functions. J Immunol 167:6140–6149. doi:10.4049/jimmunol.167.11.6140
Wang GL, Jiang BH, Rue EA, Semenza GL (1995) Hypoxia-inducible factor 1 is a basic-helix-loop-helix-PAS heterodimer regulated by cellular O2 tension. Proc Natl Acad Sci USA 92:5510–5514
Higashiyama M, Hokari R, Hozumi H, Kurihara C, Ueda T, Watanabe C, Tomita K, Nakamura M, Komoto S, Okada Y, Kawaguchi A, Nagao S, Suematsu M, Goda N, Miura S (2012) HIF-1 in T cells ameliorated dextran sodium sulfate-induced murine colitis. J Leukoc Biol 91:901–909. doi:10.1189/jlb.1011518
Gaber T, Häupl T, Sandig G, Tykwinska K, Fangradt M, Tschirschmann M, Hahne M, Dziurla R, Erekul K, Lautenbach M, Kolar P, Burmester GR, Buttgereit F (2009) Adaptation of human CD4+ T cells to pathophysiological hypoxia: a transcriptome analysis. J Rheumatol 36:2655–2669. doi:10.3899/jrheum.090255
Fitzgerald LE, Abendaño N, Juste RA, Alonso-Hearn M (2014) Threedimensional in vitro models of granuloma to study bacteria-host interactions, drug-susceptibility, and resuscitation of dormant mycobacteria. BioMed Res Int 2014:623856. doi:10.1155/2014/623856
Rich AR, Follis RH (1942) The effect of low oxygen tension upon the development of experimental tuberculosis. Bull Johns Hopkins Hosp 71:345–363
Olender S, Saito M, Apgar J, Gillenwater K, Bautista CT, Lescano AG, Moro P, Caviedes L, Hsieh EJ, Gilman RH (2003) Low prevalence and increased household clustering of Mycobacterium tuberculosis infection in high altitude villages in Peru. Am J Trop Med Hyg 68:721–727
Nickel D, Busch M, Mayer D, Hagemann B, Knoll V, Stenger S (2012) Hypoxia triggers the expression of human beta defensin 2 and antimicrobial activity against Mycobacterium tuberculosis in human macrophages. J Immunol 188:4001–4007. doi:10.4049/jimmunol.1100976
Oehlers SH, Cronan MR, Scott NR, Thomas MI, Okuda KS, Walton EM, Beerman RW, Crosier PS, Tobin DM (2015) Interception of host angiogenic signalling limits mycobacterial growth. Nature 517:612–615. doi:10.1038/nature13967
Gautam US, Mehra S, Ahsan MH, Alvarez X, Niu T, Kaushal D (2014) Role of TNF in the altered interaction of dormant Mycobacterium tuberculosis with host macrophages. PLoS One 9:e95220. doi:10.1371/journal.pone.0095220
Duque-Correa MA, Kühl AA, Rodriguez PC, Zedler U, Schommer-Leitner S, Rao M, Weiner J 3rd, Hurwitz R, Qualls JE, Kosmiadi GA, Murray PJ, Kaufmann SH, Reece ST (2014) Macrophage arginase-1 controls bacterial growth and pathology in hypoxic tuberculosis granulomas. Proc Natl Acad Sci USA 111:E4024–E4032. doi:10.1073/pnas.1408839111
Srivastava S, Ernst JD, Desvignes L (2014) Beyond macrophages: the diversity of mononuclear cells in tuberculosis. Immunol Rev 262:179–192. doi:10.1111/imr.12217
Stenger S, Rosat JP, Bloom BR, Krensky AM, Modlin RL (1999) Granulysin: a lethal weapon of cytolytic T cells. Immunol Today 20:390–394. doi:10.1016/S0167-5699(99)01449-8
Clayberger C, Krensky AM (2003) Granulysin. Curr Opin Immunol 15:560–565. doi:10.1016/S0952-7915(03)00097-9
Narni-Mancinelli E, Vivier E (2014) Delivering three punches to knockout intracellular bacteria. Cell 157:1251–1252. doi:10.1016/j.cell.2014.05.023
Stenger S, Hanson DA, Teitelbaum R, Dewan P, Niazi KR, Froelich CJ, Ganz T, Thoma-Uszynski S, Melián A, Bogdan C, Porcelli SA, Bloom BR, Krensky AM, Modlin RL (1998) An antimicrobial activity of cytolytic T cells mediated by granulysin. Science 282:121–125
Walch M, Dotiwala F, Mulik S, Thiery J, Kirchhausen T, Clayberger C, Krensky AM, Martinvalet D, Lieberman J (2014) Cytotoxic cells kill intracellular bacteria through granulysin-mediated delivery of granzymes. Cell 157:1309–1323. doi:10.1016/j.cell.2014.03.062
Krensky AM, Clayberger C (2009) Biology and clinical relevance of granulysin. Tissue Antigens 73:193–198. doi:10.1111/j.1399-0039.2008.01218.x
Ernst WA, Thoma-Uszynski S, Teitelbaum R, Ko C, Hanson DA, Clayberger C, Krensky AM, Leippe M, Bloom BR, Ganz T, Modlin RL (2000) Granulysin, a T cell product, kills bacteria by altering membrane permeability. J Immunol 165:7102–7108. doi:10.4049/jimmunol.165.12.7102
Deng A, Chen S, Li Q, Lyu SC, Clayberger C, Krensky AM (2005) Granulysin, a cytolytic molecule, is also a chemoattractant and proinflammatory activator. J Immunol 174:5243–5248. doi:10.4049/jimmunol.174.9.5243
Di Liberto D, Buccheri S, Caccamo N, Meraviglia S, Romano A, Di Carlo P, Titone L, Dieli F, Krensky AM, Salerno A (2007) Decreased serum granulysin levels in childhood tuberculosis which reverse after therapy. Tuberculosis (Edinb) 87:322–328. doi:10.1016/j.tube.2007.01.003
Mueller H, Faé KC, Magdorf K, Ganoza CA, Wahn U, Guhlich U, Feiterna-Sperling C, Kaufmann SH (2011) Granulysin-expressing CD4+ T cells as candidate immune marker for tuberculosis during childhood and adolescence. PLoS One 6:e29367. doi:10.1371/journal.pone.0029367
Ochoa MT, Stenger S, Sieling PA, Thoma-Uszynski S, Sabet S, Cho S, Krensky AM, Röllinghoff M, Nunes Sarno E, Burdick AE, Rea TH, Modlin RL (2001) T cell release of granulysin contributes to host defense in leprosy. Nat Med 7:174–179. doi:10.1038/84620
Rahman S, Gudetta B, Fink J, Granath A, Ashenafi S, Aseffa A, Derbew M, Svensson M, Andersson J, Brighenti SG (2009) Compartmentalization of immune responses in human tuberculosis: few CD8+ effector T cells but elevated levels of FoxP3+ regulatory t cells in the granulomatous lesions. Am J Pathol 174:2211–2224. doi:10.2353/ajpath.2009.080941
Rahman S, Magalhaes I, Rahman J, Ahmed RK, Sizemore DR, Scanga CA, Weichold F, Verreck F, Kondova I, Sadoff J, Thorstensson R, Spångberg M, Svensson M, Andersson J, Maeurer M, Brighenti S (2012) Prime-boost vaccination with rBCG/rAd35 enhances CD8(+) cytolytic T-cell responses in lesions from Mycobacterium tuberculosis-infected primates. Mol Med 18:647–658. doi:10.2119/molmed.2011.00222
Bastian M, Braun T, Bruns H, Röllinghoff M, Stenger S (2008) Mycobacterial lipopeptides elicit CD4 + CTLs in Mycobacterium tuberculosis-infected humans. J Immunol 180:3436–3446. doi:10.4049/jimmunol.180.5.3436
Monney L, Sabatos CA, Gaglia JL, Ryu A, Waldner H, Chernova T, Manning S, Greenfield EA, Coyle AJ, Sobel RA, Freeman GJ, Kuchroo VK (2002) Th1-specific cell surface protein Tim-3 regulates macrophage activation and severity of an autoimmune disease. Nature 415:536–541. doi:10.1038/415536a
Rustad TR, Harrell MI, Liao R, Sherman DR (2008) The enduring hypoxic response of Mycobacterium tuberculosis. PLoS One 3:e1502. doi:10.1371/journal.pone.0001502
Galagan JE, Minch K, Peterson M, Lyubetskaya A, Azizi E, Sweet L, Gomes A, Rustad T, Dolganov G, Glotova I, Abeel T, Mahwinney C, Kennedy AD, Allard R, Brabant W, Krueger A, Jaini S, Honda B, Yu WH, Hickey MJ, Zucker J, Garay C, Weiner B, Sisk P, Stolte C, Winkler JK, Van de Peer Y, Iazzetti P, Camacho D, Dreyfuss J, Liu Y, Dorhoi A, Mollenkopf HJ, Drogaris P, Lamontagne J, Zhou Y, Piquenot J, Park ST, Raman S, Kaufmann SH, Mohney RP, Chelsky D, Moody DB, Sherman DR, Schoolnik GK (2013) The Mycobacterium tuberculosis regulatory network and hypoxia. Nature 499:178–183. doi:10.1038/nature12337
Mehra S, Foreman TW, Didier PJ, Ahsan MH, Hudock TA, Kissee R, Golden NA, Gautam US, Johnson AM, Alvarez X, Russell-Lodrigue KE, Doyle LA, Roy CJ, Niu T, Blanchard JL, Khader SA, Lackner AA, Sherman DR, Kaushal D (2015) The DosR regulon modulates adaptive immunity and is essential for M. tuberculosis persistence. Am J Respir Crit Care Med 191:1185–1196. doi:10.1164/rccm.201408-1502OC
Murdoch C, Muthana M, Lewis CE (2005) Hypoxia regulates macrophage functions in inflammation. J Immunol 175:6257–6263. doi:10.4049/jimmunol.175.10.6257
Eltzschig HK, Carmeliet P (2011) Hypoxia and inflammation. New Engl J Med 364:656–665. doi:10.1056/NEJMra0910283
Schaffer K, Taylor CT (2015) The impact of hypoxia on bacterial infection. FEBS J 282:2260–2266. doi:10.1111/febs.13270
Ottenhoff TH (2012) New pathways of protective and pathological host defense to mycobacteria. Trends Microbiol 20:419–428. doi:10.1016/j.tim.2012.06.002
Palazon A, Goldrath AW, Nizet V, Johnson RS (2014) HIF transcription factors, inflammation, and immunity. Immunity 41:518–528. doi:10.1016/j.immuni.2014.09.008
Peyssonnaux C, Boutin AT, Zinkernagel AS, Datta V, Nizet V, Johnson RS (2008) Critical role of HIF-1alpha in keratinocyte defense against bacterial infection. J Invest Dermatol 128:1964–1968. doi:10.1038/jid.2008.27
Peyssonnaux C, Datta V, Cramer T, Doedens A, Theodorakis EA, Gallo RL, Hurtado-Ziola N, Nizet V, Johnson RS (2005) HIF-1alpha expression regulates the bactericidal capacity of phagocytes. J Clin Invest 115:1806–1815. doi:10.1172/JCI23865
Berger EA, McClellan SA, Vistisen KS, Hazlett LD (2013) HIF-1alpha is essential for effective PMN bacterial killing, antimicrobial peptide production and apoptosis in Pseudomonas aeruginosa keratitis. PLoS Pathog 9:e1003457. doi:10.1371/journal.ppat.1003457
Zinkernagel AS, Peyssonnaux C, Johnson RS, Nizet V (2008) Pharmacologic augmentation of hypoxia-inducible factor-1alpha with mimosine boosts the bactericidal capacity of phagocytes. J Infect Dis 197:214–217. doi:10.1086/524843
Elks PM, Brizee S, van der Vaart M, Walmsley SR, van Eeden FJ, Renshaw SA, Meijer AH (2013) Hypoxia inducible factor signaling modulates susceptibility to mycobacterial infection via a nitric oxide dependent mechanism. PLoS Pathog 9:e1003789. doi:10.1371/journal.ppat.1003789
Shalova IN, Lim JY, Chittezhath M, Zinkernagel AS, Beasley F, Hernández-Jiménez E, Toledano V, Cubillos-Zapata C, Rapisarda A, Chen J, Duan K, Yang H, Poidinger M, Melillo G, Nizet V, Arnalich F, López-Collazo E, Biswas SK (2015) Human monocytes undergo functional re-programming during sepsis mediated by hypoxia-inducible factor-1α. Immunity 42:484–498. doi:10.1016/j.immuni.2015.02.001
Doedens AL, Phan AT, Stradner MH, Fujimoto JK, Nguyen JV, Yang E, Johnson RS, Goldrath AW (2013) Hypoxia-inducible factors enhance the effector responses of CD8(+) T cells to persistent antigen. Nat Immunol 14:1173–1182. doi:10.1038/ni.2714
Zhao S, Wu J (2013) Hypoxia inducible factor stabilization as a novel strategy to treat anemia. Curr Med Chem 20:2697–2711. doi:10.2174/0929867311320210006
Bhandari T, Nizet V (2014) Hypoxia-Inducible Factor (HIF) as a pharmacological target for prevention and treatment of infectious diseases. Infect Dis Therapy 3:159–174. doi:10.1007/s40121-014-0030-1
Acknowledgments
We acknowledge the excellent technical support of Daniel Mayer and Mark Grieshober and the support of the Institute for Transfusion Medicine, University Hospital Ulm for supplying buffy coat preparations. We appreciate fruitful discussions with Prof. Robert L. Modlin, UCLA, Los Angeles. This work was funded by the European Union (TBVAC2020 consortium). S.K. was supported by a doctoral fellowship by the Land-Baden-Württemberg (“Kooperative Promotionskolleg Phamazeutische Biotechnologie der Hochschule Biberach und der Universität Ulm”) and the International Graduate School in Molecular Medicine Ulm. J.K. was supported by a fellowship of the graduate school “Experimentelle Medizin der Universität Ulm.”
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interests
The authors declare that they have no conflict of interest.
Ethical statement
This article does not contain any studies with human participants or animals performed by any of the authors. Human peripheral blood mononuclear cells (PBMC) were isolated by density gradient centrifugation of buffy coat preparations from anonymous donors (Institute of Transfusion Medicine, Ulm University).
Rights and permissions
About this article
Cite this article
Zenk, S.F., Vollmer, M., Schercher, E. et al. Hypoxia promotes Mycobacterium tuberculosis-specific up-regulation of granulysin in human T cells. Med Microbiol Immunol 205, 219–229 (2016). https://doi.org/10.1007/s00430-015-0442-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00430-015-0442-x