Abstract
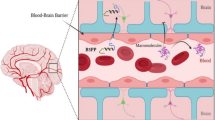
Peptides are able to cross the blood–brain barrier (BBB) through various mechanisms, opening new diagnostic and therapeutic avenues. However, their BBB transport data are scattered in the literature over different disciplines, using different methodologies reporting different influx or efflux aspects. Therefore, a comprehensive BBB peptide database (Brainpeps) was constructed to collect the BBB data available in the literature. Brainpeps currently contains BBB transport information with positive as well as negative results. The database is a useful tool to prioritize peptide choices for evaluating different BBB responses or studying quantitative structure–property (BBB behaviour) relationships of peptides. Because a multitude of methods have been used to assess the BBB behaviour of compounds, we classified these methods and their responses. Moreover, the relationships between the different BBB transport methods have been clarified and visualized.



Similar content being viewed by others
Abbreviations
- %ID:
-
Percentage injected dose
- γ :
-
Surface tension
- γ 0 :
-
Surface tension in pure buffer solution
- ε :
-
Dielectric constant
- λ :
-
Terminal rate constant
- π :
-
Surface pressure
- Г:
-
Surface excess concentration
- Г∞ :
-
Limited surface excess concentration
- A :
-
Area of the filter, membrane surface area, capillary surface area
- ABC transporter:
-
ATP-binding cassette transporter
- A D :
-
Surface area of the test compound at the air–water interface
- A m :
-
Amount of test compound in brain
- A s :
-
Cross-sectional area; surface area
- ATP:
-
Adenosine triphosphate
- AUC:
-
Area under the concentration curve
- AUCbrain :
-
Area under the concentration curve in brain
- AUCplasma :
-
Area under the concentration curve in plasma
- BB:
-
Brain-to-plasma concentration ratio at steady-state, blood–brain equilibrium distribution
- BBB:
-
Blood–brain barrier
- BBB-PI:
-
Blood–brain barrier permeability index
- BCRP:
-
Breast cancer resistance protein
- BCSFB:
-
Blood–cerebrospinal fluid barrier
- BEI:
-
Brain efflux index
- BMEC:
-
Brain microvessel endothelial cells
- B/P :
-
Brain-to-plasma concentration ratio at steady-state, blood–brain equilibrium distribution
- Brainpeps:
-
Blood–brain barrier peptide database
- BSA:
-
Bovine serum albumin
- BUI:
-
Brain uptake index
- BW:
-
Body weight
- C :
-
Concentration of test compound
- C 0 :
-
Initial concentration in donor chamber; minimum concentration to induce surface activity
- C a, C A, C acc :
-
Apical (luminal) side concentration, i.e. in the acceptor chamber
- Caco-2:
-
Human colon carcinoma cell line
- Calcein-AM:
-
Calcein acetoxymethyl ester
- CBF:
-
Cerebral blood flow
- C br, C brain :
-
Brain concentration
- C br,tot, C br (total):
-
Total brain concentration
- C buffer :
-
Concentration in buffer
- C CSF :
-
Concentration in the CSF
- CD:
-
Compartmental distribution
- C donor, C d, C D, C DO, C I :
-
Initial concentration of test compound in donor chamber
- C dial :
-
Concentration of the dialysate
- C ECF :
-
Concentration of test compound in brain ECF
- C in :
-
Concentration of the perfusate; concentration in the carotid injection solution
- C iv :
-
Concentration of intravascular marker
- Cl:
-
Clearance
- Cleff :
-
Efflux clearance
- ClH :
-
Hepatic clearance
- Clinf :
-
Uptake clearance
- Clp :
-
Systemic clearance
- ClR :
-
Renal clearance
- ClS :
-
Systemic clearance
- Cltest :
-
Clearance of the test experiment
- Clup :
-
Initial uptake clearance
- CMC:
-
Critical micelle concentration
- CNS:
-
Central nervous system
- CNS− :
-
Low brain penetrator
- CNS+ :
-
High brain penetrator
- Conc(test/ref)brain :
-
Concentration ratio of test and reference compound in brain
- Conc(test/ref)injectate :
-
Concentration ratio of test and reference compound in injection solution
- C org :
-
Concentration test compound in organic phase
- C out, C dial :
-
Concentration of the dialysate
- C p (t):
-
Plasma concentration at time t
- C pa :
-
Arterial plasma concentration
- C perfusion, C perf :
-
Concentration in the perfusion solution
- C pl :
-
Plasma concentration
- C pl,tot :
-
Total plasma concentration
- C ref :
-
Concentration of the reference compound
- C ref,brain :
-
Concentration of the reference compound in the brain
- C ref,inj :
-
Concentration of the reference compound in the injected solutions
- C s :
-
Concentration of the sample
- C sat :
-
Saturated concentration at which the surface pressure collapses
- CSF:
-
Cerebrospinal fluid
- C slice :
-
Free drug concentration in tissue slice
- C test :
-
Concentration of the test compound
- C test,brain :
-
Concentration of the test compound in the brain
- C test,inj :
-
Concentration of the test compound in the injected solutions
- C tissue :
-
Tissue concentration of the indicator
- C tot :
-
Total concentration
- C u :
-
Unbound concentration
- C u,brain :
-
Unbound concentration in brain
- C u,plasma :
-
Unbound concentration in plasma
- C wat :
-
Concentration test compound in aqueous phase
- C wat,ion :
-
Concentration of ionic species of test compound in aqueous phase
- C wat,neut :
-
Concentration of neutral species of test compound in aqueous phase
- D :
-
Distribution coefficient; dilution factor
- dQ/dt :
-
Transport rate of test compound
- E :
-
Extraction of the test compound
- ECF:
-
Extracellular fluid
- ED50 :
-
Dose producing 50% of the maximum response
- EDTA:
-
Ethylenediaminetetraacetic acid
- ER:
-
Efflux ratio; entity-relationship
- E ref :
-
Single pass extraction of the reference compound
- E refp :
-
Extraction of the permeable marker
- E refv :
-
Extraction of the vascular impermeable marker
- E test :
-
Single pass extraction of the test compound
- Exp.t :
-
Exposure time
- F :
-
Regional flow rate
- f :
-
Fraction of plasma exchangeable compound
- FK:
-
Foreign key
- f u :
-
Unbound fraction
- f u,brain :
-
Unbound fraction in brain
- f u,dil :
-
Diluted unbound fraction
- f u,meas :
-
Free fraction measured
- f u,plasma :
-
Unbound fraction in plasma
- GFR:
-
Glomerular filtration rate
- GLUT-1:
-
Glucose transporter 1
- hAAG:
-
Human α1 acid glycoprotein
- HPLC:
-
High-performance liquid chromatography
- IAM:
-
Immobilized artificial membrane
- IUPAC:
-
International Union of Pure and Applied Chemistry
- J :
-
Brain uptake rate
- J max :
-
Maximal flux
- K aw :
-
Air–water partition coefficient
- K d :
-
Dissociation constant
- k eff :
-
Apparent efflux rate constant
- k el :
-
Plasma elimination rate constant
- k el :
-
Efflux rate constant
- k i :
-
Unidirectional influx rate constant determined with imaging techniques
- k IAM :
-
IAM capacity factor
- K in :
-
Unidirectional influx rate constant
- K m :
-
Michaelis–Menten constant
- k out :
-
Brain elimination rate constant
- K p :
-
Brain-to-plasma partition coefficient
- K p,app :
-
Apparent brain-to-plasma partition coefficient
- K p,brain :
-
Brain-to-plasma concentration ratio
- K p,in :
-
Intrinsic plasma-to-brain partition coefficient
- K p,uu :
-
Brain-to-plasma partition coefficient of the free compound concentration
- LAT-1:
-
Large neutral amino acid transporter-1
- Log P cyclohexane/water :
-
Log P value of the cyclohexane/water system
- Log P oct/water :
-
Log P value of the 1-octanol/water system
- MBUA:
-
Mouse brain uptake assay
- MCT:
-
Monocarboxylic transporters
- MDCK:
-
Madin–Darby canine kidney cells
- MDR-1:
-
Multidrug resistance gene
- MID:
-
Method identification
- MRI:
-
Magnetic resonance imaging
- MRP-1:
-
Multidrug resistance associated protein-1
- N A :
-
Avogadro constant
- N serum :
-
Radioactivity measured per volume serum
- N tissue :
-
Radioactivity measured per gram tissue
- OID:
-
Origin identification
- P :
-
Partition coefficient; permeability coefficient
- PAMPA:
-
Parallel artificial membrane permeation assay
- P app :
-
Apparent permeability coefficient, determined with BMEC, co-culture, immortalized cell lines, Caco-2, MDCK and MBUA
- P app (A–B):
-
Apparent permeability coefficient from apical to basolateral side
- P app (B–A):
-
Apparent permeability coefficient from basolateral to apical side
- P app,pampa :
-
Apparent permeability coefficient, determined with PAMPA
- Par-2:
-
Brain parietal cortex area 2
- PBID:
-
Publication identification
- P c :
-
Intrinsic carrier-mediated permeability
- \( P_{\text{c}}^{\prime } \) :
-
Apparent net carrier-mediated permeability
- P e :
-
Endothelial permeability, effective PAMPA permeability
- P eff :
-
Effective PAMPA permeability
- P endoth :
-
Endothelial permeability coefficient, determined with BMEC culture
- PEPT1:
-
Peptide transporter 1
- PET:
-
Positron emission tomography
- P filter :
-
Permeability of the filter
- Pgp:
-
P-glycoprotein
- PI:
-
Permeability index
- PID:
-
Peptide IDentification
- P m :
-
Monolayer permeability determined with BMEC
- P p :
-
Passive diffusive permeability
- PR:
-
Peak response
- PS :
-
Permeability–surface area coefficient
- PS e :
-
PS product for the endothelial cell monolayer
- PS f :
-
PS product of the control filter
- PS t :
-
Total PS product
- P total :
-
Total permeability
- Q :
-
Cerebral blood flow
- \( \dot{Q} \) :
-
Rate of blood flow
- QAR:
-
Quantitative autoradiography
- R :
-
Gas constant; recovery
- Rateeff :
-
In vitro efflux rate
- RBE4:
-
Immortalized primary rat brain endothelial cells
- R dial :
-
Recovery by gain
- RID:
-
Response identification
- RL:
-
Recovery by loss, retrodialysis
- RP-HPLC:
-
Reversed-phase HPLC
- RR:
-
Relative recovery
- S :
-
Capillary surface area
- SMILES:
-
Simplified molecular input line entry specification
- SPECT:
-
Single photon emission tomography
- SV40:
-
Simian vacuolating virus 40
- T :
-
Temperature; perfusion time
- t :
-
Time
- t 0 :
-
Dead time
- t 1/2 :
-
(Terminal) half-life
- t 1/2eq :
-
Equilibration half-life
- t 1/2eq,in :
-
Intrinsic equilibration half-life
- T :
-
Perfusion time
- TEER:
-
Transendothelial electrical resistance
- TM-BBB:
-
Transfected mouse endothelial cells
- t r :
-
Retention time of test compound
- TR-BBB:
-
Transfected rat endothelial cells
- UML:
-
Unified modelling language
- V 0 :
-
Initial distribution volume; plasma distribution volume of marker
- V acc, V A :
-
Volume of the acceptor compartment
- V br, V b :
-
Distribution volume in brain
- V D :
-
Volume of donor compartment; distribution volume in brain
- V e :
-
Volume fraction of brain
- V i :
-
Initial distribution volume; Volume of buffer film remaining around sample slice
- V max :
-
Maximum uptake rate
- V p :
-
Plasma distribution volume
- V R :
-
Volume of acceptor compartment
- V u,br :
-
Unbound brain distribution volume
- V v :
-
Brain vascular volume
- X :
-
Amount of test compound in acceptor compartment
References
Alavijeh MS, Chishty M, Qaiser MZ, Palmer AM (2005) Drug metabolism and pharmacokinetics, the blood–brain barrier, and central nervous system drug discovery. NeuroRx 2:554–571
Albensi BC, Knoblach SM, Chew BGM, O’Reilly MP, Faden AI, Pekar JJ (2000) Diffusion and high resolution MRI of traumatic brain injury in rats: time course and correlation with histology. Exp Neurol 162:61–72
Audus KL, Rose JM, Wang W, Borchardt RT (1999) Brain microvessel endothelial cell culture systems. In: Pardridge WM (ed) Introduction to the blood–brain barrier: methodology, biology and pathology. Cambridge University Press, Cambridge, pp 86–93
Banks WA (2008) Delivery of peptides to the brain: emphasis on therapeutic development. Biopolymers 90:589–594
Banks WA, Kastin AJ (1985) Peptides and the blood–brain-barrier—lipophilicity as a predictor of permeability. Brain Res Bull 15:287–292
Banks WA, Kastin AJ (1990) Peptide-transport systems for opiates across the blood–brain-barrier. Am J Physiol 259:E1–E10
Banks WA, Kastin AJ (1996) Passage of peptides across the blood–brain barrier: pathophysiological perspectives. Life Sci 59:1923–1943
Banks WA, Kastin AJ, Coy DH (1984) Evidence that [125I]N-Tyr-delta sleep-inducing peptide crosses the blood–brain barrier by a non-competitive mechanism. Brain Res 301:201–207
Banks WA, Kastin AJ, Conn PM (1989) Quantifying carrier-mediated transport of peptides from the brain to the blood. Method Enzymol 168:652–660
Banks WA, Tschop M, Robinson SM, Heiman ML (2002) Extent and direction of ghrelin transport across the blood–brain barrier is determined by its unique primary structure. J Pharmacol Exp Ther 302:822–827
Becker S, Liu XR (2006) Evaluation of the utility of brain slice methods to study brain penetration. Drug Metab Dispos 34:855–861
Beekman FJ, Vastenhouw B (2004) Design and simulation of a high-resolution stationary SPECT system for small animals. Phys Med Biol 49:4579–4592
Begley DJ (1999) In situ brain perfusion. In: Pardridge WM (ed) Introduction to the blood–brain barrier: methodology, biology and pathology. Cambridge University Press, Cambridge, pp 32–40
Berezhkovskiy LM (2008) Some features of the kinetics and equilibrium of drug binding to plasma proteins. Expert Opin Drug Metab Toxicol 4:1479–1498
Bickel U (1999) Intravenous injection/pharmacokinetics. In: Pardridge WM (ed) Introduction to the blood–brain barrier: methodology, biology and pathology. Cambridge University Press, Cambridge, pp 41–48
Bickel U (2005) How to measure drug transport across the blood–brain barrier. NeuroRx 2:15–26
Bickel U, Yoshikawa T, Pardridge WM (2001) Delivery of peptides and proteins through the blood–brain barrier. Adv Drug Deliv Rev 46:247–279
Bonate PL (1995) Animal-models for studying transport across the blood–brain-barrier. J Neurosci Methods 56:1–15
Booch G, Rumbaugh J, Jacobson I (1999) The unified modelling language user guide. Addison-Wesley, Reading
Brandsch M, Knutter I, Bosse-Doenecke E (2008) Pharmaceutical and pharmacological importance of peptide transporters. J Pharm Pharmacol 60:543–585
Brasnjevic I, Steinbusch HWM, Schmitz C, Martinez-Martinez P, European NanoBioPharmaceutics R (2009) Delivery of peptide and protein drugs over the blood-brain barrier. Prog Neurobiol 87:212–251
Caboche S, Pupin M, Leclere V, Fontaine A, Jacques P, Kucherov G (2008) NORINE: a database of nonribosomal peptides. Nucleic Acids Res 36:D326–D331
Campbell M, Humphries MM, Kiang AS, Nguyen ATH, Gobbo OL, Tam LCS et al (2011) Systemic low-molecular weight drug delivery to pre-selected neuronal regions. EMBO Mol Med 3:235–245
Carrara S, Reali V, Misiano P, Dondio G, Bigogno C (2007) Evaluation of in vitro brain penetration: optimized PAMPA and MDCKII-MDR1 assay comparison. Int J Pharm 345:125–133
Cecchelli R, Dehouck B, Descamps L, Fenart L, Buée-Scherrer V, Duhem C et al (1999) In vitro model for evaluating drug transport across the blood–brain barrier. Adv Drug Deliv Rev 36:165–178
Cecchelli R, Coisne C, Dehouck L, Miller F, Dehouck M, Buée-Scherrer V, Dehouck B (2006) Modeling the blood–brain barrier. In: Dermietzel R, Spray DC, Nedergaard M (eds) Blood–brain barriers. Wiley, Weinheim, pp 337–355
Cecchelli R, Berezowski V, Lundquist S, Culot M, Renftel M, Dehouck MP et al (2007) Modelling of the blood–brain barrier in drug discovery and development. Nat Rev Drug Discov 6:650–661
Chaurasia CS, Muller M, Bashaw ED, Benfeldt E, Bolinder J, Bullock R et al (2007) Microdialysis principles, application, and regulatory perspectives report from the joint AAPS-FDA workshop. AAPS J 9:E48–E59
Chen P (1976) The entity-relationship model—toward a unified view of data. ACM T Database Syst 1:9–36
Chen WQ, Yang JZ, Andersen R, Nielsen LH, Borchardt RT (2002) Evaluation of the permeation characteristics of a model opioid peptide, H-Tyr-D-Ala-Gly-Phe-D-Leu-OH (DADLE), and its cyclic Prodrugs across the blood–brain barrier using an in situ perfused rat brain model. J Pharmacol Exp Ther 303:849–857
Chu TC, Twu KY, Ellington AD, Levy M (2006) Aptamer mediated siRNA delivery. Nucleic Acids Res 34:6
Codd E (1970) A relational model of data for large shared data banks. Commun ACM 13:377–378
Cornford EM (1985) The blood–brain-barrier, a dynamic regulatory interface. Mol Physiol 7:219–260
Cornford EM (1999) The carotid artery single injection technique. In: Pardridge WM (ed) Introduction to the blood–brain barrier: methodology, biology and pathology. Cambridge University Press, Cambridge, pp 11–23
Crone C (1965) Facilitated transfer of glucose from blood into brain tissue. J Physiol (Lond) 181:103–113
Cucullot L, Oby E, Hallene K, Aumayr B, Rapp E, Janigro D (2006) Artificial blood–brain barriers. In: Dermietzel R, Spray DC, Nedergaard M (eds) Blood–brain barriers: from ontogeny to artificial interfaces. Wiley, Weinheim, pp 375–401
Culot M, Lundquist S, Vanuxeem D, Nion S, Landry C, Delplace Y et al (2008) An in vitro blood–brain barrier model for high throughput (HTS) toxicological screening. Toxicol In Vitro 22:799–811
Dagenais C, Rousselle C, Pollack GM, Scherrmann JM (2000) Development of an in situ mouse brain perfusion model and its application to mdr1a P-glycoprotein-deficient mice. J Cerebr Blood Flow Metab 20:381–386
Dagenais C, Avdeef A, Tsinman O, Dudley A, Beliveau R (2009) P-glycoprotein deficient mouse in situ blood–brain barrier permeability and its prediction using an in combo PAMPA model. Eur J Pharm Sci 38:121–137
Dai H, Elmquist WF (2003) Drug transport studies using quantitative microdialysis. In: Nag S (ed) The blood–brain barrier: biology and research protocols. Humana, Totowa, pp 249–264
Dash AK, Elmquist WF (2003) Separation methods that are capable of revealing blood–brain barrier permeability. J Chromatogr B 797:241–254
Davies MI, Cooper JD, Desmond SS, Lunte CE, Lunte SM (2000) Analytical considerations for microdialysis sampling. Adv Drug Deliv Rev 45:169–188
de Boer AG, Breimer DD (1996) Reconstitution of the blood–brain barrier in cell culture for studies of drug transport and metabolism. Adv Drug Deliv Rev 22:251–264
de Lange ECM, de Boer AG, Breimer DD (1999) Intracerebral microdialysis. In: Pardridge WM (ed) Introduction to the blood–brain barrier: methodology, biology and pathology. Cambridge University Press, Cambridge, pp 94–112
Deguchi Y, Miyakawa Y, Sakurada S, Naito Y, Morimoto K, Ohtsuki S et al (2003) Blood–brain barrier transport of a novel mu(1)-specific opioid peptide, H-Tyr-D-Arg-Phe-beta-Ala-OH (TAPA). J Neurochem 84:1154–1161
Deguchi Y, Naito Y, Ohtsuki S, Miyakawa Y, Morimoto K, Hosoya K et al (2004) Blood–brain barrier permeability of novel [D-Arg2]dermorphin (1-4) analogs: transport property is related to the slow onset of antinociceptive activity in the central nervous system. J Pharmacol Exp Ther 310:177–184
Deli MA, Abraham CS, Kataoka Y, Niwa M (2005) Permeability studies on in vitro blood–brain barrier models: physiology, pathology, and pharmacology. Cell Mol Neurobiol 25:59–127
Di L, Kerns EH, Fan K, McConnell OJ, Carter GT (2003) High throughput artificial membrane permeability assay for blood–brain barrier. Eur J Med Chem 38:223–232
Di L, Umland JP, Chang G, Huang Y, Lin Z, Scott DOS, Troutman MD, Liston TE (2011) Species independence in brain tissue binding using brain homogenates. Drug Metab Dispos 39:1270–1277
Dienel GA (2006) Functional brain imaging. In: Dermietzel R, Spray DC, Nedergaard M (eds) Blood–brain barriers: from ontogeny to artificial interfaces. Wiley, Weinheim, pp 551–599
Dogrukol-Ak D, Banks WA, Tuncel N, Tuncel M (2003) Passage of vasoactive intestinal peptide across the blood–brain barrier. Peptides 24:437–444
Ducarme A, Neuwels M, Goldstein S, Massingham R (1998) IAM retention and blood brain barrier penetration. Eur J Med Chem 33:215–223
Ecker GF, Noe CR (2004) In silico prediction models for blood–brain barrier permeation. Curr Med Chem 11:1617–1628
Eddy EP, Maleef BE, Hart TK, Smith PL (1997) In vitro models to predict blood–brain barrier permeability. Adv Drug Deliv Rev 23:185–198
Egleton RD, Davis TP (1999) Transport of the delta-opioid receptor agonist [d-penicillamine(2,5)] enkephalin across the blood–brain barrier involves transcytosis. J Pharm Sci 88:392–397
Egleton RD, Mitchell SA, Huber JD, Palian MM, Polt R, Davis TP (2001) Improved blood–brain barrier penetration and enhanced analgesia of an opioid peptide by glycosylation. J Pharmacol Exp Ther 299:967–972
Ehrlich P (1885) Das sauerstufbudurfnis des organismus. Eine Farbenanalytische Studie. Verlag von August Hirschwald, Berlin
Engelhardt B (2006) Development of the blood–brain interface. In: Dermietzel R, Spray DC, Nedergaard M (eds) Blood–brain barrier: from ontogeny to artificial interfaces. Wiley VCH, Weinheim, pp 11–39
Ermisch A (1992) Peptide receptors of the blood–brain-barrier and substrate transport into the brain. In: Ermisch A, Landgraf R, Ruhle HJ (eds) Circumventricular organs and brain fluid environment: molecular and functional aspects. Elsevier, Amsterdam, pp 155–161
Ermisch A, Ruhle HJ, Landgraf R, Hess J (1985) Blood–brain barrier and peptides. J Cerebr Blood Flow Metab 5:350–357
Ermisch A, Ruhle HJ, Kretzschmar R, Baethmann A (1991) On the blood–brain-barrier to peptides—specific binding of atrial-natriuretic-peptide in vivo and in vitro. Brain Res 554:209–216
Ewing JR, Knight RA, Nagaraja TN, Yee JS, Nagesh V, Whitton PA et al (2003) Patlak plots of Gd-DTPA MRI data yield blood–brain transfer constants concordant with those of C-14-sucrose in areas of blood–brain opening. Magn Reson Med 50:283–292
Feng B, Mills JB, Davidson RE, Mireles RJ, Janiszewski JS, Troutman MD et al (2008) In vitro P-glycoprotein assays to predict the in vivo interactions of P-glycoprotein with drugs in the central nervous system. Drug Metab Dispos 36:268–275
Fenstermacher JD, Wei L (1999) Measuring local cerebral capillary permeability-surface area products by quantitative autoradiography. In: Pardridge WM (ed) Introduction to the blood–brain barrier: methodology, biology and pathology. Cambridge University Press, Cambridge, pp 122–132
Fiori A, Cardelli P, Negri L, Savi MR, Strom R, Erspamer V (1997) Deltorphin transport across the blood–brain barrier. Proc Natl Acad Sci USA 94:9469–9474
Fischer H, Gottschlich R, Seelig A (1998) Blood–brain barrier permeation: molecular parameters governing passive diffusion. J Membr Biol 165:201–211
Franke H, Galla HJ, Beuckmann CT (2000) Primary cultures of brain microvessel endothelial cells: a valid and flexible model to study drug transport through the blood–brain barrier in vitro. Brain Res Protoc 5:248–256
Friden M, Gupta A, Antonsson M, Bredberg U, Hammarlund-Udenaes M (2007) In vitro methods for estimating unbound drug concentrations in the brain interstitial and intracellular fluids. Drug Metab Dispos 35:1711–1719
Friden M, Ducrozet F, Middleton B, Antonsson M, Bredberg U, Hammarlund-Udenaes M (2009) Development of a high-throughput brain slice method for studying drug distribution in the central nervous system. Drug Metab Dispos 37:1226–1233
Fujikawa M, Ano R, Nakao K, Shimizu R, Akamatsu M (2005) Relationships between structure and high-throughput screening permeability of diverse drugs with artificial membranes: application to prediction of Caco-2 cell permeability. Bioorg Med Chem 13:4721–4732
Gaillard PJ, Voorwinden LH, Nielsen JL, Ivanov A, Atsumi R, Engman H et al (2001) Establishment and functional characterization of an in vitro model of the blood–brain barrier, comprising a co-culture of brain capillary endothelial cells and astrocytes. Eur J Pharm Sci 12:215–222
Ganapathy V, Miyauchi S (2005) Transport systems for opioid peptides in mammalian tissues. AAPS J 7:E852–E856
Garberg P, Ball M, Borg N, Cecchelli R, Fenart L, Hurst RD et al (2005) In vitro models for the blood–brain barrier. Toxicol In Vitro 19:299–334
Gerebtzoff G, Seelig A (2006) In silico prediction of blood–brain barrier permeation using the calculated molecular cross-sectional area as main parameter. J Chem Inf Model 46:2638–2650
Giaginis C, Tsantili-Kakoulidou A (2008) Alternative measures of lipophilicity: from octanol–water partitioning to IAM retention. J Pharm Sci 97:2984–3004
Gjedde A (1981) High-affinity and low-affinity transport of d-glucose from blood to brain. J Neurochem 36:1463–1471
Gjedde A, Christensen O (1984) Estimates of Michaelis–Menten constants for the 2 membranes of the brain endothelium. J Cerebr Blood Flow Metab 4:241–249
Golden PL, Pollack GM (2003) Blood–brain barrier efflux transport. J Pharm Sci 92:1739–1753
Goldmann EE (1913) Vitalfärbung am Zentralnervensystem. Abhandl Konigl preuss Akad Wiss 1:1–60
Grant GA, Abbott NJ, Janigro D (1998) Understanding the physiology of the blood–brain barrier: in vitro models. News Physiol Sci 13:287–293
Gray RA, Vandervelde DG, Burke CJ, Manning MC, Middaugh CR, Borchardt RT (1994) Delta-sleep-inducing peptide—solution conformational studies of a membrane-permeable peptide. Biochemistry 33:1323–1331
Gulya K, Krivan M, Nyolczas N, Sarnyai Z, Kovacs GL (1988) Central effects of the potent and highly selective-mu-opioid antagonist d-Phe-Cys-Tyr-D-Trp-Orn-Thr-Pen-Thr-NH2 (CTOP) in mice. Eur J Pharmacol 150:355–360
Gumbleton M, Audus KL (2001) Progress and limitations in the use of in vitro cell cultures to serve as a permeability screen for the blood–brain barrier. J Pharm Sci 90:1681–1698
Gupta A, Chatelain P, Massingham R, Jonsson EN, Hammarlund-Udenaes M (2006) Brain distribution of cetirizine enantiomers: comparison of three different tissue-to-plasma partition coefficients: K-p, K-p, K-u, and K-p, K-uu. Drug Metab Dispos 34:318–323
Hakkarainen JJ, Jalkanen AJ, Kaariainen TM, Keski-Rahkonen P, Venalainen T, Hokkanen J et al (2010) Comparison of in vitro cell models in predicting in vivo brain entry of drugs. Int J Pharm 402:27–36
Hammami R, Ben Hamida J, Vergoten G, Fliss I (2009) PhytAMP: a database dedicated to antimicrobial plant peptides. Nucleic Acids Res 37:D963–D968
Hammarlund-Udenaes M (2000) The use of microdialysis in CNS drug delivery studies—pharmacokinetic perspectives and results with analgesics and antiepileptics. Adv Drug Deliv Rev 45:283–294
Hansen DK, Scott DO, Otis KW, Lunte SM (2002) Comparison of in vitro BBMEC permeability and in vivo CNS uptake by microdialysis sampling. J Pharm Biomed Anal 27:945–957
Hawkins KN, Knapp RJ, Lui GK, Gulya K, Kazmierski W, Wan YP et al (1989) [H-3]-[H-D-Phe-Cys-Tyr-D-Trp-Orn-Thr-Pen-Thr-NH2] ([H-3] CTOP), a potent and highly selective peptide for mu-opioid receptors in rat-brain. J Pharmacol Exp Ther 248:73–80
Hoffmann A, Bredno J, Wendland MF, Derugin N, Hom J, Schuster T et al (2011) Validation of in vivo magnetic resonance imaging blood–brain barrier permeability measurements by comparison with gold standard histology. Stroke 42:2054–2060
Hosoya K-i, Ohtsuki S, Terasaki T (2002) Recent advances in the brain-to-blood efflux transport across the blood–brain barrier. Int J Pharm 248:15–29
Hsuchou H, Pan W, Kastin AJ (2007) The fasting polypeptide FGF21 can enter brain from blood. Peptides 28:2382–2386
Innis RB, Cunningham VJ, Delforge J, Fujita M, Giedde A, Gunn RN et al (2007) Consensus nomenclature for in vivo imaging of reversibly binding radioligands. J Cerebr Blood Flow Metab 27:1533–1539
Isakovic AJ, Abbott NJ, Redzic ZB (2004) Brain to blood efflux transport of adenosine: blood–brain barrier studies in the rat. J Neurochem 90:272–286
Jeffrey P, Summerfield S (2010) Assessment of the blood–brain barrier in CNS drug discovery. Neurobiol Dis 37:33–37
Joo F, Karnushi I (1973) Procedure for isolation of capillaries from rat-brain. Cytobios 8:41–48
Kakee A, Tersaki T, Sugiyama Y (1996) Brain efflux index as a novel method of analyzing efflux transport at the blood–brain barrier. J Pharmacol Exp Ther 277:1550–1559
Kalvass JC, Maurer TS (2002) Influence of nonspecific brain and plasma binding on CNS exposure: implications for rational drug discovery. Biopharm Drug Dispos 23:327–338
Kansy M, Senner F, Gubernator K (1998) Physicochemical high throughput screening: parallel artificial membrane permeation assay in the description of passive absorption processes. J Med Chem 41:1007–1010
Kastin AJ, Akerstrom V (1999) Nonsaturable entry of neuropeptide Y into brain. Am J Physiol Endocrinol Metab 276:E479–E482
Kastin AJ, Akerstrom V (2003) Entry of exendin-4 into brain is rapid but may be limited at high doses. Int J Obes 27:313–318
Kastin AJ, Akerstrom V, Pan WH (2001) Validity of multiple-time regression analysis in measurement of tritiated and iodinated leptin crossing the blood–brain barrier: meaningful controls. Peptides 22:2127–2136
Kastin AJ, Akerstrom V, Pan WH (2002) Interactions of glucagon-like peptide-1 (GLP-1) with the blood–brain barrier. J Mol Neurosci 18:7–14
Kleczkowska P, Kosson P, Ballet S, Van den Eynde I, Tsuda Y, Tourwé D et al (2010) PK20, a new opioid–neurotensin hybrid peptide that exhibits central and peripheral antinociceptive effects. Mol Pain 6:86–92
Knudsen GM, Paulson OB (1999) Measurement of blood–brain barrier in humans using indicator diffusion. In: Pardridge WM (ed) Introduction to the blood–brain barrier: methodology, biology and pathology. Cambridge University Press, Cambridge, pp 133–139
Kretzschmar R, Landgraf R, Gjedde A, Ermisch A (1986) Vasopressin binds to microvessels from rat hippocampus. Brain Res 380:325–330
Kumar G, Smith QR, Hokari M, Parepally J, Duncan MW (2007) Brain uptake, pharmacokinetics, and tissue distribution in the rat of neurotoxic N-butylbenzenesulfonamide. Toxicol Sci 97:253–264
Kusuhara H, Terasaki T, Sugiyama Y (2003) Brain efflux index method. In: Nag S (ed) The blood–brain barrier: biology and research protocols. Humana, Totowa, pp 219–231
Lanevskij K, Dapkunas J, Juska L, Japertas P, Didziapetris R (2010) QSAR Analysis of blood–brain distribution: the influence of plasma and brain tissue binding. J Pharm Sci 100:2147–2160
Lazaro E, Rafols CR, Roses M (2005) Characterization of immobilized artificial membrane (IAM) and XTerra columns by means of chromatographic models. J Chromatogr A 1081:163–173
Levin VA (1980) Relationship of octanol–water partition-coefficient and molecular-weight to rat-brain capillary-permeability. J Med Chem 23:682–684
Lin JH (1998) Applications and limitations of interspecies scaling and in vitro extrapolation in pharmacokinetics. Drug Metab Dispos 26:1202–1212
Liu XR, Tu MH, Kelly RS, Chen CP, Smith BJ (2004) Development of a computational approach to predict blood–brain barrier permeability. Drug Metab Dispos 32:132–139
Liu XR, Smith BJ, Chen CP, Callegari E, Becker SL, Chen X et al (2005) Use of a physiologically based pharmacokinetic model to study the time to reach brain equilibrium: an experimental analysis of the role of blood–brain barrier permeability, plasma protein binding, and brain tissue binding. J Pharmacol Exp Ther 313:1254–1262
Liu HM, Liu XF, Yao JL, Wang CL, Yu Y, Wang R (2006a) Utilization of combined chemical modifications to enhance the blood–brain barrier permeability and pharmacological activity of endomorphin-1. J Pharmacol Exp Ther 319:308–316
Liu XR, Smith BJ, Chen C, Callegari E, Becker SL, Chen X et al (2006b) Evaluation of cerebrospinal fluid concentration and plasma free concentration as a surrogate measurement for brain free concentration. Drug Metab Dispos 34:1443–1447
Liu XR, Chen CP, Smith BJ (2008) Progress in brain penetration evaluation in drug discovery and development. J Pharmacol Exp Ther 325:349–356
Liu Y, Paliwal S, Bankiewicz KS, Bringas JR, Heart G, Mitragotri S et al (2010) Ultrasound-enhanced drug transport and distribution in the brain. AAPS PharmSciTech 11:1005–1017
Logan J (2000) Graphical analysis of PET data applied to reversible and irreversible tracers. Nucl Med Biol 27:661–670
Lundquist S, Renftel M (2002) The use of in vitro cell culture models for mechanistic studies and as permeability screens for the blood-brain barrier in the pharmaceutical industry—background and current status in the drug discovery process. Vascul Pharmacol 38:355–364
Lundquist S, Renftel M, Brillault J, Fenart L, Cecchelli R, Dehouck MP (2002) Prediction of drug transport through the blood–brain barrier in vivo: a comparison between two in vitro cell models. Pharm Res 19:976–981
Madgula VLM, Avula B, Reddy VLN, Khan KA, Khan SI (2007) Transport of decursin and decursinol angelate across Caco-2 and MDR-MDCK cell monolayers: in vitro models for intestinal and blood–brain barrier permeability. Planta Med 73:330–335
Madsen SJ, Hirschberg H (2010) Site-specific opening of the blood–brain barrier. J Biophotonics 3:356–367
Malina KCK, Cooper I, Teichberg VI (2009) Closing the gap between the in vivo and in vitro blood–brain barrier tightness. Brain Res 1284:12–21
Mano Y, Higuchi S, Kamimura H (2002) Investigation of the high partition of YM992, a novel antidepressant, in rat brain—in vitro and in vivo evidence for the high binding in brain and the high permeability at the BBB. Biopharm Drug Dispos 23:351–360
Martin I (2004) Prediction of blood–brain barrier penetration: are we missing the point? Drug Discov Today 9:161–162
Maupetit J, Derreumaux P, Tuffery P (2009) PEP-FOLD: an online resource for de novo peptide structure prediction. Nucleic Acids Res 37:W498–W503
Maurer TS, DeBartolo DB, Tess DA, Scott DO (2005) Relationship between exposure and nonspecific binding of thirty-three central nervous system drugs in mice. Drug Metab Dispos 33:175–181
Mensch J, Oyarzabal J, Mackie C, Augustijns P (2009) In vivo, in vitro and in silico methods for small molecule transfer across the BBB. J Pharm Sci 98:4429–4468
Mensch J, Melis A, Mackie C, Verreck G, Brewster ME, Augustijns P (2010) Evaluation of various PAMPA models to identify the most discriminating method for the prediction of BBB permeability. Eur J Pharm Biopharm 74:495–502
Moriki Y, Suzuki T, Furuishi T, Fukami T, Tomono K, Watanabe J (2005) In vivo evidence for the efflux transport of pentazocine from the brain across the blood–brain barrier using the brain efflux index method. J Drug Target 13:53–59
Mueggler T, Baltes C, Rudin M (2009) Molecular neuroimaging in rodents: assessing receptor expression and function. Eur J Neurosci 30:1860–1869
Murakami H, Takanaga H, Matsuo H, Ohtani H, Sawada Y (2000) Comparison of blood–brain barrier permeability in mice and rats using in situ brain perfusion technique. Am J Physiol Heart Circ Physiol 279:H1022–H1028
Nag S (2003) The blood–brain barrier: biology and research protocols. Humana, Totowa
Nakagawa S, Deli MA, Kawaguchi H, Shimizudani T, Shimono T, Kittel A et al (2009) A new blood–brain barrier model using primary rat brain endothelial cells, pericytes and astrocytes. Neurochem Int 54:253–263
Nakai D, Kumamoto K, Sakikawa C, Kosaka T, Tokui T (2004) Evaluation of the protein binding ratio of drugs by a micro-scale ultracentrifugation method. J Pharm Sci 93:847–854
Navarro C, Gonzalez-Alvarez I, Gonzalez-Alvarez M, Manku M, Merino V, Casabo VG et al (2011) Influence of polyunsaturated fatty acids on cortisol transport through MDCK and MDCK-MDR1 cells as blood–brain barrier in vitro model. Eur J Pharm Sci 42:290–299
Neuhaus W, Stessl M, Strizsik E, Bennani-Baiti B, Wirth M, Toegel S et al (2010) Blood-brain barrier cell line PBMEC/C1–2 possesses functionally active P-glycoprotein. Neurosci Lett 469:224–228
Nicolazzo JA, Charman SA, Charman WN (2006) Methods to assess drug permeability across the blood–brain barrier. J Pharm Pharmacol 58:281–293
Ohno K, Pettigrew KD, Rapoport SI (1978) Lower limits of cerebrovascular permeability to non-electrolytes in conscious rat. Am J Physiol 235:H299–H307
Okura T, Komiyama N, Morita Y, Kimura M, Deguchi Y, Yamada S (2007) Comparative measurement of spinal CSF microdialysate concentrations and concomitant antinociception of morphine and morphine-6[beta]-glucuronide in rats. Life Sci 80:1319–1326
Oldendorf WH (1970) Measurement of brain uptake of radiolabeled substances using a tritiated water internal standard. Brain Res 24:372–376
Omidi Y, Campbell L, Barar J, Connell D, Akhtar S, Gumbleton M (2003) Evaluation of the immortalised mouse brain capillary endothelial cell line, b.End3, as an in vitro blood-brain barrier model for drug uptake and transport studies. Brain Res 990:95–112
Ottaviani G, Martel S, Escarala C, Nicolle E, Carrupt PA (2008) The PAMPA technique as a HTS tool for partition coefficients determination in different solvent/water systems. Eur J Pharm Sci 35:68–75
Pan WH, Banks WA, Fasold MB, Bluth J, Kastin AJ (1998a) Transport of brain-derived neurotrophic factor across the blood–brain barrier. Neuropharmacology 37:1553–1561
Pan WH, Banks WA, Kastin AJ (1998b) Permeability of the blood–brain barrier to neurotrophins. Brain Res 788:87–94
Pan WH, Yu YM, Cain CM, Nyberg F, Couraud PO, Kastin AJ (2005) Permeation of growth hormone across the blood–brain barrier. Endocrinology 146:4898–4904
Pan WH, Tu H, Kastin AJ (2006) Differential BBB interactions of three ingestive peptides: obestatin, ghrelin, and adiponectin. Peptides 27:911–916
Pardridge WM (1995) Transport of small molecules through the blood–brain-barrier—biology and methodology. Adv Drug Deliv Rev 15:5–36
Pardridge WM (1999a) Introduction to the blood–brain barrier: methodology, biology and pathology. Cambridge University Press, Cambridge
Pardridge WM (1999b) Isolated brain capillaries: an in vitro model of blood–brain barrier research. In: Pardridge WM (ed) Introduction to the blood–brain barrier. Cambridge University Press, Cambridge, pp 49–61
Pardridge WM (2004) Log(BB), PS products and in silico models of drug brain penetration. Drug Discov Today 9:392–393
Patlak CS, Blasberg RG, Fenstermacher JD (1983) Graphical evaluation of blood-to-brain transfer constants from multiple-time uptake data. J Cerebr Blood Flow Metab 3:1–7
Peremans K, De Spiegeleer B, Buntinx E, Dobbeleir A, Vermeire S, Vandermeulen E et al (2008) Evaluation of serotonin-2A receptor occupancy with I-123–5-I-R91150 and single-photon emission tomography before and after low-dose pipamperone administration in the canine brain. Nucl Med Commun 29:724–729
Petereit AC, Swinney K, Mensch J, Mackie C, Stokbroekx S, Brewster M et al (2010) Prediction of blood–brain barrier penetration of poorly soluble drug candidates using surface activity profiling. Eur J Pharm Biopharm 75:405–410
Pidgeon C, Venkataram UV (1989) Immobilized artificial membrane chromatography—supports composed of membrane-lipids. Anal Biochem 176:36–47
Plattner VE, Germann B, Neuhaus W, Noe CR, Gabor F, Wirth M (2010) Characterization of two blood–brain barrier mimicking cell lines: distribution of lectin-binding sites and perspectives for drug delivery. Int J Pharm 387:34–41
Price TO, Samson WK, Niehoff ML, Banks WA (2007) Permeability of the blood–brain barrier to a novel satiety molecule nesfatin-1. Peptides 28:2372–2381
Prieto P, Blaauboer BJ, de Boer AG, Boveri M, Cecchelli R, Clemedson C et al (2004) Blood–brain barrier in vitro models and their application in toxicology—the report and recommendations of ECVAM workshop 49. Altern Lab Anim 32:37–50
Raub TJ, Lutzke BS, Andrus PK, Sawada GA, Staton BA (2006) Early preclinical evaluation of brain exposure in support of hit identification and lead optimization. In: Borchardt RT, Kerns EH, Hageman MJ, Thakker DR, Stevens JL (eds) Optimizing the “Drug-Like” properties of leads in drug discovery. Springer, New York, pp 355–410
Raybon JJ, Boje KMK (2001) A critical evaluation of the brain efflux index method as applied to the nitric oxide synthase inhibitor, aminoguanidine. Biopharm Drug Dispos 22:391–401
Read KD, Braggio S (2010) Assessing brain free fraction in early drug discovery. Expert Opin Drug Metab Toxicol 6:337–344
Reichel A (2009) Addressing central nervous system (CNS) penetration in drug discovery: basics and implications of the evolving new concept. Chem Biodivers 6:2030–2049
Reichel A, Begley DJ (1998) Potential of immobilized artificial membranes for predicting drug penetration across the blood–brain barrier. Pharm Res 15:1270–1274
Reichel A, Begley DJ, Abbott NJ (2003) An overview of in vitro techniques for blood–brain barrier studies. In: Nag S (ed) The blood–brain barrier: biology and research protocols. Humana, Totowa, pp 307–324
Renkin EM (1959) Transport of potassium-42 from blood to tissue in isolated mammalian skeletal muscles. Am J Physiol 197:1205–1210
Rossi JJ (2011) Inducible and reversible breaching of the blood brain barrier by RNAi. EMBO Mol Med 3:186–188
Roux F, Couraud PO (2005) Rat brain endothelial cell lines for the study of blood–brain barrier permeability and transport functions. Cell Mol Neurobiol 25:41–58
Saunders NR, Dziegielewska KM (1999) Transport in the developing brain. In: Pardridge WM (ed) Introduction to the blood–brain barrier: methodology, biology and pathology. Cambridge University Press, Cambridge, pp 277–289
Scheller D, Kolb J (1991) The internal reference technique in microdialysis—a practical approach to monitoring dialysis efficiency and to calculating tissue concentration from dialysate samples. J Neurosci Methods 40:31–38
Seelig A, Gottschlich R, Devant RM (1994) A method to determine the ability of drugs to diffuse through the blood–brain-barrier. Proc Natl Acad Sci USA 91:68–72
Shayan G, Choi YS, Shusta EV, Shuler ML, Lee KH (2011) Murine in vitro model of the blood–brain barrier for evaluating drug transport. Eur J Pharm Sci 42:148–155
Shen DD, Artru AA, Adkison KK (2004) Principles and applicability of CSF sampling for the assessment of CNS drug delivery and pharmacodynamics. Adv Drug Deliv Rev 56:1825–1857
Siissalo S, Hannukainen J, Kolehmainen J, Hirvonen J, Kaukonen AM (2009) A Caco-2 cell based screening method for compounds interacting with MRP2 efflux protein. Eur J Pharm Biopharm 71:332–338
Smith QR (2003) A review of blood–brain barrier transport techniques. In: Nag S (ed) The blood–brain barrier: biology and research protocols. Humana, Totowa, pp 193–208
Smith M, Omidi Y, Gumbleton M (2007) Primary porcine brain microvascular endothelial cells: biochemical and functional characterisation as a model for drug transport and targeting. J Drug Target 15:253–268
Stenken JA (1999) Methods and issues in microdialysis calibration. Anal Chim Acta 379:337–358
Stewart BH, Chan OH (1998) Use of immobilized artificial membrane chromatography for drug transport applications. J Pharm Sci 87:1471–1478
Su Y, Sinko PJ (2006) Drug delivery across the blood–brain barrier: why is it difficult? How to measure and improve it? Expert Opin Drug Del 3:419–435
Subramanian G, Kitchen DB (2003) Computational models to predict blood–brain barrier permeation and CNS activity. J Comput Aided Mol Des 17:643–664
Summerfield SG, Read K, Begley DJ, Obradovic T, Hidalgo IJ, Coggon S et al (2007) Central nervous system drug disposition: the relationship between in situ brain permeability and brain free fraction. J Pharmacol Exp Ther 322:205–213
Suzuki T, Moriki Y, Goto H, Tomono K, Hanano M, Watanabe J (2002) Investigation on the influx transport mechanism of pentazocine at the blood–brain barrier in rats using the carotid injection technique. Biol Pharm Bull 25:1351–1355
Taheri S, Sood R (2006) Kalman filtering for reliable estimation of BBB permeability. Magn Reson Imaging 24:1039–1049
Taheri S, Sood R (2007) Partial volume effect compensation for improved reliability of quantitative blood–brain barrier permeability. Magn Reson Imaging 25:613–625
Takasato Y, Rapoport SI, Smith QR (1984) An in situ brain perfusion technique to study cerebrovascular transport in the rat. Am J Physiol 247:H484–H493
Terasaki T (1999) Development of brain efflux index (BEI) method and its application to the blood–brain barrier efflux transport study. In: Pardridge WM (ed) Introduction to the blood–brain barrier: methodology, biology and pathology. Cambridge University Press, Cambridge, pp 24–31
Terasaki T, Ohtsuki S, Hori S, Takanaga H, Nakashima E, Hosoya K-i (2003) New approaches to in vitro models of blood–brain barrier drug transport. Drug Discov Today 8:944–954
Triguero D, Buciak J, Pardridge WM (1990) Capillary depletion method for quantification of blood–brain-barrier transport of circulating peptides and plasma-proteins. J Neurochem 54:1882–1888
Tsai TH (2003) Assaying protein unbound drugs using microdialysis techniques. J Chromatogr B Technol Biomed Life Sci 797:161–173
Tunblad K, Jonsson EN, Hammarlund-Udenaes M (2003) Morphine blood–brain barrier transport is influenced by probenecid co-administration. Pharm Res 20:618–623
Uchida M, Fukazawa T, Yamazaki Y, Hashimoto H, Miyamoto Y (2009) A modified fast (4 day) 96-well plate Caco-2 permeability assay. J Pharmacol Toxicol Methods 59:39–43
Urquhart BL, Kim RB (2009) Blood–brain barrier transporters and response to CNS-active drugs. Eur J Clin Pharmacol 65:1063–1070
Usansky HH, Sinko PJ (2003) Computation of log BB values for compounds transported through carrier-mediated mechanisms using in vitro permeability data from brain microvessel endothelial cell (BMEC) monolayers. Pharm Res 20:390–396
Van Belle K, Dzeka T, Sarre S, Ebinger G, Michotte Y (1993) In vitro and in vivo microdialysis calibration for the measurement of carbamazepine and its metabolites in rat brain tissue using the internal reference technique. J Neurosci Methods 49:167–173
Van Dorpe S, Adriaens A, Polis I, Peremans K, Van Bocxlaer J, De Spiegeleer B (2010) Analytical characterization and comparison of the blood–brain barrier permeability of eight opioid peptides. Peptides 31:1390–1399
Van Dorpe S, Adriaens A, Vermeire S, Polis I, Peremans K, De Spiegeleer B (2011) Desirability function combining metabolic stability and functionality of peptides. J Pept Sci 17:398–404
Vanhee P, Reumers J, Stricher F, Baeten L, Serrano L, Schymkowitz J et al (2010) PepX: a structural database of non-redundant protein-peptide complexes. Nucleic Acids Res 38:D545–D551
Verma RP, Hansch C, Selassie CD (2007) Comparative QSAR studies on PAMPA/modified PAMPA for high throughput profiling of drug absorption potential with respect to Caco-2 cells and human intestinal absorption. J Comput Aided Mol Des 21:3–22
Walker I, Coleman MD (1995) The blood–brain barrier: in vitro methods and toxicological applications. Toxicol In Vitro 9:191–204
Wang Q, Rager JD, Weinstein K, Kardos PS, Dobson GL, Li JB et al (2005) Evaluation of the MDR-MDCK cell line as a permeability screen for the blood–brain barrier. Int J Pharm 288:349–359
Wang GS, Li X, Wang Z (2009) APD2: the updated antimicrobial peptide database and its application in peptide design. Nucleic Acids Res 37:D933–D937
Webb S, Ott RJ, Cherry SR (1989) Quantitation of blood–brain barrier permeability by positron emission tomography. Phys Med Biol 34:1767–1771
Wilson JF, Anderson S, Snook G, Llewellyn KD (1984) Quantification of the permeability of the blood–CSF barrier to [alpha]-MSH in the rat. Peptides 5:681–685
Yazdanian M, Glynn SL, Wright JL, Hawi A (1998) Correlating partitioning and Caco-2 cell permeability of structurally diverse small molecular weight compounds. Pharm Res 15:1490–1494
Yoon CH, Kim SJ, Soo BS, Lee SC, Yoo SD (2006) Rapid screening of blood–brain barrier penetration of drugs using the immobilized artificial membrane phosphatidylcholine column chromatography. J Biomol Screen 11:13–20
Zlokovic BV, Hyman S, McComb JG, Lipovac MN, Tang G, Davson H (1990) Kinetics of arginine-vasopressin uptake at the blood–brain-barrier. Biochim Biophys Acta 1025:191–198
Zlokovic BV, Mackic JB, McComb JG, Weiss MH, Kaplowitz N, Kannan R (1994) Evidence for transcapillary transport of reduced glutathione in vascular perfused guinea-pig brain. Biochem Biophys Res Commun 201:402–408
Acknowledgments
This work was supported by a PhD grant of ‘Institute for the Promotion of Innovation through Science and Technology in Flanders (IWT-Vlaanderen)’ (73402 to S.V.D.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Van Dorpe, S., Bronselaer, A., Nielandt, J. et al. Brainpeps: the blood–brain barrier peptide database. Brain Struct Funct 217, 687–718 (2012). https://doi.org/10.1007/s00429-011-0375-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00429-011-0375-0