Abstract
Purpose
Myopic regression after surgery is the most common long-term complication of refractive surgery, but it is difficult to identify myopic regression without long-term observation. This study aimed to develop machine learning models to identify high-risk patients for refractive regression based on preoperative data and fundus photography.
Methods
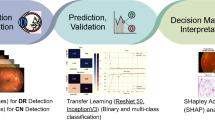
This retrospective study assigned subjects to the training (n = 1606 eyes) and validation (n = 403 eyes) datasets with chronological data splitting. Machine learning models with ResNet50 (for image analysis) and XGBoost (for integration of all variables and fundus photography) were developed based on subjects who underwent corneal refractive surgery. The primary outcome was the predictive performance for the presence of myopic regression at 4 years of follow-up examination postoperatively.
Results
By integrating all factors and fundus photography, the final combined machine learning model showed good performance to predict myopic regression of more than 0.5 D (area under the receiver operating characteristic curve [ROC-AUC], 0.753; 95% confidence interval [CI], 0.710–0.793). The performance of the final model was better than the single ResNet50 model only using fundus photography (ROC-AUC, 0.673; 95% CI, 0.627–0.716). The top-five most important input features were fundus photography, preoperative anterior chamber depth, planned ablation thickness, age, and preoperative central corneal thickness.
Conclusion
Our machine learning algorithm provides an efficient strategy to identify high-risk patients with myopic regression without additional labor, cost, and time. Surgeons might benefit from preoperative risk assessment of myopic regression, patient counseling before surgery, and surgical option decisions.




Similar content being viewed by others
References
Kim T-I, Del Barrio JLA, Wilkins M et al (2019) Refractive surgery. Lancet 393:2085–2098. https://doi.org/10.1016/S0140-6736(18)33209-4
Kim JH, Sah WJ, Park CK et al (1996) Myopic regression after photorefractive keratectomy. Ophthalmic Surg Lasers 27:S435-439
Chen Y-I, Chien K-L, Wang I-J et al (2007) An interval-censored model for predicting myopic regression after laser in situ keratomileusis. Invest Ophthalmol Vis Sci 48:3516–3523. https://doi.org/10.1167/iovs.06-1044
Hwang HS, Lee HJ, Lee SJ, Kim J-H (2020) Visual outcomes after three different surgical procedures for correction of refractive error in patients with thin corneas. Int J Ophthalmol 13:970–977. https://doi.org/10.18240/ijo.2020.06.18
Zheng Y-F, Pan C-W, Chay J et al (2013) The economic cost of myopia in adults aged over 40 years in Singapore. Invest Ophthalmol Vis Sci 54:7532–7537. https://doi.org/10.1167/iovs.13-12795
Zhou J, Gao Y, Li S et al (2020) Predictors of myopic regression for laser-assisted subepithelial keratomileusis and laser-assisted in situ keratomileusis flap creation with mechanical microkeratome and femtosecond laser in low and moderate myopia. Ophthalmic Epidemiol 27:177–185. https://doi.org/10.1080/09286586.2019.1704793
Yan MK, Chang JS, Chan TC (2018) Refractive regression after laser in situ keratomileusis. Clin Exp Ophthalmol 46:934–944. https://doi.org/10.1111/ceo.13315
Ryu I-H, Kim WK, Nam MS et al (2020) Reduction of corneal epithelial thickness during medical treatment for myopic regression following FS-LASIK. BMC Ophthalmol 20:296. https://doi.org/10.1186/s12886-020-01570-2
Gab-Alla AA (2020) Is the axial length a risk factor for post-LASIK myopic regression? Graefes Arch Clin Exp Ophthalmol 259:777–786. https://doi.org/10.1007/s00417-020-04990-4
Varadarajan AV, Poplin R, Blumer K et al (2018) Deep learning for predicting refractive error from retinal fundus images. Invest Ophthalmol Vis Sci 59:2861–2868. https://doi.org/10.1167/iovs.18-23887
Imran A, Li J, Pei Y et al (2020) Automated identification of cataract severity using retinal fundus images. Comput Methods Biomech Biomed Eng: Imaging Visual 8:691–698. https://doi.org/10.1080/21681163.2020.1806733
Hayashi K, Ohno-Matsui K, Shimada N et al (2010) Long-term pattern of progression of myopic maculopathy: a natural history study. Ophthalmology 117:1595-1611.e4. https://doi.org/10.1016/j.ophtha.2009.11.003
Yoo TK, Ryu IH, Lee G et al (2019) Adopting machine learning to automatically identify candidate patients for corneal refractive surgery. npj Digital Med 2:59. https://doi.org/10.1038/s41746-019-0135-8
Korkmaz S, Bilgihan K, Sul S, Hondur A (2014) A clinical and confocal microscopic comparison of transepithelial PRK and LASEK for myopia. J Ophthalmol 2014:e784185. https://doi.org/10.1155/2014/784185
Yoo TK, Ryu IH, Choi H et al (2020) Explainable machine learning approach as a tool to understand factors used to select the refractive surgery technique on the expert level. Transl Vis Sci Technol 9:1–8
Kang EM, Ryu IH, Lee G et al (2021) Development of a web-based ensemble machine learning application to select the optimal size of posterior chamber phakic intraocular lens. Trans Vis Sci Tech 10:5–5. https://doi.org/10.1167/tvst.10.6.5
Moon C-H (2015) Visual outcomes of laser refractive surgery in ROKAF pilot; 7-year review. Korean J Aerosp Environ Med 25:91–97
Pachade S, Porwal P, Thulkar D et al (2021) Retinal Fundus Multi-Disease Image Dataset (RFMiD): a dataset for multi-disease detection research. Data 6:14. https://doi.org/10.3390/data6020014
Fujimura F, Kamiya K, Fujiwara K et al (2013) Repeatability and reproducibility of measurements using a NT-530P noncontact tono/pachymeter and correlation of central corneal thickness with intraocular pressure. Biomed Res Int 2013:e370592. https://doi.org/10.1155/2013/370592
Arcadu F, Benmansour F, Maunz A et al (2019) Deep learning algorithm predicts diabetic retinopathy progression in individual patients. npj Digit Med 2:1–9. https://doi.org/10.1038/s41746-019-0172-3
Mallen EAH, Kashyap P, Hampson KM (2006) Transient axial length change during the accommodation response in young adults. Invest Ophthalmol Vis Sci 47:1251–1254. https://doi.org/10.1167/iovs.05-1086
Xia L-K, Ma J, Liu H-N et al (2018) Three-year results of small incision lenticule extraction and wavefront-guided femtosecond laser-assisted laser in situ keratomileusis for correction of high myopia and myopic astigmatism. Int J Ophthalmol 11:470–477. https://doi.org/10.18240/ijo.2018.03.18
Hyun S, Lee S, Kim J (2016) Visual outcomes after SMILE, LASEK, and LASEK combined with corneal collagen cross-linking for high myopic correction. Cornea 36:399–405. https://doi.org/10.1097/ICO.0000000000001089
Kanellopoulos AJ, Asimellis G, Karabatsas C (2014) Comparison of prophylactic higher fluence corneal cross-linking to control, in myopic LASIK, one year results. Clin Ophthalmol 8:2373–2381. https://doi.org/10.2147/OPTH.S68372
Poplin R, Varadarajan AV, Blumer K et al (2018) Prediction of cardiovascular risk factors from retinal fundus photographs via deep learning. Nat Biomed Eng 2:158
Ishii K, Asaoka R, Omoto T et al (2021) Predicting intraocular pressure using systemic variables or fundus photography with deep learning in a health examination cohort. Sci Rep 11:3687. https://doi.org/10.1038/s41598-020-80839-4
Yoo TK, Ryu IH, Kim JK, Lee IS (2021) Deep learning for predicting uncorrected refractive error using posterior segment optical coherence tomography images. Eye 1–7.https://doi.org/10.1038/s41433-021-01795-5
Mehta P, Petersen CA, Wen JC et al (2021) Automated detection of glaucoma with interpretable machine learning using clinical data and multimodal retinal images. Am J Ophthalmol 231:154–169. https://doi.org/10.1016/j.ajo.2021.04.021
Yoo TK, Choi JY, Seo JG et al (2019) The possibility of the combination of OCT and fundus images for improving the diagnostic accuracy of deep learning for age-related macular degeneration: a preliminary experiment. Med Biol Eng Comput 57:677–687. https://doi.org/10.1007/s11517-018-1915-z
Pugazhendhi S, Ambati B, Hunter AA (2020) Pathogenesis and prevention of worsening axial elongation in pathological myopia. Clin Ophthalmol 14:853–873. https://doi.org/10.2147/OPTH.S241435
Acknowledgements
Bo Young Lee, Hee Jin Kim, and Hee Su Kim played a significant role in pre-processing data.
Author information
Authors and Affiliations
Contributions
Juntae Kim, Ik Hee Ryu, and Tae Keun Yoo had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Juntae Kim and Ik Hee Ryu contributed equally to the work presented here and should, therefore, be regarded as equivalent authors. JK, IHR, and TKY developed the algorithm. JKK, ISL, HKK, EH, and TKY consolidated data and performed data analyses. IHR and TKY drafted the manuscript. IHR and JKK conceived of and designed the study. All authors contributed to revisions and finalization of the submitted manuscript. All authors meet the following criteria: (1) substantial contributions to the conception or design of the work or the acquisition, analysis or interpretation of the data; (2) drafting the work or revising it critically for important intellectual content; (3) final approval of the completed version; and (4) accountability for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Ethical approval
All procedures of studies involving human participants were performed in accordance with the ethical standards of the Institutional Review Board of the Korean National Institute for Bioethics Policy (KoNIBP, 2019–1685-003) and the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
The Institutional Review Board waived the requirement for informed consent because the data were fully deidentified to protect patient confidentiality.
Conflict of interest
Juntae Kim is an employee of DATARIZE. Ik Hee Ryu and Jin Kuk Kim are directors of VISUWORKS, and own company stock. Ik Hee Ryu serves on the Advisory Board for Carl Zeiss Meditec AG and Avellino Lab USA/MAB for Avellino Lab Korea. Jin Kuk Kim is an executive of the Korea Intelligent Medical Industry Association (KIMIA). Tae Keun Yoo is an employee of VISUWORKS, and received a salary or stock as part of the standard compensation package. The remaining authors declare no conflicts of interest. VISUWORKS received research grants for SMILE surgery from Carl Zeiss Meditec AG. The research grants did not affect this study.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kim, J., Ryu, I.H., Kim, J.K. et al. Machine learning predicting myopic regression after corneal refractive surgery using preoperative data and fundus photography. Graefes Arch Clin Exp Ophthalmol 260, 3701–3710 (2022). https://doi.org/10.1007/s00417-022-05738-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-022-05738-y