Abstract
Background
Trauma is the leading cause of enucleations in the USA. Current information regarding open globe injuries (OGI) is based mainly on data from individual tertiary care centers across the country which might skew the findings towards the population served by these level-one trauma centers. The aim of this study is to evaluate the demographics, characteristics, and risk factors of traumatic enucleations in a large data sample.
Methods
Descriptive cross-sectional observational study using the National Inpatient Sample (NIS) Database from 2002 to 2013. Inpatients with traumatic enucleations were identified using ICD-9 codes. Chi-square and logistic regression analyses were used to identify differences between the enucleated and non-enucleated cohorts and to evaluate the predictive factors of enucleation in OGIs.
Results
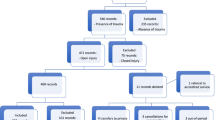
Enucleations were performed in 3020 (6.2%) of 48,563 OGIs identified. The average age in the enucleated cohort for males vs. females was 44.7 vs. 62.2 years. In the USA, the highest number of traumatic enucleations occurred in the 21–40 group (41.8%) and the fewest in the 80+ age group (11.8%). The risk of enucleation decreased across the age groups significantly. Compared with the 21–40 age group, the risk of undergoing enucleation was 15% lower in patients 41 to 60 years of age, 35% in patients 61 to 80, and 40% lower in patients over 80. In total, 5.1% OGIs in women and 6.7% of OGIs in men were enucleated. The risk of enucleation was 29% higher in men than in women. The highest absolute number of enucleations was seen in Whites. Compared with Whites, Blacks had a 63% higher risk of enucleation following an OGI. OGIs with rupture-type injury, endophthalmitis, or phthisis were significantly higher odds to be enucleated.
Conclusions
The risk of enucleation following traumatic OGI significantly increased for patients who were in the 21–40 age group, of Black race, or of male gender; the risk also increased if the injury was a rupture-type or associated with endophthalmitis or phthisis. The risk of depression was 75% higher in enucleated patients versus non-enucleated patients.





Similar content being viewed by others
References
Erie JC, Nevitt MP, Hodge D, Ballard DJ (1992) Incidence of enucleation in a defined population. Am J Ophthalmol 113(2):138–144
Setlur VJ, Parikh JG, Rao NA (2010) Changing causes of enucleation over the past 60 years. Graefes Arch Clin Exp Ophthalmol 248(4):593–597
Chan S, Wah S (2017) A decade of surgical eye removals in Ontario: a clinical-pathological study. Can J Ophthalmol 52(5):486–493
Farokhfar A, Ahmadzadeh-Amiri A, Sheikhrezaee MR, Gorji MAH, Agaei N (2017) Common causes of eye Enucleation among patients. J Nat Sci Biol Med 8(2):150–153
Savar A, Andreoli MT, Kloek CE, Andreoli CM (2009) Enucleation for open globe injury. Am J Ophthalmol 147(4):595–600
Dunn ES, Jaeger EA, Jeffers JB, Freitag SK (1992) The epidemiology of ruptured globes. Ann Ophthalmol 24(11):405–410
Klopfer J, Tielsch JM, Vitale S, See L, Canner JK (1992) Ocular trauma in the United States: eye injuries resulting in hospitalization, 1984 through 1987. Arch Ophthalmol 110(6):838–842
May DR, Kuhn FP, Morris RE, Witherspoon CD, Danis RP, Matthews GP (2000) The epidemiology of serious eye injuries from the United States eye injury registry. Graefes Arch Clin Exp Ophthalmol 238(2):153–157
Framme C, Roider J (1999) Epidemiology of open globe injuries. Klin Monatsbl Augenheilkd 215(5):287–293
Lundin AM, Azari AA, Kanavi MR, Potter HD, Lucarelli MJ, Burkat CN, Albert DM (2014) Ocular trauma resulting in Enucleation: a 12-year experience from a large regional institution. WMJ. 113(3):99–101
Emami-Naeini P, Bauza AM, Langer PD, Zarbin MA, Bhagat N (2013) Gender disparities in open globe injuries: ten-year review of an urban population. Br J Med Res 3(4):1380–1387
Burstein ES, Lazarro DR (2013) Traumatic ruptured globe eye injuries in a large urban center. Clin Ophthalmol 7:485–488
Loy KC, Obrieze A (2015) Disparities in the treatment of open globe injuries. Invest Ophthalmol Vis Sci 56(7):6035
Bauza AM, Emami P, Son JH, Langer P, Zarbin MA, Bhagat N (2013)Work-related open-globe injuries: demographics and clinical characteristics. Eur J Ophthalmol 23(2):242–248
Bauza AM, Emami P, Soni N et al (2013) A 10-year review of assault-related open-globe injuries at an urban hospital. Graefes Arch Clin Exp Ophthalmol 251:653–659
Andreoli TM, Andreoli MC (2011) Geriatric and traumatic open globe injuries. Ophthalmology. 118(1):156–159
Kavoussi SC (2015) Characteristics and outcomes of fall-related open-globe injuries in pseudophakic patients. Clin Ophthalmol 9:403–408
Sheng I, Bauza A, Langer P et al (2015) A 10-year review of open-globe trauma in elderly patients at an urban hospital. Retina. 35(1):105–110
Kolomeyer AM, Shah A, Bauza AM, Langer PD, Zarbin MA, Bhagat N (2014) Nail gun-induced open-globe injuries: a 10-year retrospective review. Retina. 34:254–261
Landen D (1990) Perforating eye injury in Allegheny County, Pennsylvania. Am J Public Health 80(9):1120–1122
Bhagat N, Li X, Bauza A, Lesniak SP (2017) Characteristics and outcomes of delayed open globe repair. Mathews J Ophthalmol 2(1):013
Katz J, Tielsch JM (1993) Lifetime prevalence of ocular injuries from the Baltimore eye survey. Arch Ophthalmol 111(11):1564–1568
Bhagat N, Turbin R, Langer P et al (2016) Approach to Management of Eyes with no light perception after open globe injury. J Ophthalmic Vis Res 11(3):313–318
Soni NG, Bauza AM, Son JH et al (2013) Open globe ocular trauma: functional outcome of eyes with no light perception at initial presentation. Retina. 33:380–386
Shah AS, Andreoli MT, Andreoli CM, Kloek C (2007) Visual recovery in patients suffering open-globe injuries caused by intraocular foreign bodies. Invest Ophthalmol Vis Sci 48(13):718
Feng K, Shen L, Pang X et al (2011)Case-control study of risk factors for no light perception after open-globe injury: eye injury vitrectomy study. Retina 31:1988–1996
Thompson JT, Parver LM, Enger CL, Mieler WF, Liggett PE (1993) Infectious endophthalmitis after penetrating injuries with retained intraocular foreign bodies. Ophthalmology. 100(10):1468–1474
Ehlers JP, Kunimoto DY, Ittoop S et al (2008) Metallic intraocular foreign bodies: characteristics, interventions, and prognostic factors for visual outcome and globe survival. Am J Ophthalmol 146(3):427–433
Loporchio D, Mukkamala L, Gorukanti K et al (2016) Intraocular foreign bodies: a review. Surv Ophthalmol 61(5):582–596
Serdarevic R (2015) The ocular trauma score as a method for the prognostic assessment of visual acuity in patients with close eye injuries. Cta informatica medica. Acta Inform Med 23(2):81–85
Shah MA, Shah SM, Gosai SR et al (2011) Comparative study of final visual outcome between open-and closed-globe injuries following surgical treatment of traumatic cataract. Greafes Arch Clin Exp Ophthalmol 249(12):1775–1781
Yu M, Yan H (2015) Prognostic factors for open globe injuries and correlation of ocular trauma score in Tianjin, China. J Ophthalmol 2015(2):345764
Ahmed Y, Schimel AM, Pathengay A et al (2012) Endophthalmitis following open-globe injuries. Eye (Lond) 26(2):212–217
Bhagat N, Li X, Zarbin MA (2016)Post-traumatic Endophthalmitis. In: Durand M, Miller J, Young L (eds) Endophthalmitis. Springer, Cham
Bhagat N, Nagori S, Zarbin MA (2011)Post-traumatic infections endophthalmitis. Surv Ophthalmol 56(3):214–251
Li X, Zarbin MA, Langer PD, Bhagat N (2018) Posttraumatic endophthalmitis: an 18-year case series. Retina. 38(1):60–71
Schrader WF (2004) Open globe injuries: epidemiological study of two eye clinics in Germany, 1981-1999. Croat Med J 45(3):268–267
Boldt HC, Pulido JS, Blodi CF, Folk JC, Weingeist TA (1989) Rural endophthalmitis. Ophthalmology. 96(12):1722–1726
Essex RW, Yi Q, Charles PG, Allen PJ (2004)Post-traumatic Endophthalmitis. Ophthalmology. 111(11):2015–2022
Jonas JB, Knorr HL, Budde WM (2000) Prognostic factors in ocular injuries caused by intraocular or retrobulbar foreign bodies. Ophthalmology. 107(5):823–828
Ferrari TM, Cardascia N, Di Gesu I, Catella N, Recchimurzo N, Boscia F (2001) Early versus late removal of retained intraocular foreign bodies. Retina. 21(1):92–93
Lu X, Ng DS, Zheng K et al (2016) Risk factors for endophthalmitis requiring evisceration or enucleation. Sci Rep 6:28100
Ye J, Lou L, Jin K et al. (2015)Vision-related quality of life and appearance concerns are associated with anxiety and depression after eye Enucleation: a cross-sectional study. Huang J, ed. PLoS One. 10(8)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
All authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ojuok, E., Uppuluri, A., Langer, P.D. et al. Predictive factors of enucleation after open globe injuries. Graefes Arch Clin Exp Ophthalmol 259, 247–255 (2021). https://doi.org/10.1007/s00417-020-04794-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-020-04794-6