Abstract
Purpose
We aimed to observe photoreceptors and outer retinal layer thickness by using an adaptive optics (AO) fundus camera and spectral domain optical coherence tomography (SD-OCT) in patients with central serous chorioretinopathy (CSC).
Methods
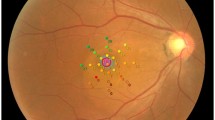
Twelve eyes of 12 patients with resolved CSC were studied. After subretinal fluid (SRF) had resolved, AO images of the macula were obtained by using the rtx1TM AO fundus camera (Imagine Eyes, France). Cones in the nasal and temporal areas of the macula, 0.5 mm from the foveal center, were counted. Outer retinal layer thickness was measured as the distance between the outer border of external limiting membrane (ELM) and the inner border of retinal pigment epithelium (RPE) at 0.5 mm from the foveal center. The first measurement was performed after resolution of the subretinal fluid and was defined as the baseline. Then, the second measurement was performed in the same location after 12 months.
Results
In the eyes with resolved CSC, the mean logMAR values of visual acuity at baseline and 12 months were 0.16 and 0.01, respectively (p = 0.0023). The mean cone densities at baseline and 12 months were 12,213 and 17,146 cones/mm2, respectively. The mean cone densities at 12 months were significantly increased compared to baseline (p = 0.0014). The mean outer retinal layer thickness at baseline (53.5 μm) was significantly thinner than that at 12 months (60.7 μm) (p = 0.0013). The mean cone densities were significantly correlated with outer retinal layer thickness and logMAR visual acuity.
Conclusions
Adaptive optics imaging revealed a gradual increase in the number of macular cone densities during 12 months in patients with resolved CSC, which was correlated with outer retinal layer thickness and visual acuity in a short term.




Similar content being viewed by others
References
Gass JD (1967) Pathogenesis of disciform detachment of the neuroepithelium. Am J Ophthalmol 63(Suppl):1–139
Klein ML, Van Buskirk EM, Friedman E, Gragoudas E, Chandra S (1974) Experience with nontreatment of central serous choroidopathy. Arch Ophthalmol 91:247–250
Yap EY, Robertson DM (1996) The long-term outcome of central serous chorioretinopathy. Arch Ophthalmol 114:689–692
Quin G, Liew G, Ho IV, Gillies M, Fraser-Bell S (2013) Diagnosis and interventions for central serous chorioretinopathy: review and update. Clin Experiment Ophthalmol 41:187–200. doi:10.1111/j.1442-9071.2012.02847.x
Piccolino FC, de la Longrais RR, Ravera G, Eandi CM, Ventre L, Abdollahi A, Manea M (2005) The foveal photoreceptor layer and visual acuity loss in central serous chorioretinopathy. Am J Ophthalmol 139:87–99. doi:10.1016/j.ajo.2004.08.037
Ojima Y, Hangai M, Sasahara M, Gotoh N, Inoue R, Yasuno Y, Makita S, Yatagai T, Tsujikawa A, Yoshimura N (2007) Three-dimensional imaging of the foveal photoreceptor layer in central serous chorioretinopathy using high-speed optical coherence tomography. Ophthalmology 114:2197–2207. doi:10.1016/j.ophtha.2007.02.015
Matsumoto H, Sato T, Kishi S (2009) Outer nuclear layer thickness at the fovea determines visual outcomes in resolved central serous chorioretinopathy. Am J Ophthalmol 148:105–110 e101. doi:10.1016/j.ajo.2009.01.018
Yalcinbayir O, Gelisken O, Akova-Budak B, Ozkaya G, Gorkem Cevik S, Yucel AA (2014) Correlation of spectral domain optical coherence tomography findings and visual acuity in central serous chorioretinopathy. Retina 34:705–712. doi:10.1097/IAE.0000000000000001
Hasegawa T, Okamoto M, Masuda N, Ueda T, Ogata N (2015) Relationship between foveal microstructures and visual outcomes in eyes with resolved central serous chorioretinopathy. Graefes Arch Clin Exp Ophthalmol 253:343–350. doi:10.1007/s00417-014-2695-2
Spaide RF, Curcio CA (2011) Anatomical correlates to the bands seen in the outer retina by optical coherence tomography: literature review and model. Retina 31:1609–1619. doi:10.1097/IAE.0b013e3182247535
Ross DH, Clark ME, Godara P, Huisingh C, McGwin G, Owsley C, Litts KM, Spaide RF, Sloan KR, Curcio CA (2015) RefMoB, a Reflectivity Feature Model-Based Automated Method for Measuring Four Outer Retinal Hyperreflective Bands in Optical Coherence Tomography. Invest Ophthalmol Vis Sci 56:4166–4176. doi:10.1167/iovs.14-15256
Hashimoto Y, Saito W, Saito M, Hirooka K, Fujiya A, Yoshizawa C, Noda K, Ishida S (2014) Retinal outer layer thickness increases after vitrectomy for epiretinal membrane, and visual improvement positively correlates with photoreceptor outer segment length. Graefes Arch Clin Exp Ophthalmol 252:219–226. doi:10.1007/s00417-013-2432-2
Hashimoto Y, Saito W, Fujiya A, Yoshizawa C, Hirooka K, Mori S, Noda K, Ishida S (2015) Changes in Inner and Outer Retinal Layer Thicknesses after Vitrectomy for Idiopathic Macular Hole: Implications for Visual Prognosis. PLoS ONE 10, e0135925. doi:10.1371/journal.pone.0135925
Terauchi G, Shinoda K, Matsumoto CS, Watanabe E, Matsumoto H, Mizota A (2015) Recovery of photoreceptor inner and outer segment layer thickness after reattachment of rhegmatogenous retinal detachment. Br J Ophthalmol 99:1323–1327. doi:10.1136/bjophthalmol-2014-306252
Rossi EA, Chung M, Dubra A, Hunter JJ, Merigan WH, Williams DR (2011) Imaging retinal mosaics in the living eye. Eye (Lond) 25:301–308. doi:10.1038/eye.2010.221
Ooto S, Hangai M, Sakamoto A, Tsujikawa A, Yamashiro K, Ojima Y, Yamada Y, Mukai H, Oshima S, Inoue T, Yoshimura N (2010) High-resolution imaging of resolved central serous chorioretinopathy using adaptive optics scanning laser ophthalmoscopy. Ophthalmology 117:1800–1809. doi:10.1016/j.ophtha.2010.01.042, 1809 e1801-1802
Zitova B, Flusser J (2003) Image registration methods: a survey. Image Vis Comput 21:977–1000. doi:10.1016/S0262-8856(03)00137-9
Bennett AG, Rudnicka AR, Edgar DF (1994) Improvements on Littmann's method of determining the size of retinal features by fundus photography. Graefes Arch Clin Exp Ophthalmol 232:361–367
Saleh M, Debellemaniere G, Meillat M, Tumahai P, Bidaut Garnier M, Flores M, Schwartz C, Delbosc B (2014) Quantification of cone loss after surgery for retinal detachment involving the macula using adaptive optics. Br J Ophthalmol 98:1343–1348. doi:10.1136/bjophthalmol-2013-304813
Park SP, Chung JK, Greenstein V, Tsang SH, Chang S (2013) A study of factors affecting the human cone photoreceptor density measured by adaptive optics scanning laser ophthalmoscope. Exp Eye Res 108:1–9. doi:10.1016/j.exer.2012.12.011
Erickson PA, Fisher SK, Anderson DH, Stern WH, Borgula GA (1983) Retinal detachment in the cat: the outer nuclear and outer plexiform layers. Invest Ophthalmol Vis Sci 24:927–942
Lewis GP, Charteris DG, Sethi CS, Fisher SK (2002) Animal models of retinal detachment and reattachment: identifying cellular events that may affect visual recovery. Eye 16:375–387. doi:10.1038/sj.eye.6700202
Lewis GP, Sethi CS, Linberg KA, Charteris DG, Fisher SK (2003) Experimental retinal reattachment: a new perspective. Mol Neurobiol 28:159–175. doi:10.1385/MN:28:2:159
Fisher SK, Lewis GP, Linberg KA, Verardo MR (2005) Cellular remodeling in mammalian retina: results from studies of experimental retinal detachment. Prog Retin Eye Res 24:395–431. doi:10.1016/j.preteyeres.2004.10.004
Sakai T, Calderone JB, Lewis GP, Linberg KA, Fisher SK, Jacobs GH (2003) Cone photoreceptor recovery after experimental detachment and reattachment: an immunocytochemical, morphological, and electrophysiological study. Invest Ophthalmol Vis Sci 44:416–425
Zhang Y, Cense B, Rha J, Jonnal RS, Gao W, Zawadzki RJ, Werner JS, Jones S, Olivier S, Miller DT (2006) High-speed volumetric imaging of cone photoreceptors with adaptive optics spectral-domain optical coherence tomography. Opt Express 14:4380–4394. doi:10.1364/OE.14.004380
Jacob J, Paques M, Krivosic V, Dupas B, Couturier A, Kulcsar C, Tadayoni R, Massin P, Gaudric A (2015) Meaning of visualizing retinal cone mosaic on adaptive optics images. Am J Ophthalmol 159:118–123 e111. doi:10.1016/j.ajo.2014.09.043
Wong RL, Lee JW, Yau GS, Wong IY (2015) Relationship between Outer Retinal Layers Thickness and Visual Acuity in Diabetic Macular Edema. Biomed Res Int 2015:981471. doi:10.1155/2015/981471
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this reserch.
Conflict of Interest
All authors have no financial interest in the subject matter or materials discussed in this manuscript.
Ethical approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and the national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
For this type of study, formal consent is not required.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Nakamura, T., Ueda-Consolvo, T., Oiwake, T. et al. Correlation between outer retinal layer thickness and cone density in patients with resolved central serous chorioretinopathy. Graefes Arch Clin Exp Ophthalmol 254, 2347–2354 (2016). https://doi.org/10.1007/s00417-016-3403-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-016-3403-1