Abstract
Background
Multiple system atrophy (MSA) is an adult onset, fatal neurodegenerative disease. However, no reliable biomarker is currently available to guide clinical diagnosis and help to determine the prognosis. Thus, a comprehensive meta-analysis is warranted to determine effective biomarkers for MSA and provide useful guidance for clinical diagnosis.
Methods
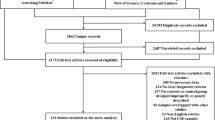
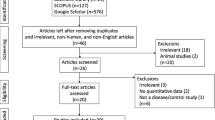
A comprehensive literature search was made of the PubMed, Embase, Cochrane and Web of Science databases for relevant clinical trial articles for 1984–2019. Two review authors examined the full-text records, respectively, and determined which studies met the inclusion criteria. We estimated the mean difference, standard deviation and 95% confidence intervals.
Results
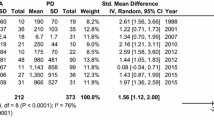
A total of 28 studies and 11 biomarkers were included in our analysis. Several biomarkers were found to be useful to distinguish MSA patients from healthy controls, including the reduction of phosphorylated tau, α-synuclein (α-syn), 42-amino-acid form of Aβ and total tau (t-tau), the elevation of neurofilament light-chain protein (NFL) in cerebrospinal fluid, the elevation of uric acid and reduction of homocysteine and coenzyme Q10 in plasma. Importantly, α-syn, NFL and t-tau could be used to distinguish MSA from Parkinson’s disease (PD), indicating that these three biomarkers could be useful biomarkers in MSA diagnosis.
Conclusion
The findings of our meta-analysis demonstrated diagnostic biomarkers for MSA. Moreover, three biomarkers could be used in differential diagnosis of MSA and PD. The results could be helpful for the early diagnosis of MSA and the accuracy of MSA diagnosis.




Similar content being viewed by others
References
Gilman S et al (2008) Second consensus statement on the diagnosis of multiple system atrophy. Neurology 71(9):670–676
Fanciulli A, Wenning GK (2015) Multiple-system atrophy. N Engl J Med 372(3):249–263
Zhang L et al (2018) Brain morphological alteration and cognitive dysfunction in multiple system atrophy. Quant Imaging Med Surg 8(10):1030–1038
Multiple-System Atrophy Research Collaboration (2013) Mutations in COQ2 in familial and sporadic multiple-system atrophy. N Engl J Med 369(3):233–244
Stefanova N et al (2009) Multiple system atrophy: an update. Lancet Neurol 8(12):1172–1178
Nuber S et al (2018) Abrogating native alpha-synuclein tetramers in mice causes a l-DOPA-responsive motor syndrome closely resembling Parkinson's disease. Neuron 100(1):75–90 (e4)
Wong YC, Krainc D (2017) Alpha-synuclein toxicity in neurodegeneration: mechanism and therapeutic strategies. Nat Med 23(2):1–13
Mondello S et al (2014) CSF alpha-synuclein and UCH-L1 levels in Parkinson's disease and atypical parkinsonian disorders. Parkinsonism Relat Disord 20(4):382–387
Wang Y et al (2012) Phosphorylated alpha-synuclein in Parkinson's disease. Sci Transl Med 4(121):121ra20
Magdalinou NK et al (2015) A panel of nine cerebrospinal fluid biomarkers may identify patients with atypical parkinsonian syndromes. J Neurol Neurosurg Psychiatry 86(11):1240–1247
Shi M et al (2011) Cerebrospinal fluid biomarkers for Parkinson disease diagnosis and progression. Ann Neurol 69(3):570–580
Chen D et al (2015) Contra-directional expression of serum homocysteine and uric acid as important biomarkers of multiple system atrophy severity: a cross-sectional study. Front Cell Neurosci 9:247
Mitsui J et al (2016) Plasma coenzyme Q10 levels in patients with multiple system atrophy. JAMA Neurol 73(8):977–980
Moher D et al (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol 62(10):1006–1012
Xu M et al (2017) Oxidative damage induced by arsenic in mice or rats: a systematic review and meta-analysis. Biol Trace Elem Res 176(1):154–175
Crippa A, Orsini N (2016) Dose–response meta-analysis of differences in means. BMC Med Res Methodol 16:91
Aerts MB et al (2012) CSF alpha-synuclein does not differentiate between parkinsonian disorders. Neurobiol Aging 33(2):430 (e1–3)
Bech S et al (2012) Amyloid-related biomarkers and axonal damage proteins in parkinsonian syndromes. Parkinsonism Relat Disord 18(1):69–72
Cao B et al (2013) Uric acid is associated with the prevalence but not disease progression of multiple system atrophy in Chinese population. J Neurol 260(10):2511–2515
Constantinescu R et al (2010) Consecutive analyses of cerebrospinal fluid axonal and glial markers in Parkinson's disease and atypical Parkinsonian disorders. Parkinsonism Relat Disord 16(2):142–145
Du J et al (2018) Clinical correlates of decreased plasma coenzyme Q10 levels in patients with multiple system atrophy. Parkinsonism Relat Disord 57:58–62
Guo Y et al (2017) Serum Klotho, vitamin D, and homocysteine in combination predict the outcomes of Chinese patients with multiple system atrophy. CNS Neurosci Ther 23(8):657–666
Hall S et al (2018) Cerebrospinal fluid concentrations of inflammatory markers in Parkinson's disease and atypical parkinsonian disorders. Sci Rep 8(1):13276
Hall S et al (2012) Accuracy of a panel of 5 cerebrospinal fluid biomarkers in the differential diagnosis of patients with dementia and/or parkinsonian disorders. Arch Neurol 69(11):1445–1452
Hansson O et al (2017) Blood-based NfL: a biomarker for differential diagnosis of parkinsonian disorder. Neurology 88(10):930–937
Herbert MK et al (2015) CSF neurofilament light chain but not FLT3 ligand discriminates Parkinsonian disorders. Front Neurol 6:91
Herbert MK et al (2014) CSF levels of DJ-1 and tau distinguish MSA patients from PD patients and controls. Parkinsonism Relat Disord 20(1):112–115
Holmberg B et al (2003) Cerebrospinal fluid Abeta42 is reduced in multiple system atrophy but normal in Parkinson's disease and progressive supranuclear palsy. Mov Disord 18(2):186–190
Holmberg B et al (2001) CSF-neurofilament and levodopa tests combined with discriminant analysis may contribute to the differential diagnosis of Parkinsonian syndromes. Parkinsonism Relat Disord 8(1):23–31
Lee PH et al (2006) The plasma alpha-synuclein levels in patients with Parkinson's disease and multiple system atrophy. J Neural Transm (Vienna) 113(10):1435–1439
Mollenhauer B et al (2011) Alpha-synuclein and tau concentrations in cerebrospinal fluid of patients presenting with parkinsonism: a cohort study. Lancet Neurol 10(3):230–240
Sakuta H et al (2017) Serum uric acid levels in Parkinson's disease and related disorders. Brain Behav 7(1):e00598
Starhof C et al (2018) Cerebrospinal fluid pro-inflammatory cytokines differentiate parkinsonian syndromes. J Neuroinflamm 15(1):305
Sun ZF et al (2014) Increase of the plasma alpha-synuclein levels in patients with multiple system atrophy. Mov Disord 29(3):375–379
Tullberg M et al (1998) CSF neurofilament and glial fibrillary acidic protein in normal pressure hydrocephalus. Neurology 50(4):1122–1127
Zhou L et al (2016) Oxidative stress and environmental exposures are associated with multiple system atrophy in chinese patients. Can J Neurol Sci 43(5):703–709
Olsson B et al (2013) The glial marker YKL-40 is decreased in synucleinopathies. Mov Disord 28(13):1882–1885
Silajdzic E et al (2014) Flt3 ligand does not differentiate between Parkinsonian disorders. Mov Disord 29(10):1319–1322
Eller M, Williams DR (2009) Biological fluid biomarkers in neurodegenerative parkinsonism. Nat Rev Neurol 5(10):561–570
Barbour R et al (2008) Red blood cells are the major source of alpha-synuclein in blood. Neurodegener Dis 5(2):55–59
Scherzer CR et al (2008) GATA transcription factors directly regulate the Parkinson's disease-linked gene alpha-synuclein. Proc Natl Acad Sci USA 105(31):10907–10912
Bougea A et al (2019) Plasma alpha-synuclein levels in patients with Parkinson's disease: a systematic review and meta-analysis. Neurol Sci 40(5):929–938
Khalil M et al (2018) Neurofilaments as biomarkers in neurological disorders. Nat Rev Neurol 14(10):577–589
Bacioglu M et al (2016) Neurofilament light chain in blood and CSF as marker of disease progression in mouse models and in neurodegenerative diseases. Neuron 91(2):494–496
Ge F et al (2018) Cerebrospinal fluid NFL in the differential diagnosis of parkinsonian disorders: a meta-analysis. Neurosci Lett 685:35–41
Marques TM et al (2019) Serum NFL discriminates Parkinson disease from atypical parkinsonisms. Neurology 92(13):e1479–e1486
Wilke C et al (2018) Serum neurofilament light is increased in multiple system atrophy of cerebellar type and in repeat-expansion spinocerebellar ataxias: a pilot study. J Neurol 265(7):1618–1624
Rodriguez-Martin T et al (2013) Tau phosphorylation affects its axonal transport and degradation. Neurobiol Aging 34(9):2146–2157
Schrag A et al (2017) Clinical variables and biomarkers in prediction of cognitive impairment in patients with newly diagnosed Parkinson's disease: a cohort study. Lancet Neurol 16(1):66–75
Ritchie C et al (2017) CSF tau and the CSF tau/ABeta ratio for the diagnosis of Alzheimer's disease dementia and other dementias in people with mild cognitive impairment (MCI). Cochrane Database Syst Rev 3:CD010803
Brouillette AM, Oz G, Gomez CM (2015) Cerebrospinal fluid biomarkers in spinocerebellar ataxia: a pilot study. Dis Markers 2015:413098
Zhang J et al (2013) Longitudinal assessment of tau and amyloid beta in cerebrospinal fluid of Parkinson disease. Acta Neuropathol 126(5):671–682
Sussmuth SD et al (2010) Differential pattern of brain-specific CSF proteins tau and amyloid-beta in Parkinsonian syndromes. Mov Disord 25(9):1284–1288
Qiang X et al (2017) DL-3-n-butylphthalide-Edaravone hybrids as novel dual inhibitors of amyloid-beta aggregation and monoamine oxidases with high antioxidant potency for Alzheimer's therapy. Bioorg Med Chem Lett 27(4):718–722
Schwarzschild MA et al (2014) Inosine to increase serum and cerebrospinal fluid urate in Parkinson disease: a randomized clinical trial. JAMA Neurol 71(2):141–150
Lee JE et al (2011) Uric acid as a potential disease modifier in patients with multiple system atrophy. Mov Disord 26(8):1533–1536
Boldyrev A et al (2013) Why is homocysteine toxic for the nervous and immune systems? Curr Aging Sci 6(1):29–36
Funding
This study was funded by the “Liaoning BaiQianWan Talents Program” and was also sponsored by Shenyang Science and technology plan project (19-112-4-045) and 345 Talent Project of Shengjing Hospital of China Medical University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical standards
This article does not contain any studies with human participants or animals performed by any of the authors.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Cong, S., Xiang, C., Wang, H. et al. Diagnostic utility of fluid biomarkers in multiple system atrophy: a systematic review and meta-analysis. J Neurol 268, 2703–2712 (2021). https://doi.org/10.1007/s00415-020-09781-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-020-09781-9