Abstract
Objective
The causative and prognostic roles of human papillomavirus (HPV) in non-oropharyngeal squamous cell carcinoma of the head and neck are uncertain. This umbrella review assessed the strength and quality of evidence and graded the evidence derived from published meta-analyses on this subject.
Data sources: MEDLINE, Embase, and the Cochrane Library were searched. Meta-analyses of observational studies and randomized trials were included.
Review methods: Evidence of association was graded according to the established criteria: strong, highly suggestive, suggestive, weak, or not significant.
Results
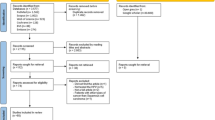
15 meta-analyses were evaluated. The association with HPV was highly suggestive of oral (OR = 2.40, [1.87–3.07], P < 0.00001) and nasopharyngeal cancers (OR = 17.82 [11.20–28.35], P < 0.00001). Improved survival emerged only in hypopharyngeal carcinoma and was confirmed in studies in which only p16 + cancers were considered.
Conclusion
HPV infection may increase the risk of oral cavity and nasopharyngeal cancer. However, the prognosis was not influenced, except in hypopharyngeal carcinoma.



Similar content being viewed by others
References
Zakeri K, Dunn L, Lee N (2021) HPV-associated oropharyngeal cancer de-escalation strategies and trials: Past failures and future promise. J Surg Oncol 124(6):962–966
Marur S, D’Souza G, Westra WH, Forastiere AA (2010) HPV-associated head and neck cancer: a virus-related cancer epidemic. Lancet Oncol 11:781–789
Wu Q, Wang M, Liu Y et al (2021) HPV positive status is a favorable prognostic factor in non-nasopharyngeal head and neck squamous cell carcinoma patients: a retrospective study from the surveillance, epidemiology, and end results database. Front Oncol 11:688615
Petrelli F, Luciani A, Ghidini A et al (2022) Treatment de-escalation for HPV+ oropharyngeal cancer: a systematic review and meta-analysis. Head Neck 44:1255–1266
Tachezy R, Klozar J, Rubenstein L et al (2009) Demographic and risk factors in patients with head and neck tumors. J Med Virol 81:878–887
Sahovaler A, Kim MH, Mendez A et al (2020) Survival outcomes in human papillomavirus-associated nonoropharyngeal squamous cell carcinomas. JAMA Otolaryngol Head Neck Surg 146(12):1–9
Liu H, Li J, Diao M, Cai Z, Yang J, Zeng Y (2013) Statistical analysis of human papillomavirus in a subset of upper aerodigestive tract tumors: human papillomavirus and tumors. J Med Virol 85:1775–1785
Liu H, Li J, Zhou Y, Hu Q, Zeng Y, Mohammadreza MM (2017) Human papillomavirus as a favorable prognostic factor in a subset of head and neck squamous cell carcinomas: a meta-analysis. J Med Virol 89:710–725
Zhu Y, Xia X, Gao L et al (2019) Prognostic implications of human papillomavirus type 16 status in non-oropharyngeal head and neck cancer: a propensity score matching analysis. Ann Trans Med 7:759
Young RJ, Urban D, Angel C et al (2015) Frequency and prognostic significance of P16(INK4A) protein overexpression and transcriptionally active human papillomavirus infection in laryngeal squamous cell carcinoma. Brit J Cancer 112:1098–1104
Nauta IH, Heideman DAM, Brink A et al (2021) The unveiled reality of human papillomavirus as risk factor for oral cavity squamous cell carcinoma. Int J Cancer 149:420–430
Clayman GL, Stewart MG, Weber RS, El-Naggar AK, Grimm EA (1994) Human papillomavirus in laryngeal and hypopharyngeal carcinomas: relationship to survival. Arch Otolaryngol-Head Neck Surg 120:743–748
Duray A, Descamps G, Decaestecker C et al (2012) Human papillomavirus DNA strongly correlates with a poorer prognosis in oral cavity carcinoma. Laryngoscope 122:1558–1565
Lee L, Huang C, Liao C et al (2012) Human papillomavirus-16 infection in advanced oral cavity cancer patients is related to an increased risk of distant metastases and poor survival. PLoS ONE 7:e40767
Papatheodorou S (2019) Umbrella reviews: what they are and why we need them. Eur J Epidemiol 34:543–546
Shea BJ, Grimshaw JM, Wells GA et al (2007) Development of AMSTAR: a measurement tool to assess the methodological quality of systematic reviews. BMC Med Res Methodol 7:10
Ahmadi N, Ahmadi N, Chan MV, Huo YR, Sritharan N, Chin R (2018) Laryngeal squamous cell carcinoma survival in the context of human papillomavirus: a systematic review and meta-analysis. Cureus 10:e2234
Chaitanya N, Allam N, Gandhi Babu D, Waghray S, Badam R, Lavanya R (2016) Systematic meta-analysis on association of human papilloma virus and oral cancer. J Cancer Res Ther 12:969–974
Shi J, Wang L, Yao N et al (2022) The effect of HPV DNA and p16 status on the prognosis of patients with hypopharyngeal carcinoma: a meta-analysis. BMC Cancer 22:1–10
Sun L, Song J, Huang Q (2019) Clinicopathological and prognostic significance of p16 protein in nasopharynx cancer patients. Med (United States) 98:e14602
Tham T, Teegala S, Bardash Y, Herman SW, Costantino P (2018) Is human papillomavirus and p16 expression associated with survival outcomes in nasopharyngeal cancer? A systematic review and meta-analysis. Am J Otolaryngol Head Neck Med Surg 39:764–770
Wang H, Wei J, Wang B et al (2020) Role of human papillomavirus in laryngeal squamous cell carcinoma: a meta-analysis of cohort study. Cancer Med 9:204–214
Zhang C, Deng Z, Chen Y, Suzuki M, Xie M (2016) Is there a higher prevalence of human papillomavirus infection in Chinese laryngeal cancer patients? A systematic review and meta-analysis. Eur Arch Oto-Rhino-Laryngology 273:295–303
Christianto S, Li KY, Huang TH, Su YX. The prognostic value of human papilloma virus infection in oral cavity squamous cell carcinoma: a meta-analysis. Laryngoscope. 2021:1–11.
Giraldi L, Collatuzzo G, Hashim D et al (2021) Infection with human papilloma virus (HPV) and risk of subsites within the oral cancer. Cancer Epidemiol 75:102020
McLaughlin L, Bultas M, Shorey S (2012) Human papillomavirus and head and neck cancer. J Nurse Pract 8:663–664
Li X, Gao L, Li H et al (2013) Human papillomavirus infection and laryngeal cancer risk: a systematic review and meta-analysis. J Infect Dis 207:479–488
O’Rorke MA, Ellison MV, Murray LJ, Moran M, James J, Anderson LA (2012) Human papillomavirus related head and neck cancer survival: a systematic review and meta-analysis. Oral Oncol 48:1191–1201
Saulle R, Semyonov L, Mannocci A et al (2015) Human papillomavirus and cancerous diseases of the head and neck: a systematic review and meta-analysis. Oral Dis 21:417–431
Liu CY, Li F, Zeng Y et al (2015) Infection and integration of high-risk human papillomavirus in HPV-associated cancer cells. Med Oncol 32:109
Taberna M, Mena M, Pavón MA, Alemany L, Gillison ML, Mesía R (2017) Human papillomavirus-related oropharyngeal cancer. Ann Oncol 28:2386–2398
Arambula A, Brown JR, Neff L (2021) Anatomy and physiology of the palatine tonsils, adenoids, and lingual tonsils. World J Otorhinolaryngol Head Neck Surg 7:155–160
Andersen AS, Koldjaer Sølling AS, Ovesen T, Rusan M (2014) The interplay between HPV and host immunity in head and neck squamous cell carcinoma: interplay between HPV and host immunity in HNSCC. Int J Cancer 134:2755–2763
Avril D, Foy JP, Bouaoud J, Grégoire V, Saintigny P. Biomarkers of radioresistance in head and neck squamous cell carcinomas. International Journal of Radiation Biology. 2022;0:1–20.
National Comprehensive Cancer Network. Head and Neck Cancers (Version 2.2022). https://www.nccn.org/professionals/physician_gls/pdf/head-and-neck.pdf Accessed 07 Aug 2022
Lucioni M, Marioni G, Bertolin A, Giacomelli L, Rizzotto G (2011) Glottic laser surgery: outcomes according to 2007 ELS classification. Eur Arch Otorhinolaryngol 268:1771–1778
Succo G, Crosetti E, Bertolin A et al (2016) Benefits and drawbacks of open partial horizontal laryngectomies, Part A: Early- to intermediate-stage glottic carcinoma. Head Neck 38(Suppl 1):E333-340
Succo G, Crosetti E, Bertolin A et al (2016) Benefits and drawbacks of open partial horizontal laryngectomies, Part B: Intermediate and selected advanced stage laryngeal carcinoma. Head Neck 38(Suppl 1):E649-657
Patel EJ, Oliver JR, Jacobson AS et al (2022) Human papillomavirus in patients with hypopharyngeal squamous cell carcinoma. Otolaryngol Head Neck Surg 166:109–117
Gatta G, Botta L, Sanchez MJ, et al. Prognoses and improvement for head and neck cancers diagnosed in Europe in early 2000s: the EUROCARE-5 population-based study. Eur J Cancer. 2015; 51:2130–2143.1.
Chen YP, Chan ATC, Le QT, Blanchard P, Sun Y, Ma J (2019) Nasopharyngeal carcinoma. The Lancet 394(64–80):1
Huang SH, Jacinto JCK, O’Sullivan B et al (2022) Clinical presentation and outcome of human papillomavirus-positive nasopharyngeal carcinoma in a North American cohort. Cancer 128:2908–2921
Hernandez BY, Lynch CF, Chan OTM, et al; HPV Typing of Cancer Workgroup. Human papillomavirus DNA detection, p16INK4a, and oral cavity cancer in a U.S. population. Oral Oncol. 2019;91:92–96.
Menegaldo A, Schroeder L, Holzinger D et al (2021) Detection of HPV16/18 E6 oncoproteins in head and neck squamous cell carcinoma using a protein immunochromatographic assay. Laryngoscope 131:1042–1048
Alotaibi M, Valova V, Hänsel T et al (2021) Impact of smoking on the survival of patients with high-risk HPV-positive HNSCC: a meta-analysis. In Vivo 35:1017–1026
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
All authors contributed equally.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Petrelli, F., Cin, E.D., Ghidini, A. et al. Human papillomavirus infection and non-oropharyngeal head and neck cancers: an umbrella review of meta-analysis. Eur Arch Otorhinolaryngol 280, 3921–3930 (2023). https://doi.org/10.1007/s00405-023-08027-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-023-08027-4