Abstract
Purpose
Septoplasty is a common rhinological procedure intended to relieve symptoms of chronic nasal obstruction. However, there remains a question as to whether patients obtain symptom improvement and are satisfied with surgical outcomes in the months and years after septoplasty. This review aims to evaluate the long-term efficacy of functional septoplasty for nasal septal deviation.
Methods
A systematic review of the literature was conducted from November 2014 to March 2016 using the Cochrane, EMBASE, and PubMed databases. Prospective trials concerning functional septoplasty, which assessed subjective outcomes and included long-term follow-up data (≥ 9 month post-septoplasty) were included.
Results
2189 articles were screened with seven meeting the criteria for inclusion. Patient satisfaction was assessed in six studies, with rates of satisfaction provided in three of these, ranging from 69 to 100%. Two studies assessed the degree of patient satisfaction, with one study indicating that 88% of patients were moderately satisfied or better at 1 year post-op, and the other reporting that 50% of patients were satisfied. In assessing symptom relief, several methods were used, including validated questionnaires, with varying degrees of improvement in nasal obstruction reported.
Conclusions
Septoplasty appears to be a far from perfect treatment for nasal obstruction due to septal deviation. However, given the heterogeneity of data and lack of randomized controlled trials (RCTs), future RCTs and use of validated questionnaires would enable generation of superior levels of evidence. We suggest future prospective trials evaluating prognostic factors in septoplasty, to better inform patients and facilitate the development of guidelines for surgical intervention.



Similar content being viewed by others
References
Vainio-Mattila J (1974) Correlations of nasal symptoms and signs in random sampling study. Acta Otolaryngol Suppl 318:1–48
Bhattacharyya N (2010) Ambulatory sinus and nasal surgery in the United States: demographics and perioperative outcomes. Laryngoscope 120(3):635–638
Ahn JC et al (2016) Prevalence and risk factors of chronic rhinosinusitus, allergic rhinitis, and nasal septal deviation: results of the Korean national health and nutrition survey 2008–2012. JAMA Otolaryngol Head Neck Surg 142(2):162–167
Salihoglu M et al (2014) Examination versus subjective nasal obstruction in the evaluation of the nasal septal deviation. Rhinology 52(2):122–126
Stefanini R et al (2012) Systematic evaluation of the upper airway in the adult population of Sao Paulo, Brazil. Otolaryngol Head Neck Surg 146(5):757–763
Stewart MG et al (2004) Development and validation of the Nasal Obstruction Symptom Evaluation (NOSE) scale. Otolaryngol Head Neck Surg 130(2):157–163
Rhee JS, McMullin BT (2008) Outcome measures in facial plastic surgery: patient-reported and clinical efficacy measures. Arch Facial Plast Surg 10(3):194–207
Swedish Association of Local Authorities and Regions, S.N.B.o.H.a.W. (2013) Quality and Efficiency in Swedish Health Care—Regional Comparisons 2012, S.N.B.o.H.a. Welfare, Editor. Ordförrådet AB, Stockholm
Andrews PJ et al (2015) The need for an objective measure in septorhinoplasty surgery: are we any closer to finding an answer? Clin Otolaryngol 40(6):698–703
Moore, M. and R. Eccles (2011) Objective evidence for the efficacy of surgical management of the deviated septum as a treatment for chronic nasal obstruction: a systematic review. Clin Otolaryngol 36(2):106–113
Sipila J, Suonpaa J (1997) A prospective study using rhinomanometry and patient clinical satisfaction to determine if objective measurements of nasal airway resistance can improve the quality of septoplasty. Eur Arch Otorhinolaryngol 254(8):387–390
Tompos T et al (2010) Sensation of nasal patency compared to rhinomanometric results after septoplasty. Eur Arch Oto Rhino Laryngo 267(12):1887–1891
Kjaergaard T, Cvancarova M, Steinsvag SK (2009) Nasal congestion index: a measure for nasal obstruction. Laryngoscope 119(8):1628–1632
Larsen K, Oxhoj H (1988) Spirometric forced volume measurements in the assessment of nasal patency after septoplasty. A prospective clinical study. Rhinology 26(3):203–208
Kimbell JS et al (2012) Computed nasal resistance compared with patient-reported symptoms in surgically treated nasal airway passages: a preliminary report. Am J Rhinol Allergy 26(3):e94–e98
Murrell GL (2014) Correlation between subjective and objective results in nasal surgery. Aesthet Surg J 34(2):249–257
Constantinides MS, Adamson PA, Cole P (1996) The long-term effects of open cosmetic septorhinoplasty on nasal air flow. Arch Otolaryngol Head Neck Surg 122(1):41–45
Kahveci OK et al (2012) The efficiency of Nose Obstruction Symptom Evaluation (NOSE) scale on patients with nasal septal deviation. Auris Nasus Larynx 39(3):275–279
Daudia A et al (2006) A prospective objective study of the cosmetic sequelae of nasal septal surgery. Acta Otolaryngol 126(11):1201–1205
Hsu HC et al (2017) Evaluation of nasal patency by visual analogue scale/nasal obstruction symptom evaluation questionnaires and anterior active rhinomanometry after septoplasty: a retrospective one-year follow-up cohort study. Clin Otolaryngol 42(1):53–59
Andre RF et al (2009) Correlation between subjective and objective evaluation of the nasal airway. A systematic review of the highest level of evidence. Clin Otolaryngol 34(6):518–525
Arunachalam PS et al (2001) Nasal septal surgery: evaluation of symptomatic and general health outcomes. Clin Otolaryngol Allied Sci 26(5):367–370
Jessen M, Ivarsson A, Malm L (1989) Nasal airway resistance and symptoms after functional septoplasty: comparison of findings at 9 months and 9 years. Clin Otolaryngol Allied Sci 14(3):231–234
Bohlin L, Dahlqvist A (1994) Nasal airway resistance and complications following functional septoplasty: a ten-year follow-up study. Rhinology 32(4):195–197
De Sousa Fontes A, Sandrea Jimenez M, Chacaltana Ayerve RR (2013) Endoscopic septoplasty in primary cases using electromechanical instruments: surgical technique, efficacy and results. Acta Otorrinolaringol Esp 64(5):317–322
Haroon Y, Saleh HA, Abou-Issa AH (2013) Nasal soft tissue obstruction improvement after septoplasty without turbinectomy. Eur Arch Otorhinolaryngol 270(10):2649–2655
Illum P (1997) Septoplasty and compensatory inferior turbinate hypertrophy: long-term results after randomized turbinoplasty. Eur Arch Oto Rhino Laryngol 254(Suppl 1):S89–S92
Konstantinidis I et al (2005) Long term results following nasal septal surgery. Focus on patients’ satisfaction. Auris Nasus Larynx 32(4):369–374
Pirila T, Tikanto J (2001) Unilateral and bilateral effects of nasal septum surgery demonstrated with acoustic rhinometry, rhinomanometry, and subjective assessment. Am J Rhinol 15(2):127–133
Meltzer EO et al (2006) Rhinosinusitis: developing guidance for clinical trials. Otolaryngol Head Neck Surg 135(5 Suppl):S31–S80
Anderson K et al (2016) The impact of septoplasty on health-related quality of life in paediatric patients. Clin Otolaryngol 41(2):144–148
Hong SD et al (2015) Predictive factors of subjective outcomes after septoplasty with and without turbinoplasty: can individual perceptual differences of the air passage be a main factor? Int Forum Allergy Rhinol 5(7):616–621
Lipan MJ, Most SP (2013) Development of a severity classification system for subjective nasal obstruction. JAMA Facial Plast Surg 15(5):358–361
Holmstrom M (2010) The use of objective measures in selecting patients for septal surgery. Rhinology 48(4):387–393
Sedaghat AR et al (2013) Clinical assessment is an accurate predictor of which patients will need septoplasty. Laryngoscope 123(1):48–52
Han JK et al (2015) Clinical consensus statement: septoplasty with or without inferior turbinate reduction. Otolaryngol Head Neck Surg 153(5):708–720
Dinis PB, Haider H (2002) Septoplasty: long-term evaluation of results. Am J Otolaryngol 23(2):85–90
Gandomi B, Bayat A, Kazemei T (2010) Outcomes of septoplasty in young adults: the Nasal Obstruction Septoplasty Effectiveness study. Am J Otolaryngol 31(3):189–192
Siegel NS et al (2000) Outcomes of septoplasty. Otolaryngol Head Neck Surg 122(2):228–232
Zeng R et al (2014) Univariate and multivariate analyses for postoperative bleeding after nasal endoscopic surgery. Acta Otolaryngol 134(5):520–524
Karatzanis AD et al (2009) Septoplasty outcome in patients with and without allergic rhinitis. Rhinology 47(4):444–449
Mondina M et al (2012) Assessment of nasal septoplasty using NOSE and RhinoQoL questionnaires. Eur Arch Otorhinolaryngol 269(10):2189–2195
Bothra R, Mathur NN (2009) Comparative evaluation of conventional versus endoscopic septoplasty for limited septal deviation and spur. J Laryngol Otol 123(7):737–741
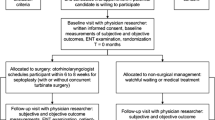
van Egmond MM et al (2015) Effectiveness of septoplasty versus non-surgical management for nasal obstruction due to a deviated nasal septum in adults: study protocol for a randomized controlled trial. Trials 16:500
Prus-Ostaszewska M et al (2017) The correlation of the results of the survey SNOT-20 of objective studies of nasal obstruction and the geometry of the nasal cavities. Otolaryngol Pol 71(2):1–7
Hopkins C et al (2009) Psychometric validity of the 22-item Sinonasal Outcome Test. Clin Otolaryngol 34(5):447–454
Piccirillo JF, Merritt Jr MG, Richards ML (2002) Psychometric and clinimetric validity of the 20-Item Sino-Nasal Outcome Test (SNOT-20). Otolaryngol Head Neck Surg 126(1):41–47
Robinson K, Gatehouse S, Browning GG (1996) Measuring patient benefit from otorhinolaryngological surgery and therapy. Ann Otol Rhinol Laryngol 105(6):415–422
Bugten V et al (2016) Quality of life and symptoms before and after nasal septoplasty compared with healthy individuals. BMC Ear Nose Throat Disord 16:13.
Sundh C, Sunnergren O (2015) Long-term symptom relief after septoplasty. Eur Arch Otorhinolaryngol 272(10):2871–2875
Acknowledgements
Mr. Lars Eriksson for his expertise in generating search criteria. Dr. Emma Badenoch-Jones for her guidance and support in the systematic review of journal articles.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Conflict of interest
The authors do not have any financial conflicts of interest. One author is a practicing Otolaryngologist who performs septoplasty as a non-financial conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tsang, C.L.N., Nguyen, T., Sivesind, T. et al. Long-term patient-related outcome measures of septoplasty: a systematic review. Eur Arch Otorhinolaryngol 275, 1039–1048 (2018). https://doi.org/10.1007/s00405-018-4874-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-018-4874-y