Abstract
Purpose
To compare the clinical outcome of fresh embryo transfer with frozen-thawed embryo transfer in subsequent cycle of GnRH antagonist protocol.
Methods
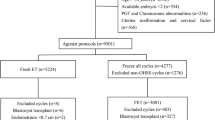
Totally, 1430 women were enrolled from the cases of our Assisted Reproduction Center from January 2015 to January 2019 for this retrospective cohort study. The inclusion criteria of the subjects included women with ages under 40 years, 3–10 oocytes retrieved, good embryo quality according to gardener score, GnRH antagonist protocol, underwent first cycle of fresh embryo transfer or freeze-all strategy and transferred in subsequent cycle. However, the patients with endometriosis, PGD/PGS cycles, history of recurrent pregnancy loss and uterine pathology were excluded. 495 women of group I underwent fresh embryo transfer in first cycle and 935 patients of group II received frozen-thawed transfer in subsequent cycle. The primary outcome was clinical pregnancy rate. A logistic regression analysis was performed to determine the variables that could be independently associated with clinical pregnancy rate. Models were adjusted for covariates including patients’ age, fertilization type, infertility type, infertility duration, the number of oocytes retrieved, the number of embryos transferred and type of embryo transferred.
Results
Clinical pregnancy rate was significantly higher in frozen-thawed embryo transfer than in fresh embryo transfer (63.70% vs. 54.50%, p < 0.001). Miscarriage rate and ectopic pregnancy rate were comparable between two groups. Variables independently associated with clinical pregnancy rate were fresh/frozen embryo transfer, patients’ age and the number of embryos transferred. After adjusting for variables, the frozen embryo transfer [adjusted odds ratio (aOR) 0.75; 95% CI, 0.59–0.95, p = 0.016] was a predictive factor of clinical pregnancy rate.
Conclusion
Frozen embryo transfer is better than fresh embryo transfer in GnRH antagonist cycle in women with 3–10 oocytes retrieved.
Similar content being viewed by others
References
Shapiro BS, Daneshmand ST, Garner FC (2011) Evidence of impaired endometrial receptivity after ovarian stimulation for in vitro fertilization: a prospective randomized trial comparing fresh and frozen-thawed embryo transfer in normal responders. Fertil Steril 96(2):344–348
Shapiro BS, Daneshmand ST, Garner FC (2014) Clinical rationale for cryopreservation of entire embryo cohorts in lieu of fresh transfer. Fertil Steril 102(1):3–9
Evans J, Hannan NJ, Edgell TA (2014) Fresh versus frozen embryo transfer: backing clinical decisions with scientific and clinical evidence. Hum Reprod Update 20(6):808–821
Pelkonen S, Koivunen R, Gissler M (2010) Perinatal outcome of children born after frozen and fresh embryo transfer: the Finnish cohort study 1995–2006. Hum Reprod 25(4):914–923
Depalo R, Jayakrishan K, Garruti G (2012) GnRH agonist versus GnRH antagonist in in vitro fertilization and embryo transfer (IVF/ET). Reprod Biol Endocrinol 10(4):26
Roque M, Valle M, Guimaraes F (2015) Freeze-all policy: fresh vs. frozen-thawed embryo transfer. Fertil Steril 103(5):1190–1193
Aflatoonian AM-TM, Mojtahedi MF (2018) Fresh versus frozen embryo transfer after gonadotropinreleasing hormone agonist trigger in gonadotropinreleasing hormone antagonist cycles among high responder women: a randomized, multi-center study. Int J Reprod Biomed (Yazd) 16(1):9–18
Kol S, Lightman A, Hillensjo T (1999) High doses of gonadotrophin-releasing hormone antagonist in in-vitro fertilization cycles do not adversely affect the outcome of subsequent freeze-thaw cycles. Hum Reprod 14(9):2242–2244
Zikopoulos K, Kolibianakis EM, Camus M (2004) Duration of gonadotropin-releasing hormone antagonist administration does not affect the outcome of subsequent frozen-thawed cycles. Fertil Steril 81(2):473–475
Garcia JE, Acosta AA, Hsiu JG (1984) Advanced endometrial maturation after ovulation induction with human menopausal gonadotropin/human chorionic gonadotropin for in vitro fertilization. Fertil Steril 41(1):31–35
Kolb BA, Paulson RJ (1997) The luteal phase of cycles utilizing controlled ovarian hyperstimulation and the possible impact of this hyperstimulation on embryo implantation. Am J Obstet Gynecol 176(6):1262–1267
Mirkin S, Nikas G, Hsiu JG (2004) Gene expression profiles and structural/functional features of the peri-implantation endometrium in natural and gonadotropin-stimulated cycles. J Clin Endocrinol Metab 89(11):5742–5752
Ubaldi F, Bourgain C, Tournaye H (1997) Endometrial evaluation by aspiration biopsy on the day of oocyte retrieval in the embryo transfer cycles in patients with serum progesterone rise during the follicular phase. Fertil Steril 67(3):521–526
Nikas G, Develioglu OH, Toner JP (1999) Endometrial pinopodes indicate a shift in the window of receptivity in IVF cycles. Hum Reprod 14(3):787–792
Kolibianakis E, Bourgain C, Albano C (2002) Effect of ovarian stimulation with recombinant follicle-stimulating hormone, gonadotropin releasing hormone antagonists, and human chorionic gonadotropin on endometrial maturation on the day of oocyte pick-up. Fertil Steril 78(5):1025–1029
Maheshwari A, Pandey S, Shetty A (2012) Obstetric and perinatal outcomes in singleton pregnancies resulting from the transfer of frozen thawed versus fresh embryos generated through in vitro fertilization treatment: a systematic review and meta-analysis. Fertil Steril 98(2):368–377
Ishihara O, Araki R, Kuwahara A (2014) Impact of frozen-thawed single-blastocyst transfer on maternal and neonatal outcome: an analysis of 277,042 single-embryo transfer cycles from 2008 to 2010 in Japan. Fertil Steril 101(1):128–133
Wennerholm UB, Henningsen AK, Romundstad LB (2013) Perinatal outcomes of children born after frozen-thawed embryo transfer: a Nordic cohort study from the CoNARTaS group. Hum Reprod 28(9):2545–2553
Wennerholm UB, Soderstrom-Anttila V, Bergh C (2009) Children born after cryopreservation of embryos or oocytes: a systematic review of outcome data. Hum Reprod 24(9):2158–2172
Pinborg A, Wennerholm UB, Romundstad LB (2013) Why do singletons conceived after assisted reproduction technology have adverse perinatal outcome? Systematic review and meta-analysis. Hum Reprod Update 19(2):87–104
Johnson KM, Hacker MR, Resetkova N (2019) Risk of ischemic placental disease in fresh and frozen embryo transfer cycles. Fertil Steril 111(4):714–721
Acknowledgements
We thank the staff from Northwest Women’s and Children’s Hospital for their assistance with the data collection. We thank all participants in this study.
Funding
The study was funded by National Natural Science Foundation of China (No. 81771657 https://www.nsfc.gov.cn/) and General Projects of Social Development in Shaanxi Province (No. 2018SF-260).
Author information
Authors and Affiliations
Contributions
XTL: manuscript writing, HYB: data analysis, WHS: manuscript writing, JZS: protocol development.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
The approval of the Institutional Review Board of Northwest Women’s and Children’s Hospital was obtained for this retrospective cohort study (Number 2018002). All research was performed in accordance with relevant guidelines and regulations.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, X., Bai, H., Shi, W. et al. Frozen-thawed embryo transfer is better than fresh embryo transfer in GnRH antagonist cycle in women with 3–10 oocytes retrieved: a retrospective cohort study. Arch Gynecol Obstet 300, 1791–1796 (2019). https://doi.org/10.1007/s00404-019-05373-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-019-05373-9