Abstract
Purpose
Some evidence suggests that low maternal vitamin D status adversely affects perinatal health but few studies have examined cord blood vitamin D status. This project aimed to determine the association between the cord blood concentration of 25-hydroxyvitamin D [25(OH)D] and neonatal outcomes.
Methods
A nested case–control study was conducted in Quebec City, Canada from 2005 to 2010. Included were 83 cases of low birthweight (LBW; <2500 g), 301 cases of small for gestational age (SGA; <10th percentile), 223 cases of preterm birth (PTB; <37 weeks’ gestation), and 1027 controls. Levels of 25(OH)D were determined by chemiluminescence immunoassay. Adjusted odds ratios (OR) and 95 % confidence intervals (CI) were estimated with logistic regression.
Results
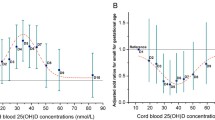
Cord blood [25(OH)D] <50 nmol/L was associated with a lower risk of LBW compared to [25(OH)D] ≥75 nmol/L (OR 0.47 95 % CI 0.23–0.97). For 25(OH)D levels 50–75 nmol/L, a significant association was not demonstrated (OR 0.58, 95 % CI 0.34–1.01). No significant associations were observed between [25(OH)D] and either SGA or PTB after adjustment.
Conclusions
Although our findings suggest that [25(OH)D] <50 nmol/L is associated with reduced risk of having a LBW infant, prenatal vitamin D recommendations require an examination of the literature that considers the full spectrum of maternal and neonatal outcomes.

Similar content being viewed by others
References
Ross AC, Taylor CL, Yatkine AL, Del Valle HB, Committee to Review Dietary Reference Intakes for Vitamin D and Calcium, Institute of Medicine (2011) Dietary reference intakes for calcium and vitamin D. National Academies Press, Washington, DC
Carlberg C, Campbell MJ (2013) Vitamin D receptor signaling mechanisms: integrated actions of a well-defined transcription factor. Steroids 78:127–136
Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, Murad MH, Weaver CM, Endocrine Society (2011) Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 96:1911–1930
Langlois K, Greene-Finestone L, Little J, Hidiroglou N, Whiting S (2010) Vitamin D status of Canadians as measured in the 2007–2009 Canadian Health Measures Survey. Health Rep 21:47–55
Whiting SJ, Langlois KA, Vatanparast H, Greene-Finestone LS (2011) The vitamin D status of Canadians relative to the 2011 dietary reference intakes: an examination in children and adults with and without supplement use. Am J Clin Nutr 94:128–135
Harvey NC, Holroyd C, Ntani G et al (2014) Vitamin D supplementation in pregnancy: a systematic review. Health Technol Assess 18:1–190
Aghajafari F, Nagulesapillai T, Ronksley PE, Tough SC, O’Beirne M, Rabi DM (2013) Association between maternal serum 25-hydroxyvitamin D level and pregnancy and neonatal outcomes: systematic review and meta-analysis of observational studies. BMJ 346:f1169
Wei SQ, Qi HP, Luo ZC, Fraser WD (2013) Maternal vitamin D status and adverse pregnancy outcomes: a systematic review and meta-analysis. J Matern Fetal Neonatal Med 26:889–899
Bowyer L, Catling-Paull C, Diamond T, Homer C, Davis G, Craig ME (2009) Vitamin D, PTH and calcium levels in pregnant women and their neonates. Clin Endocrinol (Oxf) 70:372–377
Burris HH, Rifas-Shiman SL, Camargo CA Jr et al (2012) Plasma 25-hydroxyvitamin D during pregnancy and small-for-gestational age in black and white infants. Ann Epidemiol 22:581–586
Dunlop AL, Taylor RN, Tangpricha V, Fortunato S, Menon R (2012) Maternal micronutrient status and preterm versus term birth for black and white US women. Reprod Sci 19:939–948
Hossain N, Khanani R, Hussain-Kanani F, Shah T, Arif S, Pal L (2011) High prevalence of vitamin D deficiency in Pakistani mothers and their newborns. Int J Gynaecol Obstet 112:229–233
Thorp JM, Camargo CA, McGee PL et al (2012) Vitamin D status and recurrent preterm birth: a nested case–control study in high-risk women. BJOG 119:1617–1623
Weiler H, Fitzpatrick-Wong S, Veitch R et al (2005) Vitamin D deficiency and whole-body and femur bone mass relative to weight in healthy newborns. CMAJ 172:757–761
Saigal S, Doyle LW (2008) An overview of mortality and sequelae of preterm birth from infancy to adulthood. Lancet 371:261–269
McCormick MC (1985) The contribution of low birth weight to infant mortality and childhood morbidity. N Engl J Med 312:82–90
Longo S, Bollani L, Decembrino L, Di Comite A, Angelini M, Stronati M (2013) Short-term and long-term sequelae in intrauterine growth retardation (IUGR). J Matern Fetal Neonatal Med 26:222–225
Kramer MS, Platt RW, Wen SW et al (2001) A new and improved population-based Canadian reference for birth weight for gestational age. Pediatrics 108:E35
Wagner CL, McNeil RB, Johnson DD et al (2013) Health characteristics and outcomes of two randomized vitamin D supplementation trials during pregnancy: a combined analysis. J Steroid Biochem Mol Biol 136:313–320
Yu CK, Sykes L, Sethi M, Teoh TG, Robinson S (2009) Vitamin D deficiency and supplementation during pregnancy. Clin Endocrinol (Oxf) 70:685–690
Bodnar LM, Catov JM, Zmuda JM et al (2010) Maternal serum 25-hydroxyvitamin D concentrations are associated with small-for-gestational age births in white women. J Nutr 140:999–1006
Camargo CA Jr, Ingham T, Wickens K et al (2010) Vitamin D status of newborns in New Zealand. Br J Nutr 104:1051–1057
Holmes VA, Barnes MS, Alexander HD, McFaul P, Wallace JM (2009) Vitamin D deficiency and insufficiency in pregnant women: a longitudinal study. Br J Nutr 102:876–881
Ozias MK, Kerling EH, Christifano DN, Scholtz SA, Colombo J, Carlson SE (2014) Typical prenatal vitamin D supplement intake does not prevent decrease of plasma 25-hydroxyvitamin d at birth. J Am Coll Nutr 33:394–399
Milman N, Hvas AM, Bergholt T (2011) Vitamin D status during normal pregnancy and postpartum: a longitudinal study in 141 Danish women. J Perinat Med 40:57–61
Bodnar LM, Catov JM, Wisner KL, Klebanoff MA (2009) Racial and seasonal differences in 25-hydroxyvitamin D detected in maternal sera frozen for over 40 years. Br J Nutr 101:278–284
Marwaha RK, Tandon N, Chopra S et al (2011) Vitamin D status in pregnant Indian women across trimesters and different seasons and its correlation with neonatal serum 25-hydroxyvitamin D levels. Br J Nutr 106:1383–1389
Public Health Agency of Canada (2008) Canadian Perinatal Health Report 2008 Edition. Ottawa
Auger N, Giraud J, Daniel M (2009) The joint influence of area income, income inequality, and immigrant density on adverse birth outcomes: a population-based study. BMC Public Health 9:237
Davies GA, Wolfe LA, Mottola MF, MacKinnon C (2003) Joint SOGC/CSEP clinical practice guideline: exercise in pregnancy and the postpartum period. Can J Appl Physiol 28:330–341
Acknowledgments
The Canadian Institutes of Health Research provided funding for this study (Operating Grant 244113). We acknowledge Madonna Achkar and Sherry Agellon from Dr. Hope Weiler’s laboratory at McGill University for their contribution in analyzing the cord blood samples. We thank Nathalie Bernard and Mylène Badeau from the Quebec City team for their professional assistance with the project, and our research nurses for the recruitment of participants and retrieval of data from the medical records. We acknowledge Anne Spencer for her assistance in data management and supplementary analyses. We also thank all study participants.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors do not have a financial relationship with the organization that sponsored this research. The authors had full control of all primary data and agree to allow the Journal to review their data if requested.
Rights and permissions
About this article
Cite this article
Morgan, C., Dodds, L., Langille, D.B. et al. Cord blood vitamin D status and neonatal outcomes in a birth cohort in Quebec, Canada. Arch Gynecol Obstet 293, 731–738 (2016). https://doi.org/10.1007/s00404-015-3899-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-015-3899-3