Abstract
Background
One of the important public health problems affecting maternal and child health is postpartum depression (PPD). It generally occurs within 6–8 weeks after childbirth.
Objectives
To determine the prevalence of postpartum depression (PPD) using a Kurdish version of Edinburgh postpartum depression scale (EPDS) and to analyze the risk factors for postpartum depression in a population of puerperal Kurdish women in Erbil city.
Patients and methods
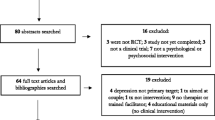
A cross-sectional study was conducted between 20th of June and 30th of November 2010, in 14 antenatal care units of primary health centers, in Erbil city, Kurdistan region, Iraq. The sample of the study included 1,000 puerperal women (6–8 weeks postpartum), ranging in age from 14 to 48 years. Data were collected after interviewing the women using a questionnaire designed by the researchers, and the Kurdish version of the EPDS. Chi square test of association and the logistic regression tests were used in the analysis.
Results
The prevalence of postpartum depression was 28.4%. Logistic regression analysis showed that the factors found to be associated with PPD were: physical or sexual abuse, delivery by cesarean section, history of past psychiatric illness, and family history of past psychiatric illness; while marriage with no previous agreement, and high socio-economic level were associated with lower levels of PPD.
Conclusion
The Kurdish version of the EPDS can be successfully used to screen depression in a Kurdish population of puerperal women.
Similar content being viewed by others
References
American Psychiatric Association (1994) Diagnosis and statistical manual of mental disorders, 4th edn. American Psychiatric association, Washington, DC
Evins GG, Theofrastous JP, Galvine SL (2000) Postpartum depression: a comparison of screening and routine clinical evaluation. Am J Obstet Gynecol 182:1080–1082
Beck C (1993) Teetering on the edge: a substantive theory of postpartum depression. Nurs Res 42(1):42–48
Leahy-Warren P, McCarthy G (2007) Postnatal Depression: prevalence, mother’s perspective, and treatments. Arch Psychiatry Nurs 21(2):91–100
Inwood DG (1994) Postpartum psychotic disorders. In: Sodock K (ed) Synopsis of psychiatry; behavioral science, clinical psychiatry, 7th edn. Williams & Wilkins, Baltimore, pp 852–858
Tannous L, Gigante L, Fuchs S, Busnello E (2008) Postnatal depression in southern Brazil: prevalence and its demographic and socioeconomic determinants. BMC psychiatry. Biomed Central Ltd
Lee D, Yip A, Chiu H (2000) Screening for postnatal depression using the double-test strategy. Psychosom Med 62:258–263
Thangappah R, Akosan TV, Rajeswari A (2005) Postpartum psychiatric illness. J Obstet Gynecol India 55(4):329–332
Beck CT (1995) Screening methods for postpartum depression. J Obstet Gynecol Neonatal Nurs 24:308–312
O’Hara MW, Swain AM (1996) Rates and risk of postpartum depression-a meta analysis. Int Rev Psychiatry 8:37–54
Cohen A (2000) Excess female mortality in India: the case of Himachal Pradesh. Am J Public Health 90:1369–1371
Dominic TS, Alexander SK, Sandra SM, Michelle HY, Tsui WS, Tony KH (2003) Post delivery screening for postpartum depression. Psychosom Med 65:357–3612
Schaper AM, Rooney BL, Kay NR, Silva PD (1994) Use of the Edinburgh postnatal depression scale to identify postpartum depression in a clinical setting. J Reprod Med 39:620–624
Cox JL, Holden JM (1994) Perinatal psychiatry: use and misuse of the Edinburgh postnatal depression scale. Gasku, London
Cox JL, Holden JM, Sagovsky R (1998) Detection of postnatal depression: development of the ten item Edinburgh postnatal Depression Scale. Br J Psychiatry 172:433–437
Adouard F, Glangeaud-Freudenthal NM, Golse B (2005) Validation of the Edinburgh postnatal depression scale (EPDS) in a sample of women with high-risk pregnancies in France. Arch Women Ment Health 8:89–95
Statistical Department/Directorate of Health/Erbil Governorate/Kurdistan Region/Iraq, 2009
Ghubash R, Abou-Saleh MT (1997) Postpartum psychiatric illness in Arab culture: prevalence and psychosocial correlates. Br J Psychiatry 171:65–68
Chaaya M, Campbell OM, El Kak F, Shaar D, Harb H, Kaddour A (2002) Postpartum depression: prevalence and determinants in Lebanon. Arch Women Ment Health 5:65–72
Kirpinar I, Gozum S, Pasinlioglu T (2010) Prospective study of postpartum depression in eastern Turkey prevalence, socio-demographic and obstetric correlates, prenatal anxiety and early awareness. J Clin Nurs Feb 19(3–4):422–431
Mohr WK; American Psychiatric Association (2003) Johndon’s psychiatric-mental health nursing. 5th edn. Lippincott Williams & Wilkins, Philadelphia
Department of Non-communicable Disease Surveillance World Health Organization 1999, Definition, diagnosis and classification of diabetes mellitus and its complications. http://www.staff.ncl.ac.uk/philip.home/who_dmc.htm
Anon (2011) Definition of hypertension. MedicineNet. http://www.medterms.com/script/main/art.asp?articlekey=3846
Cunningham FC, Leveno KJ, Bloom SL, Hauth JC, Gilstrap LC Wenstrom KD (2005) Williams obstetrics. 22nd edn. McGraw-Hill Companies, New York
Mohr WK (2003) Johndon’s psychiatric-mental health nursing. 5th ed. Lippincott Williams & Wilkins, Philadelphia
Cox JL, Holden JM, Sagovsky R (1987) Detection of postnatal depression: Development of the 10-item Edinburgh Postnatal depression Scale. Br J Psychiatry 150:782–786
Schoeman JH, Westaway MS, Neethling A (1991) The relationship between socioeconomic factors and pulmonary tuberculosis. Int J Epidemiol 20:435–440
Esquivel C, Alvarez A, Martinez C, Garcia S (2006) Validation of the Edinburgh postpartum depression scale in a population of puerperal women in Mexico. Clin Pract Epidemiol Ment health 2:33
Inandia T, Cinar T, Ozturkd A, Egrie M, Polatf A, Sahing T et al (2002) Risk factors for depression in postnatal first year, in eastern Turkey. Int J Epidemiol 31(6):1201–1207
Stern G, Kruckman L (1983) Multi-disciplinary perspectives on postpartum depression: An anthropological critique. Soc Sci Med 17:1027-1041. Cross Ref Medline Web of Science
Cox JL (1988) Childbirth as a life events: Socio-cultural aspects of postnatal depression. Acta Psychiatry Scand 344:75–82
Kumar R (1994) Postnatal mental illness: a trans-cultural perspective. Soc Psychiatry Epidemiol 29:250–264
Webster J (2001) Postnatal depression and health care use. Aust Fam Physician 30(11):1024
Patel V, Rodrigues M, DeSouza N (2002) Gender, Poverty and postnatal depression: a study of mothers in Goa, India. Am J Psychiatry 159:43–47
Prabhu TR, Asokan TV, Rajeswari A (2005) Postpartum psychiatric illness. J Obstet Gynecol India 55(4):329–332
Carter F, Farmpton C, Mulder R (2006) Cesarean section & postpartum depression: a review of the evidence examining the link. Psychosm Med 68:321–330
Fisher J, Astbury J, Smith A (1997) Adverse psychological impact of operative obstetric interventions: a prospective longitudinal study. Aust N Z J Psychiatry 31:728–738
Green J, Coupland V, Kitzinger J (1990) Expectations, experiences, and psychological outcomes of childbirth: a prospective study of 825 women. Birth 17:15–24
Seritan A (2006) Postpartum depression or medical problem? Watch for fatigue, weight change, other physical signs. Curr Psychiatry 5(9):62–75
Boyles S (2009) Diabetes in pregnancy tied to depression. WebMD Health News. http://www.webmd.com/depression/postpartum-depression/news/20090224/diabetes-in-pregnancy-tied-to-depression. Accessed 27 Feb 2011
Conflict of interest
We declare that we have no conflict of interest in the current study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ahmed, H.M., Alalaf, S.K. & Al-Tawil, N.G. Screening for postpartum depression using Kurdish version of Edinburgh postnatal depression scale. Arch Gynecol Obstet 285, 1249–1255 (2012). https://doi.org/10.1007/s00404-011-2165-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-011-2165-6