Abstract
Introduction
Hip fractures have increased medical and socio-economic importance due to demographic transition. Information concerning direct treatment costs and their reimbursement in Germany is lacking.
Materials and methods
Four hundred two hip fracture patients older than 60 years of age were observed prospectively at a German University Hospital. Treatment costs were determined with up to 196 cost factors and compared to the reimbursement. Finally, statistical analysis was performed to identify clinical parameters influencing the cost–reimbursement relation.
Results
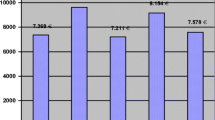
Treatment costs were 8853 € (95% CI 8297–9410 €), while reimbursement was 8196 € (95% CI 7707–8772 €), resulting in a deficit of 657 € (95% CI 143–1117 €). Bivariate analysis showed that the cost–reimbursement relation was negatively influenced mainly by higher age, higher ASA score, readmission to the intensive care unit (ICU) and red blood cell transfusion. Adjusted for other parameters, readmission to the ICU was a significant negative predictor (− 2669 €; 95% CI – 4070 to − 1268 €; p < 0.001), while age of 60–75 years was a positive predictor for the cost–reimbursement relation (1373 €; 95% CI 265–2480 €; p = 0.015).
Conclusions
Treatment of geriatric hip fracture patients in a university hospital in Germany does not seem to be cost-covering. Adjustment of the reimbursement for treatment of complex hip fracture patients should be considered.

Similar content being viewed by others
References
Ström O, Borgström F, Kanis JA, Compston J, Cooper C, McCloskey EV, Jönsson B (2011) Osteoporosis: burden, health care provision and opportunities in the EU: a report prepared in collaboration with the International Osteoporosis Foundation (IOF) and the European Federation of Pharmaceutical Industry Associations (EFPIA). Arch Osteoporos 6:59–155
Folbert EC, Hegeman JH, Gierveld R, van Netten JJ, Velde DV, Ten Duis HJ, Slaets JP (2017) Complications during hospitalization and risk factors in elderly patients with hip fracture following integrated orthogeriatric treatment. Arch Orthop Trauma Surg 137:507–515
Cha YH, Ha YC, Yoo JI, Min YS, Lee YK, Koo KH (2017) Effect of causes of surgical delay on early and late mortality in patients with proximal hip fracture. Arch Orthop Trauma Surg 137:625–630
Moerman S, Vochteloo AJ, Tuinebreijer WE, Maier AB, Mathijssen NM, Nelissen RG (2016) Factors associated with the course of health-related quality of life after a hip fracture. Arch Orthop Trauma Surg 136:935–943
Singer A, Exuzides A, Spangler L, O’Malley C, Colby C, Johnston K, Agodoa I, Baker J, Kagan R (2015) Burden of illness for osteoporotic fractures compared with other serious diseases among postmenopausal women in the United States. Mayo Clin Proc 90:53–62
Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A (2007) Incidence and economic burden of osteoporosis-related fractures in the United States, 2005–2025. J Bone Miner Res 22:465–475
Sahota O, Morgan N, Moran CG (2012) The direct cost of acute hip fracture care in care home residents in the UK. Osteoporos Int 23:917–920
Nikkel LE, Fox EJ, Black KP, Davis C, Andersen L, Hollenbeak CS (2012) Impact of comorbidities on hospitalization costs following hip fracture. J Bone Jt Surg Am 94:9–17
Leal J, Gray AM, Prieto-Alhambra D, Arden NK, Cooper C, Javaid MK, Judge A, REFReSH study group (2016) Impact of hip fracture on hospital care costs: a population-based study. Osteoporos Int 27:549–558
Baker SP, O’Neill B, Haddon W, Long WB (1974) The injury severity score: a method for describing patients with multiple injuries and evaluating emergency care. J Trauma 14:187–196
Anaestesiologists ASo (2015) American Society of Anesthesiologists. ASA physical status classification system. http://www.asahq.org/resources/clinical-information/asa-physical-status-classification-system. Accessed 18 February 2015
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
German Federal Statistical Office (2016) https://www.destatis.de/DE/ZahlenFakten/GesellschaftStaat/Gesundheit/Krankenhaeuser/Methoden/FallpauschalenbezogeneKrankenhausstatistik.html. Accessed 22 November 2016
AQUA (2010). Institut für angewandte Qualitätsförderung und Forschung im Gesundheitswesen; Sektorenübergreifende Qualitätssicherung, Hüftgelenksnahe Femurfraktur, Bundesauswertung. https://www.sqg.de/downloads/Bundesauswertungen/2010/bu_Gesamt_17N1-HUEFT-FRAK_2010.pdf (Download 21.02.2016)
Bliemel C, Lechler P, Oberkircher L, Colcuc C, Balzer-Geldsetzer M, Dodel R, Ruchholtz S, Buecking B (2015) Effect of preexisting cognitive impairment on in-patient treatment and discharge management among elderly patients with hip fractures. Dement Geriatr Cogn Disord 40:33–43
Lu Q, Tang G, Zhao X, Guo S, Cai B, Li Q (2017) Hemiarthroplasty versus internal fixation in super-aged patients with undisplaced femoral neck fractures: a 5-year follow-up of randomized controlled trial. Arch Orthop Trauma Surg 137:27–35
Knobe M, Siebert CH (2014) [Hip fractures in the elderly: osteosynthesis versus joint replacement]. Orthopade 43:314–324
Buecking B, Eschbach D, Koutras C, Kratz T, Balzer-Geldsetzer M, Dodel R, Ruchholtz S (2013) Re-admission to Level 2 unit after hip-fracture surgery—risk factors, reasons and outcome. Injury 44:1919–1925
Buecking B, Timmesfeld N, Riem S, Bliemel C, Hartwig E, Friess T, Liener U, Ruchholtz S, Eschbach D (2013) Early orthogeriatric treatment of trauma in the elderly: a systematic review and metaanalysis. Dtsch Arztebl Int 110:255–262
Gosch M, Hoffmann-Weltin Y, Roth T, Blauth M, Nicholas JA, Kammerlander C (2016) Orthogeriatric co-management improves the outcome of long-term care residents with fragility fractures. Arch Orthop Trauma Surg 136:1403–1409
Grund S, Roos M, Duchene W, Schuler M (2015) Treatment in a center for geriatric traumatology. Dtsch Arztebl Int 112:113–119
Institut für das Entgeldsystem im Krankenhaus, G-DRG-System (2016). http://www.g-drg.de/cms/G-DRG-System_2016 (Download 01.02.2016)
Prokop A, Reinauer KM, Chmielnicki M (2015) Is there sense in having a certified centre for geriatric trauma surgery? Z Orthop Unfall 153:306–311
Carson JL, Terrin ML, Noveck H et al (2011) Liberal or restrictive transfusion in high-risk patients after hip surgery. N Engl J Med 365:2453–2462
Cuenca Espiérrez J, García Erce JA, Martínez Martín AA, Solano VM, Modrego Aranda FJ (2004) Safety and usefulness of parenteral iron in the management of anemia due to hip fracture in the elderly. Med Clin (Barc) 123:281–285
Lee C, Freeman R, Edmondson M, Rogers BA (2015) The efficacy of tranexamic acid in hip hemiarthroplasty surgery: an observational cohort study. Injury 46:1978–1982
Nawata K, Nitta A, Watanabe S, Kawabuchi K (2006) An analysis of the length of stay and effectiveness of treatment for hip fracture patients in Japan: evaluation of the 2002 revision of the medical service fee schedule. J Health Econ 25:722–739
Birkmeyer JD, Gust C, Baser O, Dimick JB, Sutherland JM, Skinner JS (2010) Medicare payments for common inpatient procedures: implications for episode-based payment bundling. Health Serv Res 45:1783–1795
Acknowledgements
The authors would like to thank Mr. Gerd Bodenbender for his support in determining the treatment costs.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Aigner, R., Hack, J., Eschbach, D. et al. Is treatment of geriatric hip fracture patients cost-covering? Results of a prospective study conducted at a German University Hospital. Arch Orthop Trauma Surg 138, 331–337 (2018). https://doi.org/10.1007/s00402-017-2844-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-017-2844-2