Abstract
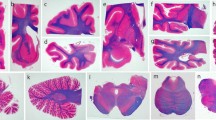
Progressive supranuclear palsy (PSP) is known to have tau-positive cytoskeletal abnormalities in astrocytes and oligodendroglia as well as neurons. Astrocytic tau-positive structures (tuft-shaped astrocytes; Tu-SA) were studied to elucidate their proper significance in the neuropathological diagnosis of PSP. The distribution and incidence of Tu-SA were examined in 26 cases of PSP. The disease specificity of Tu-SA was demonstrated by comparison with diseases accompanied by neurofibrillary tangles (NFTs) and those with or without cytoskeletal abnormalities other than NFTs. In PSP, Tu-SA appeared prominently in the precentral and premotor cortex (areas 4 and 6) of the superior and middle frontal gyri, but were quite scare in the temporal lobe and limbic area. In the subcortical nuclei, they appeared preferentially in the putamen and were also scattered in other degenerating regions. In the cerebrum the Tu-SA and NFTs were distributed in quite different regions. The assessment of the incidence of Tu-SA in area 6 revealed that only 5 of 26 PSP cases lacked Tu-SA in the examined fields. In contrast, in the control diseases, Tu-SA were found only rarely in cases of corticobasal degeneration in the cerebral cortex among other frequent tau-positive structures. One case of Pick’s disease showed occasional Tu-SA but only in the hippocampal region and not in the frontal lobe or putamen. In summary, although the absence of Tu-SA does not necessarily exclude the possibility of PSP, Tu-SA in the frontal lobe and putamen is highly suggestive for PSP. Thus, detection of Tu-SA and the ranking of the characteristic distribution of NFTs contribute to the neuropathological diagnosis of PSP.
Similar content being viewed by others
Author information
Authors and Affiliations
Additional information
Received: 22 September 1997 / Revised, accepted: 2 March 1998
Rights and permissions
About this article
Cite this article
Matsusaka, H., Ikeda, K., Akiyama, H. et al. Astrocytic pathology in progressive supranuclear palsy: significance for neuropathological diagnosis. Acta Neuropathol 96, 248–252 (1998). https://doi.org/10.1007/s004010050891
Issue Date:
DOI: https://doi.org/10.1007/s004010050891